Case Report Open Access
A Dumbbell-Shaped Extradural Intracanal Cavernous Hemangioma: A Rare Case Report and Review of Literature
Erfan sheikhbahaei and Ali andalib*Erfan sheikhbahaei isfahan university of medical sciences, Iran (Islamic Republic of)
- *Corresponding Author:
- Ali andalib
Erfan sheikhbahaei isfahan university of medical sciences
Iran (Islamic Republic of)
Tel: +98-913-22845859
E-mail: ali_andalib@yahoo.com; erfan.shikhbahaei@gmail.com
Received date: 21, March 2017; Accepted date: 27, March 2017; Published date: 30, March 2017
Citation: Sheikhbahaei E, Andalib A (2017) A Dumbbell-Shaped Extradural Intracanal Cavernous Hemangioma: A Rare Case Report and Review of Literature. J Orthop Oncol 3:116. doi: 10.4172/2472-016X.1000116
Copyright: © 2017 Andalib Ali, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Orthopedic Oncology
Abstract
Cavernous hemangiomas, first described by Globus in 1929, are one of the uncommon vascular malformations of central nervous system. They seemed to have benign vascular structure with dilated vessel bed. Cavernous hemangiomas encompass nearly ‘five’–12% of all spinal vascular malformations; however, existence in the epidural space without bone involvement is rare. Only ‘four’% of all cavernous hemangiomas are merely epidural cavernous hemangiomas. In this case report, we removed a hemorrhagic thoracic mass by T3-T5 laminectomy presenting with neurological deficits mimicking symptoms of intervertebral disk herniation in a 33-year-old male patient who came to our Clinic. We have chosen this case to be reported due to its rare characteristics and occurrence of this type of cavernous hemangioma in the world.
Keywords
Hemangioma; Cavernous hemangioma; Spinal cord; Thoracic vertebra; Extradural; Spine
Introduction
Cavernous Hemangioma is a kind of tumor with dilated blood vessels and considered benign neoplasms [1-3]. They can be located anywhere in the neural axis as well as other part of the body like liver and eyes [3-6]. Evidently, the most reported cases are intracranial and supratentorial [3]. Also Spinal Cavernous Hemangiomas commonly occur in vertebral body extradurally and in some cases extend to spinal canal, which consist of only ‘five’-12% of spinal vascular problems [1-7]. Here we report one of our rare experiences in spinal surgery with dumbbell-shaped cavernous hemangioma extended from intervertebral foramen and left its great part in the canal.
Case Report
A 33-year-old male patient was admitted to our Clinic with gait disturbance and a nonspecific back pain with history of numbness and lack of sensation in his lower limb. Neurological examinations revealed exaggerated deep tendon reflex (DTR), Clonus and positive Babinski sign. No bowel or bladder problems were noted, but he had sensory in level of xiphoid.
As usual, common blood tests ordered. Complete Blood Count, Liver Function Tests and Blood Coagulation Tests were in normal range according to his age and references.
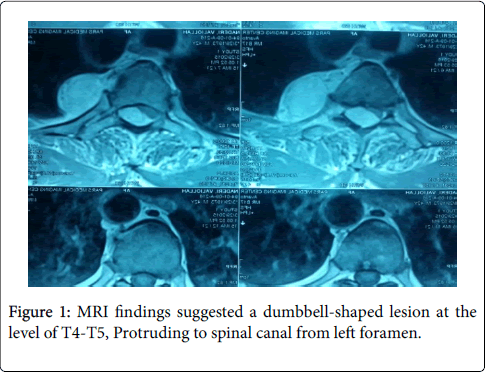
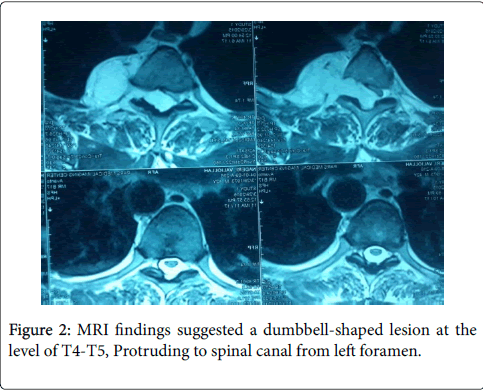
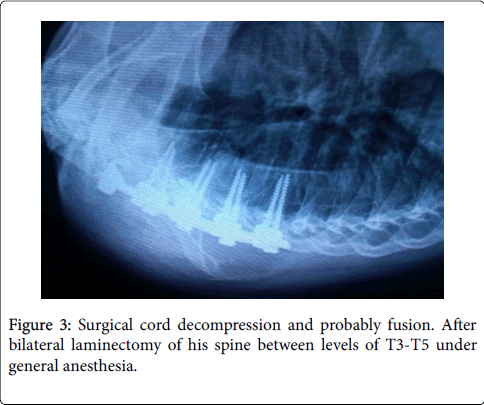
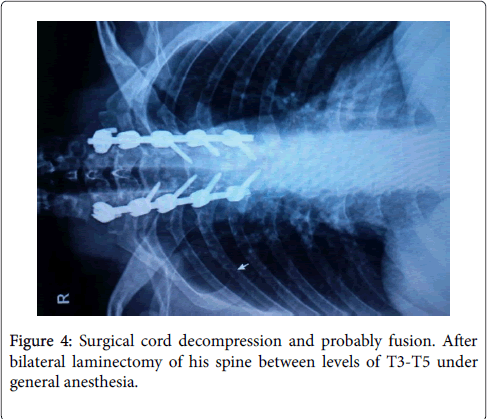
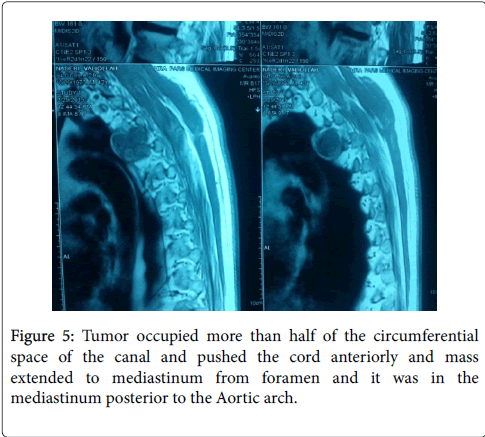
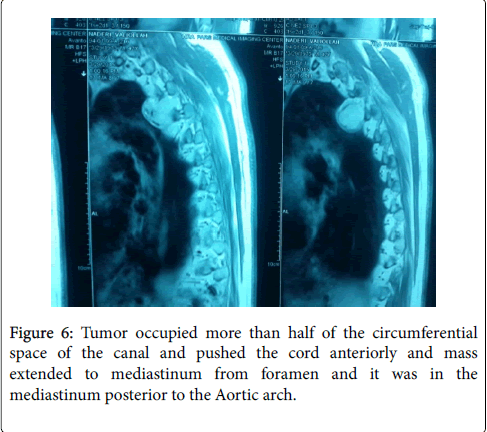
Routine X-rays were normal, therefore MRI was ordered for this patient. MRI findings suggested a dumbbell-shaped lesion at the level of T4-T5, Protruding to spinal canal from left foramen (Figures 1 and 2) [8,9]. Neurofibroma was suspected based on these findings (more common in this part of the world). This patient met the criteria for surgical cord decompression and probably fusion. After bilateral laminectomy of his spine between levels of T3-T5 under general anesthesia (Figures 3 and 4) [10,11], we found that the tumor occupied more than half of the circumferential space of the canal and pushed the cord anteriorly and mass extended to mediastinum from foramen and it was in the mediastinum posterior to the Aortic arch (Figures 5 and 6) [11]. The lesion was soft, red-pink and hemorrhagic, posterior to cord and due to extension to lamina, the bone was very thin. We suspected intracanal cavernous hemangioma instead of Neurofibroma because the tumor was hemorrhagic. The intracanal tumor was removed by microsurgery technique and for complete resection; The T5 nerve root in left side was sacrificed. Part of the tumor in foramen was resected but due to chance of bleeding into the mediastinum, we didn’t resect the mediastinal part of the mass. During the surgery the patient was sFigure and his blood pressure, heart rate and respiratory rate were under continuous control. The lesion was sent to the Pathology Lab for further investigation and revealing whether it was Neurofibroma or Cavernous Hemangioma. The Pathology Lab result confirmed our second diagnosis, Cavernous Hemangioma, composed of large dilated blood-filled vessels. The patient was discharged with good condition and without any neurologic deficit. After 4 weeks he came for routine follow up and the Babinski’s sign was negative, no strong DTR or Clonus observed. Sensory level was disappeared and the gait was normal (Figures 3 and 4) [10,11].
Discussion
In 1929 Globus reported the first Cavernous hemangioma [3,7]. Cavernous hemangiomas are comprised of large, dilated vascular channels. Compared with capillary hemangiomas, cavernous hemangiomas are more infiltrative, commonly involve deep structures, and do not regress spontaneously [2-4,7]. On histologic examination, the mass is sharply defined but not encapsulated and is composed of large, cavernous blood-filled vascular spaces, separated by connective tissue stroma [2-7]. Cavernous hemangiomas detected by imaging studies may be difficult to distinguish from their malignant counterparts, but with the magnetic resonance imaging (MRI), the lesion is more frequently diagnosed than we previously considered [1-7]. Brain hemangiomas are also problematic, as they can cause symptoms related to compression of adjacent tissue or rupture.
Cavernous hemangioma can be found in any part of CNS axis [1,5,7]; some parts more often that others. They can be found in epidural or extradural, spinal or cranial and thoracic or lumbar [1-3,7]. 10-27% of adults suffer from spinal hemangiomas, therefore they are unexpectedly common. ‘Four’% of all spinal epidural lesions are cavernous hemangiomas so evidently they are considered rare problems [3,5,7]. Spinal Cavernous hemangiomas are more common in women (70%) than in men, and the average age is 40 [3,4,7]. Primary location of most cavernous hemangiomas is in vertebral body [1,3,7]. According to recent reports the most located lesions are thoracic with myelopathy as its most occurring symptom, mimicking the disk herniation or nerve root compression. Depending on the location and growth rate, symptoms include local pain, positive neurological tests and slow progressive or acute spinal cord compression [3,5-7]. Presentations of symptoms are usually sudden because cavernous hemangiomas don’t grow by mitotic division; pregnancy, exercise, straining, infections, and trauma are common possibilities in sudden onset of admitting in the hospitals and should be considered in taking patients’ history [3,5]. It has been reported that in some cases cavernous hemangioma shaped like a dumbbell and bulge from intervertebral foramen [5]. The exact site of lesion can be detected with MRI and it is the only useful diagnostic technique, but Neurofibroma, Schwannomas, Lymphomas, extraosseous Ewing’s sarcoma, epidural Angiolipoma and rarely Meningiomas are other possible tumors that should be considered in the differential diagnosis because they appear in the same manner in the MRI, but with specific different characteristics [1,3,5,7]. Schwannomas are epidural, smooth rather that lobulated, commonly in intervertebral foramen and with cystic changes. Lymphomas and Meningiomas have some differences in their MRI characteristics and location [5]. The best way of treating these tumors is surgery with complete resection of mass by the newest technique, however, in some cases it has been reported that the lesion is adjacent to nerve root and could not be resected thoroughly without some parts of the lesion remaining at the site of involvement or sacrificed the specific nerve root [4,5]. However through the first option, there is a risk of recurrence, but according to tumor’s site, size and structure it must be the surgeon’s decision which option to be performed [5]. Furthermore, it was considered in some cases that the surgery was too risky to remove the entire tumor because of its internal structure and chances of massive bleeding or mediastinal damages as it was in our case. Radiotherapy is another option in case of an incomplete removal [3].
Conclusion
Cavernous hemangiomas, which are non-malignant vascular malformations, should be considered in the differential diagnoses of spinal dumbbell-shaped tumors as considering other differential diagnosis like: neurofibroma, lymphoma, meningioma and schwannomas. Its symptoms are non-specific; therefore, it is more difficult to be distinguished in routine history and physical examinations. It shall be treated by microsurgery complete resection if possible using combined approaches of posterior laminectomy for resection of extradural part. A good surgical result with no morbidity and mortality could be achieved.
References
- Goyal A, Singh AK, Gupta V, Tatke M (2002) Spinal epidural cavernous hemangioma: a case report and review of literature. Spinal Cord 40: 200-202.
- Sulochana S, Sundara MM (2012) Cavernous hemangioma of the spinal cord: a rare case. Journal of Clinical and Diagnostic Research: JCDR 6: 1781.
- Sharma MS, Borkar SA, Kumar A, Sharma MC, Sharma BS (2013) Thoracic extraosseous, epidural, cavernous hemangioma: case report and review of literature. Journal of Neurosciences °Rural Practice 4: 309.
- Grasso G, Alafaci C, Granata F, Cutugno M, Salpietro FM, et al. (2014) Thoracic spinal cord cavernous angioma: a case report and review of the literature. Journal of Medical Case Reports 8: 271.
- Jeong WJ, Choi I, Seong HY, Roh SW (2015) Thoracic Extradural Cavernous Hemangioma Mimicking a Dumbbell-Shaped Tumor. Journal of Korean Neurosurgical Society 58: 72-75.
- Padolecchia R, Acerbi G, Puglioli M, Collavoli PL, Ravelli V, et al. (1998) Epidural spinal cavernous hemangioma. Spine 23: 1136-1140.
- Ozkal B, Yaldiz C, Yaman O, Ozdemır N,Dalbayrak S (2015) Extraosseous, epidural cavernous hemangioma with back pain. Polish Journal of Radiology 80: 206.
- Luca D, Marta R, Salima M, Valentina B, Domenico D (2014) Spinal epidural cavernous angiomas: a clinical series of four cases. ActaNeurochir (Wien)156: 283-284.
- Park E, Park J, Kim E (2008) Spinal epidural cavernous angioma. Korean J Spine 5: 2.
- Guthkelch AN (1948)Haemangiomas involving the spinal epidural space. Journal of neurology, Neurosurgery, and Psychiatry11: 199.
- Ogawa R,Hikata T,Mikami S, Fujita N, Iwanami A (2015) Total En Bloc Spondylectomy for Locally Aggressive Vertebral Hemangioma Causing Neurological Deficits. Case Reports in Orthopedics 20: 15.
Relevant Topics
- 3D Printing in Limb-Sparing Surgery
- Adamantinoma
- Aneurysmal Bone Cysts
- Chondrosarcoma
- Chordomas
- Cryosurgery
- Enchondroma
- Ewing’s Sarcoma
- Fibrous Dysplasia
- Giant Cell Tumor of Bone
- Immunotherapy for Osteosarcoma
- Liquid Biopsy in Orthopedic Oncology
- Malignant Osteoid
- Metastatic Bone Cancer
- Molecular Profiling of Bone Tumors
- Multilobular Tumour of Bone
- Orthopaedic Oncology
- Osteocartilaginous Exostosis
- Osteochondrodysplasia
- Osteoma
- Osteonecrosis
- Osteosarcoma
- Primary Bone Tumors
- Sarcoma
- Secondary Bone Tumours
- Targeted Therapy in Bone Sarcomas
- Tumours of Bone
Recommended Journals
Article Tools
Article Usage
- Total views: 4463
- [From(publication date):
March-2017 - Jul 23, 2025] - Breakdown by view type
- HTML page views : 3554
- PDF downloads : 909