DSM-IV, ICD-10 and FTND: Discordant Tobacco Dependence Diagnoses in Adult Smokers
Received: 15-Nov-2010 / Accepted Date: 09-Dec-2010 / Published Date: 10-Dec-2017 DOI: 10.4172/2155-6105.1000105
Abstract
There are several measures that attempt to assess tobacco dependence but the most appropriate measure to use is often unclear. Tobacco dependence was assessed, in Canadian adult smokers of black African descent, with three measures: the Diagnostic and Statistical Manual of Mental Disorders Fourth Edition (DSM-IV), the International Classification of Diseases (ICD-10) and the Fagerström Test for Nicotine Dependence (FTND). The different measures resulted in very different tobacco dependence diagnosis rates: 91% were dependent by DSM-IV, 48% were dependent by ICD-10 and 48% were dependent by FTND (score ≥3). Although ICD-10 and FTND had the same diagnosis rates, they did not identify the same individuals as dependent (i.e., 35% of those dependent by ICD-10 were not dependent by FTND). For exploratory purposes, the dichotomous measures, DSM-IV and ICD-10, were scored as continuous scale measures, DSMC and ICDC. ICDC had the strongest agreement with FTND (ICC=0.76), followed by DSMC with ICDC (ICC=0.28) and DSMC with FTND (ICC=0.19). These exploratory analyses illustrate some limitations and strengths of the DSM-IV, ICD-10 and FTND. Moreover, we illustrate how measurement architecture and population specific variation may contribute to discordant diagnoses.
https://betist.fun https://betlike.fun https://betmatik.fun https://betpark.fun https://bettilt.club https://elexbet.fun https://extrabet.fun https://hepsibahis.fun https://kingbetting.fun https://maksibet.fun https://marsbahis.xyz https://matadorbet.fun https://pulibet.fun https://restbet.fun https://milanobet.fun https://supertotobet.fun https://vevobahis.fun https://imajbet4.com https://maltcasinocu.fun https://sekabetgiris.fun
Keywords: Diagnostic and Statistical Manual of Mental Disorders Fourth Edition (DSM-IV); International Classification of Diseases (ICD-10); Fagerstr?m Test for Nicotine Dependence (FTND); Black African descent; Tobacco dependence
Abbreviations
DSM-IV - Diagnostic and Statistical Manual of Mental Disorders Fourth Edition; ICD-10 - the International Classification of Diseases; FTND - Fagerström Test for Nicotine Dependence; Q - question; C - criterion; CPD - cigarettes per day
Introduction
There are numerous measures that attempt to assess tobacco dependence [1,2]; however, the most appropriate measure to use, given the research question and study population, is often unclear. Among the tobacco research community, substantial work has been done in attempting to create measures that embody the multidimensional and continuous nature of dependence [3-5]. Nonetheless, the most popular measures of tobacco dependence, often dichotomous or unidimensional, are still used in descriptive and clinical studies [1].
As part of a larger study of nicotine pharmacokinetics, pharmacogenetics and smoking in a Canadian urban population of black African descent, we assessed tobacco dependence by three measures. The first was a dichotomous measure based on seven diagnostic criteria found in the Diagnostic and Statistical Manual of Mental Disorders Fourth Edition (DSM-IV) [6]. The second was a dichotomous measure based on six diagnostic criteria found in the International Classification of Diseases Tenth Edition (ICD-10) [7]. The third, the Fagerström Test for Nicotine Dependence (FTND) is a continuous unidimensional measure composed of six questions that specifically pertain to smoking behaviors [8]. Different dependence measures can give discordant diagnosis in the same population [9]; moreover, the same nicotine dependence measure can perform differently depending on the population [10]. We propose that architectural (e.g. the type, wording and scoring of questions) and population specific (e.g. age, ethnicity, or cigarette consumption level) sources of variation contribute to the discordance; and the following exploratory analyses stem from our observation of discordant dependence diagnosis by the DSM-IV, ICD- 10 and FTND. We describe this observation and highlight issues that merit further consideration in the study of tobacco dependence.
Methods
Overview: We conducted a nicotine pharmacokinetics, pharmacogenetics and smoking study in smokers and nonsmokers in an adult population of black African descent. Participants were from a sample of unrelated healthy volunteers recruited by advertisements, radio announcements and posters that were targeted to individuals of African or black Caribbean heritage. Recruitment initially targeted nonsmokers and smokers who averaged at least 10 CPD. However, this requirement was problematic and recruitment was subsequently opened to all smokers who smoked on at least 5 out of 7 days. Qualified subjects were men and nonpregnant women (aged 18-60 years); who (a) were either current smokers or nonsmokers who had tried cigarettes, (b) had at least three grandparents of black African descent, (c) had no known contraindications to the administration of oral nicotine, (d) were not currently using any prescription or non-prescription medications thought to induce or inhibit hepatic enzymes, (e) had good general health and medical history, (f) had the capacity to give written informed consent and (g) were willing to abide by the rules of the study. Participants received 100 Canadian dollars in compensation for their time. Only smokers (=100 cigarettes lifetime and currently smoking at least five days per week; n=77 males, n=60 females) were the subjects of this secondary analysis. The smokers reported consuming a median of eight cigarettes per day (range=0-35); overall, 74% smoked =10 cigarettes per day. The University of Toronto ethics board approved the protocol and the Institutional Review Board Services (Toronto, Canada) approved and monitored the study.
Dependence Measures: Participants were interviewed using the Pharmacogenetics Drug History Questionnaire - a drug history questionnaire used to acquire information on demographics, ethnic admixture, drug use and tobacco dependence as assessed by the DSMIV, ICD-10 and FTND [12]. Individuals were considered tobacco dependent by the DSM-IV if three of seven criteria were met in the same 12-month period [6]. For exploratory purposes and because it allowed better sensitivity in testing relationships, we expressed the DSM-IV as a scale measure and renamed it DSM continuous (DSMC). DSMC was scored as follows. In the DSM-IV, there are seven criteria and 21 questions. Each question has two choices (yes, no). If yes is selected then Q1=1, Q1b=1, Q2=1, Q2a=0.48, Q2b=0.24, Q2c=0.24, either Q3 or Q3a=1, Q3b=0.48, Q4=1, either Q5a or Q5b=1, Q5c=0.48, Q6=1, Q6a=0.48, Q6b=1, Q7=1, Q7a=0.24, Q7b=0.12, Q7c=0.12 and Q8=1. This scoring satisfies the condition that, if any 2 criteria other than Q8 are met, then the score is less than 3, but if any 3 criteria are met, then the score is at least 3. Thus, except for the additional simultaneity requirement of Q8, the dependence diagnosis is met if and only if, the sum is 3 or more. In some cases, when a negative response to one question was a precondition for asking another, both questions were scored identically. The ICD-10 dichotomous diagnosis of dependence is based on the method refined by O'Loughlin and colleagues, where individuals were considered tobacco dependent if three of six criteria are met [13]. The ICD-10 was also expressed as a scale measure and named ICD-10 continuous (ICDC). ICDC was scored as follows. The ICD-10 measure consists of 18 questions, divided into 3 groups of 4 questions and 3 groups of 2 questions. Each question has multiple response choices and is considered positive only if the most extreme positive choice is selected. Scoring for most criteria, where the original diagnostic scoring required at least one positive response, is as follows, 0=no questions positive, 1=1/2 or 1/4 question positive, 1.1=2/4 questions positive, 1.2=3/4 questions positive, 1.3=2/2 or 4/4 questions positive. However, for Criterion 3, where the original diagnostic scoring required two positive responses, the scoring is 0=no questions positive, 0.3=1/4 questions positive, 1=2/4 questions positive, 1.15=3/4 questions positive, 1.3=4/4 questions positive. This scoring satisfies the condition that, if any 2 criteria are met, then the score is less than 3, but if any 3 criteria are met, then the score is at least 3. Thus, the dependence diagnosis is met if and only if, the sum is 3 or more. FTND is a six-item continuous scale of dependence. Scores range from 0 to 10; a score of 0 to 2 indicated low/no dependence, 3 to 5 indicated moderate dependence and 6 to 10 denoted high dependence [8].
Statistical Analyses: The kappa statistic was used to assess agreement between dichotomous dependence measures. Intraclass correlation coefficients were used to assess the agreement between the continuous measures. Statistical analyses were carried out using SPSS software (SPSS for Macintosh, Release 11.0.4 2004. Chicago: SPSS Inc.).
Results
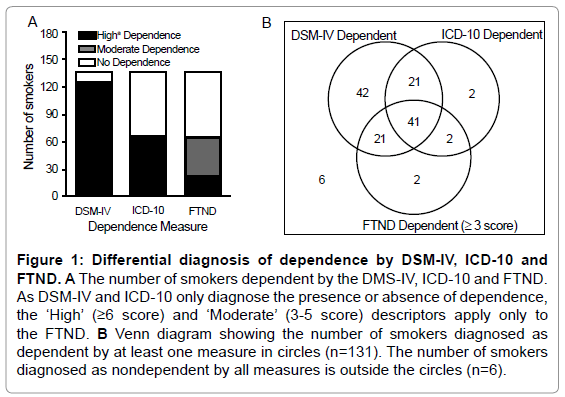
The Interesting Observation of Dependence Diagnosis Discordance: By DSM-IV, 91% of smokers were diagnosed as dependent, while only 48% were diagnosed as dependent by each of the ICD-10 and FTND (Figure 1A). The DSM-IV did not significantly agree (k=0.05, p=0.28) with either the ICD-10 or the FTND. Despite diagnosing the same overall proportion of participants as dependent, the agreement between the ICD-10 and FTND was only fair (k=0.33, p<0.001). (Figure 1B) illustrates the diagnostic discordance between measures.
Architectural Sources of Inter-Instrument Discordance: Five of the twenty DSM-IV questions (25%) are shared with ICD-10. Nine of the eighteen ICD-10 questions (50%) are shared with DSM-IV and two with FTND (11%). Two of the six FTND questions (33%) are shared with ICD-10 (Supplementary Table 2). All continuous dependence measures significantly agreed with each other. The best agreement, as assessed by intra class correlation coefficient (ICC), was between the ICDC and FTND ICC=0.76 (substantial, p<0.001), followed by DSMC and ICDC ICC=0.28 (fair, p<0.001) and DSMC and FTND ICC=0.19 (poor, p=0.002).
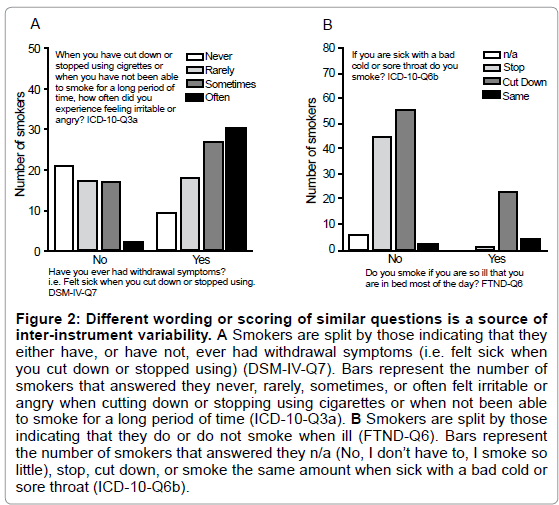
Despite shared criteria and agreement in the assessment of the continuous dependence measures, the construction of the DSM-IV and ICD-10 based measures diverge in important ways. First, questions asked to assess the same criteria differ. For example, to assess tolerance, the DSM-IV and the ICD-10 both ask if more nicotine is required for the same psychoactive effect. The DSM-IV then uniquely asks if the same amount of tobacco results in less psychoactive effect, while the ICD-10 uniquely asks if more tobacco is required to feel negative effects such as nausea. Second, the measures diverge because slightly different wording is used to ask similar questions. For instance, of the 39% of smokers who indicated in DSM-IV that they had never had withdrawal symptoms (i.e. felt sick), 60% answered in ICD-10 that they rarely, sometimes, or often felt irritable or angry when in withdrawal (Figure 2A). Third, divergence between measures occurs at the level of question scoring, when one instrument's graded response is forced to map to another instrument's binary response. For example, both the ICD-10 and the FTND ask about smoking habits when sick. The FTND only allows a yes or no answer, whereas the ICD-10 allows for a range of answers and cutting down the amount smoked is the most highly endorsed answer. The individual does not stop smoking when sick, but neither does the individual smoke as usual, a subtlety that the FTND does not capture (Figure 2A). The design and construction (i.e. the dimensions of dependence assessed, criteria, questions, wording of questions and scoring of questions) all likely contribute to differences between measures.
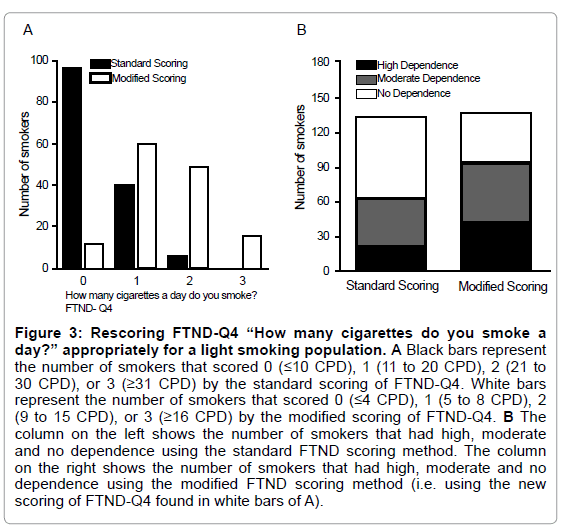
Potential Sources of Inter-Population Variability: On a similar but separate note, the scoring of questions is not always appropriate for the population under investigation. For example, 70% of participants scored zero on FTND-Q4 because they smoked fewer than ten CPD (Figure 3A). We rescored the question to be more reflective of the smoking levels in the population so that cigarette consumption scores formed a quasi-normal distribution (Figure 3A). (Figure 3B) shows the change in the dependence diagnosis with the new scoring is as follows: 31% were highly dependent compared with the original 15%; 38% were moderately dependent compared with the original 34%; and 31% were nondependent compared with the original 52%.
Figure 1: Differential diagnosis of dependence by DSM-IV, ICD-10 and FTND. A The number of smokers dependent by the DMS-IV, ICD-10 and FTND. As DSM-IV and ICD-10 only diagnose the presence or absence of dependence, the ‘High’ (=6 score) and ‘Moderate’ (3-5 score) descriptors apply only to the FTND. B Venn diagram showing the number of smokers diagnosed as dependent by at least one measure in circles (n=131). The number of smokers diagnosed as nondependent by all measures is outside the circles (n=6).
Figure 2: Different wording or scoring of similar questions is a source of inter-instrument variability. A Smokers are split by those indicating that they either have, or have not, ever had withdrawal symptoms (i.e. felt sick when you cut down or stopped using) (DSM-IV-Q7). Bars represent the number of smokers that answered they never, rarely, sometimes, or often felt irritable or angry when cutting down or stopping using cigarettes or when not been able to smoke for a long period of time (ICD-10-Q3a). B Smokers are split by those indicating that they do or do not smoke when ill (FTND-Q6). Bars represent the number of smokers that answered they n/a (No, I don’t have to, I smoke so little), stop, cut down, or smoke the same amount when sick with a bad cold or sore throat (ICD-10-Q6b).
Figure 3: Rescoring FTND-Q4 “How many cigarettes do you smoke a day?” appropriately for a light smoking population. A Black bars represent the number of smokers that scored 0 (=10 CPD), 1 (11 to 20 CPD), 2 (21 to 30 CPD), or 3 (=31 CPD) by the standard scoring of FTND-Q4. White bars represent the number of smokers that scored 0 (=4 CPD), 1 (5 to 8 CPD), 2 (9 to 15 CPD), or 3 (=16 CPD) by the modified scoring of FTND-Q4. B The column on the left shows the number of smokers that had high, moderate and no dependence using the standard FTND scoring method. The column on the right shows the number of smokers that had high, moderate and no dependence using the modified FTND scoring method (i.e. using the new scoring of FTND-Q4 found in white bars of A).
Discussion
This study is important because it illustrates that (a) different tobacco dependence measures do not necessarily diagnose the same individuals as dependent, (b) measure architecture appears to be important to the discordant diagnoses, perhaps more so than the underlying construct of the measure and (c) populations specific factors, like cigarette consumption level, can affect dependence diagnosis. Our findings are from the DSM-IV, ICD-10 and FTND; however, the issues raised could also be relevant to newer multidimensional and continuous tobacco dependence measures.
Continuous Scoring: Our aim in rescoring the DSM-IV and ICD-10 was to take advantage of the underlying continuity of tobacco dependence. Each measure's outcome is artificially dichotomized to dependent and not dependent; this limits the sensitivity in assessing relationships. Our analysis demonstrated that agreement scores between measures improved when the continuous scores were used. Although the new continuous scoring has not been validated, the DSMC and ICDC continuous scores were defined such that scores exceeding a threshold (3 of 7 for DSMC and 3 of 6 ICDC) satisfied the original binary definitions of dependence. Thus, the rankings of dependent individuals were not substantially modified but refined with the conversion of the dichotomous outcome to a continuous score. The DSMC and ICDC may be excellent tools for researchers interested in assessing the continuous nature of dependence.
DSM-IV Dependence: In the DSM-IV, criteria for dependence diagnosis are identical across substances (e.g. alcohol, marijuana, cocaine, tobacco) [6]. A moderate correlation between DSMC and ICDC has also been seen in a study of moderate smokers [14]. The relationship is likely due to similar generic definitions of dependence and content overlap. However, our findings suggest that the specific questions, the wording of questions and the scoring of questions are key sources of discordance between measures even if they are based on similar generic constructs of dependence. As in several other studies [9,14,15]; we found that the DSMC and Fagerström measure were weakly related. The DSM-IV and the FTND had no obvious criterion/question overlap; consistent with the DSM-IV identifying tobacco dependence as a psychological disorder [6], while the FTND focuses on physical tobacco dependence [8]. Despite this, the two measures still have a level of agreement, possibly reflecting a higherorder construct of dependence. Nonetheless, the categorical DSM-IV may lack sensitivity as the large majority of the current study's smokers, despite smoking a median of eight cigarettes per day, were diagnosed as tobacco dependent.
ICD-10 Dependence: The ICD-10 uses "a cluster of behavioral, cognitive and physiological phenomena that develop after repeated substance use" to diagnose a generic dependence syndrome [7]. The ICD-based measure uses questions and concepts from both the DSMIV and FTND as well as capturing the additional dimensions of craving/ compulsion [13]. Mathematically, the ICDC and FTND scores were the most strongly related. This finding differs from a study of heavier smokers, where the measures were not significantly correlated (r=0.32, p>0.05) [14]. The discrepancy may be due to: (a) distinct architecture of measures as Hughes and colleagues developed a different continuous score for the ICD-10 based on the number of criteria endorsed [14]; (b) cigarette consumption because the relationship between tobacco dependence and cigarette consumption seems to be stronger in light smokers compared to heavier smokers [16]; or (c) ethnicity since African American smokers score higher than European American smokers on some dependence dimensions, but lower on others [10]. The ICD-10 appears to have several advantages over the DSM-IV and FTND. First, it allows for a range of answers for each of its questions. Second, it is discriminating as it diagnosed approximately half of the smokers as tobacco dependent. Third, it demonstrates a degree of construct validity in that it correlated with both cigarettes per day and self-perceived addiction (data not shown).
FTND Dependence: Fagerström-based nicotine dependence measures have traditionally been the most widely used by clinicians and researchers in the tobacco field [3]; thus, several studies have compared the agreement of the FTND with alternative measures such as those based on DSM [9,14], ICD [14], the Cigarette Dependence Scale [17,18], the Nicotine Dependence Syndrome Scale [18] and the Hooked on Nicotine Checklist [19]. A disadvantage of the FTND in the current study population is that its scoring may not be appropriate; the basement effect, particularly in the cigarette consumption question, masked population variation. With our rescoring of the FTND, it is not clear if smokers should still be considered dependent if they smoke fewer cigarettes. However, there is a modified Fagerstrom questionnaire for adolescents [20] and modifying the FTND so that it has the capacity to discriminate between levels of dependence in lighter smokers (e.g. splitting the lowest category of <10 CPD into two) may be a valuable addition to the measure. The need for sensitivity to differential levels of nicotine dependence among light smokers has been suggested by others [18].
Caveats: Our ability to generalize these results is tempered by several caveats. First, these are secondary analyses of a nicotine pharmacokinetic and smoking pharmacogenetic study. As such, it has potential selection bias as participants were not sampled randomly but were selected according to eligibility criteria specific to the parent study. Moreover, participating in a full day research study may have introduced self-selection. In addition to the analyses being secondary, the numbers of study participants is small relative to the number of questions in the measures (i.e. 137 participants and 45 questions); thus, our findings must be considered hypothesis generating. Finally, because the study participants are relatively light smokers and are of black African descent, we cannot determine if the discordance between measures is influenced by ethnic specific factors. From the literature, it seems that African Americans score differently on some dimensions of dependence [3], thus ethnicity may be a variable that contributes to the magnitude of discordance we see between measures. Moreover, in a study of relatively heavy smokers the ICD-10 and DSM-IV are highly correlated [14], perhaps suggesting that the discordance between the DSM-IV and the ICD-10 may be due to daily cigarette consumption.
Implications for future tobacco research and practice: There is no gold standard for assessing of tobacco dependence but both the ICD-10 and the DSM-IV are based on similar generic constructs of dependence. The APA has defined dependence as "a maladaptive pattern of substance abuse, leading to clinically significant impairment or distress, as manifested by three (or more) specified criteria, occurring at any time in the same 12-month". A limitation of this definition is it classifies dependence as a dichotomous trait. Complex human traits are influenced by both environmental and genetic factors; consequently, they exhibit phenotypes along a continuum. A strength of the dichotomous DSM-IV and ICD-10 is that they possess content validity because they are based on a definition that recognizes multiple facets of the dependence construct. However, if dependence is a maladaptive harmful pattern of use, then the ability of a continuous measure to predict cessation of may be the most relevant test of validity.
Tobacco dependence questionnaires are often used to identify individuals suitable for inclusion in smoking cessation trials, to distinguish cases in epidemiological investigations, or as an outcome variable. Study participants classified by tobacco dependence using different measures results in practical problems comparing finding across studies and with subpopulation selection. The findings of the present study illustrate some limitations and strengths of the DSM-IV, ICD-10 and FTND in an adult population of black African descent. More generally, it highlights the importance of (a) the type, wording and scoring of the questions in tobacco dependence measures and (b) population specific factors that may confound tobacco dependence assessment. Finally, we have developed continuous scoring methods for the DSM-IV and ICD-10 that can discern ranges of tobacco dependence rather that dichotomous categorization.
Acknowledgements
Funding for this study was provided by the Centre for Addiction and Mental Health, the Canadian Institutes of Health Research (CIHR) MOP-86471, CIHR funded Scholar Program for Interdisciplinary Capacity Enhancement Grant & Tobacco Use in Special Populations awards and a Canada Research Chair in Pharmacogenetics; the funding sources had no further role in study design; in the collection, analysis, an interpretation of data; in the writing of the report; or in the decision to submit the paper for publication. We thank Dr. Howard Kaplan for his thoughtful discussion and development of the DSMC and ICDC scoring methods.
Competing Interests
Dr. RF Tyndale holds shares in Nicogen Research Inc., a company focused on novel smoking cessation treatment approaches. None of the data contained in this manuscript alters or improves any commercial aspect of Nicogen and no Nicogen funds were used in this work.
References
- Piper ME, McCarthy DE, Baker TB (2006) Assessing tobacco dependence: a guide to measure evaluation and selection. Nicotine Tob Res 8: 339-351.
- Colby SM, Tiffany ST, Shiffman S, Niaura RS (2000) Measuring nicotine dependence among youth: a review of available approaches and instruments. Drug and Alcohol Depend 1: S23-39.
- Shiffman S, Waters A, Hickcox M (2004) The nicotine dependence syndrome scale: a multidimensional measure of nicotine dependence. Nicotine Tob Res 6: 327-348.
- Johnson JL, Ratner PA, Tucker RS, Bottorff JL, Zumbo B, et al. (2005) Development of a multidimensional measure of tobacco dependence in adolescence. Addict Behav 30: 501-515.
- Shadel WG, Shiffman S, Niaura R, Nichter M, Abrams DB (2000) Current models of nicotine dependence: what is known and what is needed to advance understanding of tobacco etiology among youth. Drug Alcohol Depend 1: S9-22.
- American Psychiatric Association (1994) Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition. American Psychiatric Association, Washington, DC.
- World Health Organization (1993) The ICD-10 Classification of Mental and Behavioural Disorders: Diagnostic criteria for research. World Health Organization, Geneva, Switzerland.
- Heatherton TF, Kozlowski LT, Frecker RC, Fagerstrom KO (1991) The Fagerstrom Test for Nicotine Dependence: a revision of the Fagerstrom Tolerance Questionnaire. Br J Addict 86: 1119-1127.
- Moolchan ET, Radzius A, Epstein DH, Uhl G, Gorelick DA, et al. (2002) The Fagerstrom Test for Nicotine Dependence and the Diagnostic Interview Schedule: do they diagnose the same smokers? Addict Behav 27: 101-113.
- Schroeder JR, Moolchan ET (2007) Ethnic differences among adolescents seeking smoking cessation treatment: a structural analysis of responses on the Fagerstrom Test for Nicotine Dependence. Nicotine Tob Res 9: 137-145.
- Mwenifumbo JC, Sellers EM, Tyndale RF (2007) Nicotine metabolism and CYP2A6 activity in a population of black African descent: impact of gender and light smoking. Drug and Alcohol Depend 89: 24-33.
- Schoedel KA, Hoffmann EB, Rao Y, Sellers EM, Tyndale RF (2004) Ethnic variation in CYP2A6 and association of genetically slow nicotine metabolism and smoking in adult Caucasians. Pharmacogenetics 14: 615-626.
- O'Loughlin J, DiFranza J, Tarasuk J, Meshefedjian G, McMillan-Davey E, et al. (2002) Assessment of nicotine dependence symptoms in adolescents: a comparison of five indicators. Tob Control 11: 354-360.
- Hughes JR, Oliveto AH, Riggs R, Kenny M, Liguori A, et al. (2004) Concordance of different measures of nicotine dependence: two pilot studies. Addict Behav 29: 1527-1539.
- Breslau N, Johnson EO (2000) Predicting smoking cessation and major depression in nicotine-dependent smokers. Am J Public Health 90: 1122-1127.
- Dierker LC, Donny E, Tiffany S, Colby SM, Perrine N, et al. (2007) The association between cigarette smoking and DSM-IV nicotine dependence among first year college students. Drug and Alcohol Depend 86: 106-114.
- Etter JF (2005) A comparison of the content-, construct- and predictive validity of the cigarette dependence scale and the Fagerstrom test for nicotine dependence. Drug and Alcohol Depend 77: 259-268.
- Okuyemi KS, Pulvers KM, Cox LS, Thomas JL, Kaur H, et al. (2007) Nicotine dependence among African American light smokers: a comparison of three scales. Addict Behav 32: 1989-2002.
- Wellman RJ, DiFranza JR, Savageau JA, Godiwala S, Friedman K, et al. (2005) Measuring adults' loss of autonomy over nicotine use: the Hooked on Nicotine Checklist. Nicotine Tob Res 7: 157-161.
- Prokhorov AV, Pallonen UE, Fava JL, Ding L, Niaura R (1996) Measuring nicotine dependence among high-risk adolescent smokers. Addict Behav 21: 117-27.
Citation: Mwenifumbo JC, Tyndale RF (2010) DSM-IV, ICD-10 and FTND: Discordant Tobacco Dependence Diagnoses in Adult Smokers. J Addict Res Ther 2:105. DOI: 10.4172/2155-6105.1000105
Copyright: © 2010 Mwenifumbo JC, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 20755
- [From(publication date): 12-2011 - Dec 07, 2025]
- Breakdown by view type
- HTML page views: 15760
- PDF downloads: 4995