Research Article Open Access
A Comparison of Three types of Trail Making Test in the Korean Elderly: Higher Completion Rate of Trail Making Test-Black and White for Mild Cognitive Impairment
Karyeong Kim1, Jae-Won Jang2, Min Jae Baek1 and Sang Yun Kim1,3*
1Clinical Neuroscience Center, Seoul National University Bundang Hospital, Seongnam, Republic of Korea
2Department of Neurology, Kangwon National University Hospital, Chuncheon, Republic of Korea
3Department of Neurology, Seoul National University College of Medicine, Seoul, Korea
- Corresponding Author:
- SangYun Kim
Department of Neurology, Seoul National University Bundang Hospital
300 Gumi-dong, Bundang-gu, Seongnam-si, 463-707, Republic of Korea
Tel: +82 31 787 7462
E-mail: neuroksy@snu.ac.kr
Received Date: May 25, 2016; Accepted Date: May 30, 2016; Published Date: June 07, 2016
Citation: Kim K, Jang JW, Baek MJ, Kim SY (2016) A Comparison of Three types of Trail Making Test in the Korean Elderly: Higher Completion Rate of Trail Making Test-Black and White for Mild Cognitive Impairment. J Alzheimers Dis Parkinsonism 6:239. doi: 10.4172/2161-0460.1000239
Copyright: © 2016 Kim K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Alzheimers Disease & Parkinsonism
Abstract
Objective: A Korean version of Trail Making Test (TMT) led to reduced clinical use in Korea because of lower completion rate. The current study examines multiple TMT versions in effort to identify which type might accurately detect cognitive decline with higher completion rate.
Methods: Three versions of TMT including the original TMT, TMT-Korean Letter (TMT-K), and TMT-Black and White (TMT-B&W) were utilized. A total of 62 participants were included, comprised of 30 cognitively normal controls (NC) and 32 mild cognitive impairment (MCI). Three TMT versions were administered to subjects with other neuropsychological tests.
Results: TMT-B&W completion time as well as that of Original TMT and TMT-K was successful in distinguishing MCI from NC adjusted for age, sex and educational level. TMT-B&W also showed a high correlation with other neuropsychological tests that represent frontal executive function. Regarding completion rate in MCI patients, Original TMT and TMT-K were not successfully completed (62% and 60.6%, respectively) compared with TMT-B&W (90.1%).
Conclusion: As TMT-B&W showed higher completion rate than others and revealed significant correlation with frontal executive function, this culture-fair measure can vitalize TMT task with increased applicability in Korean elderly adults who are unfamiliar with the sequence of English or Korean alphabet.
Keywords
Trail making test; Frontal lobe function test; Mild cognitive impairment
Introduction
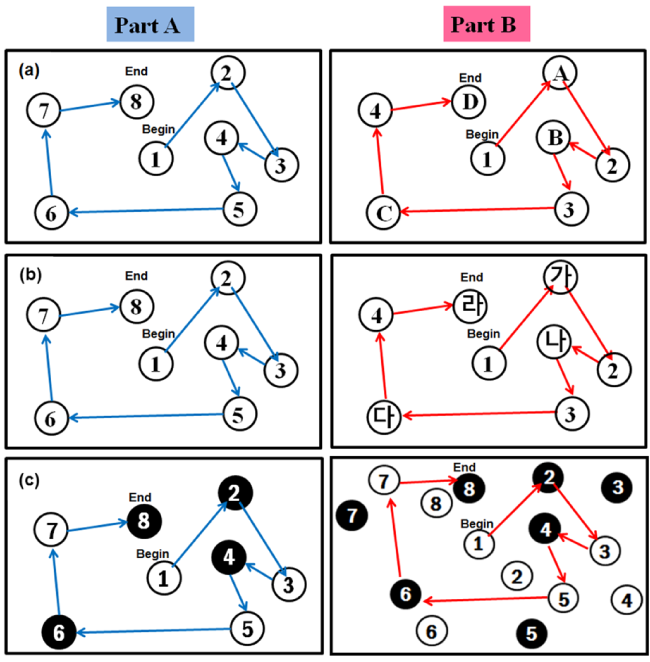
As widely used neuropsychological test in a clinical setting [1], the Trial Making Test (TMT) identifies and distinguishes cognitive impairment [2-4] in a concise and simple manner [5-7]. The TMT has two parts: part A requires the test-taker to connect numbers (1-25) that are randomly distributed on a test paper (1->2->3…), while part B calls for the test-taker to alternate numbers and letters (1->A->2->B…) (Figure 1a). Part B requires more complex cognitive functions [8], and has proven to be sensitive to prefrontal cortical damage [9,10].
Past researchers have tried to develop a Korean version of TMT (TMT-K). In the initial version of TMT-K, part A used the same test sheet as the original TMT, while part B consisted of numbers and Korean alphabet (ê°�?, ë�?�?, ë�?¤……), instead of English alphabet (Figure 1b). However, even adults with normal cognitive ability had difficulty recalling the series of Korean characters, leading to poorer than expected performance on this task [11]. To accommodate testing in the elderly, who have a shorter attention span and lower educational level; researchers devised the Korean-Trail Making Test for the Elderly (K-TMT-e) [12]. However, K-TMT-e was too simple that it did not discriminate those with mild cognitive impairment (MCI) from cognitively normal subjects and showed no correlation with other cognitive tests that represent frontal executive function. Continued efforts to develop a TMT-K by replacing the stimuli of English alphabet in TMT-B with other characters have not been successful, in turn, leading to infrequent clinical use of the TMT [13]. To overcome these problems that might be caused by using alphabet, we developed the Trail Making Test-Black & White (TMT-B&W) using colours and Figures as stimuli in the same trace as the original ones [14] (Figure 1c).
The aims of the current study were 1) to validate the new versions of TMT-B&W in effort to maximize test-taker performance, and 2) to administer the three versions of these tests in older Korean healthy and patient with cognitively impaired subjects, to distinguish groups at the stage of mild cognitive impairment.
Materials and Methods
Subjects
Our subjects sample was a group of consecutive Korean patients who visited a health care centre of Seoul National University Bundang Hospital with complaint of memory decline. Inclusion criteria for mild cognitive impairment (MCI) based on Peterson criteria [15], were as follows: 1) cognitive complaints verified by a collateral source of information; 2) objectively abnormal cognitive impairment in one or more cognitive functions; 3) preserved ADL function; 4) normal visual and auditory functions; 5) no previously diagnosed neurological or psychiatric diseases; 6) failure to meet the diagnostic criteria of dementia based on the National Institute of Neurological and Communicative Disorders and Stroke and Alzheimer’s Disease and Related Disorders Association (NINCDS-ADRDA) [16].
The outpatients from a health care centre or caregivers of patients from Clinical Neuroscience Centre of Seoul National University Bundang Hospital were recruited as subjects with normal cognition (NC). Criteria for the NC group were as follows: 1) no cognitive complaint verified by any measurable information; 2) Mini-Mental State Examination (MMSE) no more than one standard below the mean for education and age [17]; 3) absence of significant impairment in any cognitive functions; 4) preserved activities of daily living (ADL) [18,19]; 5) absence of medical history that could undermine cognitive functions [20]; and 6) Geriatric Depression Scale (GDS) of less than 17 on the 30 item scale in the past week, suggesting absence of clinically significant depression.
After assessing for eligibility test for consecutively recruited 166 subjects, we excluded 51 individuals requiring more than 300 s to complete any type of TMT-B form and 53 subjects considered to have probable AD with mild dementia according to the NINCDS-ADRDA criteria [16]. Finally, this study included 62 total participants, comprised of 30 cognitively normal controls (NC) and 32 patients diagnosed with mild cognitive impairment (MCI).
This study was approved by the Seoul National University Hospital Institutional Review Board and written informed consent was obtained from all subjects before all procedures. The approval number is “B- 1306/208-107”.
Materials
Trail making test: Th e current study used three different forms of TMT. This study used 216 × 276 mm (letter size) paper, directions, and the trace of stimuli, in the same way as the original TMT [21]. The TMT versions included:
a. The original English version of the TMT (TMT-OR) (Figure 1a)
b. The TMT-Korean Letter (TMT-K) in which English letters are replaced with Korean letters (Figure 1b)
c. the TMT-Black and White (TMT-B&W), which has white numbers in black circles and black numbers in white circles distributed on a test sheet, composed of part A and B (Figure 1c). TMT-B&W part A (TMT-B&W-A) requires participants to draw a line to connect the 25 encircled numbers in ascending order without lifting their pen or pencil from the test sheet, as they complete part A of TMT (TMT-A). For the TMT-B&W Part B (TMT-B&W-B), numbers from 1 to 25 are presented in white and black backgrounds. The participant is instructed to connect consecutive numbers, alternating between white and black circles (i.e., 1(W)-2(B)- 3(W)-4(B)…).
Instructions were conducted in the same manner of the original TMT. An exercise trial was conducted before the test trial to make sure each participant fully understood how to do the task. A researcher started recording time as soon as the participant put the pen or pencil on the first circle and stopped measuring time when the pencil touched the last number. The time taken to complete the task was measured in seconds and 300 s for each TMT were allowed as maximum time. In order to control for learning effects, three tests were assigned randomly to subjects.
Other neuropsychological tests: Given that the intention of the current study was to determine feasibility of different versions of the TMT within the context of other neuropsychological evaluation, several other standard neuropsychological assessment tools that represent frontal executive function were used. These included Controlled Oral Word Association Task (COWAT) and Stroop test.
Method
Prior to the test, all participants’ personal information and level of subjective cognitive impairment was gathered through interview, and Mini-mental state examination (MMSE) was completed. Each participant was administered three types of TMT and subsequently given the neuropsychological test in order to minimize any possible influence of other neuropsychological tests on TMT performance. All tests were individually administered.
Statistical analysis
Student’s t-test was used to assess differences in age, education level. Multivariate analysis of covariance (MANCOVA) test was used to determine presence of any group differences in TMT time-to-completion as well as the results of other neuropsychological test between clinical groups, with age, education and gender as covariates. The chi-square (χ2) test was used to assess difference in categorical variables. To ensure construct validity of each TMT, we conducted correlations between the three types of TMT and other neuropsychological tests using Pearson’s R coefficient. Receiver operating characteristics (ROC) curves were obtained to evaluate whether the TMT showed difference in the clinical groups. All analyses were done with the PASW statistics version 18.0, with the statistical significance level set to P<0.05
Results
The demographic and clinical characteristics of the participants are described in Table 1. There were significant differences in age and gender between clinical groups (p<0.006 and p<0.001, respectively). Compared to NC subjects, MCI subjects demonstrated significantly lower MMSE scores, COWAT-Semantic word fluency, COWATPhonemic word fluency scores and Stroop test scores.
| Characteristics | Normal control (n=30) | MCI (n=32) | Significant difference between MCI versus NC |
|---|---|---|---|
| Age (years) | 61.33 ± 6.59 | 67.06 ± 9.20 | 0.006 |
| Gender (%male) | 7 (23.3) | 22 (68.8) | <0.001 |
| Education (years) | 14.57 ± 2.86 | 16.03 ± 3.07 | 0.057 |
| MMSE | 28.87 ± 0.90 | 27.62 ± 1.39 | 0.004 |
| COWAT-S | 22.53 ± 6.11 | 19.44 ± 6.87 | 0.011 |
| COWAT-P | 32.03 ± 10.28 | 29.28 ± 12.08 | 0.001 |
| Stroop test-W | 112.00 ± 0.00 | 111.94 ± 0.25 | 0.020 |
| Stroop test-C | 105.93 ± 8.66 | 81.44 ± 23.46 | <0.001 |
| TMT-OR-A | 41.63 ± 7.79 | 49.19 ± 15.68 | 0.003 |
| TMT-OR-B | 89.53 ± 20.64 | 123.06 ± 42.31 | <0.001 |
| TMT-K-B | 84.63 ± 22.56 | 114.22 ± 39.94 | <0.001 |
| TMT-B&W-A | 38.47 ± 12.73 | 57.00 ± 21.69 | <0.001 |
| TMT-B&W-B | 110.30 ± 31.93 | 168.91 ± 72.25 | <0.001 |
All values except gender represent mean ± standard deviation. Significant difference between MCI versus NC was evaluated adjusted for age, gender and level of education
Table 1: Baseline demographics and characteristics according to diagnostic groups.
The original trail making test
There were significant group differences in time-to-completion of TMT-OR-A and TMT-OR-B adjusted for age, gender and level of education (p=0.003 for part A and p<0.001 for part B) (Table 1).
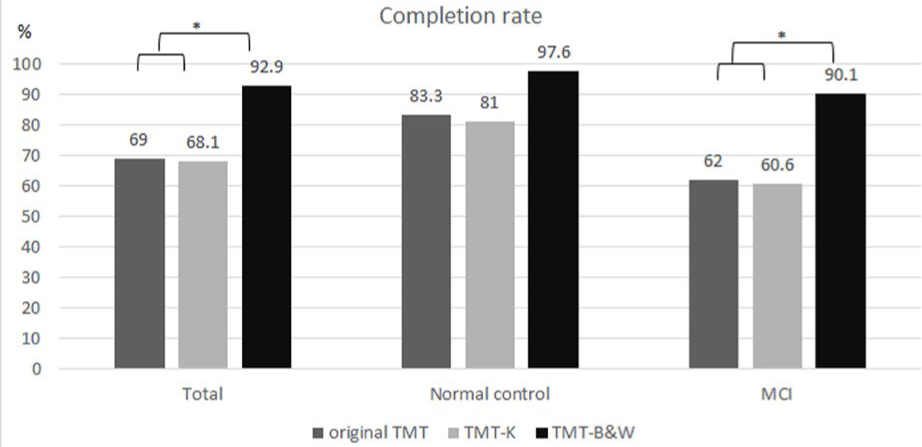
Finally, just 78 subjects out of 113 participants completed the TMT-OR that overall completion rate of TMT-OR was 69% (Figure 2). According to clinical group, 35 subjects out of 42 completed in NC and 44 subjects out of 71 in MCI completed TMT-OR that completion rate were 83.3% and 62%, respectively.
Korean version of trail making test
A significant difference in completion time for the TMT-K was noted between NC and MCI adjusted for age, gender and level of education. (p=0.003 for part A and p<0.001 for part B) (Table 1). Regarding completion of TMT-K, 77 subjects out of 113 completed the TMT-K that overall completion rate of TMT-K was 68.1% that revealed no difference compared with that of TMT-OR (Figure 2). According to clinical group, 34 subjects out of 42 completed in NC and 43 subjects out of 71 in MCI completed TMT-K that completion rate were 81.0% and 60.6%, respectively that showed no significant difference compared with those of TMT-OR.
Trail making test-black and white
Time-to-completion of TMT-B&W-A and B differentiated between NC and MCI adjusted for age, gender and level of education (p<0.001) (Table 1). Regarding completion of TMT-B&W, 105 subjects out of 113 completed the TMT-K that overall completion rate was 92.9% that revealed higher rate compared with that of TMT-OR or TMT-K (Figure 2). According to clinical group, 41 subjects out of 42 completed in NC and 64 subjects out of 71 in MCI completed TMT-B&W that completion rate were 97.6% and 90.1%, respectively that showed significantly higher rate compared with those of TMT-OR or TMT-K in MCI.
We performed a ROC analysis and estimated the area under the curve (AUC) to assess the diagnostic utility of three versions of TMT between MCI and NC. AS described in Table 2, the AUC-ROC were 0.665 and 0.774 for TMT-OR, 0.736 for part B of TMT-K, 0.790 and 0.753 for TMT-B&W. There was no significant difference in AUC value among three versions of TMT.
| AUC | SE | 95%CI | |
|---|---|---|---|
| TMT-OR-A | 0.665 | 0.074 | 0.520-0.809 |
| TMT-OR-B | 0.774 | 0.061 | 0.651-0.891 |
| TMT-K-B | 0.736 | 0.064 | 0.611-0.861 |
| TMT-BW-A | 0.790 | 0.058 | 0.676-0.904 |
| TMT-BW-B | 0.753 | 0.065 | 0.626-0.879 |
Table 2: Comparison of area under curve (AUC) of each version of TMT distinguishing clinical groups.
According to correlation analysis among age, education and each version of TMT, NC revealed no significant correlation whereas negative correlation was observed between TMT performance and age in MCI patients (Table 3).
| NC (n=30) | MCI (n=32) | |||
|---|---|---|---|---|
| Age | Education | Age | Education | |
| TMT-OR-A | 0.282 | 0.308 | 0.488** | -0.041 |
| TMT-OR-B | 0.243 | -0.058 | 0.513** | -0.002 |
| TMT-K-B | 0.276 | 0.007 | 0.576** | -0.046 |
| TMT-B&W-A | 0.192 | 0.206 | 0.423* | -0.077 |
| TMT-B&W-B | 0.230 | -0.105 | 0.470** | 0.077 |
**Statistically significant, p<0.01; *Statistically significant, p<0.05
Table 3: Pearson correlation among education, age and the indices of TMT.
Correlations between Trail Making and other neuropsychological tests
The bivariate analysis of the correlation between the neuropsychological tests scores showed significant coefficients between tests scores (Table 4). TMT-B&W significantly correlated with the TMT-OR or TMT-K. Part B of TMT-B&W also revealed significant correlation with COWAT and Stroop test-Color reading.
| TMT-OR-A | TMT-OR-B | TMT-K-B | TMT-B&W-A | TMT-B&W-B | |
|---|---|---|---|---|---|
| TMT-OR-A | - | 0.583** | 0.625** | 0.586** | 0.532** |
| TMT-OR-B | 0.583** | - | 0.827** | 0.547** | 0.684** |
| TMT-K-B | 0.625** | 0.827** | - | 0.599** | 0.769** |
| TMT-B&W-A | 0.586** | 0.547** | 0.599** | - | 0.559** |
| TMT-B&W-B | 0.532** | 0.684** | 0.769** | 0.559** | - |
| COWAT-S | -0.336** | -0.397** | -0.463** | -0.378** | -0.508** |
| COWAT-P | -0.367** | -0.457** | -0.493** | -0.388** | -0.343** |
| Stroop test-W | -0.049 | -0.057 | -0.073 | -0.068 | -0.123 |
| Stroop test-C | -0.455** | -0.605** | -0.644** | -0.439** | -0.608** |
**Statistically significant, p<0.01; *Statistically significant, p<0.05
Table 4: Correlations among neuropsychological tests scores.
Discussion
One purpose of this study was to determine if the original or Korean version of TMT would suffice for use in the Korean older adult population, or if there is a need for the development of culturefair analogue such as TMT-B&W. Previous study of our team revealed that TMT-B&W is as reliable as original TMT [14] and current study focused on the applicability as a tool for early stage of cognitive decline such as MCI compared to original and Korean version of TMT. The subjects with dementia were carefully excluded, so we think that our data can represent of TMT performance of subtle cognitive decline according to different types of TMT. Although three versions of TMT tasks discriminated between NC and MCI without significant difference of in AUC value, the completion rate was quite different.
In comparison to part A of TMT, part B demands set shifting ability such as cognitive alteration or backward inhibition [8,22,23] that it is known to be more difficult to perform [24]. Regarding completion rate of TMT with Korean and English alphabets, although better performance in writing the Korean alphabet might have been expected, most of the subjects who could not accurately complete the task in English alphabet were also unable to complete the task in Korean, and vice versa. Some previous research [25,26] and this study incorporated highly-educated subjects (mean of 15.32 years, range 9 to 23)who know both of Korean and English alphabet showed difficulty in recalling the order of Korean alphabet as well as English one. So it is possible that knowing alphabet is one thing and knowing the order of alphabet is another that two versions of TMT were inapplicable to about 40% of MCI patients. Considering these low completion rate of both versions of TMT using alphabet, the current study suggests that replacing the English alphabet with Korean letters does not provide greater benefit in detecting early stage of cognitive impairment in older Korean adults. Although the original TMT proved to be an effective tool in differentiation of MCI and NC, it is possible that the application of an alternative TMT such as TMT-B&W is still needed for those who are unable to complete the original English or Korean version of the TMT.
It has shown that cultural variables affect cognitive test performance that a cognitive test does not always measure the same construct when it is applied in a different cultural context [27]. Like other neuropsychological tests, TMT may also have limited utility in crosscultural setting that a number of modified and alternate forms of TMT have been made to overcome the shortcomings of original TMT. Oral TMT does not use pencil and paper and it is performed verbally that was meant to be free from the cultural bias [28,29]. Expanded TMT uses clock faces of different times and black dots of different diameter to systemically varying the stimuli with in the TMT format [30]. Comprehensive TMT with 5 trails was developed to discriminate and detect the normal population from the patient with cognitive difficulty that it is more complex than original TMT [31-36]. The Color Trails Test (CTT) was developed as a culturally fair analogue of the TMT that does not use any letters except Arabic numbers [37]. Although the basic designs of the TMT and CTT are similar, they were not identical because the trace of the trails was different [38]. The Shape Trail Test (STT) includes all numbers (from 1 to 25) twice, once in a circle and once in a square that it is somewhat similar to CTT [39]. Symbol TMT does use neither letters nor numbers that it can be used with people that have no familiarity with the Arabic numeric system or a specific alphabet [40]. Other variants of TMT that used walking [41] or eye tracking [42] instead of line drawing were also introduced as a tool to detect dysexecutive function. On top of all the advantages of these culture fair analogues of TMT variants, TMT-B&W has additional merit that it is composed of the identical trace to original TMT. And it is intuitively applicable to patients with cognitive impairment as a simple but efficient tool by using the contrasting stimuli of black and white circles with Arabic numbers [14]. Although older subjects known to perform significantly more poorly than younger subjects in previous reports with TMT [43-46], the significant negative correlation were observed between TMT performance and age only in the MCI group (Table 3). Considering the age of MCI patients was significantly higher than normal control, the effect of age on TMT performance might need certain threshold level of age that is in line with the result of other study [46]. Higher educational level is also important factor to perform TMT [47,48], but it showed no correlation between educational level and TMT performance in this study (Table 3). We thought that this result derived from the higher educational level of our subjects as it was already reported that the effect of education became apparent only with poorly educated population.
Conclusion
Results of the current study demonstrate that the TMT-B&W as well as other TMT using alphabet proved to be sensitive to mild cognitive decline. Like the original TMT, the TMT-B&W showed a high correlation with other neuropsychological tests that assess frontal executive function. As the TMT-B&W was created to address the need for testing to minimize effects of language that a participant does not need knowledge of the English or Koran alphabet and the trace and the test results showed a pattern consistent with the original TMT. Thus, if a researcher is inclined to control language effects with higher completion rate, the TMT-B&W is recommended in the subjects with cognitive impairment. However, our study had some limitations. Although we tried to control the demographic variables using MANCOVA, the significant differences in age and gender between MCI and NC might have been affected the reliability and reproducibility of the cognitive outcome measures. We do not have standardized large norm study or data outside Korea to be a culture-fair test. And this study was focused on the subjects with relatively higher educational level that further study with undereducated Korean subjects or norm study across different countries would be needed to better determine the potential for more general utilization of the TMT-B&W.
Acknowledgement
We would like to thank the Medical Research Collaborating Center at Seoul National University Bundang Hospital for performing the statistical analyses.
References
- Rabin LA, Barr WB, Burton LA (2005) Assessment practices of clinical neuropsychologists in the United States and Canada: A survey of INS, NAN, and APA Division 40 members. Arch ClinNeuropsychol 20: 33-65.
- Lezak MD (2004) Neuropsychological Assessment. Oxford University Press.
- Reitan RM, Wolfson D (1994) A selective and critical review of neuropsychological deficits and the frontal lobes. Neuropsychol Rev 4: 161-198.
- Strauss E, Sherman EMS, Spreen OA (2006) Compendium of neuropsychological tests: Administration, norms and commentary, Oxford University Press.
- Heun R, Papassotiropoulos A, Jennssen F (1998) The validity of psychometric instruments for detection of dementia in the elderly general population.Int J Geriatr Psychiatry 13: 368-380.
- Kraybill ML, Larson EB, Tsuang DW, Teri L, McCormick WC, et al. (2005) Cognitive differences in dementia patients with autopsy-verified AD, Lewy body pathology, or both. Neurology 64: 2069-2073.
- Walker AJ, Meares S, Sachdev PS, Brodaty H (2005) The differentiation of mild frontotemporal dementia from Alzheimer's disease and healthy aging by neuropsychological tests. IntPsychogeriatr 17: 57-68.
- Crowe SF (1998) The differential contribution of mental tracking, cognitive flexibility, visual search, and motor speed to performance on parts A and B of the Trail Making Test. J ClinPsychol 54: 585-591.
- Anderson CV, Bigler ED, Blatter DD (1995) Frontal lobe lesions, diffuse damage and neuropsychological functioning in traumatic brain-injured patients. J ClinExpNeuropsychol 17: 900-908.
- Stuss DT, Bisschop SM, Alexander MP, Levine B, Katz D, et al. (2001) The trail making test: A study in focal lesion patients. Psychol Assess13: 230-239.
- Seo EH, Lee DY, Kim KW, Lee JH, Jhoo JH, et al. (2006) A normative study of the trail making test in Korean elders. Int J Geriatr Psychiatry 21: 844-852.
- Yi HS, Chin JH (2007) Development andvalidation of Korean version of trail making test for elderly persons. Dementia and Neurocognitive Disorders6: 54-66.
- Park JS, Kang YW, Yi HS, Kim YJ, Ma HI, et al. (2007) Usefulness of the Korean trail making test for the elderly (K-TMT-e) in detecting the frontal lobe dysfunction. Dementia and Neurocognitive Disorders 6: 12-17.
- Kim HJ, Baek MJ, Kim S (2014) Alternative type of the trail making test in non-native English-speakers: The trail making test-black and white. PLoS One 9: e89078.
- Petersen RC (2004) Mild cognitive impairment as a diagnostic entity. J Intern Med 256: 183-194.
- McKhann G, Drachman D, Folstein M, Katzman R, Price D, et al. (1984) Clinical diagnosis of Alzheimer’s disease: Report of the NINCDS-ADRDA work group under the auspices of department of health and human services task force on Alzheimer’s disease. Neurology 34: 939-944.
- Kang Y, Na DL, Hahn S (1997) A validity study on the Korean mini-mental state examination (K-MMSE) in dementia patients. J Korean NeurolAssoc 15: 300-308.
- Kang SJ, Choi SH, Lee BH, Kwon JC, Na DL, et al. (2002) The reliability and validity of the Korean instrumental activities of daily living (K-IADL). J Korean NeurolAssoc 20: 8-14.
- Christensen KJ, Multhaup KS, Nordstrom S, Voss K (1991) A cognitive battery for dementia: Development and measurement characteristics. Psychol Assess J Consult ClinPsychol 3: 168-174.
- Marshall GA, Fairbanks LA, Tekin S, Vinters HV, Cummings JL (2006) Neuropathologic correlates of activities of daily living in Alzheimer disease. Alzheimer Dis AssocDisord 20: 56-59.
- Reitan RM (1955) The relation of the trail making test to organic brain damage. J Consult Psychol 19: 393-394.
- Miner T, Ferraro FR (1998) The role of speed of processing, inhibitory mechanisms and presentation order in trail-making test performance. Brain Cogn 38: 246-253.
- Mayr U, Keele SW (2000) Changing internal constraints on action: The role of backward inhibition. J ExpPsychol Gen 129: 4-26.
- Vickers D, Vincent N, Medvedev A (1996) The geometric structure, construction and interpretation of path-following (trail-making) tests. J ClinPsychol 52: 651-661.
- Gaudino EA, Geisler MW, Squires NK (1995) Construct validity in the trail making test: What makes Part B harder? J ClinExpNeuropsychol 17: 529-535.
- Ivnik RJ, Malec JF, Smith GE, Tangalos EG, Petersen RC (1996) Neuropsychological tests’ norms above age 55: COWAT, BNT, MAE token, WRAT-R reading, AMNART, STROOP, TMT, and JLO. ClinNeuropsychol 10: 262-278.
- Fernández AL, Marcopulos BA (2008) A comparison of normative data for the trail making test from several countries: Equivalence of norms and considerations for interpretation. Scand J Psychol 49: 239-246.
- García-Tuñón MAS (2008) “Trazadosorales”: un test neurológico multicultural con bajosrequerimientosacadémicos. Int J Psychol Res 1: 20-26.
- DeCristoforo L, García-Tuñón MAS (2001) Test verbales-no ligados la lenguajelibre de barreraslingüísticas. Rev EspNeuropsicol 3: 68-82.
- Stanczak DE, Lynch MD, McNeil CK, Brown B (1998) The expanded trail making test: Rationale, development and psychometric properties. Arch ClinNeuropsychol 13: 473-487.
- Homack S, Lee D, Riccio CA (2005) Test review: Delis-Kaplan executive function system. J ClinExpNeuropsychol 27: 599-609.
- Moses J (2002) Comprehensive trail making test (CTMT)By Cecil R. Reynolds. Austin, Texas: PRO-ED, Inc. Arch ClinNeuropsychol 19: 703-708.
- Allen DN, Thaler NS, Ringdahl EN, Barney SJ, Mayfield J (2012) Comprehensive trail making test performance in children and adolescents with traumatic brain injury. Psychol Assess 24: 556-564.
- Bauman Johnson WL, Maricle DE, Miller DC, Allen DN, Mayfield J (2010) Utilization of the comprehensive trail making test as a measure of executive functioning in children and adolescents with traumatic brain injuries. Arch ClinNeuropsychol 25: 601-609.
- Armstrong CM, Allen DN, Donohue B, Mayfield J (2008) Sensitivity of the comprehensive trail making test to traumatic brain injury in adolescents. Arch ClinNeuropsychol 23: 351-358.
- Salthouse TA, Toth J, Daniels K, Parks C, Pak R, et al. (2000) Effects of aging on efficiency of task switching in a variant of the trail making test. Neuropsychology 14: 102-111.
- D’Elia L, Satz P, Uchiyama C, White T (1996) Colortrails test professional manual.
- deFrias CM, Dixon RA, Strauss E (2006) Structure of four executive functioning tests in healthy older adults. Neuropsychology 20: 206-214.
- Zhao Q, Guo Q, Li F, Zhou Y, Wang B, et al. (2013) The shape trail test: Application of a new variant of the trail making test. PLoS One 8: e57333.
- Barncord SW, Wanlass RL (2001) The symbol trail making test: Test development and utility as a measure of cognitive impairment. ApplNeuropsychol 8: 99-103.
- Perrochon A, Kemoun G (2014) Thewalking trail-making test is an early detection tool for mild cognitive impairment. ClinInterv Aging 9: 111-119.
- Hicks SL, Sharma R, Khan AN, Berna CM, Waldecker A, et al. (2013) An eye-tracking version of the trail-making test. PLoS One 8: e84061.
- Kennedy KJ (1981) Age effects on trail making test performance. Percept Mot Skills 52: 671-675.
- Tombaugh TN (2004) Trail making test A and B: Normative data stratified by age and education. Arch ClinNeuropsychol 19: 203-214.
- Abe M, Suzuki K, Okada K, Miura R, Fujii T, et al. (2004) [Normative data on tests for frontal lobe functions: Trail making test, verbal fluency, wisconsin card sorting test (Keio version)]. No to Shinkei 56: 567-574.
- Hashimoto R, Meguro K, Lee E, Kasai M, Ishii H, et al. (2006) Effect of age and education on the trail making test and determination of normative data for Japanese elderly people: the Tajiri Project. Psychiatry ClinNeurosci 60: 422-428.
- Bornstein RA, Suga LJ (1988) Educational level and neuropsychological performance in healthy elderly subjects. DevNeuropsychol 4: 17-22.
- Giovagnoli AR, Del Pesce M, Mascheroni S, Simoncelli M, Laiacona M, et al. (1996) Trail making test: Normative values from 287 normal adult controls. Ital J NeurolSci 17: 305-309.
Relevant Topics
- Advanced Parkinson Treatment
- Advances in Alzheimers Therapy
- Alzheimers Medicine
- Alzheimers Products & Market Analysis
- Alzheimers Symptoms
- Degenerative Disorders
- Diagnostic Alzheimer
- Parkinson
- Parkinsonism Diagnosis
- Parkinsonism Gene Therapy
- Parkinsonism Stages and Treatment
- Stem cell Treatment Parkinson
Recommended Journals
Article Tools
Article Usage
- Total views: 17714
- [From(publication date):
June-2016 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 16535
- PDF downloads : 1179