Case Report Open Access
A Case with Ileoileal Intussusception Secondary to Malignant Melanoma Metastasis
Süleyman Baldane1* and Ersin Ozaslan21Department of Internal Medicine, Faculty of Medicine, Selcuk University, Konya, Turkey
2Department of Oncology, Faculty of Medicine, Erciyes University, Kayseri, Turkey
- *Corresponding Author:
- Suleyman Baldane
Department of Internal Medicine, Faculty of Medicine
Selcuk University, Konya
Postal code: 42075, Turkey
Tel: +903322244685
Fax: +903322412184
E-mail: baldane42@hotmail.com
Received date: June 2, 2015 Accepted date: June 30, 2015 Published date: July 5, 2015
Citation: Baldane S, Ozaslan E (2015) A Case with Ileoileal Intussusception Secondary to Malignant Melanoma Metastasis. J Gastrointest Dig Syst 5:305. doi:10.4172/2161-069X.1000305
Copyright: © 2015 Baldane S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Keywords:
Malignant melanoma; Small-bowel intussusception; Metastasis
Case Report
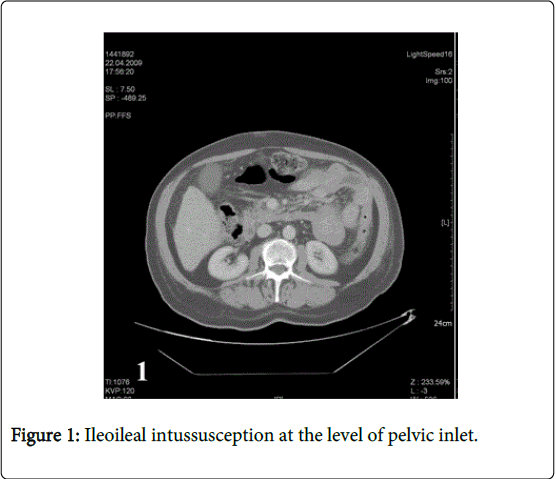
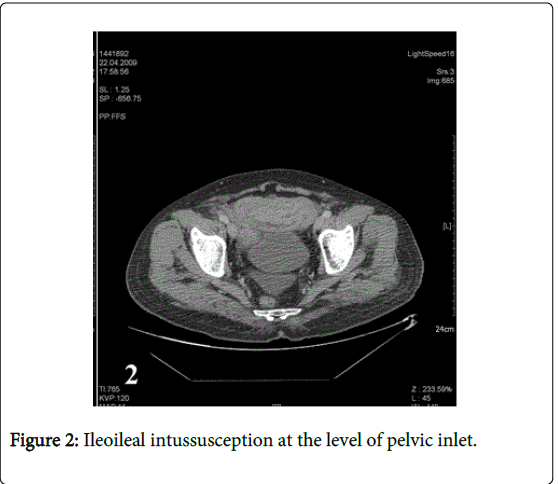
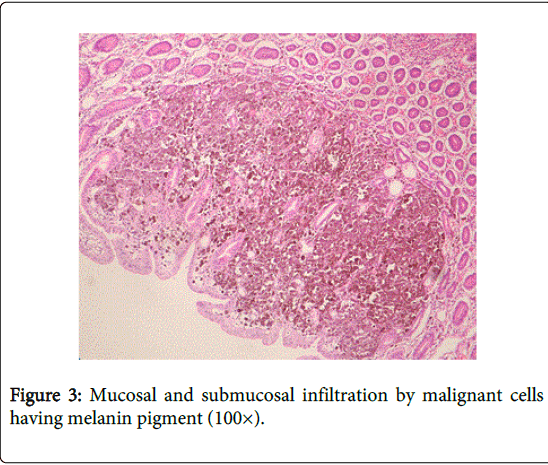
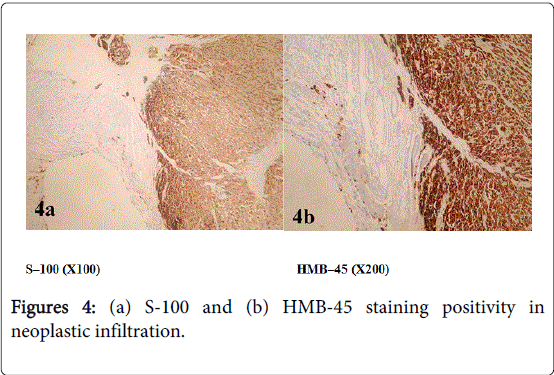
58-year old male patient consulted a doctor 4 years ago with the complaint of an enlarging congenital skin spot above the navel. Pathological examination of excisional biopsy specimen of the lesion was reported as malignant melanoma (tumor thickness 0.4 cm, clark level III, clean surgical margins). The patient who had not been re-examined during the last four years was admitted to emergency department with severe abdominal pain, nausea and vomiting. Abdominal computerized tomography examination revealed multiple metastatic lesions in the liver, the diameter of the largest lesion is being 1.5 cm, lymph nodes in mesenteric fatty tissue, the largest one is being about 2 cm and ileoileal invagination in pelvic inlet (Figures 1 and 2). The patient having intestinal obstruction findings was taken to operating room for urgent operation. In the operation, two separate invaginations originating from the mass in the lumen were detected. The first one was 90 cm proximal to ileocecal valve, the other one was located 70 cm distal to treitz ligament and both were resected leaving a margin of normal tissue around. Pathological examination of small intestine samples revealed malignant melanoma metastasis (Figures 3, 4a and 4b).
Cutaneous malignant melanoma is a tumor with high metastatic capacity and may spread to many tissues including gastrointestinal system. Jejunum and ileum are the parts of gastrointestinal system to which malignant melanoma mostly metastasizes [1]. Primary small intestinal melanoma is very rare and many authors accept it as metastasis of a cutaneous malignant melanoma of unknown origin.
Median time from the diagnosis of cutaneous malignant melanoma to the development of intestinal metastasis is 3-6 years, while cases with synchronous metastasis or who had developed metastasis 6 months after the diagnosis have also been reported [2]. The diagnosis of metastasis is usually delayed due to long asymptomatic period or nonspecific abdominal symptoms. As it was also seen in our case, acute presentation related to some conditions such as intestinal intussusception may also be seen due to delayed diagnosis.
Capsule endoscopy, computed tomography (CT), magnetic resonance (MR) and positron emission tomography (PET) may be used in preoperative diagnosis of small intestinal melanoma. Sensitivity of capsule endoscopy in detecting small intestinal metastases is high but extra-intestinal intra-abdominal metastases may be detected by CT, MR and PET [3]. However, definitive diagnosis of small bowel metastasis can be obtained only after explorative laparotomy.
More frequent gastrointestinal system spread is seen in the patients with a primary lesion classified as Clark III or higher, while spread to gastrointestinal system is quite rare in the patients with Clark I and II lesions [4]. Pathological diagnosis of gastrointestinal system metastasis of malignant melanoma requires a careful examination of mucosa and metastatic lesion and use of some immunohistochemical staining methods such as S-100 and HMB-45.
Surgical resection is the standard treatment modality in this patient group, especially in the patients with limited metastatic spread. Although surgical resection is not curative, it should be remembered that it provides a good increase in the prognosis in case of clear surgical margins [5].
In conclusion, gastrointestinal system metastasis of malignant melanoma may appear after a long silent period. It is very important to closely follow the patients with a primary lesion classified as Clark III or higher for the development of gastrointestinal system metastasis. Nonspecific abdominal symptoms or emergent conditions such as intestinal obstruction should raise the suspicion of gastrointestinal system metastasis.
References
- Reintgen DS, Thompson W, Garbutt J, Seigler HF (1984) Radiologic, endoscopic, and surgical considerations of melanoma metastatic to the gastrointestinal tract. Surgery 95: 635-639.
- Bender GN, Maglinte DD, McLarney JH, Rex D, Kelvin FM (2001) Malignant melanoma: patterns of metastasis to the small bowel, reliability of imaging studies and clinical relevance. Am J Gastroenterol 96: 2392–2400.
- Iddan GJ, Swain CP (2004) History and development of capsule endoscopy. GastrointestEndoscClin N Am 14: 1-9.
- Jorge E, Harvey HA, Simmonds MA, Lipton A, Joehl RJ (1984) Symptomatic malignant melanoma of the gastrointestinal tract. Operative treatment and survival. Ann Surg199:328-331.
- Schuchter LM, Green R, Fraker D (2000) Primary and metastatic diseases in malignant melanoma of the gastrointestinal tract. CurrOpinOncol12:181-185.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 14959
- [From(publication date):
August-2015 - Aug 16, 2025] - Breakdown by view type
- HTML page views : 10368
- PDF downloads : 4591