Indexed In
- Open J Gate
- Genamics JournalSeek
- Academic Keys
- JournalTOCs
- RefSeek
- Hamdard University
- EBSCO A-Z
- SWB online catalog
- Publons
- Geneva Foundation for Medical Education and Research
- Euro Pub
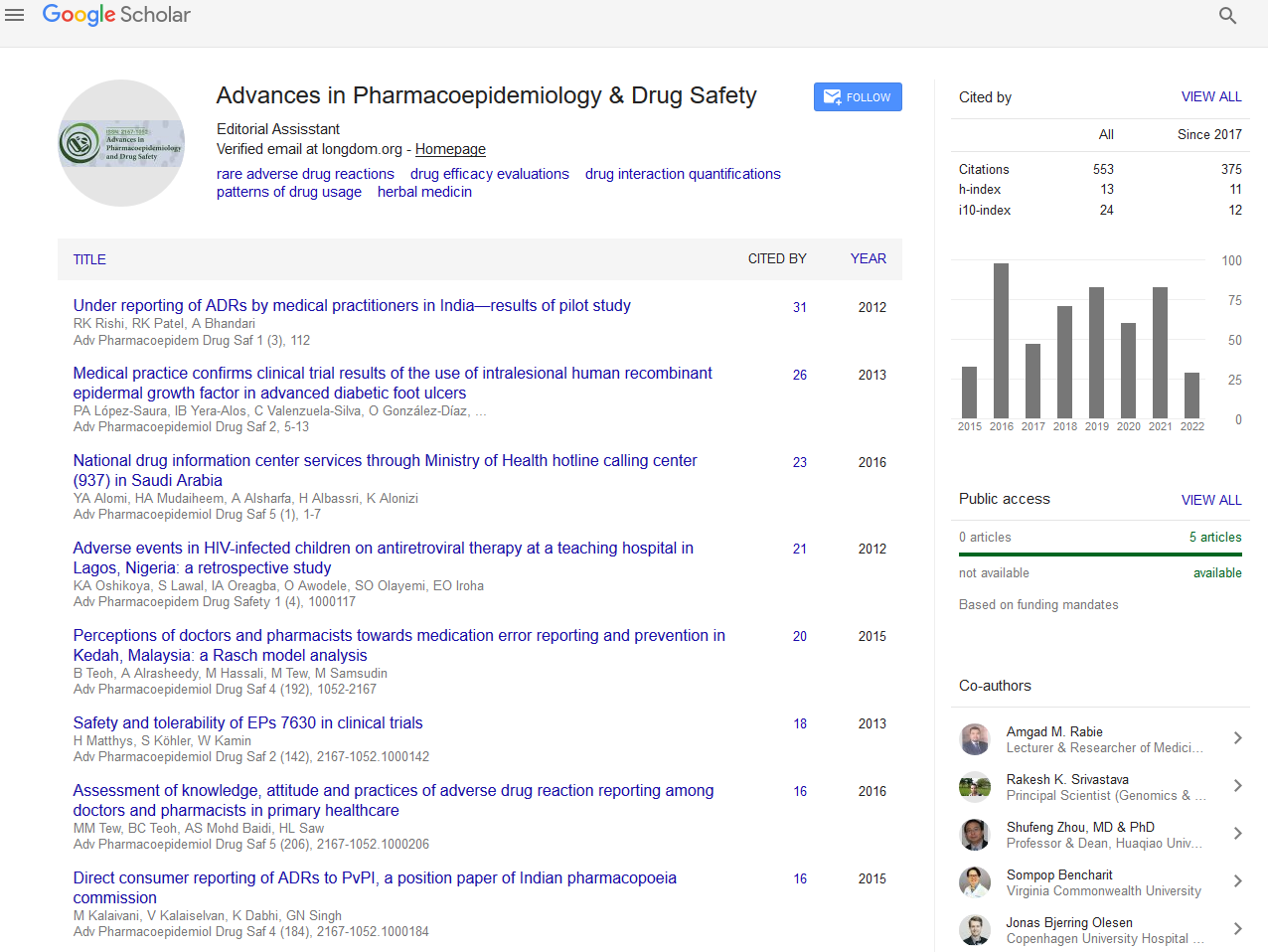
- Google Scholar
Useful Links
Share This Page
Journal Flyer

Open Access Journals
- Agri and Aquaculture
- Biochemistry
- Bioinformatics & Systems Biology
- Business & Management
- Chemistry
- Clinical Sciences
- Engineering
- Food & Nutrition
- General Science
- Genetics & Molecular Biology
- Immunology & Microbiology
- Medical Sciences
- Neuroscience & Psychology
- Nursing & Health Care
- Pharmaceutical Sciences
Abstract
Challenge of Using Antiplatelet Drugs in Patients with Primary Immune Thrombocytopenia and Recently Implanted Coronary Stents-Splenectomy as a Therapeutic Option
Dragomir Marisavljevic, Olivera Markovic, Marija Zdravković, Saša Hinić, Nada Suvajdžić-Vuković and Branka Filipović
Background: Immune thrombocytopenic purpura (ITP) in the patients with implanted coronary stents is related with serious risks of haemorrhage related to dual antiplatelet therapy on the one hand and stent thrombosis if antiplatelet therapy is interrupted on the other hand. Therefore, the main objective in these patients is the correction of thrombocytopenia and continuous use of antiplatelet drugs.
Case report: We present the patient with implanted stents after acute myocardial infarction (AMI) and severe ITP who was successfully treated with splenectomy. After the patient experienced AMI, primary percutaneous coronary intervention (PCI) with implantation of stents has been performed. Thrombocytopenia (21 × 109/L) was registered for the first time after PCI intervention when it has been noticed a massive hematoma of whole right arm at the site of radial artery puncture. Immediately after the intervention dual antiplatelet therapy and prednisone has been started. Since corticosteroids and azathioprine treatment proved unsuccessful (platelet count <10 × 109/L), the patient has been prepared for splenectomy with intravenous immunoglobulins. As the platelet count was in stable range (40-50 × 109/L) after splenectomy, antiplatelet therapy has been readministered safely.
Conclusion: As there are no definitive guidelines for treatment of patients with ITP and implanted stents, the treatment should be individualized to minimize risk of hemorrhagic as well as thrombotic complications. Our case suggests that splenectomy is an available and safe treatment for these patients. However, decision on splenectomy is a challenge; and before the surgical intervention the risk-benefit assessment should be considered.