What is the Safety and Efficacy of Platelet Rich Plasma in Adults Pertaining to Wound Healing and Aesthetic Rejuvenation?
Received: 12-Jul-2017 / Accepted Date: 08-Sep-2017 / Published Date: 20-Sep-2017
Abstract
As per the Cochrane collaboration, a systematic review evaluates and compiles the findings of multiple clinical trials and provides best evidence to address the chosen research question. Conclusion can then be made and future recommendations suggested. Below are the steps in a systematic review as per Cochrane: a. Identify your research question; b. Search for studies; c. Define inclusion and exclusion criteria; d. Extract studies that fulfill the above criteria; e. Perform data analysis of selected studies; f. Evaluate the degree of bias of the above; g. Present findings and assess the quality and level of evidence.
Keywords: Platelet; Chemokines; Implementation; Rejuvenation; Plasma
37761Abbreviation
RCT: Randomized Controlled Trials; PRP: Platelet Rich Plasma; MRI: Magnetic Resonance Imaging; TGF: Transforming Growth Factor
Introduction
Healing of wound is considered as a complex and dynamic process because once a wound begins healing, generally the process resolves with complete wound cessation. Nevertheless, healing of acute and chronic wounds can become impaired by patient factors and/or wound factors. Restarting a wound with impaired healing is difficult as good standard wound care does not always provide an improved healing outcome and often more advanced therapies are employed. Platelet rich plasma (PRP) gel is considered to be advanced wound therapy for chronic and acute wounds. PRP is a highly concentrated autologous solution of plasma prepared from a patient's own blood. PRP contains platelets that are purported to release numerous growth factors that may be valuable in numerous dermatologic applications. For more than 20 years, PRP gel has been used to stimulate wound healing. Autologous PRP gel consists of cytokines, growth factors, chemokines, and a fibrin scaffold derived from a patient's blood. The mechanism of action for PRP gel is thought to be the molecular and cellular induction of normal wound healing responses similar to that seen with platelet activation.
Discussion
Research question
• Target population-Adults, Intervention-Aesthetic rejuvenation and wound healing with platelet-rich-plasma, Outcome(s)-Safety, Efficacy
• ‘What’s the safety and efficacy of platelet rich plasma in adults pertaining to wound healing and aesthetic rejuvenation?’
Search strategy
A comprehensive search of the current literature was undertaken using 3 databases, Cochrane Library, Medline via the PubMed interface, and Google scholar for an extensive review. Search was performed from 2006 to 2016. The search parameters were limited to all English Language articles from 2006 to 2016, excluding animal studies, in vitro studies and articles with no measureable endpoint. The search strategy was designed to select all relevant articles via Mesh terms combined with key text terms to address our research question. Different constructs of search terms were formed by the implementation of truncation of the following terms:
a. PRP wound healing; b. PRP facial rejuvenation; c. PRP plateletrich plasma; d. platelet preparations; e. PRFM platelet-rich fibrin matrix; f. growth factors; g. platelet therapy; h. platelet facial platelet wound healing; i. platelet plastic surgery; j. facial rejuvenation or aesthetic rejuvenation or wound healing.
Search parameters
• Platelet-Rich Plasma [Mesh], last 10 years [PDat], Humans [Mesh], facial rejuvenation or wound healing-552 results on PubMed.
• Safety or efficacy, Platelet-Rich Plasma [Mesh] sort by: Relevance Filters: Published in the last 10 years; Humans-325 results on PubMed.
• Platelet-Rich Plasma [Mesh], last 10 years [PDat], Humans [Mesh], facial rejuvenation or wound healing, last 10 years [PDat], Humans [Mesh] and systematic review or critical review-161 results on PubMed.
• Safety or efficacy, Platelet-Rich Plasma [Mesh], last 10 years [PDat], Humans, systematic review sort by: Relevance Filters: Published in the last 10 years; Humans-102 results on PubMed.
• Safety or efficacy, Platelet-Rich Plasma [Mesh], last 10 years [PDat], Humans [Mesh], systematic review last 10 years [PDat], Humans [Mesh] wound healing sort by: Relevance Filters: Published in the last 10 years; Humans-39 results on PubMed.
• Safety or efficacy, Platelet-Rich Plasma [Mesh] last 10 years [PDat], Humans [Mesh] systematic review, last 10 years [PDat], Humans [Mesh], aesthetic rejuvenation sort by: Relevance Filters: Published in the last 10 years; Humans-0 results on PubMed.
• Platelet rich plasma-9 results on Cochrane.
• Platelet rich plasma, wound healing and facial rejuvenation-1470 results on Google scholar.
• Platelet rich plasma, wound healing or aesthetic rejuvenation-612 results on Google scholar.
• Platelet rich plasma, wound healing and aesthetic rejuvenation-589 results on Google scholar.
Search outcome
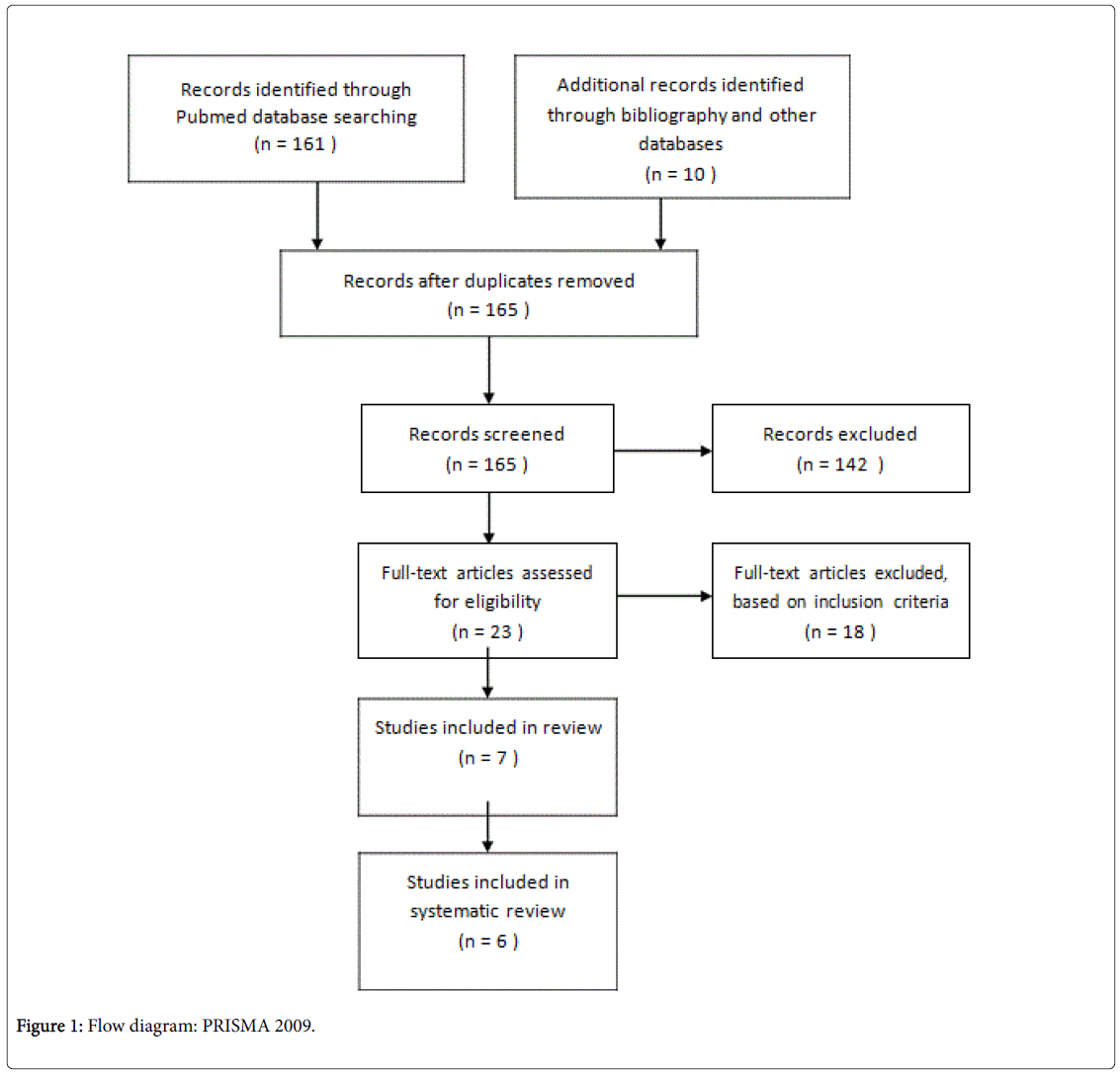
Initial search yielded 552 from PubMed, 9 from Cochrane Library, 1470 from Google Scholar. The search term was refined further to identify relevant articles, adhering to the steps of PRISMA 2009 (Figure 1).
A review of the title and abstract of these papers was undertaken to determine their relevance to our research question, and this then yielded 23 potentially relevant papers. Scanning the references of these papers yielded further studies. Next, an in-depth analysis of these papers was carried out to ascertain the level of evidence, quality and whether they met all of our inclusion and exclusion criteria, 6 systematic reviews and 1 critical review were eventually extracted.
Inclusion criteria
• Adults>19 years old
• Skin rejuvenation or Wound healing
• Timeframe for 2006 to 2016
• English language publications
• Highest quality papers with best evidence, so only level 1 evidence papers
Exclusion criteria
• Animal studies
• In vitro studies
• Articles with no measurable endpoint
Data Analysis
Efficacy
Of the 6 systematic reviews and 1 critical review, 5 evaluated various types of wound healing from post-surgical ulcers, sports related and 2 evaluated aesthetic rejuvenation. Studies varied in design, size and power, hence this lack of uniformity results in complexity in comparison, and poor validity and reproducibility of findings. Reports varied in outcome measures. In wound healing, common parameters used were complete wound healing, wound area reduction, wound depth, healing rate, time to heal, complications, example wound infection, quality of life and pain reduction. As wounds cover a wide spectrum, from medical to post-surgical, and consists of a wide degree of variation, the studies unfortunately did not indicate a detailed description of the type of wounds investigated to correct for inter wound variability.
In aesthetic rejuvenation, common parameters used were subjective doctor and patient evaluation, photo reviews, and objective skin biopsy, trichoscan hair measurements etc. Noting the above variation in outcome measures, findings tend to lack statistical power. Several studies lacked controls, split-face comparisons. Studies were often small scale, with few subjects. There is a high likelihood of publication bias favoring positive results with the use of PRP in both cases, which demonstrated positive effects on cellular changes, wound healing and aesthetic rejuvenation. Many of the studies demonstrated results that were difficult to quantify objectively. PRP treatment protocol lacked standardization for extraction, injection, dosing, and volume. Lack of studies evaluating different forms of PRP and variation in the PRP collection process, leads to difficulty in comparing the study.
Safety
On the aspect of safety, PRP is superior to filler agents, with selflimiting minor side effects of swelling, erythema and bruising as per QMUL module 8 coursework. The above studies have not reported any long term or permanent side effects (Table 1).
| Author and date | Intervention | Sample size | Outcome measure | Evidence level | Weakness |
|---|---|---|---|---|---|
| Martinez et al. [1] | Tissue regeneration | 20 RCTs | Oral and maxillofacial surgery, skin ulcers and surgical wounds. Bone biopsy Gingival index complete epithelialization, TGF-beta edema and ecchymosis via photography. | 1 | 20 quality RCTs found, based on Jadad scale which is outdated. Publication bias as no attempt to look at unpublished data. Results not reproducible. Methodological limitations due to heterogeneity and lack of description. Allocation concealment is questionable in the studies. Little data on safety. Small study size with large confidence intervals. |
| Villela et al. [2] | Diabetic Ulcer | 18 studies | Number of healed ulcers. | 1 | Research question was too broad. Eligibility criteria were not defined. Heterogeneity and methodological flaws, example volume of blood used varied from 20 to 240ml. Poor reporting on the review process. Lack of data on the included studies, example intervention, control and treatment regimen. |
| Carter et al. [3] | Wound healing in 3 main types of wounds, acute primary closure, acute secondary closure and chronic wounds. | 24 papers ( 21 clinical studies and 3 systematic reviews) | PRP can positively impact wound healing, pain and infection in both acute and chronic cutaneous cases. Complete wound healing, superficial infection and pain reduction. Wound area reduction, wound depth, healing rate, time to heal, complications, quality of life. | 1 | Wide variation in quality of studies and a risk of publication bias. Outcome measures for wound healing were too diverse. |
| Taylor et al. [4] | Tendon and ligament injuries | 13 articles | Constant score, MRI, serum cytokine concentration via Elisa assay. | 1 | From the studies, only 3 were RCTs. Wide variation in the method of collection, preparation, administration amongst the studies. Sample size was small in majority, with limited data and short term follow-up. |
| Wang et al. [5] | PRP for treatment of acute wounds (meta- analysis) | 13 articles | Wound healing time, length of hospital stay, incidence of disturbed wound healing, post traumatic pain, wound infections. Findings: Use of PRP can shorten acute wound healing time and length of hospital stay, reduce the incidence of disturbed wound healing and blood products transfusion and alleviate post-traumatic pain, and wound infections. |
1 | Good statistical analysis with use of wide range of RCTs in the study. Role of publication bias. Wide variation in the method of collection, preparation, administration amongst the studies. |
| Leo et al. [6] | Aesthetic Dermatology | 22 manuscripts | Outcome measure not detailed. Benefit in scar revision, androgenic alopecia, post laser recovery and rejuvenation. | 1 | Bias Results not reproducible. Several studies lack controls, split-face comparisons, To better evaluate PRP efficacy and reduce inter-subject variability. Studies were often small scale, with few subjects. Lack of studies evaluating different forms of PRP and variation in the PRP collection process, which leads to difficulty in comparing studies. |
| Sclafani et al. [7] | Facial rejuvenation and wound healing | 61 reports, divided into in vitro, animal studies and clinical studies. | Varied outcome measures, positive effect on cellular changes, wound healing and facial rejuvenation. | 5 | Limitation: Reports varied widely in measurable endpoints. |
Table 1: Data analysis of safety and efficacy of platelet rich plasma in adults pertaining to wound healing and aesthetic rejuvenation.
Clinical Application
Hence, with reference to the research question, our findings review that results though encouraging, high level evidence and high quality RCTs are still lacking. That said, the evidence for wound healing appears to be more substantial than for aesthetic rejuvenation as seen by the quality, design and number of RCTs.
Conclusion
There is still a wide variation in the types and uses of platelet preparation, with no universal standard. Combination of PRP with other modalities is a big scope for future evaluation, specifically the choice, dosing, sequencing, interval and frequency. Future recommendations would be for large robust RCTs to be conducted; however a suitable split face intervention as a control to Platelet rich plasma has yet to be established. Another challenge would be the fact that pharmaceutical companies would hesitate to fund a trial with no intellectual property rights.
References
- Martinez MJ, Marti A, Sola I, Bolibar I, Angel Exposito J, et al. (2009) Efficacyand safety of the use of autologous plasma rich in platelets for tissue regeneration: A systematic review. J Transfus 49: 44-56.
- Villela DL, Santos VL (2010) Evidence on the use of platelet-rich plasma for diabetic ulcer: A systematic review. Growth Factors 28: 111-116.
- Carter MJ, Fylling CP, Parnell LK (2011) Use of platelet rich plasma gel on wound healing: A systematic reviewand meta-analysis. Eplasty 11: e38.
- Taylor DW, Petrera M, Hendry M, Theodoropoulos JS (2011) A systematic review of the use of platelet-rich plasma in sports medicine as a new treatment for tendonand ligament injuries. Clin J Sport Med 21: 344-352.
- Wang L, Gu Z, Gao C (2014) Platelet-rich plasma for treating acute wounds: A meta-analysis. J Chin Med Assoc 94: 2169-2174.
- Leo MS, Kumar AS, Kirit R, Konathan R, Sivamani RK (2015) Systematic review of the use of platelet-rich plasma in aesthetic dermatology. J Cosmet Dermatol 14: 315-323.
- Sclafani AP, Azzi J (2015) Platelet preparations for use in facial rejuvenationand wound healing: A critical review of current literature. Aesthet Surg J 39: 495-505.
Citation: Chang D (2017) What is the Safety and Efficacy of Platelet Rich Plasma in Adults Pertaining to Wound Healing and Aesthetic Rejuvenation? Cosmetol & Oro Facial Surg 3: 119.
Copyright: © 2017 Chang D. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Open Access Journals
Article Usage
- Total views: 3831
- [From(publication date): 0-2017 - Aug 20, 2025]
- Breakdown by view type
- HTML page views: 2935
- PDF downloads: 896