Indexed In
- Open J Gate
- Genamics JournalSeek
- Academic Keys
- JournalTOCs
- China National Knowledge Infrastructure (CNKI)
- Ulrich's Periodicals Directory
- RefSeek
- Hamdard University
- EBSCO A-Z
- Directory of Abstract Indexing for Journals
- OCLC- WorldCat
- Publons
- Geneva Foundation for Medical Education and Research
- Euro Pub
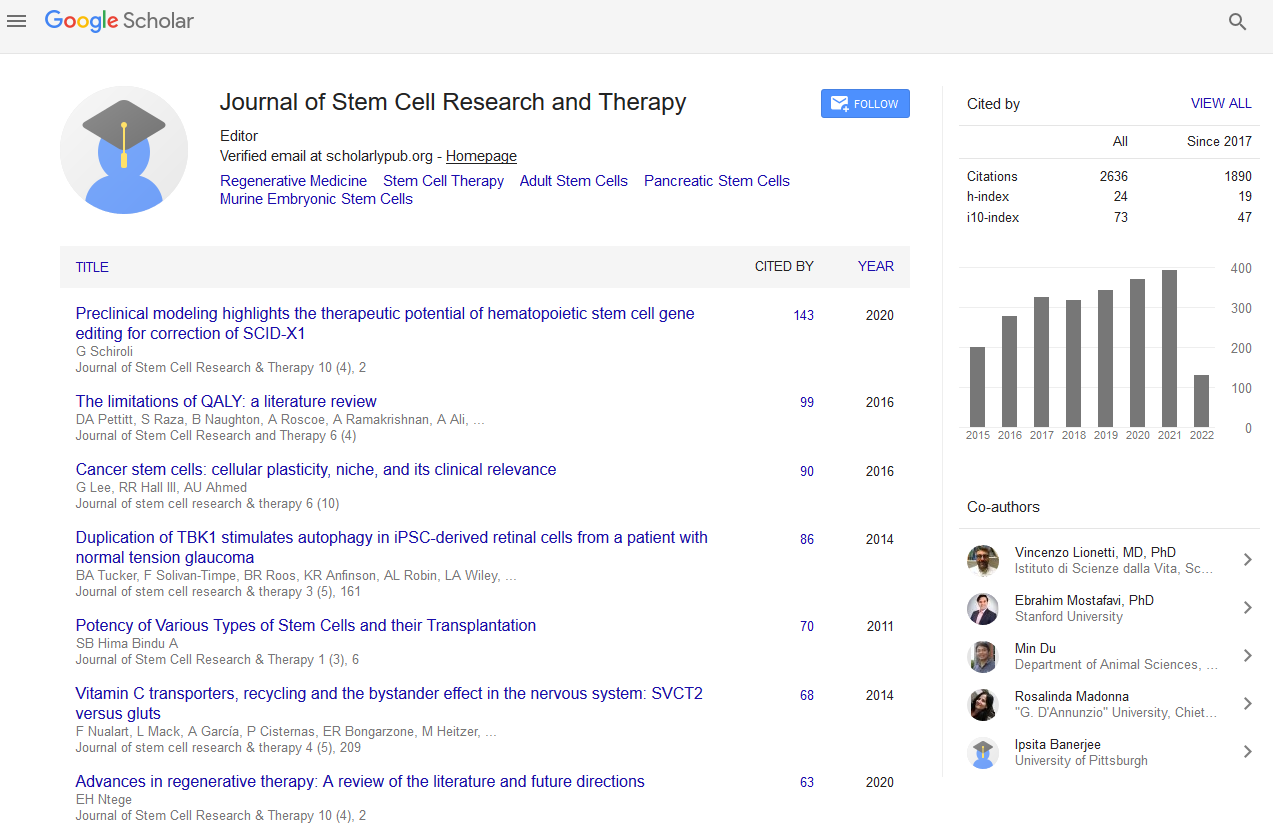
- Google Scholar
Useful Links
Share This Page
Journal Flyer

Open Access Journals
- Agri and Aquaculture
- Biochemistry
- Bioinformatics & Systems Biology
- Business & Management
- Chemistry
- Clinical Sciences
- Engineering
- Food & Nutrition
- General Science
- Genetics & Molecular Biology
- Immunology & Microbiology
- Medical Sciences
- Neuroscience & Psychology
- Nursing & Health Care
- Pharmaceutical Sciences
Abstract
Long-Term Results of Cultured Autologous Oral Mucosa Epithelial Cell-Sheet (CAOMECS) Graft for the Treatment of Blindness Due to Bilateral Limbal Stem Cell Deficiency
Kocaba V, Thépot A, Yamato M, Daisuke M, Kellal M, Mojallal A, Damour O and Burillon C
Purpose: To treat bilateral corneal blindness due to limbal stem cell deficiency (LSCD) thanks to corneal transplant of an autologous epithelium of stem cells cultivated by the oral mucous membrane by the technology UpCell®-Insert (CAOMECS for Cultured Autologous Oral Mucosal Epithelial Cell-Sheet). Methods: The efficacy of a CAOMECS corneal graft was assessed over the long term for 23 out of 26 eyes presenting severe bilateral LSCD. This study follows a clinical trial evaluated, which lasted for 12 months. The major evaluation criterion was visual acuity and the minor criteria were the condition of the epithelium (a composite criterion assessed by grading superficial punctate keratitis, the presence of ulcer, the number and activity of neovessels and the presence of conjunctivalization) and the quality of life (grading of photophobia, dryness and pain). The mean follow-up was of 28 months [18-48 months]. Findings: Visual acuity was increased for 17 patients out of 23 treated (74%), the state of the epithelium was improved for 15 patients (62.5%) and the quality of life was improved for 22 patients (95.6%). For the nine patients with stromal opacity, CAOMECS grafting, reducing limbal neovascularization also made it possible to perform a penetrating keratoplasty (until then impossible because of insufficient stem cells causing acute graft rejection). In this group, visual acuity was increased in 66.7% of the cases; the state of the epithelium was improved in 66.7% and the quality of life in 100%. Interpretation: These long-term results demonstrate that CAOMECS contains the stem cells necessary for the constant renewal of the epithelium and restores the epithelial function of the cornea by delaying neovascularization and conjunctivalization. For patients with healthy stroma, an increase in visual acuity is possible with no other treatment. For those whose stroma is severely deteriorated, penetrating keratoplasty is then possible and improved visual acuity can be achieved. This study demonstrates that CAOMECS graft appears as an innovative and safe treatment for blindness due to LSCD.