Research Article Open Access
A Pediatric Infection Screening System with a Radar Respiration Monitor for Rapid Detection of Seasonal Influenza among Outpatient Children
| Guanghao Sun1, Yu Yao2, Ritsu Yoshinaka3, Mayumi Ikegami4, Seokjin Kim1, Michael Schiek2 and Takemi Matsui1* | ||
| 1Graduate School of System Design, Tokyo Metropolitan University, Japan | ||
| 2Central Institute ZEA-2–Electronic Systems, Research Center Jülich, Germany | ||
| 3Ritsu Pediatric Dental Clinic, 1-8-7 Honda, Kokubunji, Tokyo 185-0011, Japan | ||
| 4Nishi-kokubunji Clinic, 3-24-3 Nishi-koigakubo, Kokubunji, Tokyo 185-0013, Japan | ||
| Corresponding Author : | Takemi Matsui Graduate School of System Design Tokyo Metropolitan University 6-6 Asahigaoka, Hino, Tokyo 191-0065, Japan Tel: +81 42 585 8669 Fax: +81 42 585 8467 E-mail: tmatsui@tmu.ac.jp |
|
| Received June 26, 2014; Accepted September 09, 2014; Published September 15, 2014 | ||
| Citation: Sun G, Yao Y, Yoshinaka R, Ikegami M, Kim S, et al. (2014) A Pediatric Infection Screening System with a Radar Respiration Monitor for Rapid Detection of Seasonal Influenza among Outpatient Children. J Infect Dis Ther 2:163. doi:10.4172/2332-0877.1000163 | ||
| Copyright: © 2014 Sun G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | ||
Related article at Pubmed Pubmed  Scholar Google Scholar Google |
||
Visit for more related articles at Journal of Infectious Diseases & Therapy
Abstract
Background: Seasonal influenza virus outbreaks cause annual epidemics, mostly during winter in temperate zone countries, especially resulting in increased morbidity and higher mortality in children. In order to conduct rapid screening for influenza in pediatric outpatient units, we developed a pediatric infection screening system with a radar respiration monitor.
Methods: The system conducts influenza screening within 10 seconds based on vital signs (i.e., respiration rate monitored using a 24 GHz microwave radar; facial temperature, using a thermopile array; and heart rate, using a pulse photosensor). A support vector machine (SVM) classification method was used to discriminate influenza children from healthy children based on vital signs. To assess the classification performance of the screening system that uses the SVM, we conducted influenza screening for 70 children (i.e., 27 seasonal influenza patients (11 ± 2 years) at a pediatric clinic and 43 healthy control subjects (9 ± 4 years) at a pediatric dental clinic) in the winter of 2013-2014.
Results: The screening system using the SVM identified 26 subjects with influenza (22 of the 27 influenza patients and 4 of the 43 healthy subjects). The system discriminated 44 subjects as healthy (5 of the 27 influenza patients and 39 of the 43 healthy subjects), with sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV) of 81.5%, 90.7%, 84.6%, and 88.6%, respectively.
Conclusion: The SVM-based screening system achieved classification results for the outpatient children based on vital signs with comparatively high NPV within 10 seconds. At pediatric clinics and hospitals, our system seems potentially useful in the first screening step for infections in the future.
| Keywords |
| Influenza; Pediatric; Outpatient; Infection control; Microwave radar |
| Introduction |
| Seasonal influenza causes an annual epidemic in wintertime and frequently elevates children’s risk of developing acute respiratory infection [1]. Such influenza-related infections not only result in increased mortality but also in increased morbidity in this age group [2,3]. During an epidemic season, rapid screening for influenza and isolating suspected patients in pediatric outpatient units will be effective in reducing the risk of secondary infection. To meet this need, we developed a pediatric infection screening system based on vital signs for pediatric outpatient settings. |
| We previously developed an infection screening system for medical inspection using multiple vital signs (i.e., heart rate, respiration rate, and facial temperature) and evaluated the possibility of applying it in clinical practice at the Japan Self-Defense Forces Central Hospital [4-6]. By using the three vital signs, the sensitivity of the system was improved to higher than 88% in case control studies. However, the main limitation of our previous studies was that they were conducted in a specialized hospital with patients in a limited age group (range, 19-40 years). Therefore, in present study, we focus on investigating the usefulness of the system in children with ages ranging from 4 to 15 years. To apply the system in pediatric outpatient units, we redesigned our previous system to improve its usefulness. Moreover, we included a new algorithm for predicting the occurrence of influenza using the measured vital signs based on the support vector machine (SVM) classification [7]. We tested the system at the Nishi-kokubunji Clinic and Ritsu Pediatric Dental Clinic during the 2013-2014 influenza seasons in Tokyo, Japan. |
| Materials and Methods |
| An Overview of the Pediatric Infection Screening System |
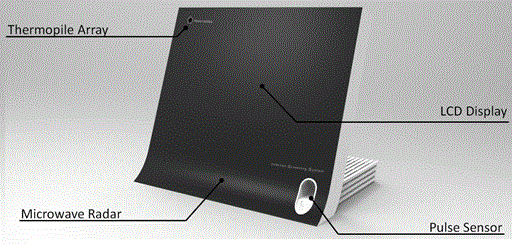
| The configuration of the pediatric infection screening system is shown in Figure 1. The system consists of three biosensors, namely a small-pixel and compact thermopile array to measure facial skin temperature (Chino, Tokyo, Japan) [8], a 24 GHz microwave radar (New-JRC, Tokyo, Japan) to measure respiration rate in a noncontact manner [9], and a pulse photosensor (Sparkfun Electronics, Colorado, USA) to measure heart rate. A 13-inch liquid crystal display (LCD) and a single-board computer were embedded in the system. Moreover, an analog-to-digital converter (National Instruments, Texas, USA) was used to convert the related biosignals from the sensor components to digital and then send them to the computer for data analysis and display. The system is powered by a 19-V wall plug AC/DC adapter or a battery. |
| A Support Vector Machine Classification Method to Predict the Occurrence of Influenza |
| The use of the support vector machine (SVM) is a popular method for binary classification. In binary classification, one receives a set of training data points, each of which belongs to one of two possible classes. The task is to train a classifier, who finds the class labels of the test data, given that the test data are new and unlabeled. In our case, the two classes are infected and not infected. |
| The SVM is a sparse method. This means that the SVM will only use the most informative part of the training data and ignore the remaining data. This reduces computational complexity when classifying new test data points. |
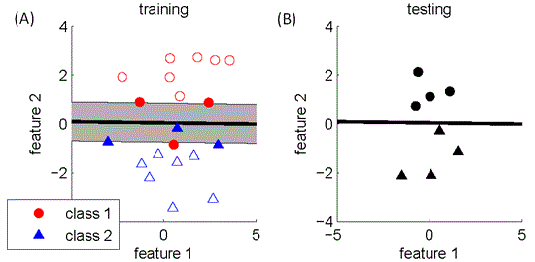
| During training, the SVM will select part of the training data points. The selected data points are called support vectors (SVs) and define a decision boundary. This is illustrated in Figure 2A using a two-dimensional toy example. In the figure, the SVs are highlighted by filled circles and triangles, and the thick black line represents the decision boundary. |
| The decision boundary is calculated as follows: First, the SVM tries to find a boundary that clearly separates the two classes and maximizes the distance of the SVs to the boundary. This distance is called the margin and is marked in gray in Figure 2A. If no such boundary exists, the SVM will allow some data points to lie in the margin or even on the wrong side of the boundary. The topmost triangle and lowest circle in Figure 2A are examples of this case. However, each point on the margin or wrong side of the boundary incurs a penalty. The optimum decision boundary is chosen as the one with the least penalty. |
| The data points not selected as SVs are so far away from the decision boundary that even if they were taken into account, the decision boundary would not change. |
| After optimization, the SVM uses the boundary to classify new test data points. This is illustrated in Figure 2B, where test data points above the boundary are labelled as class 1 and points below the boundary are labelled as class 2. |
| A more detailed description of the SVM and mathematical tools used for optimizing the boundary can be found in many textbooks [7]. |
| Clinical Tests in Pediatric Outpatient Units |
| This study was designed as a cross-sectional investigation at the Nishi-kokubunji Clinic and Ritsu Pediatric Dental Clinic (both located in Tokyo) from September 11, 2013, to March 1, 2014. The data collection was conducted at the Nishi-kokubunji Clinic for seasonal influenza patients and at the Ritsu Pediatric Dental Clinic for healthy control subjects. The influenza patients in this study included 27 patients (16 boys and 11 girls) diagnosed with seasonal influenza. The mean age of the patients was 11 years (range, 7-15 years). Their mean axillary body temperature was 38.2 ± 0.9°C (36.1°C ≤ axillary temperature ≤ 39.8°C). The 43 healthy control subjects (25 boys and 18 girls) in this study included those who visited the Ritsu Pediatric Dental Clinic with no symptoms of fever, headache, or sore throat. Their mean age was 9 years (range, 4-15 years). Their mean axillary body temperature was 36.4 ± 0.3°C (35.8°C ≤ axillary temperature ≤ 37.1°C). |
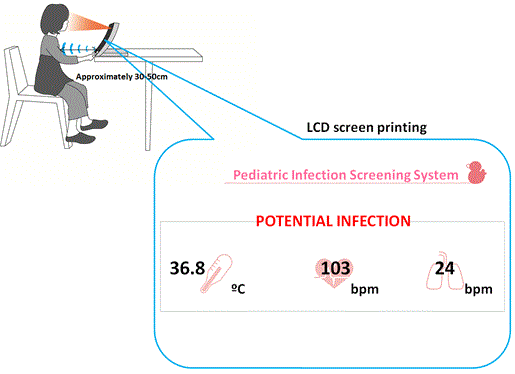
| Measurements using the newly developed pediatric infection screening system were performed for the above-mentioned influenza patients at the Nishi-kokubunji Clinic, whereas measurements using the previous system were performed for the healthy control subjects at the Ritsu Pediatric Dental Clinic. It must be noted, however, that although we used different prototype systems, the embedded biosensors were the same. As shown in Figure 3, the subject was seated at a distance (approximately 30-50 cm) away from the system for 10 seconds, the related biosignals were recorded, and then the facial temperature, respiration rate, heart rate, and screening results (“PASS” or “POTENTIAL INFECTION”) were displayed on the LCD screen. The axillary body temperatures were measured using a contact-type clinical thermometer (Terumo, Tokyo, Japan) for both influenza patients and healthy control subjects. The present study was approved by the Committee on Human Research of the Faculty of System Design, Tokyo Metropolitan University. This study included children aged between 4 and 15 years whose parents were fully informed of the purposes and procedures of the study before giving their written consent to participate. |
| Results |
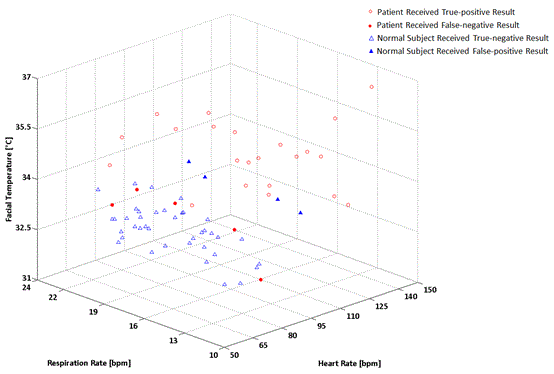
| The three vital signs measured (i.e., facial temperature, respiration rate, and heart rate) were used as inputs to the SVM. Leave-one-out cross-validation was used to assess the performance of the SVM classification and avoid overfitting [7]. The SVM parameters of cost and gamma were chosen by minimizing the leave-one-out error. The optimum values for cost and gamma were 3.0 and 6.5, respectively. Figure 4 shows the screening results of the SVM in a three-dimensional scatter plot. The 70 subjects were classified into either an influenza or healthy group. The screen results of the system showed that of the 27 influenza patients, 22 received true positive screening results (indicated by the red open circle), whereas 5 received false-negative screening results (indicated by the red closed circle). Of the 43 healthy control subjects, 39 received true negative screening results (indicated by the blue open triangle), whereas 4 received false-positive results (indicated by the blue closed triangle). Thus, the corresponding sensitivity, specificity, positive predictive value, and negative predictive value were 81.5%, 90.7%, 84.6%, and 88.6%, respectively. Moreover, the vital signs were compared between the influenza and healthy control groups. Significant differences (p<0.01) in facial temperature, respiration rate, and heart rate were found between the two groups. In particular, the mean heart rate of the influenza patients (95.6 ± 23.1 bpm) was 13.2 bpm faster than that of the healthy control subjects (82.4 ± 13.4 bpm). |
| Discussion |
| Seasonal influenza is a serious public health problem, which causes huge economic loss in healthcare services and families annually [10,11]. Children younger than 5 years and the elderly older than 65 years were associated with a significantly higher risk for severe influenza outcomes [12,13]. During an epidemic season, rapid screening for influenza patients at outpatient units can prevent the spread of the infection and secondary infection. Therefore, we designed a pediatric infection screening system based on vital signs. |
| In the present study, we redesigned our previous system to improve its usefulness and investigated the performance of the new system in outpatient children. The system showed a sensitivity of 81.5%, which was higher than the sensitivity reported in some recent studies on fever-based screening using infrared thermography [14]. Considering that not only body temperature but also heart and respiration rates increase as aftereffects of infectious diseases such as influenza, we designed our system to monitor these three vital signs to improve its sensitivity in detecting infected patients. Therefore, some of the patients had lower facial temperatures, but they were still classified into the influenza group. Moreover, by evaluating the system in outpatient children, we found that the vital signs, especially the heart rate, vary according to age. For instance, in the present study, the mean heart rate was 95.6 bpm for the influenza group and 82.4 bpm for the healthy control group, with the age ranging from 4 to 15 years. By contrast, in our previous study [4], the mean heart rate was 90 bpm for the influenza group and 66 bpm for the healthy control group, with the ages ranging from 19 to 40 years. This result suggests that different discriminant functions must be used to predict infected individuals, depending on their age. Therefore, it is important to accumulate data from people of various ages. |
| The SVM-based pediatric infection screening system achieved 10 seconds of screening of outpatient children based on vital signs. The system is potentially useful for rapid influenza screening in pediatric outpatient units during the epidemic season. |
| Authors’ contributions |
| Study concept and design: GS, SK, and TM; Acquisition of data: RY and MI; Analysis and interpretation of data: GS, YY, MS, and TM; Drafting of the manuscript: GS, YY, and TM |
| Acknowledgment |
| This research was supported by the Tokyo Metropolitan Government Asian Human Resources Fund and the Japan Society for the Promotion of Science Research Fellowships for Young Scientists. We would also like to thank Ms. Saeko Nozawa at Tokyo Metropolitan University for her help in the drafting of this manuscript. |
References
- Ruf BR, Knuf M (2014) The burden of seasonal and pandemic influenza in infants and children. Eur J Pediatr 173: 265-276.
- Kesson AM (2007) Respiratory virus infections. PaediatrRespir Rev 8: 240-248.
- Kang JH (2014) Effectiveness and safety of seasonal influenza vaccination in children with underlying respiratory diseases and allergy. Korean J Pediatr 57: 164-170.
- Matsui T, Hakozaki Y, Suzuki S, Usui T, Kato T, et al. (2010) A novel screening method for influenza patients using a newly developed non-contact screening system. J Infect 60: 271-277.
- Sun G, Hakozaki Y, Abe S, Vinh NQ, Matsui T (2012) A novel infection screening method using a neural network and k-means clustering algorithm which can be applied for screening of unknown or unexpected infectious diseases. J Infect 65: 591-592.
- Matsui T, Suzuki S, Ujikawa K, Usui T, Gotoh S, et al. (2009) Development of a non-contact screening system for rapid medical inspection at a quarantine depot using a laser Doppler blood-flow meter, microwave radar and infrared thermography. J Med EngTechnol 33: 403-409.
- Bishop C (2006) Pattern recognition and machine learning. Springer Press, ISBN: 9780387310732
- Sun G, Saga T, Shimizu T, Hakozaki Y, Matsui T (2014) Fever screening of seasonal influenza patients using a cost-effective thermopile array with small pixels for close-range thermometry. Int J Infect Dis 25: 56-58.
- Lin JC (1975) Noninvasive microwave measurement of respiration. Proc IEEE 63: 1530.
- Principi N, Esposito S, Marchisio P, Gasparini R, Crovari P (2003) Socioeconomic impact of influenza on healthy children and their families. Pediatr Infect Dis J 22: S207-210.
- Halder N, Kelso JK, Milne GJ (2014) A model-based economic analysis of pre-pandemic influenza vaccination cost-effectiveness. BMC Infect Dis 14: 266.
- Neuzil KM, Zhu Y, Griffin MR, Edwards KM, Thompson JM, et al. (2002) Burden of interpandemic influenza in children younger than 5 years: a 25-year prospective study. J Infect Dis 185: 147-152.
- Lee SS, To KW, Wong NS, Choi KW, Lee KC (2014) Comparison of the characteristics of elderly influenza patients in two consecutive seasons. Int J Infect Dis 24: 40-42.
- Chiang MF, Lin PW, Lin LF, Chiou HY, Chien CW, et al. (2008) Mass screening of suspected febrile patients with remote-sensing infrared thermography: alarm temperature and optimal distance. J Formos Med Assoc 107: 937-944.
Tables and Figures at a glance
 |
 |
 |
 |
|||
| Figure 1 | Figure 2 | Figure 3 | Figure 4 |
Relevant Topics
- Advanced Therapies
- Chicken Pox
- Ciprofloxacin
- Colon Infection
- Conjunctivitis
- Herpes Virus
- HIV and AIDS Research
- Human Papilloma Virus
- Infection
- Infection in Blood
- Infections Prevention
- Infectious Diseases in Children
- Influenza
- Liver Diseases
- Respiratory Tract Infections
- T Cell Lymphomatic Virus
- Treatment for Infectious Diseases
- Viral Encephalitis
- Yeast Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 15351
- [From(publication date):
October-2014 - Aug 15, 2025] - Breakdown by view type
- HTML page views : 10704
- PDF downloads : 4647
