Case Report Open Access
Case Report: Clozapine Induced Ogilvies Syndrome
Mahmoud Mosli* and Melanie Beaton
London Health Sciences Centre, Department of Medicine, London, Ontario, Canada
- *Corresponding Author:
- Mahmoud Mosli
MBBS, FRCPC, ABIM
London Health Sciences Centre
Department of Medicine, London
Ontario, Canada
E-mail: ma7mos@yahoo.com
Received date: January 02, 2012; Accepted date: March 07, 2012; Published date: March 09, 2012
Citation: Mosli M, Beaton M (2012) Case Report: Clozapine Induced Ogilvie’s Syndrome. J Gastrointest Dig Syst 2:105. doi: 10.4172/2161-069X.1000105
Copyright: © 2011 Mosli M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
We report a case of clozapine induced acute intestinal pseudo obstruction (also known as Ogilvie’s syndrome) in a 54-year female with a history significant for multiple psychiatric disorders. The diagnosis was made after a challenging clinical presentation where collaboration between multiple medical services resulted in reaching a unified diagnosis. The diagnosis was established based on multiple radiological imaging modalities and confirmed by a documented response to colonic decompression through colonoscopy and discontinuation of the offending medication.
Keywords
Oglives’s syndrome; Lithium; Clozapine
Case Report
A 54-year-old female presented to the gastroenterology service through the emergency department (ED) with abdominal pain & diarrhea for 3 weeks. Past medical history was significant for bipolar disorder, Schizophrenia and chronic obstructive pulmonary disease. She was on regular daily Lithium (450 mg/day), clozapine (337.5 mg/day), oxybutynin (10 mg/day), valproic acid (1000 mg/day), and tiotropium bromide (18 mc/day) inhaler. There were no recent changes made to drug dosages and no history of previous abdominal surgeries.
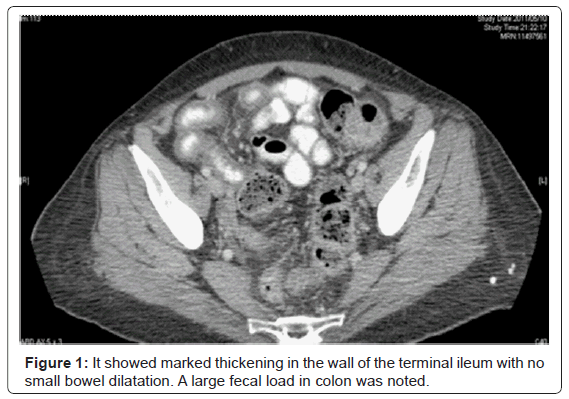
The abdominal pain started suddenly and gradually progressed. It was more in the right lower quadrant, dull in character and intermittent in nature. It was non-radiating and associated with abdominal distention and bloating. The diarrhea was watery, small in amount and occurred up to eight times per day, there was no blood or mucous seen. There were no further gastrointestinal symptoms. History was negative for travel, infectious contacts or antibiotic use. Review of systems was negative apart from chronic fatigue and weakness. Socially, the patient resided at the Regional Mental Hospital (RMH) due to her severe psychiatric disability. On physical examination, the abdomen appeared distended; on palpation there were no signs of peritonitis, bowel sounds heard on auscultation and percussion revealed diffuse tympany. The patient had been seen in the ER 3 weeks earlier for abdominal pain and a CT abdomen was done at that time to rule out appendicitis (Figure 1); it showed marked thickening in the wall of the terminal ileum with no small bowel dilatation. A large fecal load in colon was noted. Infectious work-up was done at that time and was negative and the patient was sent back to RMH.
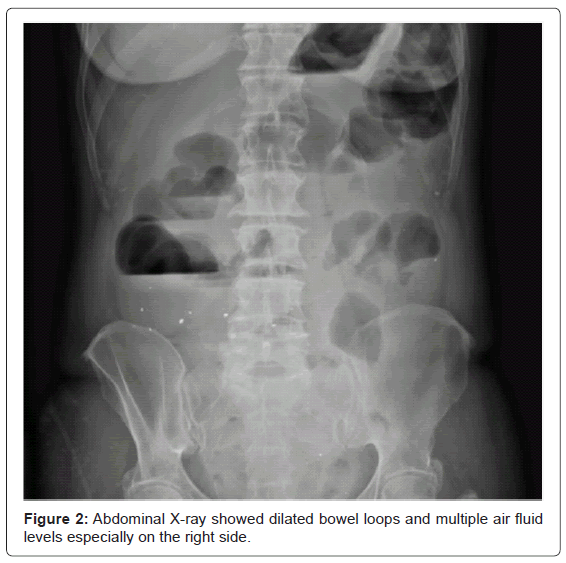
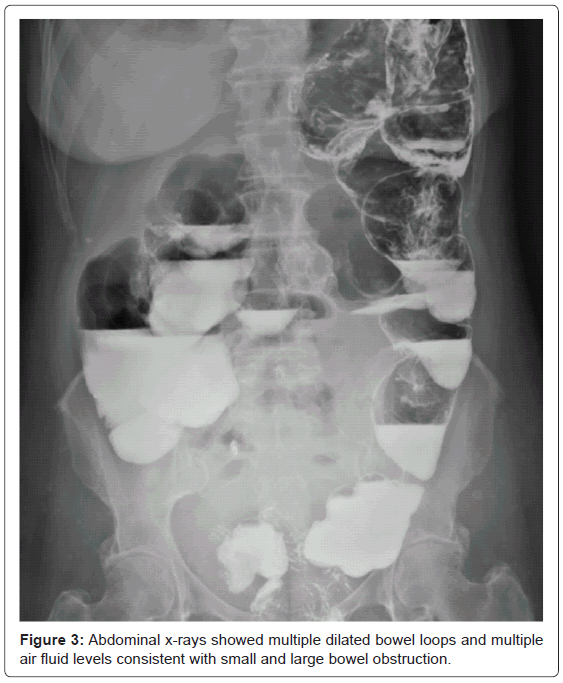
During the current ED visit, investigations were reported as follows, sodium 133, potassium 3.4, chloride 98, HCO3 27, urea 1.6, creatinine 53, WBC 17.2, hemoglobin 132, platelets 389, ESR 2, CRP 17, lactate 2.2, stool for clostridial difficile, cultures and O&P were all negative. Blood cultures were negative. Abdominal X-ray (Figure 2) showed dilated bowel loops and multiple air fluid levels especially on the right side. The general surgery team was consulted; their assessment concluded that the patient had a non-surgical abdomen, unlikely to be mechanically obstructed given the benign physical examination. The patient was admitted and a nasogastric tube was inserted which drained 500 ml of bilious fluid. The patient was kept nil per mouth and a colonoscopy was organized. Abdominal x-rays were repeated (Figure 3) and showed again multiple dilated bowel loops and multiple air fluid levels consistent with small and large bowel obstruction.
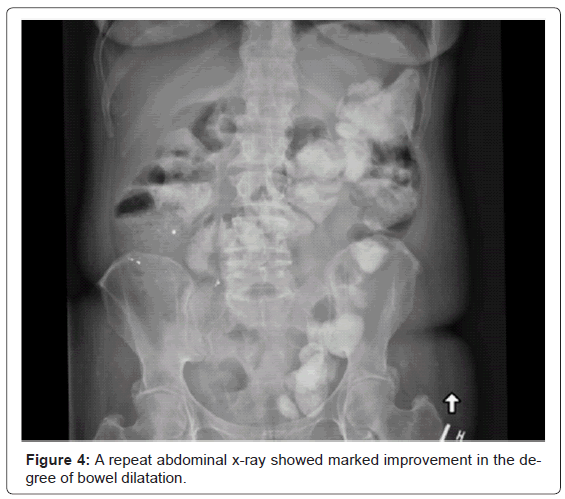
The diagnosis of acute intestinal pseudo obstruction was made after a collaborative discussion between the gastroenterology, radiology and general surgery teams. The patient’s medication list was reviewed with the hospital pharmacist and both clozapine and lithium were suspected. Other secondary causes were excluded. A clozapine level was ordered and found to be critically high at 5950 nm/l, while the lithium level was within the therapeutic range. The decision was made to stop the lithium. The patient’s symptoms resolved and she underwent an uneventful colonoscopy, which revealed normal mucosa throughout the large bowel and terminal ileum. A repeat abdominal x-ray (Figure 4) showed marked improvement in the degree of bowel dilatation. The patient was able to go back to RMH free of any abdominal complaints. A long-term plan regarding her psychiatric illness management was to be arranged by the psychiatry team as an outpatient.
Discussion
Acute intestinal pseudo-obstruction, also known as Ogilvie’s syndrome, is characterized by acute massive colon dilatation involving primarily the right side of the colon and without a mechanical cause [1,2]. It is most often diagnosed in hospitalized, debilitated medical or surgical patients with a wide array of medical conditions [3,4]. A watersoluble contrast enema or CT scan can exclude mechanical obstruction if gas and distention are present throughout all colonic segments, including the rectum and sigmoid colon [5].
A long list of medications that can cause this condition exists [6]. Most often a narcotic is the offending agent and many of these medications are associated with potent anticholinergic effects [7,8]. Antipsychotics are generally not a common cause of acute colonic pseudo obstruction [9]. However, clozapine has been recently recognized as an under-reported etiology [10].
Clozapine is an atypical antipsychotic used to treat resistant schizophrenia. The most likely mechanisms by which clozapine leads to this condition are through anticholinergic and antiserotonin-like effects [10,11]. A large Australian case series reported by Palmer et al. [12], suggested that this is a dose related phenomenon and is also directly related to serum drug levels. There is one case report in the literature reporting lithium as a cause of intestinal pseudo obstruction [13], but none exist that report the combination of lithium and clozapine as a cause that renders patients as higher risk. Patients with psychiatric disorders are usually treated with multiple medications, which generally have a large side effect profile. One of the most troublesome side effects is constipation, which theoretically can ultimately lead to intestinal pseudo obstruction through the same mechanism [14,15]. Multiple medications with anticholinergic activity can obviously predispose these patients to such a condition especially if their underlying disease leads to decreased oral intake and eventually dehydration in addition other metabolic derangements. Psychiatrists and general practitioners should be aware of the seriousness of such side effects and how to recognize when patients are heading towards developing complications of serious and potentially fatal outcomes.
References
- Maloney N, Vargas HD (2005) Acute intestinal pseudo-obstruction (Ogilvie’s syndrome). Clin Colon Rectal Surg 18: 96-101.
- Tack J (2006) Acute Colonic Pseudo-Obstruction (Ogilvie’s Syndrome). Curr Treat Options Gastroenterol 9: 361-368.
- Batke M, Cappell MS (2008) Adynamic ileus and acute colonic pseudo-obstruction. Med Clin North Am 92: 649-670.
- Amboldi M, Mezzabotta M, Zanotti M, Amboldi A, Morandi E (2009) Unusual causes of acute intestinal obstruction in adults. Int Surg 94: 99-110.
- Ozkurt H, Yilmaz F, Bas N, Coskun H, Basak M (2009) Acute colonic pseudo-obstruction (Ogilvie’s syndrome): radiologic diagnosis and medical treatment with neostigmine. Report of 4 cases. Am J Emerg Med 27: 757.
- Rondeau M, Weber JC, Nodot I, Storck D (2001) Acute colonic pseudo-obstruction in internal medicine: etiology and prognosis, report of a retrospective study. Rev Med Interne 22: 536-541.
- Cappell MS (2004) Colonic toxicity of administered drugs and chemicals. Am J Gastroenterol 99: 1175-1190.
- Beall DP, Hofmann LV (1996) Medication-induced adynamic ileus. Md Med J 45: 415-416.
- Levin TT, Barrett J, Mendelowitz A (2002) Death from clozapine-induced constipation: case report and literature review. Psychosomatics 43: 71-73.
- Pelizza L, De Luca P, La Pesa M, Borella D (2007) Clozapine-induced intestinal occlusion: a serious side effect. Acta Biomed 78: 144-148.
- Rondla S, Crane S (2007) A case of clozapine-induced paralytic ileus. Emerg Med J 24: e12.
- Palmer SE, McLean RM, Ellis PM, Harrison-Woolrych M (2008) Life-threatening clozapine-induced gastrointestinal hypomotility: an analysis of 102 cases. J Clin Psychiatry 69: 759-768.
- Perale L, Strizzolo L, Apollonio L, Calci M (2010) Adynamic ileus in chronic lithium intoxication. J Emerg Med 38: 502.
- De Bruin GJ, Bac DJ, Van Puijenbroek EP, van der Klooster JM (2009) Ogilvie Syndrome induced by clozapine. Ned Tijdschr Geneeskd 153: B437.
- Lu MK (1991) Clinical analysis in the main side effects of clozapine: enclosed 600 cases report. Zhonghua Shen Jing Jing Shen Ke Za Zhi 24: 71-74,123.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 16406
- [From(publication date):
May-2012 - Dec 01, 2025] - Breakdown by view type
- HTML page views : 11692
- PDF downloads : 4714