Acupuncture Treatment for Allergic Rhinitis: Why should Physicians Recommend it?
Received: 12-Jun-2017 / Accepted Date: 13-Jul-2017 / Published Date: 20-Jul-2017
Abstract
Allergic rhinitis is an IgE-mediated inflammation of the nasal mucosa that is clinically expressed with sneezing, nasal congestion/pruritus and rhinorrhea, in any combination. With nearly 10%-20% of the global population suffering from allergic rhinitis, it is obvious that it affects significantly patient’s quality of life and productivity, as well as imposes a huge economic burden through associated healthcare costs. Current pharmacological treatment (H1- antihistamines, glucocorticosteroids, leukotriene antagonists, decongestants, anticholinergics), as well as allergen immunotherapy, usually fail to achieve complete remission of symptoms or cause treatment-related side-effects. Extensive clinical and experimental investigations over the last decades have shed light on the efficacy, as well as mechanisms of action of acupuncture treatment for allergic rhinitis. We present the available data, to date, which suggest that acupuncture should be part of the treatment algorithm for allergic rhinitis patients.
Keywords: Allergic rhinitis; Rhinorrhea; Acupuncture treatment; Global population
5736Introduction
Allergic rhinitis is an immune-mediated inflammation of the nasal mucosa that is characterized by sneezing, nasal congestion/pruritus and rhinorrhea, in any combination [1]. It can be classified as seasonal allergic rhinitis or persistent allergic rhinitis based on the duration and severity of symptoms. Although it is not a life-threatening condition (unless accompanied by severe asthma or anaphylaxis), associated morbidity can be significant and include: otitis media sleep disturbance, acute/chronic sinusitis, palatal abnormalities and eustachian tube dysfunction [2]. It has been found that nearly 10%-20% of the global population suffers from allergic rhinitis and this affects their quality of life and productivity [3].
Despite recent advances in pharmacological treatment (H1- antihistamines, glucocorticosteroids, leukotriene antagonists, decongestants, anticholinergics), as well as allergen immunotherapy, a large proportion of patients with allergic rhinitis fail to achieve remission of symptoms or present treatment-related side-effects [4,5]. Furthermore, the annual cost of treatment for allergic rhinitis patients exceeds the enormous amount of $1.2 billion in the USA and €1-1.5 billion in Europe, thus it is obvious that there is an unmet need for a more effective and less expensive treatment modality [4].
Acupuncture has been extensively used in China for many centuries and recently in many Western countries as well, for the treatment of a wide range of diseases, including allergic rhinitis. We present the latest available clinical and experimental data regarding acupuncture treatment's efficiency in allergic rhinitis that justify its incorporation into modern medical practice.
Mechanisms of Action
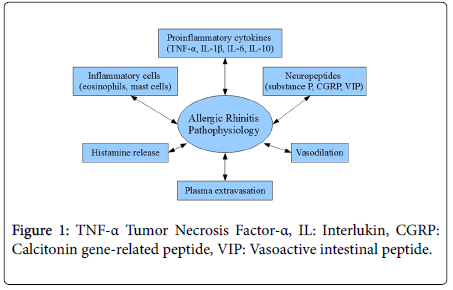
Allergic rhinitis is an IgE-mediated inflammatory response, that involves interaction between inflammatory cells (eosinophils and mast cells), proinflammatory cytokines (such as TNF-α, IL-1β, IL-6, and IL-10) and neuropeptides [like substance P, calcitonin gene-related peptide (CGRP) and vasoactive intestinal peptide (VIP), that induce histamine release, vasodilation and plasma extravasation] Figure 1 [6-8]. Nearly 90% of patients with allergic rhinitis can react, not only to allergens, but also to environmental irritants such as cold air, smoke and perfumes [9].
Acupuncture-induced anti-inflammatory effects are mediated via several physiological pathways, such as the hypothalamus-pituitaryadrenal (HPA) axis, the sympathetic and parasympathetic (cholinergic) pathways, as well as actions on histamine, cytokines (such as TNF-α, IL-1β, IL-6 and IL-10) and neuropeptides (such as substance P, CGRP, and VIP) release Figure 2 [10-19].
Hypothalamus-pituitary-adrenal axis
Electroacupuncture (a more potent form of classical acupuncture) has been shown to significantly increase ACTH and cortisone levels in experimental animal studies of induced inflammation [17,18]. The anti-inflammatory effects of these hormones can be associated with the reduction of nasal congestion in patients with allergic rhinitis via inhibition of mucosal edema [20].
Autonomic nervous system
Sympathetic post-ganglionic neurons, as well as sympathoadrenal medullary axis have also been found to play significant role in edema suppression after electroacupuncture treatment [21].
It has been shown recently that the cholinergic anti-inflammatory pathway (via activation of the vagus nerve) can be activated by acupuncture [19]. Therefore, parasympathetic innervation mediated by acetylcholine (Ach) that binds to α7-nicotinic receptors (α7nAChR), also contributes to acupuncture's anti-inflammatory effects [14,22].
Histamine - IgE
Acupuncture has been found to inhibit histamine-induced symptoms of allergic rhinitis (such as nasal pruritus), possibly through down-regulation of TRPV1 receptors signaling which in turn reduces degranulation of mast cells and thus, histamine release and histamine activation of TRPV1 via H1R [13,23,24]. IgE blood concentration has also been reported to be reduced after acupuncture treatment [25,26].
Cytokines
CD4+ lymphocytes play a key role in mediating allergic rhinitis. Particularly, the alteration of Th1/Th2 cells ratio seems to be of high significance for the development of allergic rhinitis [27-30]. Th1 cells produce cytokines interleukin(IL)-2, IFN-γ and TNF-β that lead to a cellular immune response, while Th2 cells on the other hand, produce IL-4, IL-5, IL-10 and IL-13 that regulate the development of B cells to plasma cells and immunoglobulin E (IgE) production [31,32].
Acupuncture is believed to alter cytokines profile and consequently improve patients' signs and symptoms. It down-regulates Th2 and proinflammatory cytokines such as IL-1, IL-4, IL-6 and IL-10, but also upregulates Th1 cytokines such as IL-2 and IFN-γ [11,20,33,34]. It is noteworthy that not all cytokines are equally affected, with IL-2, IL-10 and IFN-γ expression being predominately altered [11,35,36].
Signal transducer and activator of transcription 6 (STAT6) is involved in the production of interleukin (IL)–4, an important Th2 cytokine in allergic disease [37]. Nuclear factor kappa B (NFkB) is the most important transcription factor in iNOS gene expression [38]. Inducible nitric oxide synthase (iNOS) is involved in nitric oxide production which increases the mucociliary movement of paranasal mucosa [39]. In an experimental mouse model of ovalbumin-induced allergic rhinitis, acupuncture treatment resulted in significant decreases in blood eosinophil count, substance P and activities of STAT6, NFkB, and iNOS, compared to levocetirizine administration (antihistaminic drug) [40].
Neuropeptides-Neurotrophins
Regarding proinflammatory neuropeptides, electroacupuncture was found to significantly decrease substance P and VIP levels, which correlates with clinical improvement in patients with allergic rhinitis [16,40]. Finally, it down-regulates neurotrophins (nerve growth factor - NGF and brain-derived neurotrophic factor - BDNF) which are considered key players of the inflammatory cascade that leads to allergic rhinitis [20,41,42].
Clinical efficacy
A multicenter, randomized controlled study (ACUSAR: Acupuncture in Seasonal Allergic Rhinitis) found statistically significant improvement of allergic rhinitis symptoms and quality of life in patients receiving verum acupuncture compared to conventional symptomatic therapy with antihistamines or “sham” acupuncture [43]. The same results were also found from another multicenter, randomized controlled trial in terms of allergic rhinitis symptoms improvement [44].
In a multicenter, randomized, sham-controlled study four weeks of acupuncture treatment was found to be effective in improving allergic rhinitis symptoms and patients' quality of life [45]. Specifically, it resulted in a statistically significant change in participants’ total nasal symptom score (TNSS), total non-nasal symptom score (TNNSS) and Rhinitis Quality of Life Questionnaire (RQLQ) score (P<0.0001, P=0.0002 and P45]. The RQLQ score evaluates activities, sleep, non-nasal/eye symptoms, practical problems, nasal problems, eye symptoms and emotional function of allergic rhinitis patients. Moreover, acupuncture seems to be a safe treatment modality since no serious adverse effects were observed during this study [45].
Discussion
Current treatment strategy for allergic rhinitis include allergen exposure avoidance, pharmacological treatment (such as antihistamines and intranasal glucocorticosteroids) and immunotherapy [46,47]. However, these treatment modalities are often cost-ineffective, since they usually fail to provide complete symptom remission and they are often associated with several undesirable side effects [46-49].
Recent evidence suggest that acupuncture is an effective and safe treatment modality for allergic rhinitis, when practiced by an experienced acupuncturist, and may even be superior to routine medication [50]. Moreover, the combination of acupuncture and routine medication is associated with statistically beneficial clinical outcome [51].
The efficacy of acupuncture in allergic rhinitis and other allergic diseases, such as asthma or allergic eczema, appears to be due to cytokine profile regulation of Th1/Th2 cells and particularly in the expression of IL-10, IL-2 and IFN-γ [11,35,36]. However, numerous other pathways are also involved, such as the HPA axis, the sympathetic/parasympathetic nervous system and neuropeptides/ neurotrophins alteration.
Conclusion
Given the clinical efficacy and safety of acupuncture treatment, as well as its multiplicity of therapeutic pathways for allergic rhinitis, it should be part of the armamentarium of each physician treating patients with this condition.
Conflicts of Interest
The authors declare that they have no conflicts of interest.
Author Contribution
All authors contributed with manuscript writing.
References
- Druce HM (1998) Allergic and nonallergic rhinitis. Middleton EM Jr, Reed CE, Ellis EF, Adkinson NF Jr, Yunginger JW, Busse WW, eds. Allergy: Principles and Practice. 5th ed. St. Louis, Mo: Mosby Year-Book. 1005-1016.
- Togias AG (2000) Systemic immunologic and inflammatory aspects of allergic rhinitis. J Allergy ClinImmunol 106: S247-250.
- Schoenwetter WF (2000) Allergic rhinitis: epidemiology and natural history. Allergy Asthma Proc 21: 1-6.
- Van Cauwenberge P, Bachert C, Passalacqua G, Bousquet J, Canonica GW, et al. (2000) Consensus statement on the treatment of allergic rhinitis. European Academy of Allergology and Clinical Immunology Allergy 55: 116–134.
- Brozek JL, Bousquet J, Baena-Cagnani CE, Bonini S, Canonica GW, et al. (2010) Allergic Rhinitis and its Impact on Asthma (ARIA) guidelines: 2010 revision. J Allergy ClinImmunol 126: 466-476.
- Lundberg JM, Hokfelt T, Martling CR, Saria A, Cuello C (1984) Substance P–immunoreactive sensory nerves in the lower respiratory tract of various mammals including man. Cell Tissue Res 235: 251-261.
- Hanf G, Schierhorn K, Brunnee T, Noga O, Verges D, et al. (2000) Substance P induced histamine release from nasal mucosa of subjects with and without allergic rhinitis. Inflamm Res 49: 520-523.
- Dykewicz MS, Hamilos DL (2010) Rhinitis and sinusitis. J Allergy Clinical Immuno 125: 103-115.
- Wallace DV, Dykewicz MS, Bernstein DI, Blessing-Moore J, Cox L, et al. (2008) The diagnosis and management of rhinitis: an updated practice parameter. J Allergy ClinImmunol 122: 1-84.
- Ai MK, Guan XM, Zhu CG, Vacca LL (1986) The influence of electroacupuncture and morphine on substance P (SP), enkephalin (ENK) and acetylcholine esterase (AChE) in the spinal cord of rats.Zhen Ci Yan Jiu 11: 96–95.
- Petti FB, Liguori A,Ippoliti F (2002) Study on cytokines IL-2, IL-6, IL-10 in patients of chronic allergic rhinitis treated with acupuncture. J Traditional Chinese Medicine 22: 104-111.
- Pfab F, Hammes M, Bäcker M, Huss-Marp J, Athanasiadis GI, et al. (2005) Preventive effect of acupuncture on histamine-induced itch: a blinded, randomized, placebo-controlled, crossover trial. J Allergy Clinical Immuno 116: 1386-1388.
- Kavoussi B, Ross BE (2007) Theneuroimmune basis of anti-inflammatory acupuncture. Integrative Cancer Therapies6: 251-257.
- Kim HW, Kang SY, Yoon SY, Roh DH, Kwon YB, et al. (2007) Low-frequency electroacupuncture suppresses zymosan-induced peripheral inflammation via activation of sympathetic post-ganglionic neurons. Brain Research 1148:69-75.
- Li YM, Zhuang LX, Lai X, Jiang GH (2007) Effects of electroacupuncture on plasma vasoactive intestinal peptide and substance P in perennial allergic rhinitis patients. Zhen Ci Yan Jiu 32: 136-138.
- Li A, Zhang RX, Wang Y, Zhang H, Ren K, et al. (2007) Corticosterone mediates electroacupuncture-produced anti-edema in a rat model of inflammation. BMC Complementary and Alternative Medicine 7: 1-6.
- Li A, Lao L, Wang Y, Xin J, Ren K, et al. (2008) Electroacupuncture activates corticotrophin-releasing hormone-containing neurons in the paraventricular nucleus of the hypothalammus to alleviate edema in a rat model of inflammation. BMC Complementary and Alternative Medicine 8: 1-8.
- Zogopoulos P, Karavis M, Venetikidis A, Vretakos G, Theocharis S, et al. (2017) Acupuncture- Mediated Activation of the Cholinergic Anti-Inflammatory Pathway- A Review of the Literature. Open Access J Neurol Neurosurg 2: 555-582.
- McDonald JL, Cripps AW, Smith PK, Smith CA, Xue CC, et al. (2013) The Anti-Inflammatory Effects of Acupuncture and Their Relevance to Allergic Rhinitis: A Narrative Review and Proposed Model. Evidence-Based Complementary and Alternative Medicine 591796: 1-12.
- Kim HW, Uh DK, Yoon SY, Roh DH, Kwon YB, et al. (2008) Low-frequency electroacupuncture suppresses carrageenan-induced paw inflammation in mice via sympathetic post-ganglionic neurons, while high-frequency EA suppression is mediated by the sympathoadrenal medullary axis. Brain Research Bulletin 75: 698-705.
- Pavlov VA, Wang H, Czura CJ, Friedman SG, Tracey KJ (2003) The cholinergic anti-inflammatory pathway: a missing link in neuroimmunomodulation. Molecular Medicine 9: 125-134.
- Shim WS, Oh U (2008) Histamine-induced itch and its relationship with pain. Molecular Pain 4: 29.
- Alenmyr L, Högestätt ED, Zygmunt PM, Greiff L (2009) TRPV1-mediated itch in seasonal allergic rhinitis. Allergy 64: 807-810.
- Lau BH, Wong DS, Slater JM (1975) Effect of acupuncture on allergic rhinitis: clinical and laboratory evaluations. Am J Chin Med 3: 263-270.
- Jianli CJ (2006) The effect of acupuncture on serum IgE level in patients with chronic urticaria. Tradit Chin Med 26: 189-190.
- Romagnani S (1998) The Th1/Th2 paradigm and allergic disorders. Allergy 53: 12-15.
- Woodfolk J (2007) T-cell responses to allergens. Allergy Clin Immunol 119: 280-294.
- Annunziato F, Romagnani S (2009) Heterogeneity of human effector CD4+ T cells. Arthritis Res Ther 11: 257.
- Kim SK, Bae H (2010) Acupuncture and immune modulation. Auton Neurosci 157: 38–41.
- Cutler A, Brombacher F (2005) Cytokine therapy. Ann N Y Acad Sci 1056: 16-29.
- Woodfolk JA (2006) Cytokines as a therapeutic target for allergic diseases: a complex picture. Curr Pharm Des 12: 2349-2363.
- Rao YQ, Han NY (2006) Therapeutic effect of acupuncture on allergic rhinitis and its effects on immunologic function. Zhongguo Zhen Jiu26: 557–560.
- Shiue HS, Lee YS, Tsai CN,Hsueh YM, Sheu JR, et al. (2008) DNA microarray analysis of the effect on inflammation in patients treated with acupuncture for allergic rhinitis. Journal of Alternative and Complementary Medicine 14: 689-698.
- Joos S, Schott C, Zou H, Daniel V, Martin E (2000) Immunodulatory effects of acupuncture in the treatment of allergic asthma. J Altern Complement 6: 519-525.
- Hauswald B, Schmidt Ch, Knothe J, Hüttenbrink KB, ZahnertTh (2009) Effects of acupuncture in treatment of perennieal allergic rhinitis in comparison to antihistaminic medication.DtZtschr f Akup 52: 31.
- Tamura K, Arakawa H, Suzuki M, Kobayashi Y, Mochizuki H, et al. (2001) Novel dinucleotide repeat polymorphism in the first exon of the STAT-6 gene is associated with allergic diseases. ClinExp Allergy.31: 1509-1514.
- Xie QW, Kashiwabara Y, Nathan C (1994) Role of transcription factor NF-kappa B/Rel in induction of nitric oxide synthase. J BiolChem 269: 4705-4708.
- Alberty J, August C, Stoll W, Rudack C (2004) The effect of endogenous nitric oxide on cholinergic ciliary stimulation of human nasal mucosa. Laryngoscope 114: 1642-1647.
- Jung D, Lee S, Hong S (2012) Effects of Acupuncture and Moxibustion in a Mouse Model of Allergic Rhinitis. Otolaryngology-Head and Neck Surgery 146: 19-25.
- Sanico AM, Koliatsos VE, Stanisz AM, Bienenstock J, Togias A (1999) Neural hyperresponsiveness and nerve growth factor in allergic rhinitis. Int Arch Allergy Immunol118: 154-158.
- Jin P, AndiappanAK, Quek JM, Lee B, Au B, et al. (2015) A functional brain-derived neurotrophic factor (BDNF) gene variant increases the risk of moderate-to-severe allergic rhinitis. J Allergy Clin Immunol 135:1486-1493.
- Brinkhaus B, Ortiz M, Witt CM, Roll S, Linde K, et al. (2013) Acupuncture in patients with seasonal allergic rhinitis: a randomized trial. Ann Intern Med 158: 225-234.
- Kim JI, Lee MS, Jung SY, Choi JY, Lee S, et al. (2009) Acupuncture for persistent allergic rhinitis: a multi-centre, randomised, controlled trial protocol. Trials 10: 54.
- Choi SM, Park JE, Li SS, Jung H, Zi M, et al. (2013) A multicenter, randomized, controlled trial testing the effects of acupuncture on allergic rhinitis. Allergy 68: 365-374.
- Bousquet J, Khaltaev N, Cruz AA,Denburg J, Fokkens WJ, et al. (2008) Allergic Rhinitis and its Impact on Asthma (ARIA) 2008 update (in collaboration with the World Health Organization, GA (2)LEN and AllerGen). Allergy 63: 8-160.
- Cauwenberge P van, Bachert C, Passalacqua G, Bousquet J, Canonica GW, et al. (2000) Consensus statement on the treatment of allergic rhinitis. European Academy of Allergology and Clinical Immunology. Allergy 55: 116-34.
- Nathan RA (2009) Management of patients with allergic rhinitis and asthma: literature review. South Med J102: 935-941.
- Simoens S (2012) The cost-effectiveness of immunotherapy for respiratory allergy: a review. Allergy 7: 1087-1105.
- Xiao L, Li B, Du YH, Xiong J, Gao X (2009) Systematic evaluation of the randomized controlled trials about acupuncture and moxibustion treatment of allergic rhinitis. Zhongguo Zhen Jiu 29: 512-516.
- Brinkhaus B, Witt CM, Jena S, LieckerB, Wegscheider K, et al. (2008) Acupuncture in patients with allergic rhinitis: a pragmatic randomized trial. Annals of Allergy, Asthma and Immunology 101: 535-543.
Citation: Panagiotis Z, Vasileios G, Anastasios V, Konstantinos S, Georgios V, et al. (2017) Acupuncture Treatment for Allergic Rhinitis: Why should Physicians Recommend it? J Clin Exp Neuroimmunol 2: 113.
Copyright: © 2017 Panagiotis Z, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Usage
- Total views: 6024
- [From(publication date): 0-2017 - Aug 18, 2025]
- Breakdown by view type
- HTML page views: 5047
- PDF downloads: 977