Case Report Open Access
A Remarkable Pitfall in Inguinal Open Mesh Herniorrhaphy
Zwaans WAR1*, Scheltinga MRM1,2 and Roumen RMH1,2
1Department of General Surgery, Máxima Medical Centre, Veldhoven/Eindhoven, The Netherlands
2SolviMáx, Centre of Excellence for Abdominal Wall and Groin Pain, Eindhoven, The Netherlands
- *Corresponding Author:
- Zwaans WAR
Maxima Medisch Centrum
General Surgery, De Run 4600
P.O. Box 7777, Veldhoven
5500 MB, The Netherlands
Tel: 0031630548248
E-mail: willemzwaans@gmail.com
Received date: August 19, 2015 Accepted date: September 14, 2015 Published date: September 21, 2015
Citation: Zwaans WAR, Scheltinga MRM, Roumen RMH (2015) A Remarkable Pitfall in Inguinal Open Mesh Herniorrhaphy. J Gastrointest Dig Syst 5:343. doi:10.4172/2161-069X.1000343
Copyright: © 2015 Zwaans WAR, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
A patient was referred to SolviMáx, our 'centre of excellence for chronic abdominal wall and groin pain' because of persistent inguinodynia after a Lichtenstein repair. A surgical exploration revealed a spermatic cord that was divided by the mesh, supposedly during the primary repair. As a consequence, the patient had developed severe neuropathic pain originating from a damaged genitofemoral nerve. Following a tailored neurectomy, he became pain free.
Keywords
Hernia; Inguinal herniorrhaphy pain; Postoperative surgical mesh
Introduction
Inguinal herniorrhaphy is one of the most frequently performed procedures in general surgery [1]. In Europe, the majority of adult inguinal hernias is still repaired by open mesh approach such as a Lichtenstein technique [2]. This evidence based operation is thoroughly investigated and universally recommended for unilateral hernia repair by international guidelines [2]. Although the sequence of surgical steps of this Lichtenstein approach is well documented, pitfalls are potentially looming. Results of a questionnaire completed by Dutch surgeons and surgical residents demonstrated that more than half actually does not implement all of the surgical steps as described by the Lichtenstein Hernia Institute [3]. Specific attention should be paid to the inguinal nerves and the spermatic cord to prevent untoward damage leading to persistent postoperative pain. Therefore, deviating from this suggested road map may result in specific complications.
A patient was referred to SolviMáx, our ‘centre of excellence for chronic abdominal wall and groin pain’ because of persistent inguinodynia after a Lichtenstein repair. A surgical exploration revealed a spermatic cord that was divided by the mesh, supposedly during the primary repair. As a consequence, the patient had developed severe neuropathic pain originating from a damaged genitofemoral nerve. Following a tailored neurectomy, he became pain free.
Case Report
A 52-year-old man presented with severe groin pain that started immediately after a Lichtenstein hernia repair six months previously in another hospital. His level of pain as scored using a Numerical Rating Scale was 8-9 on a 0-10 scale. Pain worsened during exercise, during flexion of the hip, during micturition and following sexual activity (dysejaculation) [4]. At physical examination, signs of neuropathic pain (hyperpathy, allodynia) in the right groin area as well as the area of the right testicle and right upper leg were found. Extreme tenderness was present along the entire length of the spermatic cord. Slight traction onto the scrotum even intensified this severe pain. In addition, hypoalgesia was present in the right hemiscrotum and medial upper leg. The patient was diagnosed with an entrapment of the genital branch of the genitofemoral nerve. A lidocaine injection into the most painful spot in the groin offered a 50% albeit temporary relief.
Following informed consent, an open exploration under general anaesthesia via the prior groin incision demonstrated a congested and obstructed but small spermatic cord. After releasing a ventrolateral portion of the cord, the mesh was lifted exposing a second portion of the spermatic cord. The mesh apparently had split the duct into two halves. In these remains, an oedematous genitofemoral nerve was identified that was trapped between the mesh and the pubic bone. A tailored neurectomy of the nerve was performed and the mesh was partially removed. However, the medial part of the mesh was left in situ to prevent a recurrence. Postoperatively, the patient was immediately pain free and recovered uneventful. Histopathological examination of the resected specimen did not showed traumatic neuroma formation of the nerve.
Discussion
A host of papers alert surgeons regarding difficulties that may be encountered during a Lichtenstein hernia repair. Known pitfalls include a too tight mesh fixation, periostitis by placement of sutures too close to the pubic bone and ilioinguinal nerve damage. Amid (2004) described the key principles of the Lichtenstein tension-free herniorrhaphy as a step-by-step guideline for surgeons [5]. His main message was that, despite the procedure is easy to learn, perform and teach, some key principles must always be respected in order to obtain success [5]. A recent report, however, suggests that just half of the surgeons followed all of these consecutive steps [3]. If these Lichtenstein guidelines are ignored, some form of groin pain may potentially occur.
In the present case, we found a spermatic cord that was split during the index surgical procedure, while the mesh was placed over the medial portion causing severe inguinodynia. This cause of groin pain is, to our knowledge, not earlier described. In 1984, when the first Lichtenstein first tension-free herniorrhaphy was proposed, description of the technique did not allow for a careful dissection of the genitofemoral nerve [5]. It was even advised to separate the genital branch and external spermatic vessels from the rest of the cord. In fact, attention was mainly paid to preservation of the duct, the testicular artery and the ilioinguinal nerve. As a consequence, the so-called ‘lesser cord’ (genitofemoral nerve and external spermatic vessels) was at risk of being entrapped underneath the mesh that was placed over the pubic bone. This approach may have resulted in persistent inguinodynia in some patients [5]. This splitting technique was subsequently abandoned (Figure 1).
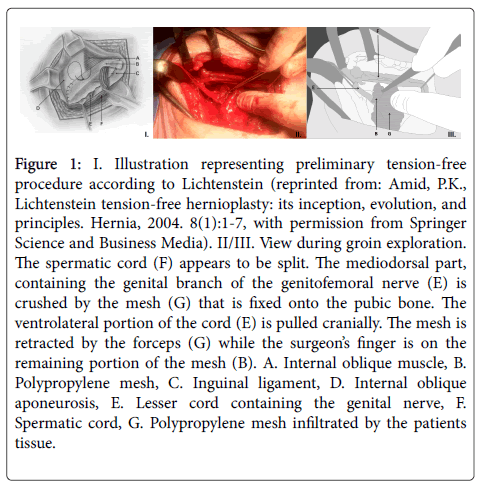
Figure 1: I. Illustration representing preliminary tension-free procedure according to Lichtenstein (reprinted from: Amid, P.K., Lichtenstein tension-free hernioplasty: its inception, evolution, and principles. Hernia, 2004. 8(1):1-7, with permission from Springer Science and Business Media). II/III. View during groin exploration. The spermatic cord (F) appears to be split. The mediodorsal part, containing the genital branch of the genitofemoral nerve (E) is crushed by the mesh (G) that is fixed onto the pubic bone. The ventrolateral portion of the cord (E) is pulled cranially. The mesh is retracted by the forceps (G) while the surgeon’s finger is on the remaining portion of the mesh (B). A. Internal oblique muscle, B. Polypropylene mesh, C. Inguinal ligament, D. Internal oblique aponeurosis, E. Lesser cord containing the genital nerve, F. Spermatic cord, G. Polypropylene mesh infiltrated by the patients tissue.
Identification and preservation of all three inguinal nerves (ilioinguinal, iliohypogastric and genitofemoral nerve) are nowadays considered important steps in the prevention of postoperative groin pain. Wijsmuller and co-authors also concluded that most respondents of a questionnaire on hernia surgical techniques were not sufficiently experienced with the neuro-anatomy of the groin [3]. Incomplete knowledge of the inguinal anatomy can result in debilitating groin pain due to nerve injury. The present case demonstrates that inadequate freeing of the entire spermatic cord prior to dorsal mesh placement can result in separation of the genitofemoral nerve from this cord, leaving it onto the pubic region. The mesh is then placed (and often fixed) onto the nerve possibly leading to an immediate postoperative severe neuropathic groin pain
Conclusion
Performing a Lichtenstein hernia repair requires meticulous dissection according to a set of key steps including nerve identification. If not, inguinodynia may occasionally occur. The number of patients with persistent groin pain following a standard open repair is still over 10 percent [6]. If, before mesh placement, the spermatic cord is not complete freed from its surroundings, entrapment of the genital branch of the genitofemoral nerve may occur that most likely results in persistent groin pain.
References
- Sarosi GA, Wei Y, Gibbs JO, Reda DJ, McCarthy M, et al. (2011) A clinician's guide to patient selection for watchful waiting management of inguinal hernia.Ann Surg 253: 605-610.
- Simons MP, Aufenacker T, Bay-Nielsen M, Bouillot JL, Campanelli G, et al. (2009) European Hernia Society guidelines on the treatment of inguinal hernia in adult patients.Hernia 13: 343-403.
- Wijsmuller AR, Lange JF, van Geldere D, Simons MP, Kleinrensink GJ, et al. (2007) Surgical techniques preventing chronic pain after Lichtenstein hernia repair: state-of-the-art vs daily practice in the Netherlands.Hernia 11: 147-151.
- Verhagen T, Loos MJ, Scheltinga MR, Roumen RM (2015) Surgery for chronic inguinodynia following routine herniorrhaphy: beneficial effects on dysejaculation.Hernia.
- Amid PK (2004) Lichtenstein tension-free hernioplasty: its inception, evolution, and principles.Hernia 8: 1-7.
- Nienhuijs S, Staal E, Strobbe L, Rosman C, Groenewoud H, et al. (2007) Chronic pain after mesh repair of inguinal hernia: a systematic review.Am J Surg 194: 394-400.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 14183
- [From(publication date):
October-2015 - Aug 23, 2025] - Breakdown by view type
- HTML page views : 9598
- PDF downloads : 4585