Research Article Open Access
Accuracy of Self-reported Height and Weight in low-income, Rural African American Children
Leah E Robinson*, Richard R Suminski, Kara K Palmer, J Megan Irwin, and Gabriela PerezAuburn University, Kinesiology, 301 Wire Road, Auburn, AL 36849, USA
- *Corresponding Author:
- Leah E Robinson
Auburn University, Kinesiology, 301 Wire Road
Auburn, AL 36849, USA
Tel: 3348448055
Fax: 3348441467
E-mail: ler0004@auburn.edu
Received Date: May 13, 2014; Accepted Date: June 16, 2014; Published Date: June 23, 2014
Citation: Robinson LE, Suminski RR, Perez G, Palmer KK, Irwin JM (2014) Accuracy of Self-reported Height and Weight in low-income, Rural African American Children. J Child Adolesc Behav 2:144. doi:10.4172/2375-4494.1000144
Copyright: © 2014 Robinson LE, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Child and Adolescent Behavior
Abstract
Objective: To validate self-report anthropometric data in a sample of low-income, rural African American youth. Methods: Ninety-two youth, 10.16 ± 0.85 years of age, were recruited from one school in a rural area of the southeast U.S. Youth were asked to self-report height and weight prior to having their height and weight measurements recorded by trained researchers. Body Mass Index (BMI) was calculated and BMI percentile rank (BMIpct) were used to classify adolescents as non-overweight/obese or overweight/obesity. Differences between measured and self-reported values were assessed using paired t-tests, and differences between weight categories were examined with independent t-tests. Agreement between classification of overweight/obesity by self-report and measured values was assessed using Chi Square. Results: Self-report and measured weight, but not height, differed significantly with the self-reported weight value being 3.1 kg lower than the measured value. Neither height nor weight differed between methods for nonoverweight/ obese youth. For overweight/obese youth, height values were similar but weight values differed between methods (p<0.001) with overweight/obese youth under-reporting their weight to a greater extent than nonoverweight/ obese youth (-8.3 + 9.9 vs. -0.74 + 5.0; p<0.001). The prevalence of overweight/obesity from measured values was 31.5% compared to 30.4% from self-reported values. However, the sensitively was low (58.6%) because of overweight/obese youth’s inability to accurately self-report their weight. Conclusion: The use of self-reported heights and weights for deriving estimates of overweight/obesity rates in lower-income, rural African American youth was not supported by this study
Keywords
Obesity; Epidemiology; Prevalence; Measurement; Validation; Methodology
Introduction
Height and weight are important anthropometric measures used to derive age and gender specific body mass index (BMI) percentiles in youth (i.e., children and adolescents). If they are categorized as overweight or obese, their risk of chronic health issues is greatly increased [1-3]. For example, a review of 63 studies conducted by Friedeman and colleagues [4] indicated that overweight and obese children had significantly higher/increased blood pressure (systolic, diastolic, and 24 h ambulatory), total cholesterol, triglycerides, fasting insulin (obese only), insulin resistance (obese only), and left ventricular mass compared with normal weight children.
Height and weight are typically assessed in-person using specialized equipment. However, in epidemiological studies on youth, measuring anthropometrics is not often feasible, necessitating the use of self-reported heights and weights [5,6]. Evidence suggests that weight status (e.g., overweight) derived from self-reported heights and weights is related to adverse events such as suicide and poor health outcomes [7,8]. Despite these findings, little is known about discrepancies between self-report and measured heights and weights in youth. According to some studies, it is common to see misclassification of weight status based on BMI due to underreporting of weight [5,9-11]. The underestimating of weight may be associated with several factors including weight perception, sex, socio-economic status, and weight status [5,6,10,12-14]. Recently, Kreatsoulas et al. [9] determined the accuracy of self-reported height and weight measures in urban adolescents and young adults. Findings support that this population could accurately report their height and weight leading to a reliable BMI measure.
However, there is a need to extend upon these findings to further advance the literature along with the need to address this question in a more diverse population. African American youth living in low-income, rural areas of the U.S. are at-risk for obesity and related diseases [1,2,12,14,15]. The use of self-reported heights and weights would be very useful in this population; however, no studies have examined the validity of this approach, which is especially relevant for this group [12-14]. Therefore, the purpose of the current study was to establish the validity of self-reported height and weight in a sample of low-income African American youth residing in a rural area of the southeastern U.S.
Methods
Design: This cross-sectional study was part of a cohort study that assessed stages of behavior change for physical activity and healthy eating behaviors in rural pre-adolescent youth. According to the most recent US Census, participants were from a rural area and all attended a single elementary school located in the southeastern region of the United States.
Participants: At time of data collection, the school enrolled 316 students (52% females, 48% males) in grades K-6. Non-Hispanic Blacks (85%) were the predominant racial/ethnic group that attended the school. For this study, participants included youth enrolled in 4 – 6th grade (N=92, M age=10.16 ± 0.85 years; 58.7% female). A recruitment letter and consent/assent form was distributed to the caregivers of each student. Parental consent and child assent were obtained in accordance with the project protocol approved by the Institutional Review Board at Auburn University. Date of birth and race/ethnicity data was collected from school records. Data collection for the specific measures used in this study occurred over a span of 2.5 weeks.
Procedures: To eliminate any bias, self-reported and measured heights and weights were assessed during the participants’ physical education period on two separate days. On day one, they completed questionnaires in private and were asked to report their current height and weight as well as sex, date of birth, and race/ethnicity. Date of birth was confirmed with school records. On day two, measured heights and weights were collected by two trained researchers. The same researchers and equipment were used to collect all anthropometric measures. Additionally to ensure the reliability of measured weights, the scale was calibrated against 100 kg weight at the beginning of each data collection day.
Measures: Participants were asked to record their current height in inches (in) and weight in pounds (lb) on a data collection form, which was not visible to other participants or staff. Height measurements were made with a stadiometer (SECA Model 213) to the nearest 0.1 cm. Weight was recorded to the nearest 0.1 kg using a SECA Model 769 Digital Medical Scales (SECA Scale Corp, Munich, Germany). Shoes, coats, and other heavy outerwear were removed for all measurements. Participants were instructed to stand with their head aligned in the Frankfurt plane with shoulders relaxed and arms hanging freely by their sides as the measurements were being completed.
BMI Classification: Both self-reported and measured anthropometrics were used to calculate BMI according to the sex and age-specific growth charts for each participant. In accordance with the Centers for Disease Control and Prevention, all participants were assigned one of the following percentile classifications: “normal weight” (84th percentile and below), “overweight” (85th to 94th” percentile), and “obese” (95th percentile and above) [16].
Statistical analysis
Paired t-tests were used to examine differences between self-reported and measured height in cm and weight in kg for all participants and within the non-overweight/obese and overweight/obese groups. Independent t-tests were employed to test for differences between non-overweight/obese and overweight/obese children in terms of relative and absolute differences in self-reported and measured heights and weights. Relative differences were calculated as (Σself-report value – measured value)/93 and absolute differences were calculated as (Σ self-report value – measured value x -1 if difference was negative)/93. Levene’s test for equality of variance indicated variances in relative (F value=17.5;p<0.001) and absolute (F value=28.8;p<0.001) differences in weights between self-report and measured were not equal between non-overweight/obese and overweight/obese groups. Therefore, the Welch t-test for independent samples was used along with a Satterthwaite approximation for the degrees of freedom. Correlations between self-reported and measured heights and weights were analyzed by Pearson’s correlation coefficient. The Chi Square procedure was used to determine if the percent correctly categorized as non-overweight/obese or overweight/obese based on self-reported heights and weights varied as a function of weight status classification based on BMI percentile derived from measured heights and weights. For descriptive purposes, sensitivity and specificity were calculated as tp/(tp + tn) and tn/(tp + fp), respectively, where; tp=identified as overweight/obese by BMI percentile derived from both self-report and measured, tn=identified as non-overweight/obese by BMI percentile derived from both self-report and measured, and fp=identified as overweight/obese by BMI percentile derived from self-report, only. The level of significance was set at p<0.05 and all analyses were conducted with IBM SPSS Statistics, Version 21.
Results
All variables subjected to analyses displayed normal distributions. Self-reported and measured heights and weights are given in Table 1 for all participants together and Table 2 for non-overweight/obese and overweight/obese groups. Results are not presented by sex because no significant differences were found between boys and girls. For all participants, the means of self-reported and measured height were nearly identical differing by only 1.9 cm; however, self-reported height values displayed considerable variance compared to measured (26.7 cm vs. 8.9 cm). Height values obtained from the two methods were significantly but moderately correlated (r=0.32; p<0.05). Weights obtained from self-report were statistically significantly lower (-3.1 ± 7.7 kg) than measured weights (p<0.001) although the two values were highly correlated (r=0.88; p<0.001).
| Self-reported | Measured | t-value | r-value | |
|---|---|---|---|---|
| Height (cm) | 155.1 + 26.7 | 153.2 + 8.9 | 0.7 | 0.32* |
| Weight (kg) | 49.0 + 13.4 | 52.1 + 16.3 | -3.89** | 0.88** |
Mean difference height (cm) 1.9 + 25.3
Mean difference weight (kg) -3.1 + 7.7
Table 1: Means of self-reported and measured heights and weights for the entire sample (n=92). *p<0.05;**p<0.001
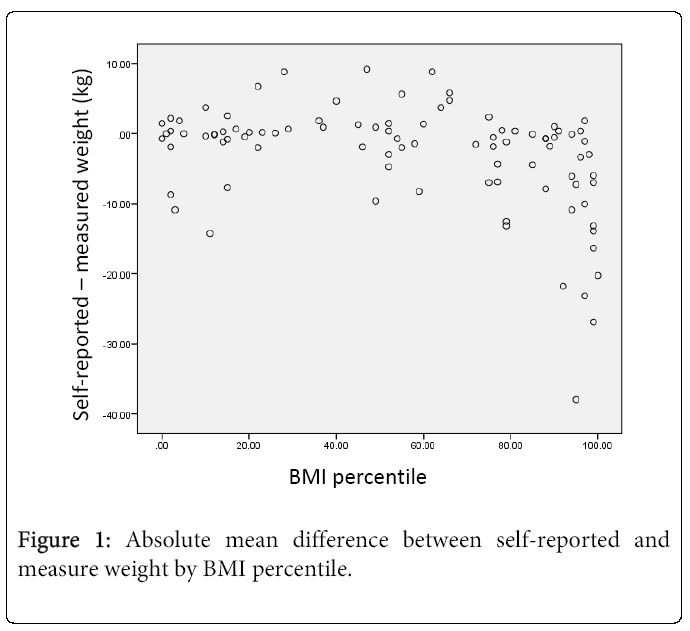
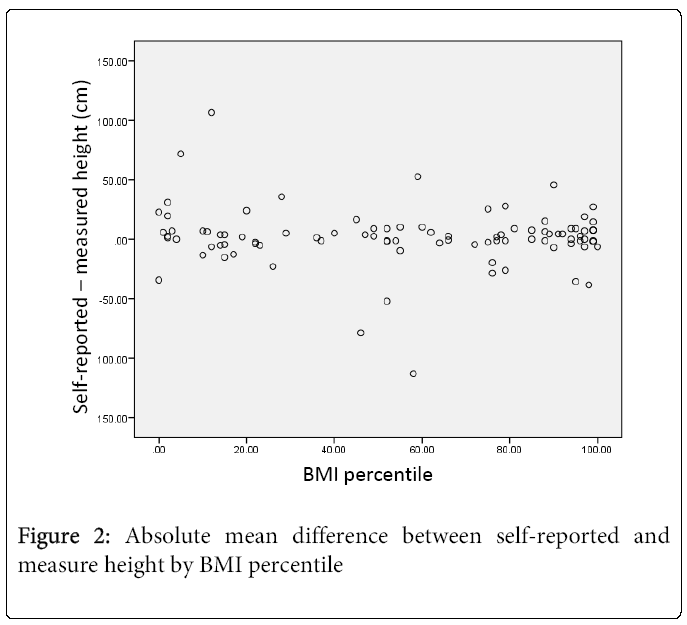
Provided in Table 2 and Figures 1 and 2 are data expressing self-reported and measured heights and weights relative to weight status as defined by BMI percentile ranks based on measured heights and weights. Self-reported and measured heights did not vary within nor between non-overweight/obese and overweight/obese youth, but as with the entire sample, variance was considerably larger for self-reported measures. Self-reported weights were lower than measured for both groups; however, the values were significantly different only for the overweight/obese youth (62.4 kg vs. 70.7 kg). The mean difference between self-reported and measured weights was -0.74 kg in non-overweight/obese and -8.3 kg in overweight/obese (p<0.001). Pearson’s correlation analyses showed statistically significant positive correlations between self-reported and measured heights for both groups. This same relationship existed for weight. The correlation coefficients were much larger for weight (r=0.83 and r=0.73) than height (r=0.28 and r=0.42). Visual representations of the associations between weight status and self-reported and measured height and weight differences are provided in Figures 1 and 2. For height, the differences between self-reported and measure values remained relatively constant throughout the range of BMI percentile (3rd to 99th percentile). For weight, differences between self-reported and measured values are also fairly consistent but only up to the 70th BMI percentile. After that, self-reported values tend to be lower than measured values and after the 90th BMI percentile the under-reporting becomes substantial.
| Non-overweight/obese (n=63) | Overweight/obese (n=29) | |||||||
|---|---|---|---|---|---|---|---|---|
| Self-reported | Measured | t- value | r | Self-reported | Measured | t- value | r | |
| Height (cm) | 152.9 + 30.0 | 151.6 +8.8 | 0.35 | .28* | 159.7 + 17.1 | 156.7 + 8.2 | 1.06 | .42** |
| Weight (kg) | 42.8 + 8.8 | 43.6 + 8.1 | -1.18 | .83*** | 62.4 + 12.0 | 70.7 + 14.1 | -4.54*** | .73*** |
| Mean difference height (cm) | 1.3 + 28.8 | 0.31 | 3.1 + 15.5 | |||||
| Mean difference weight (kg) | -0.74 + 5.0 | -3.9*** | -8.3 + 9.9 | |||||
Table 2: Means of self-reported and measured heights and weights for non-overweight/obese and overweight / obese youth. *p<0.05;**p<0.01;***p<0.001
The prevalence rates of overweight/obesity were 31.5% and 30.4% according to BMI percentile rankings derived from measured and self-reported heights and weights, respectively. Table 3 presents statistical parameters related to the classification performance of self-reported heights and weights when using different cut points compared to actual classifications based on BMI percentile derived from measured values. When the standard 85th BMI percentile cut point derived from self-reported values was used to define overweight/obesity, the specificity was 82.5% (correct classification rate of true negatives) and the sensitivity (correct classification rate of true positives) was only 58.6%. Although lowering the cut point to the 75th BMI percentile increased sensitivity to almost 80.0%, specificity fell to 70.0%. When the 80th BMI percentile was used both sensitivity and specificity were near 75.0%. The correct identification of either non-weight/obese or overweight/obese youth using self-report values was similar between cut points used (72.8%, 75.0%, and 76.1% for the 75th, 80th, and 85th BMI percentile).
| Using ≥ 85th BMI percentile from self-report to define overweight/obesity | |
|---|---|
| Sensitivity [Tp/(Tp + Fn)] | 58.6% |
| Specificity [Tn/(Tn + Fp)] | 82.5% |
| Accuracy [(Tp + Tn)/(p + n)] | 75.0% |
| Using≥80th BMI percentile from self-report to define overweight/obesity | |
| Sensitivity | 72.4% |
| Specificity | 77.8% |
| Accuracy | 76.1% |
| Using≥75th BMI percentile from self-report to define overweight/obesity | |
| Sensitivity | 79.3% |
| Specificity | 69.8% |
| Accuracy | 72.8% |
Table 3: Prediction parameters for self-report and measured BMI percentile.
Discussion
The purpose of this study was to validate self-reported height and weight in low-income, African American youth from a rural area in the southeast U.S. The main impetus for this was to provide support for the use of self-reported anthropometrics in epidemiological studies or large-scale surveillance efforts with this population. This is a highly warranted endeavor given the magnitude of the obesity epidemic and related co-morbidities experienced in this population. The results were less than encouraging for the use of self-reported heights and weights to derive BMI percentile related prevalence rates of overweight/obesity due to overweight/obese youth significantly under-reporting their weight.
Results of this study align with the recently published findings of Kreatsoulas et al. [9]. The results are also consistent with those of others regarding the under-estimation of weight and accurate report of height although some studies suggest height is over-estimated [10,11,17,18]. Additionally, these results correspond with other studies indicating that such errors are common across racial/ethnic subgroups of children/adolescents [10,11]. The propensity to underestimate weight appears to be associated with one’s ability to self-report weight/height and weight/height measurement history (i.e., recent weight measurement equates to a more accurate self-report; 6). As suggested by Rasmussen et al. [6] adolescents who are more likely to underestimate height and weight values can be identified by asking questions related to their recall ability on survey instruments. Data manipulation techniques (i.e., imputation) could be applied to “underestimators” in order to significantly improve accuracy; however, additional work in this area, is needed, especially with children [19].
The accuracy of self-reported weight was significantly lower for the overweight/obese youth examined in this study. On average, estimated weights were approximately 8 kg lower than measured values. Greater under-estimation of weight in overweight/obese has been demonstrated in children and adolescents and in other racially/ ethnically defined groups [10,11,20]. One interesting difference is that the underestimation noted in the current study was largely relative to the non-overweight/obese youth compared to overweight/obese youth examined in other studies. For instance, Lee et al. [11] observed only a 1.52 kg underestimation in weight by overweight/obese children as opposed to 8 kg seen here. This systematic bias would need to be addressed prior to any application of self-report height/weight protocols in this population, particularly given the high rates of obesity in this group.
One previous investigation suggests that even though accuracy of self-reporting height and weight is a problem in youth, the self-reported values are valid enough to correctly identify weight status [11]. Similarly, we found only a slight (1.1%) difference between overweight/obesity prevalence rates based on self-reported and measured values. Follow-up analyses indicate that the prevalence of obesity based on self-report values may be questionable because the accuracy of self-reported weight is reduced when there is a greater percentage of overweight/obese youth in the sample/population. Additionally, a literature review by Sherry et al. [20] found that prevalence rates of overweight are clearly underestimated when self-reported values are used (-0.4% to -17.7%). This review also predicted that up to 50% of overweight adolescents would be unidentified using self-reported values. This result is very similar to our finding, that using self-reported measures and the cut-off point at the 85th percentile- overweight/obese youth are only correctly identified about 60% of the time. Furthermore, lowering the BMI percentile cut-point values to the 80th percentile improves accuracy of overweight/obese classification to 72.4% and non-overweight/obese to 76.1%. Lowering the cut point to the 75th BMI percentile is possible, however, the risk of identifying non-overweight/obese youth as overweight/obese is fairly high (~30% incorrectly classified as having a weight issue) and thus, stigmatization may be an issue.
As with all research, this study contains various strengths and limitations. This sample was taken from a population that suffers a disproportionate distribution of the obesity related burden. But the targeted population is also a strength that supports the need and feasibility for studying and monitoring the accuracy of self-report anthropometrics in this population. Furthermore, the participants in this study represent a single sample from a hard-to-reach population. Very few studies examine low-income, African American youth living in rural areas. This sample was relatively small and from only one school servicing one rural geographical area. A sampling scheme utilizing a larger number of schools and areas would convey a higher level of confidence when generalizing the results to similar youth residing in other low-income, rural areas.
Based on these results, the use of self-reported heights and weights for deriving estimates of overweight/obesity rates in lower-income, rural African American youth is not advisable. Additional work is needed to create methods for correcting self-report bias, which will most likely entail after-data acquisition techniques such as the creation of multivariable equations to more accurately predict particular measures, for example, BMI percentile.
References
- Huh D, Stice E, Shaw H, Boutelle K (2012) Female overweight and obesity in adolescence: developmental trends and ethnic differences in prevalence, incidence, and remission. J Youth Adolesc 41: 76-85.
- Spruijt-Metz D (2011) Etiology, Treatment and Prevention of Obesity in Childhood and Adolescence: A Decade in Review. J Res Adolesc 21: 129-152.
- Owen CG, Whincup PH, Orfei L, Chou QA, Rudnicka AR, et al. (2009) Is body mass index before middle age related to coronary heart disease risk in later life? Evidence from observational studies. Int J Obes (Lond) 33: 866-877.
- Friedemann C, Heneghan C, Mahtani K, Thompson M, Perera R, et al. (2012) Cardiovascular disease risk in healthy children and its association with body mass index: systematic review and meta-analysis. BMJ 345: e4759.
- Lassale C, Péneau S, Touvier M, Julia C, Galan P, et al. (2013) Validity of web-based self-reported weight and height: results of the Nutrinet-Santé study. J Med Internet Res 15: e152.
- Rasmussen M, Holstein BE, Melkevik O, Damsgaard MT (2013) Validity of self-reported height and weight among adolescents: the importance of reporting capability. BMC Med Res Methodol 13: 85.
- Whetstone LM, Morrissey SL, Cummings DM (2007) Children at risk: the association between perceived weight status and suicidal thoughts and attempts in middle school youth. J Sch Health 77: 59-66.
- Chan NP, Choi KC, Nelson EA, Sung RY, Chan JC, et al. (2013) Self-reported body weight and height: an assessment tool for identifying children with overweight/obesity status and cardiometabolic risk factors clustering. Matern Child Health J 17: 282-291.
- Kreatsoulas C, Hassan A, Subramanian SV, Fleegler EW (2014) Accuracy of self-reported height and weight to determine body mass index among youth. J Child Adolesc Behav 2: 126.
- Morrissey SL, Whetstone LM, Cummings DM, Owen LJ (2006) Comparison of self-reported and measured height and weight in eighth-grade students. J Sch Health 76: 512-515.
- Lee B, Chung SJ, Lee SK, Yoon J (2013) Validation of self-reported height and weight in fifth-grade Korean children. Nutr Res Pract 7: 326-329.
- St George SM, Wilson DK (2012) A qualitative study for understanding family and peer influences on obesity-related health behaviors in low-income African-American adolescents. Child Obes 8: 466-476.
- Merrill RM, Richardson JS (2009) Validity of self-reported height, weight, and body mass index: findings from the National Health and Nutrition Examination Survey, 2001-2006. Prev Chronic Dis 6: A121.
- Chau N, Chau K, Mayet A, Baumann M, Legleye S, et al. (2013) Self-reporting and measurement of body mass index in adolescents: refusals and validity, and the possible role of socioeconomic and health-related factors. BMC Public Health 13: 815.
- Senese LC, Almeida ND, Fath AK, Smith BT, Loucks EB (2009) Associations between childhood socioeconomic position and adulthood obesity. Epidemiol Rev 31: 21-51.
- Kuczmarski RJ, Ogden CL, Guo SS, Grummer-Strawn LM, Flegal KM, et al. (2002) 2000 CDC Growth Charts for the United States: methods and development. Vital Health Stat 11 : 1-190.
- Elgar FJ, Roberts C, Tudor-Smith C, Moore L (2005) Validity of self-reported height and weight and predictors of bias in adolescents. J Adolesc Health 37: 371-375.
- Elgar FJ, Stewart JM (2008) Validity of self-report screening for overweight and obesity. Evidence from the Canadian Community Health Survey. Can J Public Health 99: 423-427.
- Drake KM, Longacre MR, Dalton MA, Langeloh G, Peterson KE, et al. (2013) Two-method measurement for adolescent obesity epidemiology: reducing the bias in self-report of height and weight. J Adolesc Health 53: 322-327.
- Sherry B, Jefferds ME, Grummer-Strawn LM (2007) Accuracy of adolescent self-report of height and weight in assessing overweight status: a literature review. Arch Pediatr Adolesc Med 161: 1154-1161.
Relevant Topics
- Adolescent Anxiety
- Adult Psychology
- Adult Sexual Behavior
- Anger Management
- Autism
- Behaviour
- Child Anxiety
- Child Health
- Child Mental Health
- Child Psychology
- Children Behavior
- Children Development
- Counselling
- Depression Disorders
- Digital Media Impact
- Eating disorder
- Mental Health Interventions
- Neuroscience
- Obeys Children
- Parental Care
- Risky Behavior
- Social-Emotional Learning (SEL)
- Societal Influence
- Trauma-Informed Care
Recommended Journals
Article Tools
Article Usage
- Total views: 15134
- [From(publication date):
July-2014 - Sep 01, 2025] - Breakdown by view type
- HTML page views : 10411
- PDF downloads : 4723