Indexed In
- Open J Gate
- Genamics JournalSeek
- Academic Keys
- JournalTOCs
- RefSeek
- Hamdard University
- EBSCO A-Z
- SWB online catalog
- Publons
- Geneva Foundation for Medical Education and Research
- Euro Pub
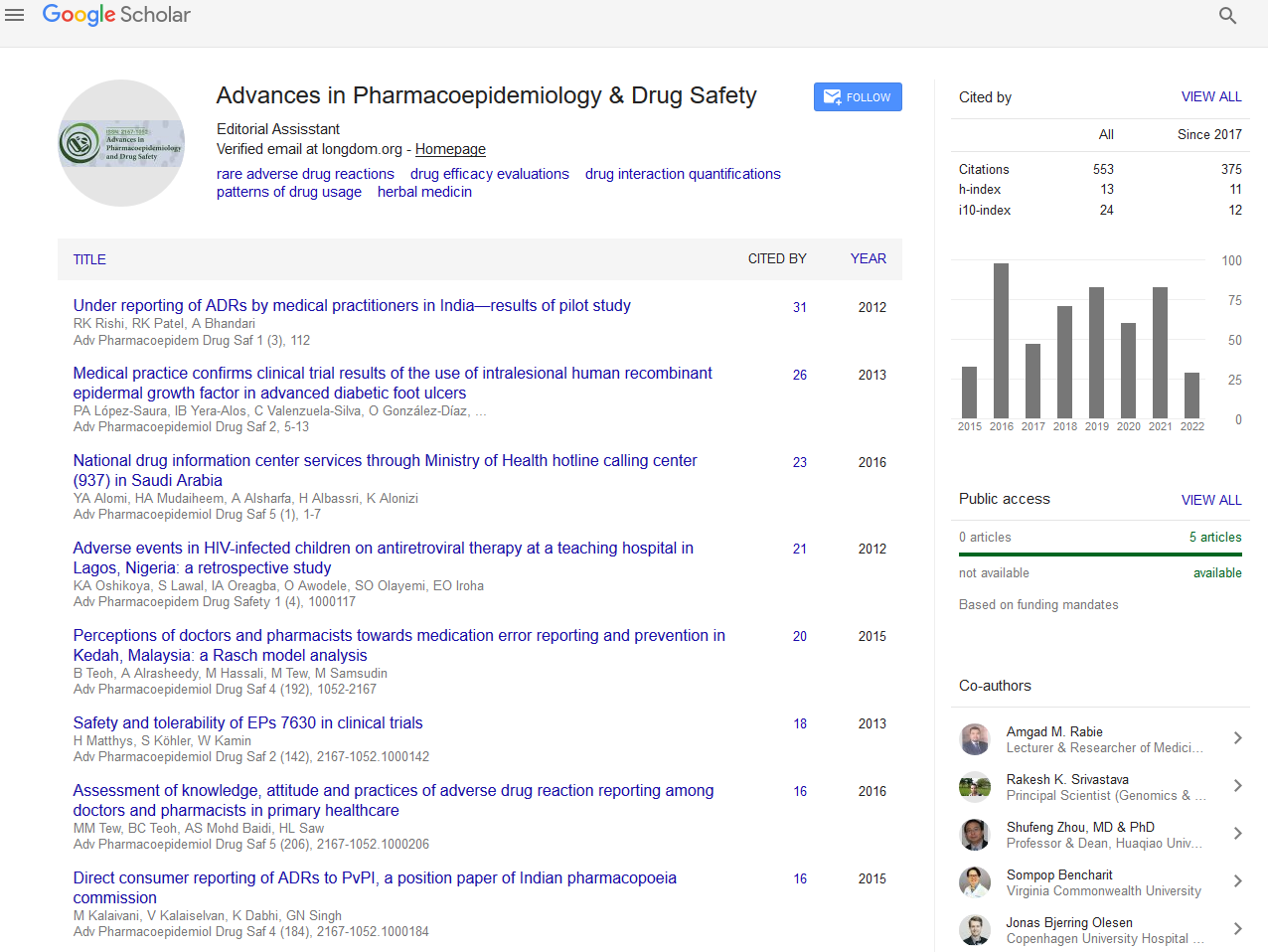
- Google Scholar
Useful Links
Share This Page
Journal Flyer

Open Access Journals
- Agri and Aquaculture
- Biochemistry
- Bioinformatics & Systems Biology
- Business & Management
- Chemistry
- Clinical Sciences
- Engineering
- Food & Nutrition
- General Science
- Genetics & Molecular Biology
- Immunology & Microbiology
- Medical Sciences
- Neuroscience & Psychology
- Nursing & Health Care
- Pharmaceutical Sciences
Abstract
The Effects of Obesity on the Comparative Effectiveness of Linezolid and Vancomycin in Suspected Methicillin-Resistant Staphylococcus aureus Pneumonia
Caffrey AR, Noh E, Morrill HJ and LaPlante KL
Background: Methicillin-Resistant Staphylococcus aureus (MRSA) has become a leading cause of pneumonia in the United States and there is limited data on treatment outcomes in obese patients.We evaluated the effectiveness of linezolid compared to vancomycin for the treatment of MRSA pneumonia in a national cohort of obese Veterans.
Methods: This retrospective cohort study included obese patients (body mass index ≥ 30) admitted to Veterans Affairs hospitals with MRSA-positive respiratory cultures and clinical signs of infection between 2002 and 2012. Patients initiating treatment with either vancomycin or linezolid, but not both, were selected for inclusion. Propensity matching and adjustment of Cox proportional hazards regression models quantified the effect of linezolid compared with vancomycin on time to hospital discharge, intensive care unit discharge, 30-day mortality, inpatient mortality, therapy discontinuation, therapy change, 30-day readmission, and 30-day MRSA reinfection. We performed sensitivity analyses by vancomycin Minimum Inhibitory Concentrations (MICs) and true trough levels.
Results: We identified 101 linezolid and 2,565 vancomycin patients. Balance in baseline characteristics
between the treatment groups was achieved within propensity score quintiles and between propensity matched pairs (76 pairs). No significant differences were observed for the outcomes assessed. Among patients with vancomycin MICs of ≤ 1 μg/mL, the linezolid group had a significantly lower mortality rate, increased length of hospital stay, and longer therapy duration. There were no differences between the linezolid and vancomycin MICs of ≥ 1.5 μg/mL groups. Clinical outcomes among those with vancomycin trough concentrations of 15-20 mg/L were similar to patients treated with linezolid.
Conclusions: In our real-world comparative effectiveness study among obese patients with suspected MRSA pneumonia, linezolid was associated with a significantly lower mortality rate as compared to the vancomycin-treated patients with lower vancomycin MICs. Further studies are needed to determine whether this beneficial effect is observed in other study populations.