An Unusual Case of Postoperative Late Onset Sudden Sensorineural Hearing Loss
Received: 07-Jan-2014 / Accepted Date: 21-Jan-2014 / Published Date: 29-Jan-2014 DOI: 10.4172/2161-119X.1000155
Abstract
Sudden sensorineural hearing loss, is a clinical entity of ambiguously defined etiology manifested by hearing loss of more than 30 dB on three contiguous frequencies occurring within 72 hours. Sudden sensorineural hearing loss has been called an otologic emergency and patient evaluation should proceed promptly. Early presentation to a physician and early institution of treatment improves the prognosis for hearing recovery. Although it is not an infrequent condition in otolaryngology practice, sudden sensorineural hearing loss following non-otologic surgery is an extremely rare complication.
In literature, there are some case reports presenting, postoperative sudden sensorineural hearing loss after spinal and cardiac surgery. In all of the reported cases hearing loss existing during the first week of post operative period. In the present case of a 67 years old female patient who underwent coronary artery bypass surgery under general anesthesia and developed hearing loss of the left ear on postoperative fifteenth day. Because the patient were under anticoagulant, antihypertensive, and antidiabetic therapy, we only gave 1 mg/kg corticosteroid treatment for two weeks. Pure tone audiograms were repeated at daily intervals but no improvement seen in hearing.
A high index of suspicion and close follow up are required to early diagnosis of this complication. It is crucial that individuals with sudden hearing loss are identified as soon as possible as the recovery rate had been shown to be higher in those who presented early.
Keywords: Coronary artery bypass surgery, Hearing loss, Sudden sensorineural hearing loss
Introduction
Sudden Sensorineural Hearing Loss (SSHL) is classified as an acute unexplained hearing loss of more than 30 dB on three contiguous frequencies, nearly always unilateral, that occurs in a period less than a 72 hours period. SSHL can occur at any age, but most commonly affects individuals 43 to 53 years of age. SSHL is a medical emergency for which definitive diagnosis and treatment is still largely unknown. Since recovery is often spontaneous, many affected people likely never seek medical attention. The severity of sensorineural hearing loss can vary between mild, moderate, or severe, and may cause total deafness [1].
The etiologies for individuals suffering SSHL can be: idiopathic (71.0%), infectious disease (12.8%), otologic disease (4.7%), trauma (4.2%), vascular or hematologic (2.8%), neoplastic (2.3%), and other causes (2.2%) [2]. SSHL can be a rare complication of the non-otologic surgery under general anestesia. The risk factors for the most cases of SSHL (idiopathic causes) are uncertain, being present in similar numbers of affected men and women. Diagnostic evaluation of the patient with sudden hearing loss begins with a thorough history and physical examination.Details of the circumstances about the hearing loss and the time course of its onset should be obtained.Associated symptoms, such as tinnitus, vertigo or dizziness, and aural fullness should also be questioned. Complete audiometric evaluation, Brainstem Evoked-Response Audiometry (BERA) and MRI are crucial investigations to explore the etiology [3].
Herein, we report a case of late onset postoperative SSHL, after two weeks, in a 67 years old woman who underwent cardiopulmonary bypass surgery. This is the first case in literature with late-onset SSHL occuring after the first week of postoperative period.
Case Presentation
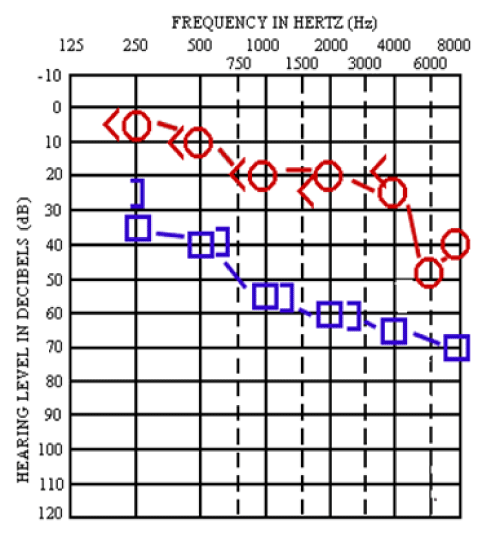
A 67 years old female patient, who had hypertension and type II diabetes mellitus for a long time, presented to the emergency clinic with a three weeks history of exertional chest pain. She had recently undergone a myocardial infarction and subsequent cardiac catheterization had revealed severe three-vessel coronary artery disease. Finally she underwent coronary artery bypass surgery under general anesthesia and developed postoperative hearing loss of the left ear. The patient suffered from profound hearing loss and tinnitus that was recognized on postoperative fifteenth day, and audiometry tests confirmed the diagnosis (Figure 1).
On otoscopic examination, tympanic membranes were normal. Rinne test was positive bilaterally and weber test demonstrated lateralized conduction to the right ear. She denied aural fullness and vertigo. The rest of the cranial nerves and peripheral neurologic examination were grossly intact. Cranial MRI and routine biochemical laboratory findings were normal. Because the patient were under anticoagulant, antihypertensive, and antidiabetic therapy, we only gave 1 mg/kg corticosteroid treatment for 2 weeks. Pure tone audiograms were repeated at daily intervals but no improvement seen in hearing. Her follow up pure tone audiogram at six months showed no improvement either.
Discussion
There are many potential causes of SSHL, but despite extensive investigations, the majority of cases elude definitive diagnosis and therefore, remain idiopathic. The differential diagnosis of SSHL is extensive and a wide variety of diseases should be taken into account. Infectious causes may be bacterial due to meningitis and labyrinthitis or viral due to mumps, HSV, and CMV.Inflammatory and autoimmune disorders such as Cogan syndrome, systemic lupus, multiple sclerosis, ischemic changes may be associated with SSHL. Traumatic injury from temporal bone fracture, acoustic trauma, and perilymph fistula possibly due to exposure to sudden changes in barometric pressure (such as during flying or diving), or exposure to a loud noise may also result in acute hearing loss. Neoplastic disorders such as a cerebellopontine angle tumors, internal acoustic canal tumors are possible.Vascular and/ or hematologic causes may include thromboembolism, cerebral infarct, transient ischemic attack, sickle cell disease, and macroglobulinemia. Drug toxicity from aspirin, aminoglycosides, and chemotherapeutic agents may also lead to sudden hearing loss [1,2].
Hearing loss followed by non-otologic surgical procedures is not often mentioned in the literature, it is associated to cardiopulmonary bypass and spinal anesthesia most of time [4]. Various etiologies had thus been proposed to look into the pathophysiology of this phenomenon and thus offer a possible preventive or curative measure. Microemboli phenomena (fat, air or particulate thrombi), perioperative hypotension or perfusion failure, hypercoagulable states, and ototoxic drug usage are some of the better recognized ones [5,6]. Microemboli occluding internal auditory artery is proposed underlying mechanism of SSHL associated with cardiac surgery, taking into consideration that the blood supply to the cochlea take place through an end artery [7,8].
All of the reported cases of SSHL following cardiopulmunary bypass surgery were during the first week of post operative period [4-7]. To the best of our knowledge, this is the first case with late-onset SSHL occured on the postoperative fifteenth day.
This acute dysfunction of the inner ear consists a controversial subject in terms of etiological mechanisms and treatment modalities. In this case, the etiology is probably multi-factorial and there are several factors that should be considered. First of all, the patient has been taking loop diuretics in order to control hypertension and these agents may cause ototoxic effects. Furthermore, it should be taken into account that she was diabetic and it could be established a diabetic microangiopathy at the artery of cochlea. This possible vasculopathy in association with an episode of vasospasm could interrupt blood supply to the cochlea. Finally a microemboli due to postoperative hypercoagulability could be the etiologic factor. The duration of high dose anticoagulant therapy after cardiopulmonary surgery might be elongated in such high risk patients in order to decrease the thrombus formation.
In the literature there are conflicting data about the prognosis of postoperative SSHL. Severe hearing loss, down-sloping audiogram, presence of vertigo and advanced age are the unfavorable factors for recovery [9]. Although improvement in hearing level was not seen in our case, we believe that early detection and prompt evaluation of hearing loss may improve outcome.
Conclusion
Temporary forms of SSHL following anesthesia usually go unrecognized by the patient and clinician but probably occur more often than is generally assumed. There are a lot of hypotesis about SSHL etiology, but since it is multifactorial in nature, analyzing this issue in more cases and prospective clinic studies is required. We encourage the continued reporting of this rare complication following non-otologic surgery. To understand the exact cause, and the pathophysiology and to determine better curative and preventive measures to eliminate any further incidence of the sudden SNHL from not only coronary artery surgical interventions but other non-otologic procedures as well, is a source of some concern to surgeons and the solution lies in evidence based medicine in this direction.
References
- Rauch SD (2008) Clinical practice. Idiopathic sudden sensorineural hearing loss. N Engl J Med 359:833.
- Fetterman BL, Luxford WM, Saunders JE (1996) Sudden bilateral sensorineural hearing loss. Laryngoscope 106: 1347-1350.
- Castro TM, Costa LA, Nemezio ME, Fonseca LJ (2011) Bilateral sudden deafness. Braz J Otorhinolaryngol 77: 678.
- Walsted A, Andreassen UK, Berthelsen PG, Olesen A (2000) Hearing loss after cardiopulmonary bypass surgery. Eur Arch Otorhinolaryngol 257: 124-127.
- Sprung J, Bourke D, Contreras M, Warner M, Findlay J (2003) Perioperative hearing impairment. Anesthesiology 98: 241-257.
- Shapiro MJ, Purn JM, Raskin C (1981) A study of the effects of cardiopulmonary bypass surgery on auditory function. Laryngoscope 91: 2046-2052.
- Linares RAP (2005) Sudden Sensorineural Hearing Loss after General Anesthesia to Laparoscopic Colecystectomy. Int. Arch. Otorhinolaryngol 9: 320-324.
- Evan K, Tavill M, Goldberg A, Silverstein H (1997)Suddensensorineural hearing loss after general anesthesia for nonotologic surgery. Laryngoscope 107: 747-752.
- Eisenman D, Arts HA (2000) Effectiveness of treatment for sudden sensorineural hearing loss. Arch Otolaryngol Head Neck Surg1261161-1614.
Citation: Kucur C, Kuduban O, Simsek E, Ozkan O, Oghan F (2014) An Unusual Case of Postoperative Late Onset Sudden Sensorineural Hearing Loss. Otolaryngology 4:155. DOI: 10.4172/2161-119X.1000155
Copyright: © 2014 Kucur C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 15767
- [From(publication date): 2-2014 - Oct 06, 2024]
- Breakdown by view type
- HTML page views: 11325
- PDF downloads: 4442