Indexed In
- Open J Gate
- Genamics JournalSeek
- CiteFactor
- Cosmos IF
- Scimago
- Ulrich's Periodicals Directory
- Electronic Journals Library
- RefSeek
- Hamdard University
- EBSCO A-Z
- Directory of Abstract Indexing for Journals
- OCLC- WorldCat
- Proquest Summons
- Scholarsteer
- ROAD
- Virtual Library of Biology (vifabio)
- Publons
- Geneva Foundation for Medical Education and Research
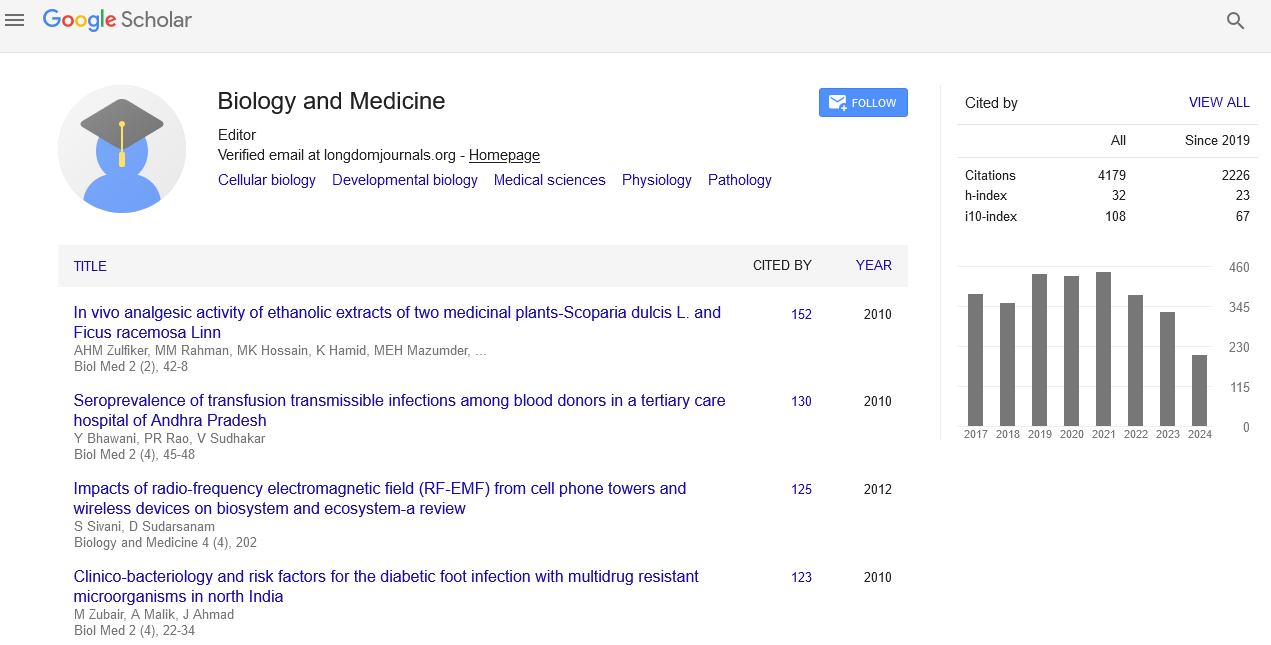
- Google Scholar
Useful Links
Share This Page
Journal Flyer

Open Access Journals
- Agri and Aquaculture
- Biochemistry
- Bioinformatics & Systems Biology
- Business & Management
- Chemistry
- Clinical Sciences
- Engineering
- Food & Nutrition
- General Science
- Genetics & Molecular Biology
- Immunology & Microbiology
- Medical Sciences
- Neuroscience & Psychology
- Nursing & Health Care
- Pharmaceutical Sciences
Abstract
Estrogen-Dependent Downregulation of Hepcidin Synthesis Induces Intracellular Iron Efflux in Cancer Cells In Vitro
Jasmin Shafarin, Khuloud Bajbouj, Ahmed El-Serafy, Divyasree Sandeep and Mawieh Hamad
It is well accepted that intracellular iron overload that associate with various forms of cancer fuels tumor mutagenesis and growth. Hence, iron chelation therapy is being increasingly used to minimize iron overload in cancer patients despite significant safety and efficacy concerns. Mounting evidence suggests that estrogen (E2) downregulates hepcidin synthesis and increases serum iron concentration. It is postulated therefore that, by downregulating hepcidin synthesis, E2 may maintain ferroportin integrity and enhance intracellular iron efflux. Here, MCF-7 and SKOV-3 cancer cells treated with increasing concentrations (5, 10 and 20 nM) of E2 were assessed for intracellular labile iron content, the expression of hepcidin, ferroportin, and transferrin receptors 1 and 2 along with cell viability at different time points post treatment. In MCF-7 cells, E2 treatment resulted in a significant reduction in hepcidin synthesis, most noticeably at the 20 nM/24 h dose, a significant increase in ferroportin expression and a marked decrease in transferrin receptors 1 and 2 expression. E2-treated cells also showed reduced intracellular labile iron content most evidently at 20 nM/48 h dose and reduced viability especially at 20 nM/72 h dose. E2-treated SKOV-3 showed slightly reduced intracellular labile iron content, reduced expression of hepcidin and significantly increased expression of TFR1 but not TFR2; FPN expression was overall similar to that of controls. The effects of E2 on intracellular iron metabolism in SKOV-3 were most evident at 5 nM/24 h dose. These findings suggest that E2 treatment induces intracellular iron efflux, which may minimize intracellular iron overload in cancer cells; disrupted expression of transferrin receptor 1 and/or 2 may help sustain a low intracellular iron environment.