 |
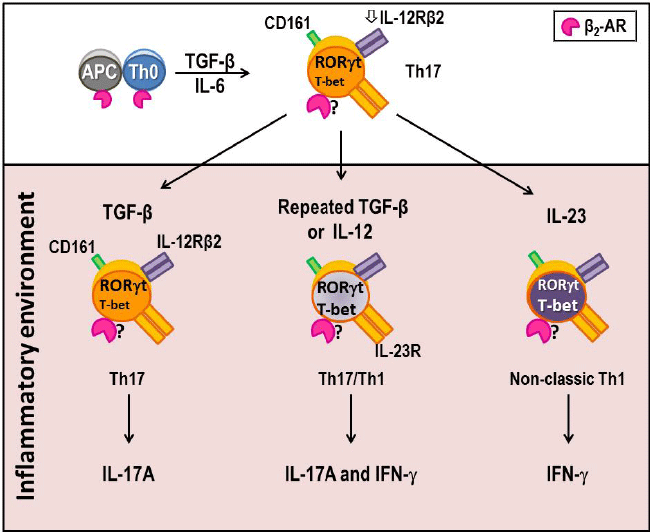
| Figure 14: Late Th17 cell plasticity. Naïve Th cells that have been activated by antigen in the presence of TGF-β and IL-6 differentiate into Th17 cells via activation of the RORγt transcription program. IL-6 induces Th17 cells to produce IL-12, which subsequently up regulates RORγt expression. In an inflammatory environment, stimulation with re-stimulation with TGF-β, Th17 cells regain their high production of IL-17A. However, re-stimulation with IL-12 leads to the expression of IL-23R in addition to low levels of IL-12Rβ2. Thus, Th17 cells are responsive to both IL-23 and IL-12. Th17 cells exhibit high late plasticity, depending upon the balance of TGF-β, IL-23 and IL-12 in the milieu. In the repeated presence of relatively high TGF-β (compared to IL-23 or IL- 12), Th 17 cells derived from Th0 cells produce high levels of IL-17A and IL- 17F. If IL-23 is the dominant cytokine, then T-bet expression is increase and these cells further differentiate to IL-17A and IFN-γ producing Th17/Th1 cells. Interestingly, either repeated stimulation with TGF-β in the absence of IL-12 or IL-23 or a dominant presence of IL-12 can induce shift the transcriptional program towards higher activation of T-bet, resulting in Th17 cells that produce both IL-17A and IFN-γ. In contrast, Th17 cells restimulated in an inflammatory environment with IL-23 induce a differentiation shift towards non-classic Th1 cells that produce IFN-γ due to activation of the T-bet transcription program. All of these Th17 subtypes express CD161, a traditional marker of Th17 cells. |