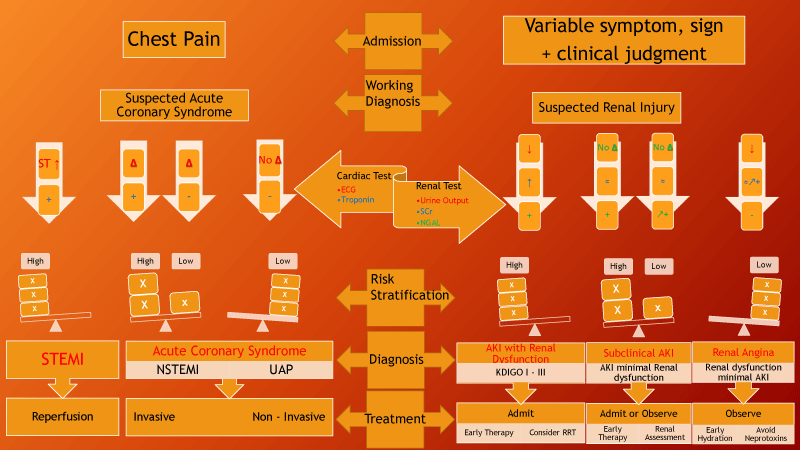
 Two clinical pathways are shown. Chest pain pathways are well established.
Renal pathways are less well established. Urine output and SCr provide surrogate
information on renal function. With the advent of AKI biomarkers, clinicians now
have the ability to anticipate renal injury, with or without functional changes, as
early as 2 hours from the insult. With more specific and comprehensive renal
injury and function information we also begin the paradigm of reclassification the
spectrum of “acute kidney syndromes”. We have chosen the term “Kidney Attack”
as it highlights firstly the urgency involved and secondly there are correlations with
the lessons learnt from the heart. We emphasize that the role of AKI biomarkers
are still partly in the research domain, and so to our understanding of “acute
kidney syndromes”. As such the schema proposed, has a degree of conjecture,
however we feel that significant impetus is needed to highlight renal injury risks
and as such the severity of the “Kidney Attack”. We have chosen NGAL from the
spectrum of renal biomarkers as it remains the most likely candidate for a “Renal
Troponin”. Renal injury biomarkers have a broader pathogenic base than serum
troponin, for those discussion we point readers initially to Ref 15. (Diagram and
concepts modified from ref 14, 15).
Two clinical pathways are shown. Chest pain pathways are well established.
Renal pathways are less well established. Urine output and SCr provide surrogate
information on renal function. With the advent of AKI biomarkers, clinicians now
have the ability to anticipate renal injury, with or without functional changes, as
early as 2 hours from the insult. With more specific and comprehensive renal
injury and function information we also begin the paradigm of reclassification the
spectrum of “acute kidney syndromes”. We have chosen the term “Kidney Attack”
as it highlights firstly the urgency involved and secondly there are correlations with
the lessons learnt from the heart. We emphasize that the role of AKI biomarkers
are still partly in the research domain, and so to our understanding of “acute
kidney syndromes”. As such the schema proposed, has a degree of conjecture,
however we feel that significant impetus is needed to highlight renal injury risks
and as such the severity of the “Kidney Attack”. We have chosen NGAL from the
spectrum of renal biomarkers as it remains the most likely candidate for a “Renal
Troponin”. Renal injury biomarkers have a broader pathogenic base than serum
troponin, for those discussion we point readers initially to Ref 15. (Diagram and
concepts modified from ref 14, 15).ABBREVIATIONS: AKI = acute kidney injury; ECG = electrocardiogram; EF = ejection fraction , surrogate for cardiac function. EKG = electrocardiogram; NGAL = neutrophil gelatinase associated lipocalin; NSTEMI = non ST elevation myocardial infarction; ST segments; STEMI = ST elevation myocardial infarction; Sym = symptom; UAP = unstable angina pectoris; UO = urine output;
SYMBOLS: ↑ increased; ↓ = decreased; ↑ = Trend; + = positive; - negative; ± equivocal; Δ = changes; ↑ + range from equivocal to positive