An Unusual Variant of Cerebellopontine Angle Schwannoma in a Young Nepalese Girl
Received: 03-Mar-2017 / Accepted Date: 20-Mar-2017 / Published Date: 24-Mar-2017 DOI: 10.4172/2161-0681.1000307
Abstract
An unusual variant of cerebellopontine angle schwannomas is extremely rare. Histologically, the tumor has atypical changes misleading the diagnosis. We report 20-year-old Nepalese girl from far-eastern community presented with features of raised intracranial pressure and difficulty in walking. MR imaging revealed intensely contrast enhanced well defined huge solid tumor in right cerebellopontine angle region with foci of multiple cystic components. The tumor was displacing the brain stem structures with dilatation of lateral and third ventricles. The altered radiological finding made discrepancy diagnosis. Conventional angiography demonstrated major feeders from the auricular branch of the right external carotid artery. The tumor was embolized with polyvinyl alcohol particles followed by gross total lateral suboccipital excision. Histopathology unit detailed it as ancient schwannoma with pleomorphic changes.
Keywords: Ancient schwannoma; Cerebellopontine angle tumor; Pleomorphism
315631Introduction
Since cerebellopontine angle (CPA) schwannomatous lesion may have the unusual radiological pattern and histopathological alteration resembling malignant degeneration, one would accept uncommon kind called Ancient schwannoma. About 5-10% of all intracranial tumors in adults occupies CPA region and 80% of them are vestibular schwannomas [1]. They are slow growing benign solitary lesions arise 8-12 mm distal to the brain stem, near the porus at the Obersteiner- Redlich junction. They alone constitute 25-40% of head and neck tumors [2]. Several cases of extracranial ancient schwannoma have been reported in English literature [2-5]. However an ancient variant involving CPA is particularly rare and our case presentation is one of them.
Case Report
Herein we report a case of ancient schwannoma of CPA in a 20- year-old young girl from the far eastern community of Nepal. She presented with insidious onset of moderate to severe type of a global headache associated with nausea and vomiting. Symptoms were progressive and worsening. Her mother noted the difficulty in walking in later days. MRI demonstrated intensely contrast enhanced, well defined solid CPA lesion with foci of multiple cystic components measuring 5 cm x 6 cm in size with evidence of brain stem compression and dilatation of ventricular system (Figure 1). Real-time digital subtraction angiography (DSA) of the right external carotid artery (ECA) revealed the presence of rich vascular supply from the posterior auricular artery (PAA). Hence, preoperative tumor embolization was considered. The angiographic catheter 4F (VER 1350 Cordis) was selectively wedged above the origin of the PAA. The tumor was then embolized with polyvinyl alcohol (PVA) particles of size between 150-350 microns (Cook Med Inc.). Postembolization angiography showed no residue filling of arterial supply to the tumor. Intraoperative dissection was easier due to the bloodless surgical field and the tumor was completely excised. Histopathology unit reported it to be ancient schwannoma containing loose sheets of cells with pleomorphic changes (Figure 1).
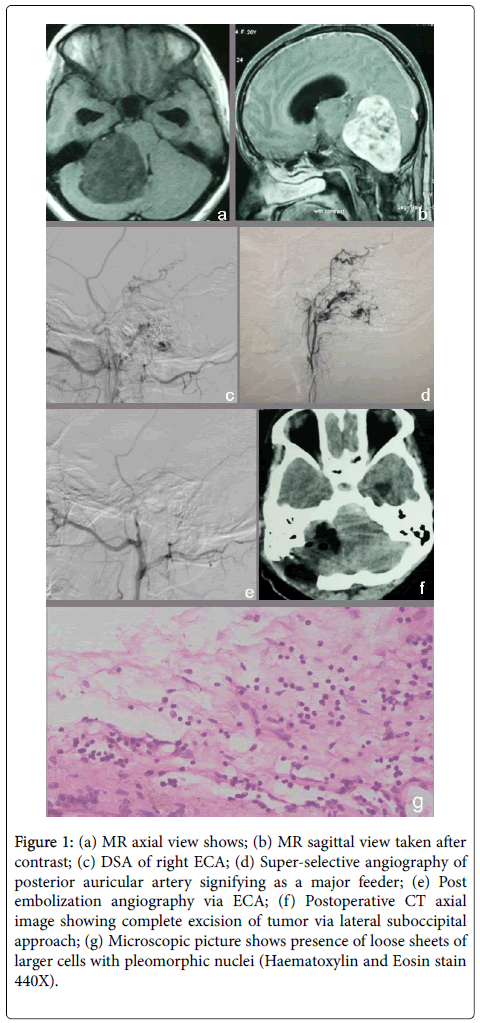
Figure 1: (a) MR axial view shows; (b) MR sagittal view taken after contrast; (c) DSA of right ECA; (d) Super-selective angiography of posterior auricular artery signifying as a major feeder; (e) Post embolization angiography via ECA; (f) Postoperative CT axial image showing complete excision of tumor via lateral suboccipital approach; (g) Microscopic picture shows presence of loose sheets of larger cells with pleomorphic nuclei (Haematoxylin and Eosin stain 440X).
Discussion
The slowly growing tumor protrudes from the internal auditory canal (IAC) into an area behind the temporal bone called the CPA. CPA is the potential space in posterior fossa which is related to the posterior surface of the temporal bone anteriorly, the anterior surface of cerebellum posteriorly, pontine and medullary cisterns medially and inferior border of the pons and cerebellar peduncle superiorly. Trigeminal nerve lies superiorly whereas glossopharyngeal vagus and cranial portion of accessory nerves transverse the cephalic and caudal extent of CPA. Facial and vestibulocochlear nerves cross the central part carrying a thin sheet of the arachnoid layer into the IAC. The anterior inferior cerebellar artery is the major feeder of the CPA and gives rise to the labyrinthine artery for hearing and balance organs. The majority of the tumors arise from the inferior vestibular nerve followed by the superior vestibular nerve. However, cases have been reported about the rare origin from the cochlear and facial nerve as well [6,7]. Tumors may arise in the medial part of the IAC or in the lateral part of the CPA. They usually attain the shape of a pear with its small attachment point to be at IAC. The Larger tumor may compress adjacent nerve producing the symptoms of facial pain or numbness if trigeminal nerve is involved. The patient may present with facial palsy when facial nerve is affected. When brain stem and cerebellum are involved, alteration in blood pressure, respiration, and pulse rate are affected. Cerebellar signs like ataxia, nystagmus or disequilibrium will be more prominent. Typical age at presentation is between 40-60 years with a female preponderance. Patients usually present with sensorineural hearing loss, tinnitus, and vestibular disorder. Otherwise, schwannomas remain asymptomatic till it attains the huge size and produces features of raised intracranial pressure caused by obstructive hydrocephalus or multiple cranial nerve palsies displacing normal brain tissue. Brain structure is usually not invaded by the tumor but pushes the nearby normal brain tissue either up through incisura or down through the foramen magnum producing herniation syndromes. 95% are unilateral in origin whereas 4% are bilateral. In children, bilateral vestibular schwannomas are commonly found in cases of Neurofibromatosis type 2 [8]. Schwannomas can be classified as glandular, plexiform, cellular, epitheloid, melanotic and ancient variant based on histopathological examination [9]. The classic histological finding reflects presence of Antoni A and Antoni B regions. Antoni A region described as densely packed cellular areas containing spindle-shaped nuclei with a tapered end. Verocay bodies and palisading clusters of nuclei may be seen. Antoni B, in contrast, describes as relatively hypocellular with vacuolated areas. Classic vestibular schwannoma does not show degenerative changes and rarely may undergo malignant transformation [9,10]. Ancient schwannoma is notorious for cellular pleomorphism which is a prominent pathological feature and the pathologist may have a misleading report on histological examination [11]. The presence of either fatty or cystic degeneration with foci of hyaline material, thick capsule, infiltration of histiocytes siderophages and hyperchromatism attributed to the long duration of the Schwannomas [4]. Nuclear atypia, xanthomatous change, and fibrosis are additional histopathological findings. The abundance of foamy macrophages, discreet verocay bodies may misdiagnose malignancy [12]. The above longstanding histopathological alteration has yielded the term as “Ancient Schwannoma”.
Surgical excision is the treatment of choice. Microsurgical gross total removal of CPA tumor with preservation of the neurological function is gaining the popularity. Preservation of facial nerve function hearing ability and lower cranial nerves preservation are the main focus of the surgery. Trans-labyrinthine, suboccipital retrosigmoid, and middle fossa approaches are the day to day practice for the total removal of CPA tumors depending upon the neurological presentation. Trans-labyrinthine approach mainly performed in large tumor present with preoperative lack of serviceable hearing. The suboccipital retrosigmoid approach is done for hearing preservation irrespective to the size of the tumor. Middle fossa approach is primarily for those tumors which are limited to the internal auditory canal and preserves hearing functions. Limited access to CPA and temporal lobe retraction are two main disadvantages of this approach [13]. Mortality and morbidity have been reduced grossly in the recent years. CSF leakage, meningitis, postoperative headache, intraoperative vascular accidents, cranial nerve injuries are the main complications [14]. Availability of ultrasonic aspirators, shavers, and fiber lasers make the total excision more promising in reducing the morbidity. Use of endoscope is another innovation for wide visualization of the surgical field and helps to identify the possible CSF leak and decrease the chances of residual tumor. However, sophisticated tools are still lacking in developing couturiers due to limited resources. Most of the complications are the consequences of the inadequate surgical maneuvers ascertaining the vital structures complicated by the tumor [14]. Meticulous surgical excision and postoperative care are always mandatory for gross total removal without complications (Figure 1).
Conclusion
This is a rare case of CPA ancient type of schwannoma arising from the vestibular nerve. Unusual histological variation having a loose sheet of larger cells with foci of degeneration and pleomorphic changes discloses the diagnosis of ancient type.
References
- Moffat DA, Ballagh RH (1995) Rare tumours of the cerebellopontine angle. Clin Oncol 7: 28-41.
- Bindra R, Gupta S, Gupta N, Asotra S, Sharma A (2010) Ancient schwannoma of the neck mimicking soft tissue sarcoma. J Cancer Res Ther 6: 234-235.
- Touati MM, Darouassi Y, Chihani M, Jalil AA, Tourabi K, et al (2015) Malignant schwannoma of the infratemporal fossa: a case report. J Med Case Rep 9: 153.
- Balasubramaniam S, Balasubramanian S, Thirunavukkarasu R (2014) Ancient schwannoma of the infratemporal fossa. Ann Maxillofac Surg 4: 224-226.
- Mortuza S, Esmaeli B, Bell D (2014) Primary intraocular ancient schwannoma: a case report and review of the literature. Head Neck 36: E36-38.
- Kohan D, Downey LL, Lim J, Cohen NL, Elowitz E (1997) Uncommon lesions presenting as tumors of the internal auditory canal and cerebellopontine angle. Am J Otol 18: 386-392.
- Ugokwe K, Nathoo N, Prayson R, Barnett GH (2005) Trigeminal nerve schwannoma with ancient change. Case report and review of the literature. J Neurosurg 102: 1163-1165.
- Stivaros SM, Stemmer-Rachamimov AO, Alston R, Plotkin SR, Nadol JB, et al. (2015) Multiple synchronous sites of origin of vestibular schwannomas in neurofibromatosis Type 2. J Med Genet 52: 557-562.
- Papiez J, Rojiani MV, Rojiani AM (2014) Vascular alterations in schwannoma. Int J Clin Exp Pathol 7: 4032-4038.
- Preuss M, Stein M, Huegens-Penzel M, Kuchelmeister K, Nestler U (2008) Metastatic tumours mimicking vestibular schwannoma. Acta Neurochir (Wien) 150: 915-919.
- Gochhait D, Chatterjee D, Bal A, Dey P (2015) Cerebellopontine angle schwannoma masquerading as a malignant tumour in cytology fluid of cyst. Cytopathology 26: 56-57.
- Dahl I (1977) Ancient neurilemmoma (schwannoma). Acta Pathol Microbiol Scand A 85: 812-818.
- Cardoso AC, Fernandes YB, Ramina R, Borges G (2007) Acoustic neuroma (vestibular schwannoma): surgical results on 240 patients operated on dorsal decubitus position. Arq Neuropsiquiatr 65: 605-609.
- Betka J, Zvěřina E, Balogová Z, Profant O, Skřivan J, et al (2014) Complications of microsurgery of vestibular schwannoma. Biomed Res Int 2014: 315952.
Citation: Karki KT, Koirala S (2017) An Unusual Variant of Cerebellopontine Angle Schwannoma in a Young Nepalese Girl. J Clin Exp Pathol 7:307. DOI: 10.4172/2161-0681.1000307
Copyright: © 2017 Karki KT, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 4664
- [From(publication date): 0-2017 - Aug 29, 2025]
- Breakdown by view type
- HTML page views: 3759
- PDF downloads: 905