Case Report Open Access
Incisionless Laparoscopic Colectomy for Colorectal Cancer “Hybrid NOTES Technique Applied to Traditional Laparoscopic Colorectal Resection”
| Goutaro Katsuno*, Masaki Fukunaga, Kunihiko Nagakari, Yoshifumi Lee, Seiichiro Yoshikawa and Yoshitomo Ito |
|
| Department of Surgery, Juntendo Urayasu Hospital, Juntendo University, 2-1-1 Tomioka, Urayasu 279-0021, Japan | |
| Corresponding Author : | Goutaro Katsuno, MD Department of Surgery Juntendo Urayasu Hospital Juntendo University, 2-1-1 Tomioka Urayasu 279-0021, Japan Tel: 81 47 353 3111 Fax: 81 47 353 9264 E-mail: gkatsuno4596@sd5.so-net.ne.jp |
| Received September 11, 2011; Accepted December 11, 2011; Published December 13, 2011 | |
| Citation: Katsuno G, Fukunaga M, Nagakari K, Lee Y, Yoshikawa S, et al. (2011) Incisionless Laparoscopic Colectomy for Colorectal Cancer “Hybrid NOTES Technique Applied to Traditional Laparoscopic Colorectal Resection”. J Gastroint Dig Syst S6:001.. doi: 10.4172/2161-069X.S6-001 | |
| Copyright: © 2011 Katsuno G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
Background: We recently developed a new technique of laparoscopic colectomy (LAC) for colorectal cancer. This procedure, called “Incisionless LAC (iLAC)”, involves completely laparoscopic double stapling technique (DST) without mini-laparotomy. Methods: This technique was applied in the cases with relatively early-stage cancer of the sigmoid colon or rectum. The procedure involved 5 ports. Lymph node dissection and mobilization of the bowel were carried out completely via a laparoscope. The specimen was extracted through the original anus. Anastomosis was laparoscopically performed with DST. Method A: The proximal and distal parts of the lesion are transected with laparoscopic staplers. The staple at the upper rectum is released, and the lesion is removed out of the body through the anus. The anvil is attached to the proximal part of the bowel laparoscopically, followed by intracorporeal side-to-end anastomosis with DST. Method B: The proximal part of the lesion is transected with laparoscopic staplers. Then, the lesion and bowel are pulled out of the body through the anus by means of inversion, followed by transection of the distal side of the bowel with a stapler. The distal side of the bowel is pushed back into the body, and the anvil is attached to the proximal part of the bowel laparoscopically. Then, intr acorporeal anastomosis with DST is performed. Results: Method A was applied in eight cases. Method B was applied in twelve cases. Postoperative complications developed in none of the cases. Although the postoperative follow-up period to date is still short, no tumor recurrence in the stump has occurred in any of the cases. Conclusion: Our experience indicates this “iLAC” technique is feasible for selected patients with left-sided colonic tumors. Complications related to mini-laparotomy can be prevented completely with this hybrid approach.
| Keywords | |
| Incisionless laparoscopic Colectomy; Colon cancer; Hybrid NOTES technique | |
| Introduction | |
| In conventional laparoscopic surgery for left-sided colorectal cancers, the mesorectum and the rectum is divided using a laparoscopic stapler, and the subsequent anastomosis is performed laparoscopically by per-anal passage of a circular stapler. However, this technique requires a mini-laparotomy for specimen retrieval, which is often the cause of postoperative pain, wound infection, and as other pain-related or wound-related complications [1]. We recently developed a new technique of laparoscopic surgery for colorectal cancer. This procedure, called Incisionless laparoscopic colectomy (Incisionless LAC), involves completely laparoscopic double stapling technique (DST) without mini-laparotomy. We report here the early series of 20 patients who were treated with “Incisionless LAC (iLAC)” for colon cancer. | |
| Patients and Methods | |
| Between April 2007 and June 2011, 20 patients underwent “iLAC” for colon cancer at the Department of Surgery of Juntendo University Urayasu Hospital. This technique was applied in the cases with relatively early-stage cancer of the distal part of the sigmoid colon or upper rectum. The exclusion criteria were as follows: (1) tumors located at the right-sided colon, transverse colon, descending colon, or lower rectum; (2) T4 cancer or bulky tumor (circumferential rate > 50%); (3) bulky mesenterium including visceral fat accumulation; and (4) presence of anal stricture. All patients were informed about the advantages and disadvantages of this technique, and each of them provided a written consent. This procedure was performed by four surgeons who had wide experience in the use of conventional laparoscopic surgery. | |
| Surgical technique for iLAC | |
| Setting: General anesthesia was used in the same fashion as for conventional laparoscopic colectomy (LAC). All patients were placed in the lithotomy position. | |
| Access: A camera trocar (10 mm) was inserted at the umbilicus using an open insertion technique. Four additional trocars were inserted under direct vision: a 12-mm trocar in the right lower quadrant and a 5-mm trocar in the left lower quadrant and in the mid-clavicular line on each side at the level of the umbilicus. | |
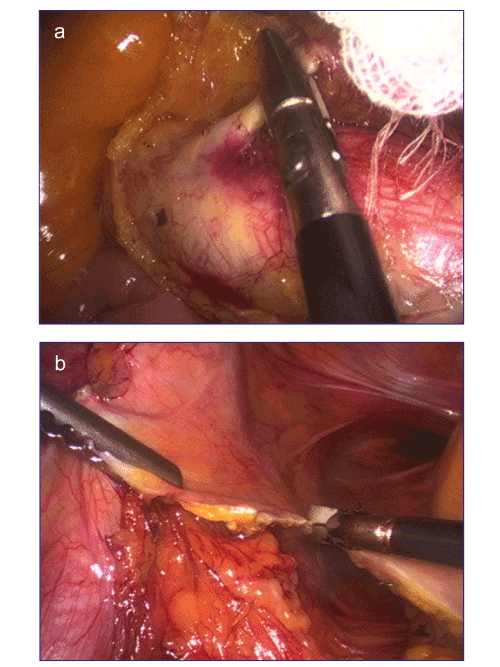
| Mobilization, Lymph node dissection: (Figure 1) After inspection of the diseased segment, mobilization was performed using a medial to lateral approach with mobilization of the mesentery of the sigmoid and the descending colon with the use of ultrasonically activated device (USAD) or laparoscopic bipolar scissors (Figure 1b). Routinely, the root of the inferior mesenteric vascular pedicles was initially dissected with lymphadenectomy using by LigaSure™ vessel sealing systems (Covidien) (Figure 1a). | |
| Bowel extraction through the anus (Hybrid NOTES technique): The specimen was extracted through the original anus using either Method A or Method B. | |
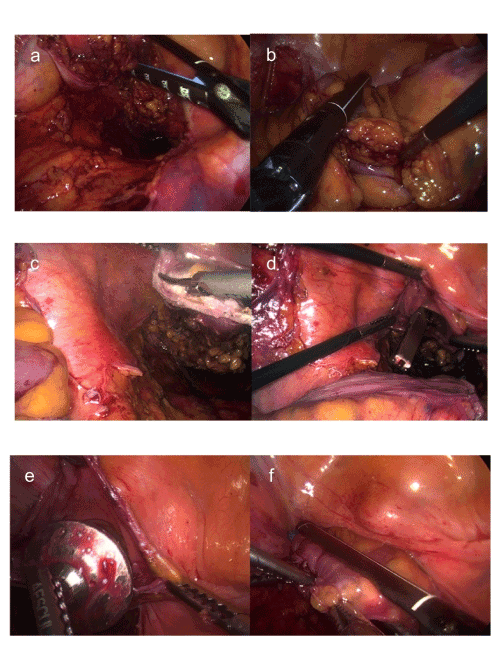
| Method A: (Figure 2) The mesentery is divided at the selected levels to secure the adequate proximal and distal surgical margins according to the JSCCR General Rules for Clinical and Pathological Studies on Cancer of the Colon, Rectum and Anus [2] using LigaSureTM (Covidien) device until the bowel tube is exposed. After cytocidal lavage of the distal rectal stump is carried out by the perineal surgeon, the bowel is transected with laparoscopic staplers at the chosen levels (Figure 2a,b). Next, an enterotomy is made immediately proximal to the staple at the upper rectum (Figure 2c), and then, the diseased segment is removed out of the body through the anus (Figure 2d), and the detachable anvil is gently passed into the colonic lumen through the anus using anvil grasping forceps (Figure 2e). Finally, the stump of the rectum is closed by a laparoscopic stapler (Figure 2f). | |
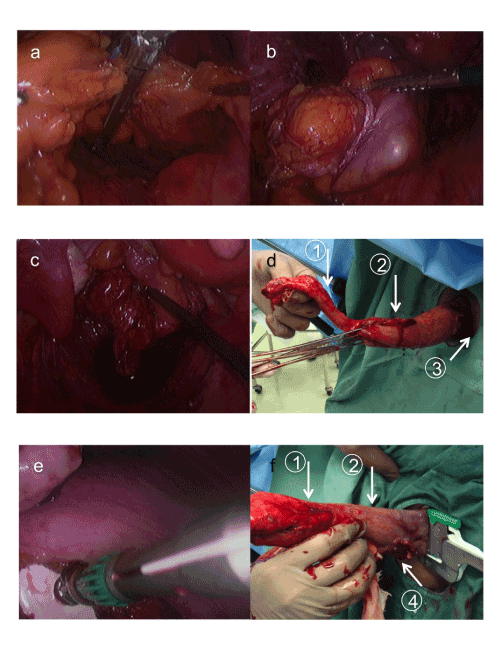
| Method B: After the mesentery is divided to secure the adequate proximal surgical margin according to the JSCCR General Rules for Clinical and PathologicalStudies on Cancer of the Colon, Rectum and Anus [2] with a LigaSureTM (Covidien) device until the bowel tube is exposed, the bowel is transected with a laparoscopic stapler at the intended level (Figure 3a). Next, the anus is carefully distended digitally, a grasping forceps is inserted under the laparoscope from the anus to secure the staple line of the distal rectum safely (Figure 3b), and the distal rectum is gradually everted and pulled transanally out of the body (Figure 3c,d). Rectal washout and wiping off are performed extracorporeally by the perineal surgeon, and then an enterotomy is made proximal to the staple line at the prolapsed rectum, and the detachable anvil is gently passed into the colonic lumen through the anus (Figure 3e), followed by transection of the distal side of the bowel with a stapler (Figure 3f). The distal side of the bowel is pushed back into the body [3]. | |
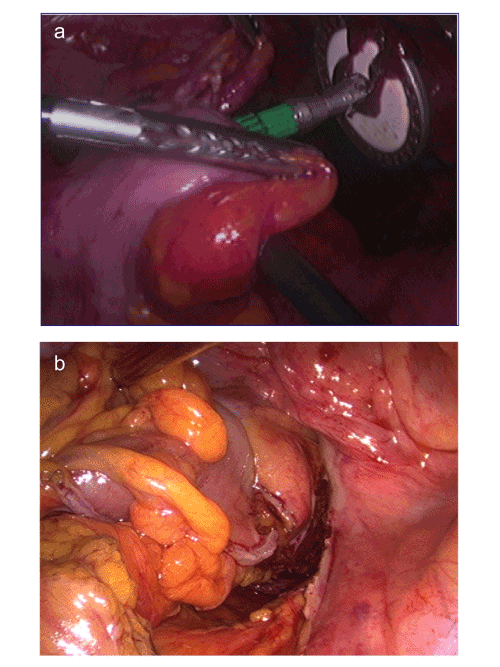
| Anastomosis: The anvil was attached to the proximal part of the bowel laparoscopically (Figure 4a), followed by intracorporeal sideto- end anastomosis with DST (Figure 4b). The spike was removed via the 12-mm port in the right iliac fossa. All anastomoses were tested by rectal air insufflation. | |
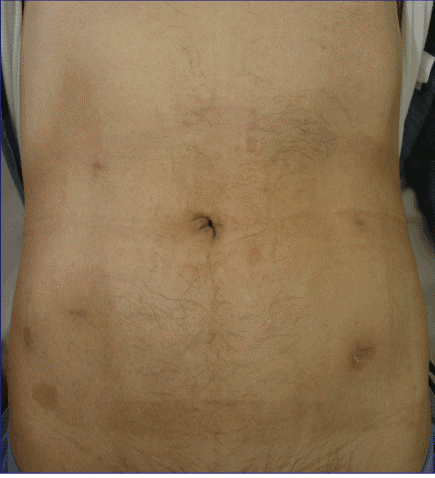
| Wound closure: The trocar sites on the fascia and a skin incision were closed with absorbable sutures. Finally, the fascial layers at the subumbilical port and the 5–12-mm port sites were closed (Figure 5). No drain was required. | |
| Results | |
| We reviewed the clinical records of 20 patients who underwent “iLAC” for colon cancer between Aug 2007 and Jun 2011. There were seven (35%) men and thirteen (65%) women. The mean age of the patients was 57.3±11 years (range, 38–73) and the mean body mass index (BMI) was 23.1±2.0 (range, 20–27) (Table 1). Of the 20 patients, ten had a tumor in the sigmoid colon, and ten in the rectum. Method A was employed in eight patients and Method B in twelve patients. The operating time ranged from 101 to 160 (mean, 134.4 ± 49) min. The volume of bleeding ranged from 5 to 50 (mean, 23±13) ml. There was no intraoperative complication. No patients required conversion to conventional LAC or open surgery. Postoperatively, there was no mortality. The time to adequate oral intake was 1.8±1.1 days. The mean hospital stay was 10.2±3.2 days. Postoperatively, there was no anastomotic leakage, wound infection, postoperative bleeding, intra-abdominal abscess or small bowel obstruction. The overall rate of postoperative complications was 0% (0/20) (Table 2). Histological examinations revealed a T1 tumor in eight patients, a T2 tumor in five, and a T3 tumor in seven. The number of harvested lymph nodes was 19±5, and eight patients had lymph node metastasis. Seven cases were classified as stage I, five as stage II, and eight as stage III. Most of the tumors were well or moderately-differentiated tubular adenocarcinomas (Table 3). | |
| Discussion | |
| Currently, laparoscopic colectomy (LAC) is gradually being regarded as the gold standard for the treatment of early colon cancer, even of advanced colon cancer [4-10]. Specimen retrieval in conventional LAC usually entails a 4–8-cm abdominal incision. This mini-laparotomy can be the cause of postoperative pain, wound infection, or other pain-related complications. | |
| In recent years, natural orifice transluminal endoscopic surgery (NOTES) has been offered as the next-generation minimally-invasive surgery with no scars [11,12]. However, NOTES is still considered experimental treatment; the risks inherent in this technique in terms of access, orientation, safety of closure have discouraged surgeons to use NOTES [13,14]. Because of the inconveniences associated with NOTES, transumbilical single port surgery [15] has gained greater interest and popularity. Some authors reported that this technique was safe and feasible for Single Incision Laparoscopic Colectomy (SILS colectomy) [16-19]. Since 2007, we have attempted to disuse an incision for specimen-retrieval in laparoscopic colectomy by incorporating a ‘‘natural orifice’’ technique. With two hybrid NOTES techniques, Method A or Method B, the anus is the natural orifice employed both for specimen extraction and anvil delivery and creation of a transanal stapled anastomosis. These hybrid procedures, called “iLAC”, enabled us to perform completely intracorporeal anastomosis using double stapling technique (DST) without mini-laparotomy. “iLAC” could be more easily performed than NOTES or SILS colectomy. | |
| In our small series, there were no postoperative complications. However, hospital stay in our study seemed longer. This could be explained by that the Japanese health insurance system is considerably different from the Western one. Although the postoperative followup period to date is still short, no tumor recurrence in the stump has been observed in any of the cases. These hybrid techniques are safe and feasible with existing instruments, and may represent a bridge-use for NOTES or SILS colectomy. In 2009, Cheung, et al. [20] reported that laparoscopic colectomy without mini-laparotomy could be performed using a per-anal transanal endoscopic operation (TEO) device (Karl Storz Endoscopy, Tuttlingen, Germany); none of the patients in their series developed postoperative complications. Cheung’s method is almost similar to our Method A. Method B was our original method using a prolapsing method [3]. We think that our results are acceptable comparable to Cheung’s published series. However, further work is needed to evaluate the potential benefits of this new technique before its use can be widely recommended. | |
| Conclusions | |
| Our findings indicate this “iLAC” technique is feasible for selected patients with left-sided colonic tumors. Complications related to minilaparotomy can be prevented entirely with this hybrid approach. | |
| References | |
References
- Christen D, Buchmann P, Klingler K (1995) How safe is laparoscopic colon surgery? Schweiz Med Wochenschr 125: 1597–1601.
- Japanese Society for Cancer of the Colon and Rectum (2009) General Rules for Clinical and Pathological Studies on Cancer of the Colon, Rectum and Anus 7th edn (in Japanese) Kanehara-Syuppan, Tokyo.
- Fukunaga M, Kidokoro A, Iba T, Sugiyama K, Fukunaga T, et al. (2005) Laparoscopy-assisted low anterior resection with a prolapsing technique for low rectal cancer. Surg Today 35: 598–602.
- Lacy AM, Garcia-Valdecasas JC, Delgado S, Castells A, Taura P, et al. (2002) Laparoscopy-assisted colectomy versus open Colectomy for treatment of non-metastatic colon cancer: a randomised trial. Lancet 359: 2224–2229.
- Lacy AM, Delgado S, Castells A, Prins HA, Arroyo V, et al. (2008) The long-term results of a randomized clinical trial of laparoscopy-assisted versus open surgery for colon cancer. Ann Surg 248: 1-7.
- Guillou PJ, Quirke P, Thorpe H, Walker J, Jayne DG, et al. (2005) Shortterm endpoints of conventional versus laparoscopic-assisted surgery in patients with colorectal cancer (MRC CLASICC trial): multicentre, randomized controlled trial. Lancet 365: 1718–1726.
- Jayne DG, Guillou PJ, Thorpe H, Quirke P, Copeland J, et al. (2007) Randomized trial of laparoscopic-assisted resection of colorectal carcinoma: 3-year results of the UK MRC CLASICC Trial Group. J Clin Oncol 25: 3061-3068.
- Veldkamp R, Kuhry E, Hop WC, Jeekel J, Kazemier G, et al. (2005) Laparoscopic surgery versus open surgery for colon cancer: short-term outcomes of a randomised trial. Lancet Oncol 6: 477-484.
- Colon Cancer Laparoscopic or Open Resection Study Group, Buunen M, Veldkamp R, Hop WC, Kuhry E, et al. (2009) Survival after laparoscopic surgery versus open surgery for colon cancer: long-term outcome of a randomised clinical trial. Lancet Oncol 10: 44-52.
- Clinical Outcomes of Surgical Therapy Study Group (2004) A comparison of laparoscopically assisted and open colectomy for colon cancer. N Engl J Med 350: 2050-2059.
- Kalloo AN, Singh VK, Jagannath SB, Niiyama H, Hill SL, et al. (2004) Flexible transgastric peritoneoscopy: a novel approach to diagnostic and therapeutic interventions in the peritoneal cavity. Gastrointest Endosc 60: 114–117.
- Marescaux J, Dallemagne B, Perretta S, Wattiez A, Mutter D, et al. (2007) Surgery without scars: report of transluminal cholecystectomy in a human being. Arch Surg 142: 823–826.
- de la Fuente SG, Demaria EJ, Reynolds JD, Poertenier DD, Pryor AD (2007) New development in surgery: natural orifice transluminal endoscopic surgery (NOTES). Arch Surg 142: 295–297.
- Leroy J, Cahill RA, Peretta S, Forgione A, Dallemagne B, et al. (2009) Natural orifice translumenal endoscopic surgery (NOTES) applied totally to sigmoidectomy: an original technique with survival in a porcine model. Surg Endosc23: 24–30.
- Tacchino R, Greco F, Matera D (2009) Single-incision laparoscopic cholecystectomy: surgery without a visible scar. Surg Endosc 23: 896–899.
- Remzi FH, Kirat HT, Kaouk JH, Geisler DP (2008) Single-port laparoscopy in colorectal surgery. Colorectal Dis 10: 823–826.
- Bucher P, Pugin F, Morel P (2008) Single port access laparoscopic right hemicolectomy. Int J Colorectal Dis 23: 1013–1016.
- Geisler DP, Condon ET, Remzi FH (2010) Single incision laparoscopic total proctocolectomy with ileopouch anal anastomosis. Colorectal Dis 12: 941-943.
- Katsuno G, Fukunaga M, Nagakari K, Yoshikawa S, Ouchi M, et al. (2011) Single-incision laparoscopic colectomy for colon cancer: early experience with 31 cases. Dis Colon Rectum 54: 705-710.
- Cheung HY, Leung AL, Chung CC, Ng DC, Li MK (2009) Endo-laparoscopic colectomy without mini laparotomy for left-sided colonic tumors. World J Surg 33: 1287-1291.
Tables and Figures at a glance
| Table 1 | Table 2 | Table 3 |
Figures at a glance
 |
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 | Figure 5 |
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 14420
- [From(publication date):
specialissue-2013 - Dec 20, 2025] - Breakdown by view type
- HTML page views : 9758
- PDF downloads : 4662
