Research Article Open Access
Diabetic Foot Ulcer Registry at a Tertiary Care Hospital in Semarang, Indonesia: an Overview of its Clinical Profile and Management Outcome
Tjokorda Gde Dalem Pemayun* and Ridho M Naibaho
Division of Endocrinology, Department of Medicine, Diponegoro University/Dr. Kariadi General Hospital, Semarang, Indonesia
- Corresponding Author:
- Tjokorda Gde Dalem Pemayun
Medical Faculty, Division of Endocrinology
Department of Medicine, Diponegoro University/Dr. Kariadi General Hospital
Dr. Soetomo Street No. 16-18, Semarang 50244, Indonesia
Tel: +62248454873
Fax: +62248454873
E-mail: tjokdalem_smg@yahoo.com
Received Date: June 28, 2016; Accepted Date: August 24, 2016; Published Date: September 01, 2016
Citation: Pemayun TGD, Naibaho RM (2016) Diabetic Foot Ulcer Registry at a Tertiary Care Hospital in Semarang, Indonesia: an Overview of its Clinical Profile and Management Outcome. J Clin Diabetes Pract 1:111.
Copyright: © 2016 Pemayun TGD. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at
Abstract
Aim: To determine the disease burden in terms of clinical profile and management outcome of diabetic foot complication at a tertiary care hospital in a developing country. Material and methods: In this descriptive study, data were collected from the medical record of patients with diabetic foot ulcers (DFU) who were referred to Dr. Kariadi General Hospital from January 2012 to December 2014. The demographic characteristic, type of foot lesion, etiology, clinical complication, isolated microorganism, treatment, and outcome were reviewed. All the data were analyzed using SPSS version 21. Results: As much as 3.7% of our hospital diabetic admission was related to foot problems. All patients had type 2 diabetes with no gender predominance. The mean age was 54.3 ± 8.6 years. Most of them had poor diabetes control and disease duration>5 years. Peripheral neuropathy was found in 72.8% and peripheral arterial disease (PAD) associated with 40.6% of cases. Before hospitalization, the ulcers had already developed for 4.7 ± 2.9 weeks. Infection present invariably in nearly all patients, and gram-negative microorganisms were the most common isolates. More than 70% of ulcers were in Wagner grade ≥ 3 and gangrene was already present in 38.5% of cases. A total of 98 (41.5%) lower extremity amputation (LEA) at various level of the foot were carried out. Mortality rate due to DFU reached 10.7%. Conclusions: A significant number of patients with DFU lead to high LEA rates in our study. Designing a diabetic foot management protocol and initiating a specialized diabetic foot unit of these patients can reduce the associated morbidity and mortality, also improves patient’s overall outcome.
Keywords
Diabetic foot ulcers; Clinical profiles; Outcomes
Introduction
Diabetes mellitus is the most common endocrine disease among adults that affect millions of people around the world. One of the clinical importance of diabetes lies in associated complications that involves many organs, including the diabetic foot [1]. Diabetic foot ulcers (DFU) are common occurrence in clinical practice with the lifetime risk of a patient with diabetes developing an ulcer may be as high as 25% during their lifetime [2]. Diabetic foot tends to numb, ischemic, and deformed, which increased the likelihood to develop an ulcer [3]. An initially trivial amount of trauma may often result in chronic ulcers and become the reason for hospital admission thus entails high cost to the patients [4]. The co-existence of neuropathy, peripheral arterial disease (PAD), and poor glycemic control may favor the development of severe infections and/or foot gangrene, which if not treated properly, can lead to lower extremity amputation (LEA) or even death [3,5]. Therefore, the DFU have a major medical, social, and economic consequences, especially when hospitalization become necessary [6].
In Indonesia, DFU may become more common given the fact that the prevalence of diabetes is predicted to increase 69% in developing countries in the next 20 years [7]. Nevertheless, foot problems received less attention than other diabetic complications and it is not yet a priority of medical service in Indonesia [6,8]. We signify the need for comprehensive descriptive studies on this diabetic complications in developing countries considering its epidemiological transition. Published local studies describing demographic data, clinical and impacting factors in DFU is also relatively few. For this reason, we conducted a review of patients with diabetic foot problems who were admitted to our institution for treatment. This study was design to obtain a real picture from DFU patients which being seen in a tertiary care teaching hospital, in a developing country. Ultimately, this study will become a reference for further improvement of diabetic foot management in our centre and provide a preliminary communication for our future research in the field of diabetic foot.
Material and Methods
This is a retrospective study reviewing the medical records of diabetic patients who admitted to Dr. Kariadi General Hospital with foot problems. Dr. Kariadi General Hospital is a provincial hospital, which also the central referral in Central Java and main teaching hospital of the Medical Faculty of Diponegoro University. Our hospital serves a population of approximately 974,092 inhabitants in the top end of Semarang territory, an area of almost 946.86 km2 [9]. Patients with various diabetic complications are referred to this hospital and many come from other hospitals within and around the city. The study was conducted over a period of 3 years between January 2012 and December 2014 of which the studied population was already referred to our previous publication [10]. Ethical approval for the study protocol was granted from the Research Ethics Committee from Dr. Kariadi General Hospital and Medical Faculty of Diponegoro University prior to the commencement of the study (Number: 269/EC/FK-RSDK/2015).
All patients with diabetes mellitus and foot ulcer were included in the study. We defined a foot ulcer as a full-thickness wound located distal to the level of malleoli in patients with diabetes [10]. For patients with multiple episodes of admission, an ulceration was decent analized whenever the ulcer was a new episode or if any previous has healed. If more than one ulcer was present, the primary ulcer was defined by the ulcer with the largest cross-sectional area. The worst ulcer was chosen as the representative lesion and graded according to Wagner grade [11]. To classify the presence and severity of infection, PEDIS system was used as suggested by the Infectious Disease Society of America [12]. In our hospital, patients with diabetic foot problems were evaluated by a team consisting of endocrinologist, surgeons, infectious disease specialist, microbiologist, nutritionist, rehabilitation specialist, residents and nurses. The protocol of acute DFUs management included off-loading, diagnosis and treatment of infection, assessment of neuropathy and vascular status, treatment of PAD, and regular wound debridement [13].
We are greatly helped by the SIRUS (Sistem Informasi Rumah Sakit) database to provide the medical records number and ICD-10 diagnoses (International Classification of Disease), which has continually received patient’s data over the last 5 years. A diagnosis of diabetes mellitus was defined as at least one record of ICD-10 code E10 for type 1 and E11 for type 2 diabetes. Diabetic foot problems was confirmed by one of the following doctor’s handwritten diagnosis as: “diabetic foot”, “diabetic foot ulcers”, “diabetic foot infections”, or “diabetic foot gangrene”. Data were further extracted on a pro-forma which was constructed in sections to address different aspects of the following information: (1) personal data, (2) diabetes history, (3) laboratory results, (4) diabetes-related complications and comorbidities, (5) diabetic foot investigation, (6) microbiological profile, (7) treatment, and (8) observed outcomes including the specific levels of LEA and in-hospital mortality.
Details of current and past foot disease were recorded, giving attention to pedal pulses, ankle brachial index (ABI) measurement and sensation of the feet. PAD was diagnosed as ABI<0.9 in either leg using a bidirectional hand-held Doppler ultrasound instrument (Huntleigh Diagnostics, Cardiff, UK). In patients with ABI>1.4, the toe/brachial index (TBI) was calculated and PAD was diagnosed as TBI<0.7 in either leg [14]. Peripheral neuropathy was defined as reduced vibration (by 128 Hz tunning fork) or light touch perception evaluated using a 10-g Semmes-Weinstein monofilament (Huntleigh Diagnostics, Cardiff, UK), as previously described [15]. The practice and recording of non-invasive investigations were performed by internal medicine residents. Foot ulcers were then classified as neuropathic, neuroischemic, pure ischemic, or non-classified through detailed history, physical examination and appropriate investigations conducted early or during the hospitalization.
After the medical records within the predetermined period have been reviewed thoroughly, the collected data was first checked manually for its completeness. Thirteen patients left the hospital against medical advice at different stage of treatment. Seventeen patients had refused surgical or vascular intervention in their primary admission. Futhermore, 14 patients refused LEA even they were advised on the risk of progressive infection. Our method is about to use all of the available data to describe the population characteristics [16]. Incomplete data were deleted in pairwise, however, throughout the record were kept to provide a complete epidemiological information such as demographic data, outcomes, microbiological study, level of amputation, and mortality rate. Admission with medical record stated that the patient had self-discharged or refused LEA does not include in the analysis. All the data were analyzed using the Statistical Package for Social Science version 21 [IBM version 21.0; SPSS Inc., Chicago, IL, USA].
Results
There were 232 admissions with DFU involving 189 patients; these concerned 96 males and 93 females. Some patients (n=27) were admitted to hospital more than once for a new lesion. The percentage of diabetic foot admission in our department was 3.7% (232 out of 6,239 admission of diabetes) during 3-year period. The reasons for diabetic foot admission included uncontrolled infection (69.3%), cardiovascular events (9.3%), diabetic ketoacidosis (5.1%), worsening renal function (3.2%), acute critical limb ischemia (2.8%), hypoglycemic coma (2.8%) and others (7.5%).
Majority of the patients was admitted through emergency department, while only 21 patients were admitted through outpatient clinic. The mean length of stay per admission for DFU was 17.8 days (range 5 to 71 days).
Table 1 summarizes the demographic and clinical features of patients. The patients (n=130) had type 2 diabetes mellitus with the age range between 34 and 79 years. The average duration of diabetes was 6.4 years and majority of the patients had diabetes of more than 5 years. The mean HbA1c at the time of admission was 11.3 ± 2.8%. Sixteen patients (12.3%) were newly diagnosed to be diabetes as they were presented to the hospital with an ulcer. The percentage of first foot lesions was 64.6% (n=84) while the rest had history of DFU (35.4%) and previous amputations were reported in 24 (18.5%) of them. The prevalence of diabetic peripheral neuropathy was 72.8% (n=129) and PAD was present in 40.6% (n=72) of patients. Foot ulcers in 19 patients had purely ischemic origin while 53 had neuro-ischemic ulcers. The mean age and duration of diabetes were higher in the neuro-ischemic ulcers, also higher rate of foot gangrene and thus higher LEA rate (Table 2). In 19.6% of cases (n=29), lesion occurred although there was no peripheral neuropathy or PAD.
| Overall | |
| Age (year) | 54.3 ± 8.6 |
| Male/Female (n=189)† | 96/93 |
| Duration of ulcers before admission (week) | 4.7 ± 2.9 |
| History of ulceration, n (%) | 46 (35.4%) |
| Previous amputation, n (%) | 24 (18.5%) |
| Diabetes duration (year) | 6.4 ± 4.9 |
| Newly detected | 16 (12.3%) |
| <1 year | 5 (3.8%) |
| 1– 5 years | 41 (31.5%) |
| 5–10 years | 46 (35.4%) |
| >10 years | 22 (16.9%) |
| Diabetes treatment (n=114) | |
| OHA | 52 (45.6%) |
| Insulin+OHA | 37 (32.5%) |
| Insulin alone | 25 (21.9%) |
| Smoking (n=92) | |
| Never | 77 (59.2%) |
| Ever | 53 (40.8%) |
| Systolic BP (mmHg) | 130.8 ± 23.4 |
| Diastolic BP (mmHg) | 79.7 ± 12.5 |
| BMI (kg/m2) | 22.5 ± 3.6 |
| Hemoglobin (gr/dL) | 9.9 ± 1.7 |
| Leukocytes (×103/µL) | 17.2 ± 8.3 |
| Admission BG (gr/dL) | 359.3 ± 235.9 |
| FPG (gr/dL) | 199.2 ± 81.7 |
| HbA1c (%) | 11.2 ± 2.8 |
| < 7% (good control) | 5 (3.8%) |
| 7.1–8% (fair control) | 16 (12.3%) |
| 8.1–10% (poor control) | 31 (23.8%) |
| >10% (very poor control) | 78 (60%) |
| Serum creatinine (mg/dL) | 1.6 ± 1.4 |
| GFR (mL/min) | 63.0 ± 30.5 |
| Hospital stay (days) | 17.8 ± 10.1 |
| In-hospital mortality‡ | 10.70% |
Table 1: Demographic details and clinical characteristics of DFU patients, n=130.
| Baseline characteristics | Neuropathic ulcers (n=76) | Ischemic ulcers (n=19) | Neuro-ischemic ulcers (n=53) |
|---|---|---|---|
| Age (years), mean | 54.1 ± 7.7 | 56.6 ± 8.9 | 56.6 ± 8.3 |
| BMI (kg/m2), mean | 23.1 ± 3.7 | 22.8 ± 3.6 | 22.2 ± 3.2 |
| Duration of DM (years), mean | 5.9 ± 5.2 | 5.5 ± 4.7 | 6.3 ± 4.5 |
| HbA1c (%), mean | 11.3 ± 2.7 | 9.7 ± 2.6 | 11.1 ± 2.6 |
| Duration of DFU (week), median | 2 (1-11) | 2 (1-9) | 4 (1-12) |
| Previous foot problem, n (%)b | 26 (17.5) | 10 (6.7) | 23 (15.5) |
| Wagner grade ≥ 3, n (%) | 39 (26.3) | 15 (10.1) | 47 (31.7) |
| Foot with gangrene, n (%) | 19 (12.8) | 12 (8.1) | 27 (18.2) |
| LEA rate, n (%) | 31 (20.9) | 12 (8.1) | 36 (24.3) |
| Length of stay (days), median | 14 (5-52) | 16 (6-51) | 17 (5-69) |
Table 2: Characteristics of the hospitalized DFU patients according to DFU type, n=148a.
Common precipitating event of ulcers are shown in Table 3 that include minor trauma, walking barefoot, spontaneous blisters and illfitting shoes.
| Factors | Number of patients | % |
|---|---|---|
| Unknown | 51 | 23.7 |
| Minor trauma | 38 | 17.6 |
| Walking barefoot | 21 | 9.7 |
| Spontaneous blisters | 19 | 8.8 |
| Ill-fitting shoes or sandals | 9 | 4.1 |
| Thermal injury | 7 | 3.2 |
| Complications of amputation stump | 5 | 2.3 |
| Nail puncture | 4 | 1.8 |
| Ingrown nails | 2 | 0.9 |
| Others | 7 | 3.2 |
| Not mentioned | 54 | 25.1 |
| Total | 215 | 100 |
Table 3: Frequency of antecedent contributory factors for the foot ulcer among patients reviewed, n=215.
It was found that 23.7% of patients could not even remember the initiating events of the wound. The enrolled cases were in Wagner grade 0 to 5 with the duration of the ulcer ranged from 1 week to 2 years. In this study, 154 (71.5%) patients were in high grade Wagner, i.e. Wagner grade ≥ 3 (Table 4). The infection status of ulcers was graded using PEDIS system, and accordingly, it was present invariably in nearly all patients (Table 5).
| Wagner Grade | Signs | N | % |
|---|---|---|---|
| 0 | No ulcer in a high-risk foot | 1 | 0.4 |
| 1 | Superficial ulcer involving the full skin thickness | 5 | 2.3 |
| 2 | Deep ulcer penetrating to ligaments/muscle, but no bone involvement or abscess formation | 51 | 23.7 |
| 3 | Deep ulcer with cellulitis or abscess formation, often with osteomyelitis | 71 | 33 |
| 4 | Localized gangrene | 70 | 32.5 |
| 5 | Extensive gangrene involving the whole foot | 13 | 6 |
| Missing data | 4 | 1.8 | |
| Total | 215 | 100 | |
Table 4: Distribution of foot lesion in accordance with Wagner grading system, n=215.
| Grades of infection | N | % | |
|---|---|---|---|
| Grade 1 | No symptoms or signs of infection | 4 | 1.8 |
| Grade 2 | Inflammation of skin/cutaneous tissue only | 32 | 14.8 |
| Grade 3 | Extensive erythema deeper than 2 cms than skin/subcutaneous tissue | 124 | 57.7 |
| Grade 4 | Systemic inflammatory response syndrome | 28 | 13 |
| Missing data | 27 | 12.5 | |
| Total | 215 | 100 | |
Table 5: PEDIS classification of infection, n=215.
Total of 189 specimens were cultured from foot infection and yielded 114 positive cultures. As many as 19 samples were polymicrobial infection with a total 138 isolates recovered that includes 133 bacterial and 5 fungal organisms.
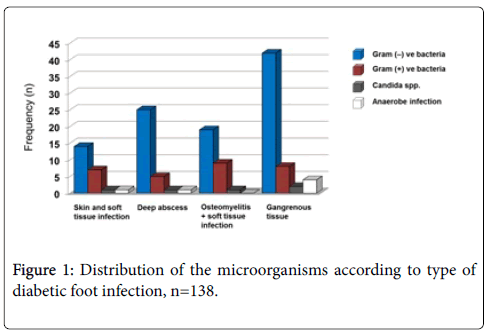
Table 6 gives the distribution of organism isolated from the study population. Among the positive-cultured specimen, gram-negative bacilli constituted the majority (70.8%) and Escherichia coli was the most common isolates. Anaerobic microorganisms constituted to 4.3% of the total isolates. The most commonly isolated anaerobe was Peptostreptococcus spp., and taking the type of lesions into account, maximum isolation of anaerobes was discovered from gangrenous tissue (Figure 1).
| Microorganisms | N | % |
|---|---|---|
| Gram negative | ||
| Escherichia coli | 21 | 15.2 |
| Klebsiella pneumonia | 20 | 14.5 |
| Proteus mirabilis | 18 | 13 |
| Pseudomonas aeruginosa | 13 | 9.4 |
| Enterobacteraerogenes | 10 | 7.2 |
| Acitenobacterbaumanii | 8 | 5.8 |
| Burkholderiacepacia | 4 | 2.9 |
| Morganellamorganii | 2 | 1.4 |
| Providenciastuartii | 1 | 0.7 |
| Enterobacter cloacae | 1 | 0.7 |
| Total | 98 | 70.8 |
| Gram positive | ||
| Staphylococcus aureus | 11 | 7.9 |
| Streptococcus hemolyticus | 7 | 5.1 |
| Streptococcus viridans | 5 | 3.6 |
| Staphylococcus epidermidis | 3 | 2.1 |
| Enterococcus faecalis | 2 | 1.4 |
| Streptococcus pneumoniae | 1 | 0.7 |
| Total | 29 | 20.8 |
| Anaerobic bacteria | ||
| Peptostreptococcus spp. | 4 | 2.9 |
| Fusobacterium spp. | 1 | 0.7 |
| Bacterioides spp. | 1 | 0.7 |
| Total | 6 | 4.3 |
| Fungi | ||
| Candida sp. | 5 | 3.6 |
| Total | 5 | 3.6 |
| Total no. of isolates | 138 | 100 |
Table 6: Distribution of microorganism isolated from diabetic foot infectiona,b.
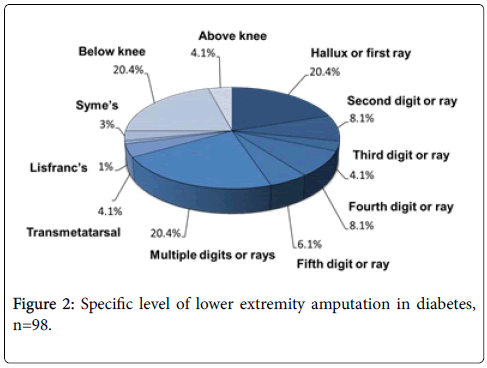
In our series of 189 patients with DFU, an overall amputation rate was 41.5%. Minor LEA was performed in 74 cases. Major LEA was the outcome for 24 patients with four (4.1%) undergoing above-knee and twenty (20.4%) below-knee amputation. Ray-type amputation was performed in two patients (12.5%), transmetatarsal amputation in three patients (18.8%) and Syme’s amputation in two patients (12.5%). Specific levels of all LEA procedure are depicted in Figure 2. Finally, there were 23 deaths among the study sample making the mortality rate of 10.7% and sepsis was the main cause in mortality cases (59%), except 3 cases with sudden cardiac death. Among them who died, seven (30.4%) had grade 3 ulcer, 11 (47.8%) had grade 4 ulcer and 2 (8.7%) had grade 5 ulcer. In this report, 6.0% of the patients with DFU took discharge against medical advice due to variable reasons such as financial constrain, undue delays while awaiting surgical procedure, and refusal of treatment offered, included amputation.
Discussion
Diabetes mellitus is a metabolic disorder characterized with chronic hyperglycemia and target organ damage [1]. In Indonesia, large population of citizens are affected by diabetes and the number of patients with diabetic foot problems is also high [6,8]. Our study documented a 3.7% prevalence rate of foot ulcers among consecutive, unselected diabetic patients admitted to the largest medical in-patients service in Semarang city, Indonesia. They present with many different problems, but the most important was foot ulceration with various degree of infection, osteomyelitis, and gangrene. Hospital-based studies from other literature demonstrated that the prevalence of DFU were varied between 4 to 20.4% among individuals with diabetes and may be a reflection of regional variations in diabetes prevalence [17,18]. Though we have not quantified patient bed occupancy as a proportion of total medical admission, diabetic foot complications represents our main workload.
In previous study, the majority of DFU patients are male and the reason was the fact that male are more active in work and more prone to get foot trauma compared to female. In our study, the proportion of male and female were relatively comparable as well as the middle-aged (mean 54.3 ± 8.6 years). The reason may be due to both gender in their productive age were equally active and spent most of their time in farm area or outdoors. Most of Indonesian people also use sandal jepit as footwear which only covers the plantar area of the feet so that the foot remains at risk from external trauma. A potentially precipitating event was identified in most of the cases and 23.7% of patients were unaware of the cause of their ulcers, certainly related to high prevalence of peripheral neuropathy in our studied population. Twenty one patients also mentioned a clear origin for the ulcers of trauma on sharp or hard objects while walking barefoot. This observation illustrated the importance of giving education concerning footwear practice and frequent examination of the feet in diabetic patients.
The present study assumes significance of patients with DFU in tertiary care hospital in the Indonesian context where diabetes is poorly controlled, there was also little awareness for foot care, and significant delay in seeking treatment. The late presentation in most of our cases contributed to ulcers being indolent, get infected or has developed gangrenous tissue were in consonance with other experiences made from several reports in our country [19-21]. The data from this study showed that LEA is a frequent outcome (41.5%) in patients with DFU, which lies within the ranges of reported 39.5% LEA rate in a study from Dr. M. Djamil Hospital in Padang, Indonesia [19]. In the Netherland [22] and England [23], the amputation rates were found to be lower at 15.5% and 16.0%, respectively, related to better preventative measures and standard of care in Europe. The fact that 71.5% of patients in this study presented with Wagner grades 3-, 4-, and 5- was related to the high LEA rates than those who presented with grade 1- or 2- disease. The mortality was also relatively high in this study (10.7%). Reasons for death in both who died pre- and those post-operatively included sepsis, cardiovascular accidents and sudden death.
Now everyone are aware that the scenario of diabetic foot problems in our study is one of the grave concern in terms of disease burden. We have experienced many cases due to people in our teritory possessed some misperception and misinformation regarding diabetes, in particularly about foot care and foot ulcer. Patients in our territory tends to assume that DFUs are usual, or simple, just as usual as wounds in non-diabetics. They usually treat the lesion by themselves first, dried in sunlight exposure, soaked in a hot water, etc., see traditional healers first, then paramedic after the lesion enlarges, and doctors was their last resort. There were reluctancy to visit family doctors, even less to diabetologist, only because they wish to avoid high cost of consultation or just simply as fear of doctors. These makes early stage DFU were rare occasions in doctor’s practice. Diabetes as its primary disease tends to uncontrolled and associated risk factors unmanageable. Nonformal diabetic foot clinic also exist in our city to give low price orientation, however, the providers did not educate the patient. Unfortunately, no objective survey was published and we are truly need for a local study concerning knowledge, practice, behavior and barrier of foot care among diabetic patients in Semarang city and surrounds.
Finally, the most important massage is, that the current situation can be regenerate even we should sought this current situation as a potential room for improvement and about time to put feet first for diabetic patients. It is worth to note that diabetic foot complication represents a public health concern whose solution is first and foremost is prevention [24]. However, we believe that not all lesion can be prevented, often LEA is inevitably offered when DFU becomes gangrenous and life-threatening when they arrived at the hospital. At the level of tertiary hospital care, a corollary to this preventative action is the development of well purposes teamwork and establishing a diabetic foot clinic with well-trained staff [25]. Specialized diabetic foot clinic is our short-term project to develop in the future which not only capable to treat complex lesions but also concerns on preventative measures, to educate all diabetic patients with proper foot care, detection of high-risk foot and early treatment when lesions begin to occur.
Limitations
There were some limitation to the present study, just as there are limitations in retrospective studies using a hospital databases and medical record review [16]. First, a selection bias may exist because physicians or hospital facilities influence the treatment modality. Second, since our study was embedded in daily clinical practice, limitations had to be set with regard to the number and type of data collected, such as size of ulcers and foot deformity for instance. We also present several variables with missing data, as presented in the tables in the text. Lastly, this study is not population-based and represents patients referred to a tertiary care hospital. It has advantage of characterization of the severity of foot ulceration and LEA rates. However, the samples of this study were also relative small and single centre, so it clearly indicates the need for multicentre study to provide the real size of this problem.
Conclusion
Foot ulcers are common in diabetics and pose serious health problems for developing countries. Our center being a tertiary referral center with patients referred who have rather advanced diseases. Trauma was the most common precipitating factors in underlying neuropathic feet that lead to ulceration and yet, there is considerable delay before hospital presentation. Also, there were complexity of factors related to outcome, of which poor glycemic control, infection and PAD are the most important. In the end, LEA is a common outcome of DFU who admitted to our hospital, and also a notable cause of death. Specialized diabetic foot clinic is our short-term project to be established in order to overcome the problem of diabetic foot in our territory. We hope that this study will stimulate further research in diabetic foot field and provide baseline data to guide measures aimed at reducing the burden of diabetic foot complications in Indonesia.
Declaration of conflict interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
This study was supported by a grant from the Semarang Society of Endocrinology (Perkeni cabang Semarang) for publication of this article.
The author(s) received no external financial support for the research and/or authorship of this article.
Acknowledgements
The author(s) are grateful to the staff of the medical records department of Dr. Kariadi General Hospital who assisted in retrieving the patient’s records.
We would like to acknowledge the assistance from dr. Diana Novitasari, Sp. PD, dr. Nurmilawati Amin, Sp. PD, FINASIM and dr. Tania Tedjo Minuljo, Sp. PD for their help in patient’s data collection from medical records.
References
- Palfai TP, Monti PM, Ostafin B, Hutchison K (2000) Effects of nicotine deprivation on alcohol-related information processing and drinking behavior. J Abnorm Psychol 109: 96-105.
- Harrison EL, Hinson RE, McKee SA (2009) Experimenting and daily smokers: episodic patterns of alcohol and cigarette use. Addict Behav 34: 484-486.
- Howell A, Leyro T, Hogan J, Buckner J, Zvolensky M (2010) Anxiety sensitivity, distress tolerance, and discomfort intolerance in relation to coping and conformity motives for alcohol use and alcohol use problems among young adult drinkers. Addictive Behaviors 35:1144-1147.
- Krukowski RA, Solomon LJ, Naud S (2005) Triggers of heavier and lighter cigarette smoking in college students. J Behav Med 28: 335-345.
- Reed MB, Wang R, Shillington AM, Clapp JD, Lange JE (2007) The relationship between alcohol use and cigarette smoking in a sample of undergraduate college students. Addictive Behaviors 32: 449-464.
- Hughes JR, Kalman D (2006) Do smokers with alcohol problems has more difficulty quitting? Drug Alcohol Depend 82: 91-102.
- Hurt RD, Offord KP, Croghan IT, Gomez-Dahl L, Kottke TE, et al. (1996) Mortality following inpatient addictions treatment: Role of tobacco use in a community-based cohort. JAMA: Journal of the American Medical Association 275: 1097-1103.
- Lisha NE, Carmody TP2, Humfleet GL2, Delucchi KL2 (2014) Reciprocal effects of alcohol and nicotine in smoking cessation treatment studies. Addict Behav 39: 637-643.
- Taylor B, Rehm J (2006) When risk factors combine: The interaction between alcohol and smoking for aerodigestive cancer, coronary heart disease, and traffic and fire injury. Addictive Behaviors 31: 1522-1535.
- Jarvis CM, Hayman LL, Braun LT, Schwertz DW, Ferrans CE, et al. (2007) Cardiovascular risk factors and metabolic syndrome in alcohol- and nicotine-dependent men and women. J CardiovascNurs 22: 429-435.
- Joseph AM, Willenbring ML, Nugent SM, Nelson DB (2004) A randomized trial of concurrent versus delayed smoking intervention for patients in alcohol dependence treatment. Journal of Studies on Alcohol, 65: 681-691.
- Kodl M, Fu SS, Joseph AM (2006) Tobacco cessation treatment for alcohol-dependent smokers: when is the best time? Alcohol Res Health 29: 203-207.
- Fu S, Kodl M, Willenbring M, Nelson D, Nugent S, et al. (2008) Ethnic differences in alcohol treatment outcomes and the effect of concurrent smoking cessation treatment. Drug and Alcohol Dependence 92: 61-68.
- Holt LJ, Litt MD, Cooney NL (2012) Prospective analysis of early lapse to drinking and smoking among individuals in concurrent alcohol and tobacco treatment. Psychology of Addictive Behaviors 26:561-572.
- Centers for Disease Control and Prevention (CDC) (2009) Cigarette smoking among adults and trends in smoking cessation - United States, 2008. MMWR Morb Mortal Wkly Rep 58: 1227-1232.
- Irving LM, Seidner AL, Burling TA, Thomas RG, Brenner GF (1994) Drug and alcohol abuse inpatients' attitudes about smoking cessation. J Subst Abuse 6: 267-278.
- Macnee CL, Talsma A (1995) Development and testing of the barriers to cessation scale. Nurs Res 44: 214-219.
- Orleans CT, Rimer BK, Cristinzio S, Keintz MK, Fleisher L (1991) A national survey of older smokers: treatment needs of a growing population. Health Psychol 10: 343-351.
- Kristeller JL (1994) Treatment of hard-core, high-risk smokers using FDA approved pharmaceutical agents: An oral health team perspective. Health Values 18: 25-32.
- Asher MK, Martin RA, Rohsenow DJ, MacKinnon S, Traficante R, et al. (2003) Perceived barriers to quitting smoking among alcohol dependent patients in treatment. Journal of Substance Abuse Treatment 24: 169-174.
- Martin RA, Rohsenow DJ, MacKinnon SV, Abrams DB, Monti PM (2006) Correlates of motivation to quit smoking among alcohol dependent patients in residential treatment. Drug Alcohol Depend 83: 73-78.
- Marlatt GA, Gordon JR (1985) Relapse prevention. New York: Guilford Press.
- Velicer WF, DiClemente CC, Prochaska JO, Brandenburg N (1985) Decisional balance measure for assessing and predicting smoking status. J PersSoc Psychol 48: 1279-1289.
- DiClemente CC, Prochaska JO (1982) Self-change and therapy change of smoking behavior: a comparison of processes of change in cessation and maintenance. Addict Behav 7: 133-142.
- Curry SJ, Grothaus L, McBride C (1997) Reasons for quitting: intrinsic and extrinsic motivation for smoking cessation in a population-based sample of smokers. Addict Behav 22: 727-739.
- Baha M, Le Faou AL (2010) Smokers' reasons for quitting in an anti-smoking social context. Public Health 124: 225-231.
- Curry SJ, McBride C, Grothaus LC, Louie D, Wagner EH (1995) A randomized trial of self-help materials, personalized feedback, and telephone counseling with nonvolunteer smokers. J Consult Clin Psychol 63: 1005-1014.
- Saunders JB, Aasland OG, Babor TF, de la Fuente JR, Grant M (1993) Development of the Alcohol Use Disorders Identification Test (AUDIT): WHO Collaborative Project on Early Detection of Persons with Harmful Alcohol Consumption--II. Addiction 88: 791-804.
- First MB, Williams JB, Spitzer RL, Gibbon M (2002) Structured Clinical Interview for DSM-IV-TR Axis I Disorders, Clinical Trials Version (SCID-CT). New York: Biometrics Research, New York State Psychiatric Institute.
- Brown RA, Lejuez CW, Kahler CW, Strong DR (2002) Distress tolerance and duration of past smoking cessation attempts. J Abnorm Psychol 111: 180-185.
- Heatherton TF, Kozlowski LT, Frecker RC, Fagerström KO (1991) The Fagerström Test for Nicotine Dependence: a revision of the Fagerström Tolerance Questionnaire. Br J Addict 86: 1119-1127.
- Pomerleau CS, Carton SM, Lutzke ML, Flessland KA, Pomerleau OF (1994) Reliability of the Fagerstrom Tolerance Questionnaire and the Fagerstrom Test for Nicotine Dependence. Addict Behav 19: 33-39.
- Fagerstrom KO, Heatherton TF, Kozlowski LT (1990) Nicotine addiction and its assessment. Ear Nose Throat J 69: 763-765.
- Filbey FM, Claus E, Audette AR, Niculescu M, Banich MT, et al. (2007) Exposure to the taste of alcohol elicits activation of the mesocorticolimbicneurocircuitry. Neuropsychopharmacology 33: 1391-1401.
- Fleming MF, Barry KL, MacDonald R (1991) The alcohol use disorders identification test (AUDIT) in a college sample. Int J Addict 26: 1173-1185.
- Cherpitel CJ (1995) Analysis of cut points for screening instruments for alcohol problems in the emergency room. J Stud Alcohol 56: 695-700.
- Macnee CL, Talsma A (1995) Predictors of progress in smoking cessation. Public Health Nurs 12: 242-248.
- Curry S, Wagner EH, Grothaus LC (1990) Intrinsic and extrinsic motivation for smoking cessation. J Consult Clin Psychol 58: 310-316.
- McBride CM, Pollak KI, Bepler G, Lyna P, Lipkus IM, et al. (2001) Reasons for quitting smoking among low-income African American smokers. Health Psychol 20: 334-340.
- Bonn-Miller MO, Zvolensky MJ (2009) An evaluation of the nature of marijuana use and its motives among young adult active users. Am J Addict 18: 409-416.
- Buckner JD, Zvolensky MJ, Schmidt NB (2012) Cannabis-related impairment and social anxiety: the roles of gender and cannabis use motives. Addict Behav 37: 1294-1297.
- Agrawal A, Budney AJ, Lynskey MT (2012) The co-occurring use and misuse of cannabis and tobacco: a review. Addiction 107: 1221-1233.
- Degenhardt L, Hall W, Lynskey M (2001) The relationship between cannabis use and other substance use in the general population. Drug Alcohol Depend 64: 319-327.
- Cohen J, Cohen P (1983) Applied multiple regression/correlation analysis for the behavioral sciences. Hillsdale, NJ: Lawrence Erlbaum.
- Cohen J, Cohen P, West SG, Aiken LS (2003) Applied multiple regression/correlation analysis for the behavioral sciences (3rd ed.). Mahwah, NJ US: Lawrence Erlbaum Associates Publishers.
- Lipkus IM, Feaganes JR, Green JD, Sedikides C (2001) The Relationship Between Attitudinal Ambivalence and Desire to Quit Smoking Among College Smokers. Journal of Applied Social Psychology, 31: 113-133.
- Wilson SJ, Creswell KG, Sayette MA, Fiez JA (2013) Ambivalence about smoking and cue-elicited neural activity in quitting-motivated smokers faced with an opportunity to smoke. Addict Behav 38: 1541-1549.
- Festinger LA (1957) A theory of cognitive dissonance. Evanston, IL: Row, Peterson.
- Markowitz LJ (2000) Smoker's perceived self-exemption from health risks. Psi Chi Journal of Undergraduate Research 5: 119-124.
- Jamieson P, Romer D (2001)What do young people think they know about the risks of smoking? In P. Slovic (Ed.), Smoking: Risk, perception, and policy (pp. 51-63). Thousand Oaks, CA US: Sage Publications, Inc.
- Schane RE, Glantz SA, Ling PM (2009) Social smoking implications for public health, clinical practice, and intervention research. American Journal of Preventive Medicine 37: 124-131.
- DaniJA, De Biasi M (2001) Cellular mechanisms of nicotine addiction. PharmacolBiochemBehav 70: 439-446.
- Nestler EJ (2005) Is there a common molecular pathway for addiction? Nat Neurosci 8: 1445-1449.
- Ehrman RN, Robbins SJ, Bromwell MA, Lankford ME, Monterosso JR, et al. (2002) Comparing attentional bias to smoking cues in current smokers, former smokers, and non-smokers using a dot-probe task. Drug Alcohol Depend 67: 185-191.
- Kerst WF, Waters AJ (2014)Attentional retraining administered in the field reduces smokers’ attentional bias and craving.
- Wiers RW, Rinck M, Kordts R, Houben K, Strack F (2010) Retraining automatic action-tendencies to approach alcohol in hazardous drinkers. Addiction 105: 279-287.
- Raupach T, West R, Brown J (2013) The most "successful" method for failing to quit smoking is unassisted cessation. Nicotine Tob Res 15: 748-749.
- Korte KJ, Capron DW, Zvolensky M, Schmidt NB (2013) The Fagerström test for nicotine dependence: do revisions in the item scoring enhance the psychometric properties? Addict Behav 38: 1757-1763.
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 19919
- [From(publication date):
September-2016 - Aug 31, 2025] - Breakdown by view type
- HTML page views : 19021
- PDF downloads : 898