 |
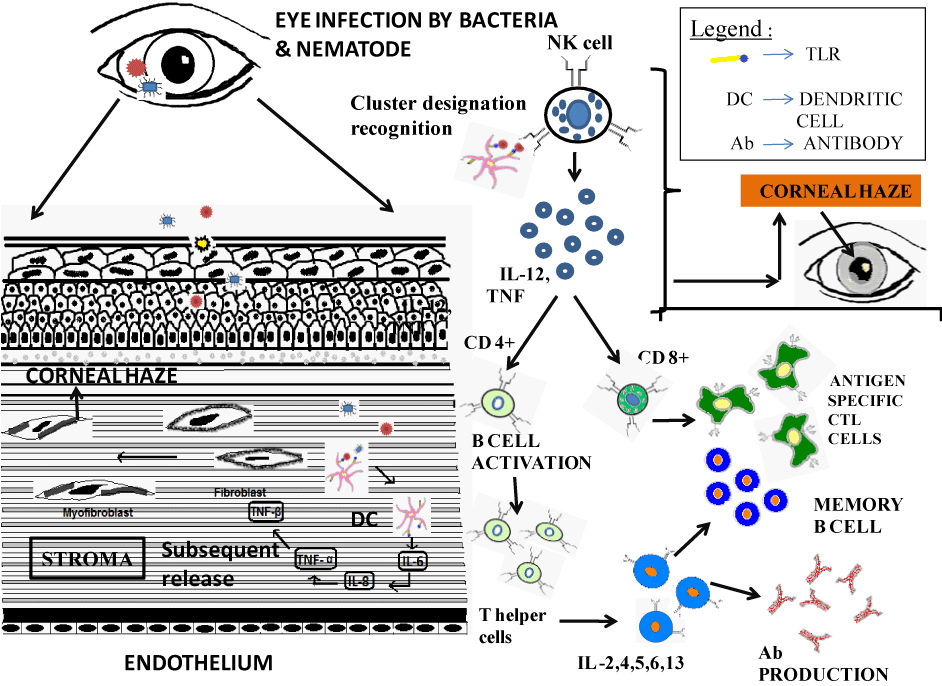
| Figure 1: Cornea is made of three layers such as outer epithelium, middle stromal cells and inner endothelium cells. Inflammation of eye can lead to serious loss of vision and is a leading cause of blindness. Immune responses in the eye are modulated by tissue resident cells. Cornea is exposed to microbes constantly. Entry of bacteria into the eye results in rapid proliferation since vitreous acts an excellent medium. Ocular barrier breakdown and inflammatory cell recruitment is expected due to initiation of inflammatory products cascade. Though lysozyme secretion catalyzes the hydrolysis of cell membrane, some pathogenic bacteria possess high in vitro resistance to lysozyme. When they breach the epithelial layer, TLRs of ocular cells recognise the Ag and secrete proinflammatory cytokines like IL-8, IL-1 and TNF- a. These chemokines attract DCs to the infection site. Release of TGF-ß, IL and CXC-2 recruits neutrophils to the infected site. This process results in transformation of normal fibroblast to myofibroblast, thus reducing corneal transparency. Once the sentinels take up the Ag, they present it to NK cells which then activate T-helper cells and indirectly the B cells. As a result antibodies are raised against the Ag. |