Case Report Open Access
Urachal Abscess Clinically Mimicking a Malignancy
Peralta João Pedro1*, Vaz Edgar2, Rabaça Carlos2 and Sismeiro Amilcar21Department of Urology, Portuguese Institute of Oncology of Coimbra, Portugal
2Department of Urology of the Portuguese Institute of Oncology of Coimbra, Faculty of Medicine of the University of Coimbra, Portugal
- *Corresponding Author:
- Peralta Joao Pedro
Department of Urology
Portuguese Institute of Oncology of Coimbra, Portugal
Tel: 351239400263
E-mail: joaopedroperalta@gmail.com
Received date: September 25, 2013; Accepted date: December 20, 2013; Published date: December 23, 2013
Citation: Pedro PJ, Edgar V, Carlos R, Amilcar S (2013) Urachal Abscess Clinically Mimicking a Malignancy. J Clin Exp Pathol 4:154. doi: 10.4172/2161-0681.1000154
Copyright: © 2013 Pedro PJ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Clinical & Experimental Pathology
Introduction
The authors report a case of a 56 year-old patient with smoking habits that was sent for urological consultation due to suspicion of a locally advanced bladder neoplasm. On physical examination he presented with an infra-umbilical mass, with no apparent connection to the supra-pubic area. Complementary imaging showed a considerable, heterogeneous mass, with no separation plan from the anterior abdominal wall or the bladder dome, indicating a differential diagnosis between a locally advanced neoplasm and an urachal tumor. Due to remaining doubts, after pathology results from a trans-urethral biopsy, complete surgical excision was performed and the histological study revealed a chronic inflammatory process, compatible with an urachal abscess.
Background
This report is an evidence of an atypical form of presentation of an urachal abscess, that, that sometimes obscure a serious pathology like urachal carcinoma.
Case Presentation
A 56 year-old patient was referred for urological consultation for a suspected locally advanced bladder neoplasm. He had complained of pain on the infra-umbilical area for about a year, as well as weight loss. There were no micturition complaints.
On physical examination he presented with an infra-umbilical mass, with no apparent connection to the supra-pubic area.
Investigations
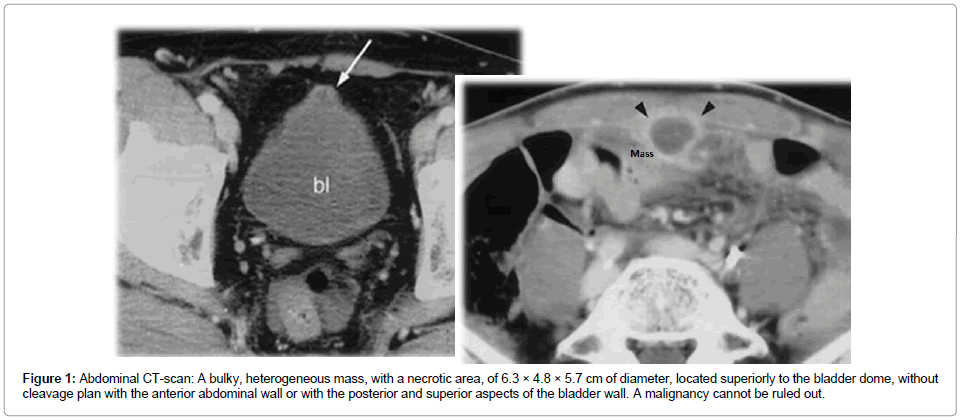
Complementary imaging with abdominal ultrasound and abdominal CT scan (Figure 1) showed a considerable, heterogeneous mass, with no cleavage to the anterior abdominal wall or the bladder dome, indicating a differential diagnosis between a locally advanced neoplasm and an urachal tumour. Cystoscopy showed a solid, hypervascular mass, possibly with local invasion and/or extrinsic compression. Posteriorly, transurethral bladder biopsy showed a follicular cystitis and no signs of atypical urothelial cells.
Figure 1: Abdominal CT-scan: A bulky, heterogeneous mass, with a necrotic area, of 6.3 × 4.8 × 5.7 cm of diameter, located superiorly to the bladder dome, without cleavage plan with the anterior abdominal wall or with the posterior and superior aspects of the bladder wall. A malignancy cannot be ruled out.
Treatment
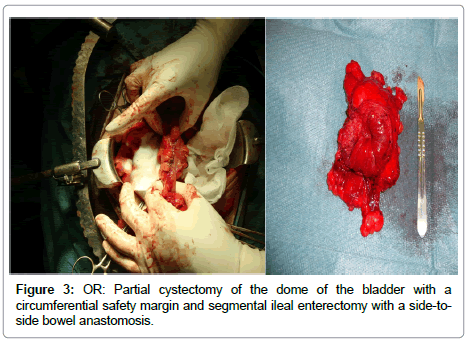
In face of the imaging and pathology results, an exploratory laparotomy was performed, resulting in complete surgical excision: a partial cystectomy of the dome with circumferential safety margin and segmental ileal enterectomy (Figure 2) due to direct local involvement of the intestinal loop, partially compromising intestinal transit.
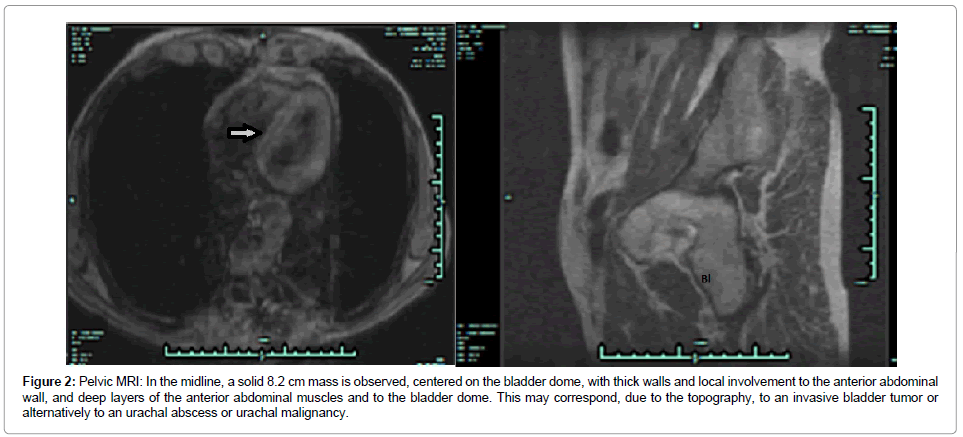
Figure 2: Pelvic MRI: In the midline, a solid 8.2 cm mass is observed, centered on the bladder dome, with thick walls and local involvement to the anterior abdominal wall, and deep layers of the anterior abdominal muscles and to the bladder dome. This may correspond, due to the topography, to an invasive bladder tumor or alternatively to an urachal abscess or urachal malignancy.
Outcome and Follow-up
Pathology report of the surgical piece revealed “a cavity without epithelial lining with necrosis, inflammatory material and abundant pus in adipose tissue around the bladder and outer layer of the detrusor muscle, like a foreign body reaction with granulomas. Combining these results, the TURB pathology and the MRI features observed the aspects are consistent with urachal abscess without signs of malignancy”.
The patient fully recovered, with no new complaints up to this day.
Discussion
Urachal anomalies may be defined as congenital or acquired and are more frequent in children. Congenital anomalies are due to noncomplete obliteration of the canal and may result in patent urachus, urachal cyst, urachus-umbilical sinus or vesicourachal diverticulum [1-3]. On the other hand, malignant degeneracy or infections are more frequent when the anomaly is acquired [4].
Patent urachus accounts for up to 50% of cases in children, usually diagnosed in the neonatal period and due to the reflux from superior side of the bladder. In 30% of cases it may be associated to posterior urethral valves and urethral atresia [5]. In about 30% of cases an urachal cyst is present, consisting of a cystic cavity of the median umbilical ligament, closed off in its umbilical and vesical ends. An infected urachal cyst is the most usual presentation in the adult [2,6,7].
In the urachal sinus, presenting in up to 15% of cases, the apical segment of the urachus remains open and communicates with the umbilicus [8]. A vesicourachal diverticulum is more uncommon (3-5% of cases), which is an incomplete obliteration of the inferior portion of the median umbilical ligament that communicates with the vesical end [9,10]. In most cases these abnormalities are asymptomatic, usually giving off signs when infection befalls due to their remainders becoming overt [11].
The biggest problem with this kind of pathology is its atypical presentation, mimicking different signs and symptoms of seemingly usual urological problems, due to their close relation to neighboring structures, especially the bladder. Because of this and of the diagnostic tests findings, many times these abnormalities fall into the spectrum of urological cancer [12].
Urachal infection usually presents as pain, redness, warmth and purulent exudate, sometimes with clinical and analytical signs of systemic dissemination. The route of infection may be lymphatic, hematogenous or vesical. Thus, the choice of a specific antibiotic may be difficult due to the diversity of involved germs. The site of secretion may vary according to the level and degree of overture of the urachal lumen: the umbilicus in a urachal sinus; the bladder in a vesicourachal diverticulum; or both in a patent urachus. Intra-peritoneal rupture may be a serious complication due to the risk of peritonitis [13-15].
Imagiology demonstrate the complexity of this kind of pathology, because they may not allow for a clear diagnosis, showing solid and cystic components, and not able of distinguishing malignant degeneration. Most times, only pathology findings are able to do so, a posteriori. More so because false negatives are very prevalent in directed percutaneous or transurethral bladder biopsies [16].
The mainstay of treatment is radical surgical excision because of the risk of relapse and the high frequency of malignant transformation with persistent infection [7]. Because of its extraperitoneal location, local and systemic dissemination are common at the time of diagnosis of urachal carcinomas. Benign tumors (adenomas, fibromas, fibromiomas and hamartomas) are rare but almost impossible to differentiate from adenocarcinoma (which accounts for about 0.5% of vesical tumors), so en bloc excision of the suspected mass is usually performed to allow for a full histological analysis. Radical excision usually consists of removal of the urachus in its entire path with a circumferential safety margin guaranteed by a bladder cuff [17,18].
If a benign infected mass is strongly suspected, a two-step surgical approach might be an option consisting, primarily, of a percutaneous drainage with large-spectrum antibiotic coverage and the en bloc excision, secondarily. More and more, however, authors defend an initial two to four weeks course with a systemic large-spectrum antibiotic followed by a one-step deferred surgery, after the acute inflammatory phase, hence minimizing the risks of reinfection [19].
All-in-all, this is a rare kind of pathology, with multiple forms of presentation which may delay diagnosis. Thus, the urologist needs a high degree of suspicion because micturition dysfunction is not always present. On the other hand, because complementary studies also have a low specificity and sensitivity, when neoplastic pathology is involved, the risk of advanced disease at the time of diagnosis is high and rates of survival are low.
Learning Points/Take Home Messages
• Urachal mass are rare in adults.
• High degree of suspicion is suggested for urachal cancer because delay in diagnosis may carry bad prognosis.
Urologist have to be aware that not all patients have urinary complaints, so the diagnosis is harder in daily practice.
References
- Ekwueme KC, Parr NJ (2009) Infected urachal cyst in an adult: a case report and review of the literature. Cases J 2: 6422.
- Yoo KH, Lee SJ, Chang SG (2006) Treatment of infected urachal cysts. Yonsei Med J 47: 423-427.
- Hernandez DM, Matos PP, Hernandez JC, Muñoz JL, Villasana Lde C (2009) Persistence of an infected urachus presenting as acute abdominal pain. Case report. Arch Esp Urol 62: 589-592.
- Suita S, Nagasaki A (1996) Urachal remnants. Semin Pediatr Surg 5: 107-115.
- Risher WH, Sardi A, Bolton J (1990) Urachal abnormalities in adults: the Ochsner experience. South Med J 83: 1036-1039.
- Boothroyd AE, Cudmore RE (1996) Ultrasound of the discharging umbilicus. Pediatr Radiol 26: 362-364.
- Blichert-Toft M, Nielsen OV (1971) Congenital patient urachus and acquired variants. Diagnosis and treatment. Review of the literature and report of five cases. Acta Chir Scand 137: 807-814.
- Berman SM, Tolia BM, Laor E, Reid RE, Schweizerhof SP, et al. (1988) Urachal remnants in adults. Urology 31: 17-21.
- Donate Moreno MJ, Giménez Bachs JM, Salinas Sánchez AS, Lorenzo Romero JG, Segura Martín M, et al. (2005) [Urachal pathology: an overview review and report of three clinical cases]. Actas Urol Esp 29: 332-336.
- Blichert-Toft M, Koch F, Nielsen OV (1973) Anatomic variants of the urachus related to clinical appearance and surgical treatment of urachal lesions. Surg Gynecol Obstet 137: 51-54.
- Yu JS, Kim KW, Lee HJ, Lee YJ, Yoon CS, et al. (2001) Urachal remnant diseases: spectrum of CT and US findings. Radiographics 21: 451-461.
- MacNeily AE, Koleilat N, Kiruluta HG, Homsy YL (1992) Urachal abscesses: protean manifestations, their recognition, and management. Urology 40: 530-535.
- Iuchtman M, Rahav S, Zer M, Mogilner J, Siplovich L (1993) Management of urachal anomalies in children and adults. Urology 42: 426-430.
- Friedland GW, Devries PA, Matilde NM, Cohen R, Rifkin MD (1990) Congenital anomalies of the urinary tract. In: Pollack HM, (ed.) Clinical urography. Saunders, Philadelphia, PA, USA, 559-787.
- Agatstein EH, Stabile BE (1984) Peritonitis due to intraperitoneal perforation of infected urachal cysts. Arch Surg 119: 1269-1273.
- Spataro RF, Davis RS, McLachlan MS, Linke CA, Barbaric ZL (1983) Urachal abnormalities in the adult. Radiology 149: 659-663.
- Goldman IL, Caldamone AA, Gauderer M, Hampel N, Wesselhoeft CW, et al. (1988) Infected urachal cysts: a review of 10 cases. J Urol 140: 375-378.
- Holten I, Lomas F, Mouratidis B, Malecky G, Simpson E (1996) The ultrasonic diagnosis of urachal anomalies. Australas Radiol 40: 2-5.
- McCollum MO, Macneily AE, Blair GK (2003) Surgical implications of urachal remnants: Presentation and management. J Pediatr Surg 38: 798-803.
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 14481
- [From(publication date):
January-2014 - Dec 07, 2025] - Breakdown by view type
- HTML page views : 9817
- PDF downloads : 4664