Indexed In
- Open J Gate
- Genamics JournalSeek
- CiteFactor
- Cosmos IF
- Scimago
- Ulrich's Periodicals Directory
- Electronic Journals Library
- RefSeek
- Hamdard University
- EBSCO A-Z
- Directory of Abstract Indexing for Journals
- OCLC- WorldCat
- Proquest Summons
- Scholarsteer
- ROAD
- Virtual Library of Biology (vifabio)
- Publons
- Geneva Foundation for Medical Education and Research
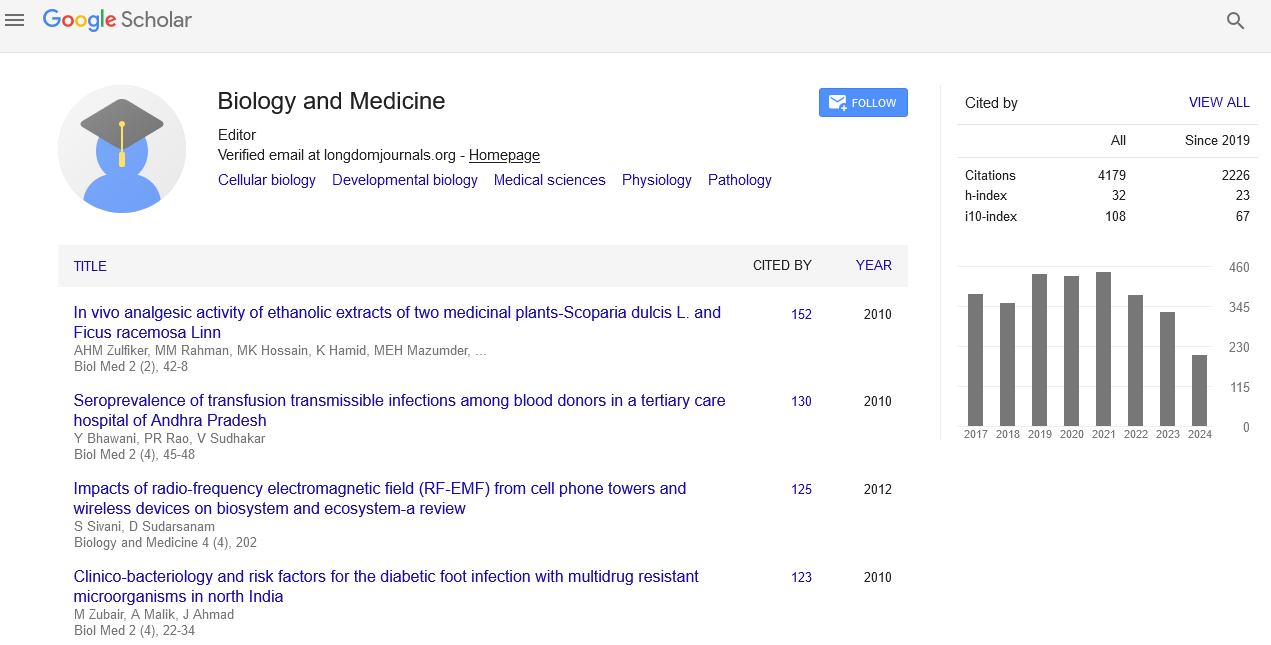
- Google Scholar
Useful Links
Share This Page
Journal Flyer

Open Access Journals
- Agri and Aquaculture
- Biochemistry
- Bioinformatics & Systems Biology
- Business & Management
- Chemistry
- Clinical Sciences
- Engineering
- Food & Nutrition
- General Science
- Genetics & Molecular Biology
- Immunology & Microbiology
- Medical Sciences
- Neuroscience & Psychology
- Nursing & Health Care
- Pharmaceutical Sciences
Abstract
Systemic Inflammation Mediates the Effects of Endotoxemia in the Mechanisms of Heat Stroke
Chin Leong Lim and Katsuhiko Suzuki
Heat stroke is triggered by heat, but is driven by endotoxemia and the downstream effects of systemic inflammation, acute phase response and the pyrogenic response. Whereas heat stroke and its related fatality commonly occur at core temperature (Tc) >40°C, healthy individuals have tolerated Tc 40°C-42°C without symptoms of heat stroke, suggesting that besides hyperthermia, there are other factors that can also cause heat stroke. The “Dual-pathway model (DPM)” suggests that heat stroke is triggered by the endotoxemia pathway at Tc up to ~ 42°C and independently, by heat toxicity at Tc >42°C. The second pathway in the DPM is based on evidence showing that cytoskeletal structures start to disintegrate at ambient temperature >41.5°C. Since most exertional stroke cases occur at Tc <42°C, the endotoxemia pathway, and not heat, might be the primary cause of heat stroke in the active population. Current evidence suggests that exercising under a poor state of health and a compromised immune system may also cause heat stroke, independent from the effects of hyperthermia. Strategies to prevent heat stroke should put equal emphasis on maintaining a good state of health and immune function. The current practice of focusing primarily on heat strain and hydration to prevent heat stroke may not have comprehensively addressed the pathophysiology of heat stroke and may explain why heat stroke continues to occur after more than 2000 years.