Zika Virus Encefalitis
Received: 11-Sep-2017 / Accepted Date: 14-Sep-2017 / Published Date: 24-Sep-2017 DOI: 10.4172/2329-6879.1000i101
19363Clinical Image
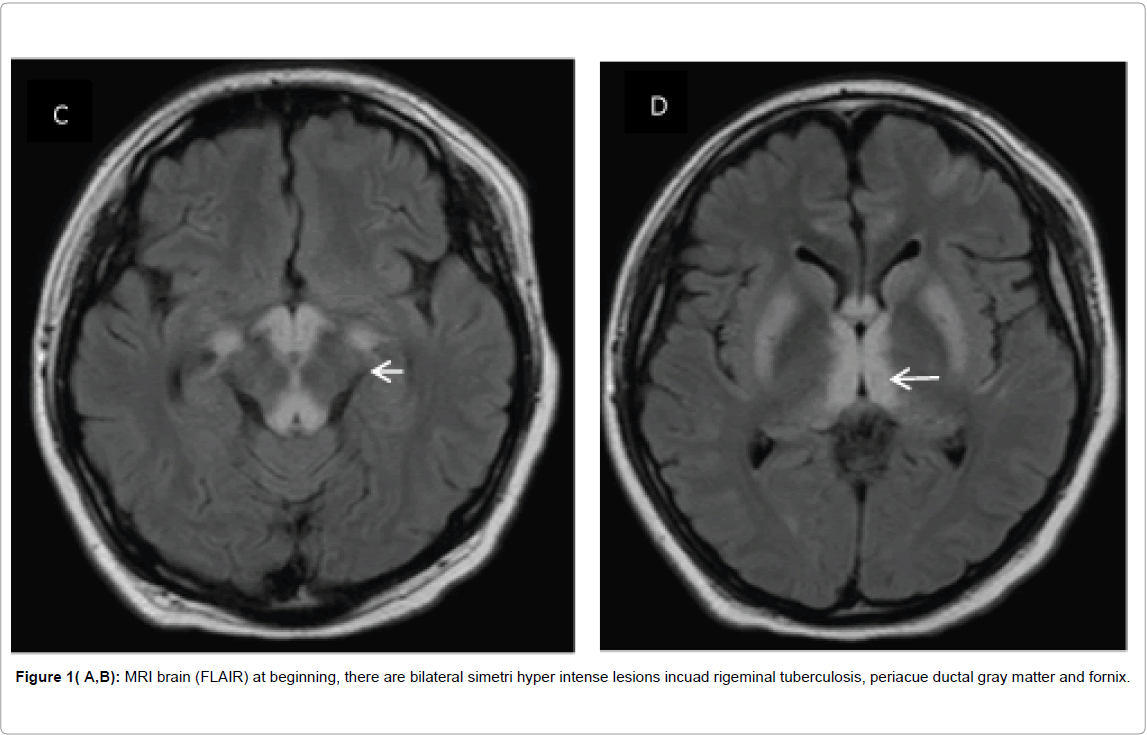
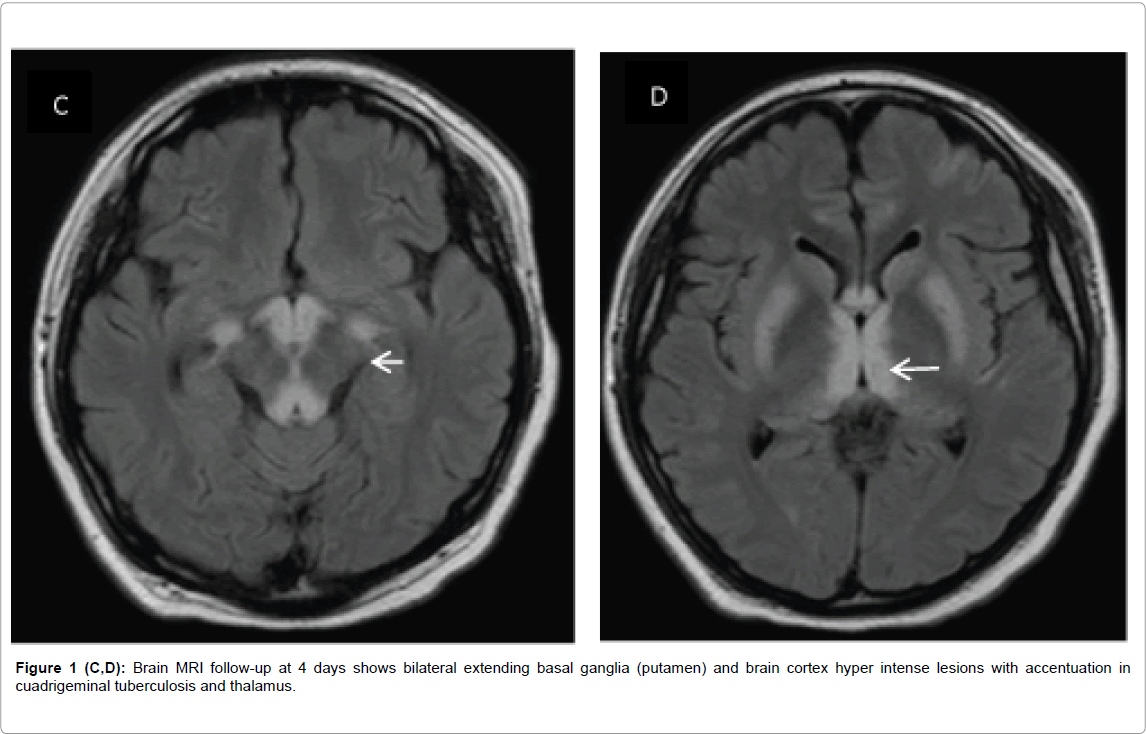
A Male, 23 years old, pancreatitis and cholecystectomy 1 month ago, presented to our ED with a history of 6 days of fever, dizziness and confusion. He reported no headache, neck stiffness or seizures. Physical examination the patient was somnolent, with reactive isochoric pupils, quadriparetic with hyporeflexia. He became stuporous with shock and leukocytosis. Treatment with meropenem and vancomycin were initiated empirically. Magnetic resonance imaging (MRI) of the brain revealed hyper intense lesions in the brain stem, fornix and bilateral thalamus (Figures 1A and 1B) with no midline shift. The CSF analysis results were non-specific with mild protein elevation. CSF molecular biology testing with PCR RNA for Zika virus was positive. A diagnosis of acute disseminated Zika virus encephalitis was made. Immunomodulatory therapy with IVIG was initiated. Follow-up MRI of the brain showed progression of lesions to midbrain, basal ganglia and brain cortex (Figures 1C and 1D). He had no response to 5 days of IVIG therapy and subsequently the patient died.
Citation: González ZL, Vergara CJ, Jáuregui SJ (2017) Zika Virus Encefalitis. Occup Med Health Aff 5: i101. DOI: 10.4172/2329-6879.1000i101
Copyright: © 2017 Luis González Z, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 3682
- [From(publication date): 0-2017 - Aug 29, 2025]
- Breakdown by view type
- HTML page views: 2831
- PDF downloads: 851