Indexed In
- Open J Gate
- Genamics JournalSeek
- Academic Keys
- JournalTOCs
- China National Knowledge Infrastructure (CNKI)
- Ulrich's Periodicals Directory
- RefSeek
- Hamdard University
- EBSCO A-Z
- Directory of Abstract Indexing for Journals
- OCLC- WorldCat
- Publons
- Geneva Foundation for Medical Education and Research
- Euro Pub
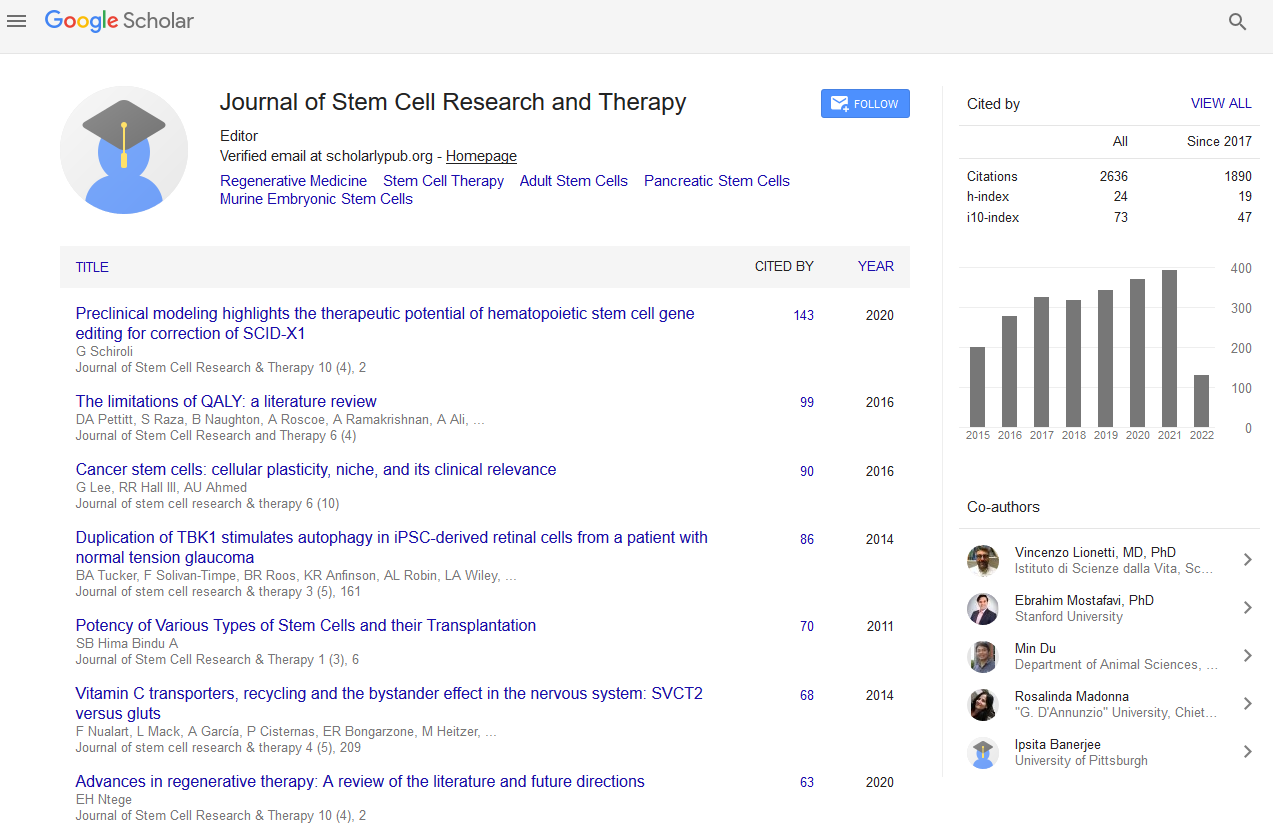
- Google Scholar
Useful Links
Share This Page
Journal Flyer

Open Access Journals
- Agri and Aquaculture
- Biochemistry
- Bioinformatics & Systems Biology
- Business & Management
- Chemistry
- Clinical Sciences
- Engineering
- Food & Nutrition
- General Science
- Genetics & Molecular Biology
- Immunology & Microbiology
- Medical Sciences
- Neuroscience & Psychology
- Nursing & Health Care
- Pharmaceutical Sciences
Abstract
Mesenchymal Stem Cell Therapy in Type 1 Diabetes Mellitus and Its Main Complications: From Experimental Findings to Clinical Practice
Marcelo Ezquer, Martha Arango-Rodriguez, Maximiliano Giraud-Billoud and Fernando Ezquer
Type 1 diabetes mellitus (T1DM) is a complex multifactorial disorder which involves a loss of self-tolerance leading to the autoimmune destruction of pancreatic β−cells. Exogenous insulin administration cannot mimic precise pancreatic β-cell regulation of glucose homeostasis, thereby leading to severe long-term complications. Pancreas or islet transplant only provides partial exogenous insulin independence and induces several adverse effects, including increased morbidity and mortality. The scientific community and diabetic patients are thus, still waiting for an effective therapy which could preserve the remaining β-cells, replenish islet mass and protect newly-generated β-cells from autoimmune destruction. Mesenchymal stem cells (MSCs) have been envisioned as a promising tool for T1DM treatment over the past few years, since they could differentiate into glucose-responsive insulin-producing cells. Their immunomodulatory and proangiogenic roles can be used to help arrest β-cell destruction, preserve residual β-cell mass, facilitate endogenous β-cell regeneration and prevent disease recurrence, thereby making them ideal candidates for the comprehensive treatment of diabetic patients. This review focuses on recent pre-clinical data supporting MSC use in regenerating β-cell mass and also in treating several T1DM-associated complications. Clinical trial results and the ongoing obstacles which must be addressed regarding the widespread use of such therapy are also discussed.