Case Report Open Access
Amniotic Band Syndrome: A Case Series
| Srinivasan H1*, Dhungel P1, Harper T2 and Lampley C3 | |
| 1Department of Pediatrics, Mount Sinai Hospital, Chicago, IL, USA | |
| 2Department of Pathology, Mount Sinai Hospital, Chicago, IL, USA | |
| 3Department of Obstetrics and Gynecology, Mount Sinai Hospital, Chicago, IL, USA | |
| Corresponding Author : | Dr Hari Srinivasan Mount Sinai hospital. Pediatrics 15th and California, Chicago, IL 60608, USA Tel : 7732575392 E-mail: hari.srinivasan@sinai.org |
| Received July 11, 2014; Accepted September 09, 2014; Published September 15, 2014 | |
| Citation: Srinivasan H, Dhungel P, Harper T, Lampley C (2014) Amniotic Band Syndrome: A Case Series. J Preg Child Health 1:109. doi: 10.4172/2376-127X.1000109 | |
| Copyright: © 2014 Srinivasan H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Pregnancy and Child Health
Abstract
Three cases of amniotic band syndrome (ABS) were studied to highlight the clinicopathologic characteristics. The diagnosis was based on the following manifestations: cranio facial clefts; limb body wall defects and amniotic band attachment. All three cases were stillborn and associated with defects in the central nervous system, heart or gastrointestinal system. Phenotypic features included craniofacial clefting, thoracoabdominoschisis, amputation, ring constriction, amniotic band adhesion, placental adhesions, and internal malformations. When analyzing the phenotype in relation to their etiology, it was found that amniotic disruption, vascular disruption or genetic disruption could explain the amniotic band syndrome/limb body wall complexes, alone or in combinations.
| Keywords |
| Amniotic band syndrome; Amputation; Cranio facial cleft; Placental adhesion; Ring constriction |
| Introduction |
| ABS is a disruption sequence with a broad spectrum of clinical manifestations ranging from partial amputations to major craniofacial and limb-body wall defects. The prevalence is approximately 1 in 1200 to 1 in 15,000 live births [1,2]. Its presentation is so variable that no two cases are exactly alike. |
| Case 1 |
| 19 year old G1P0 African American mother had regular antenatal care during this pregnancy and tested negative for hepatitis B and HIV antibodies and was immune to rubella. |
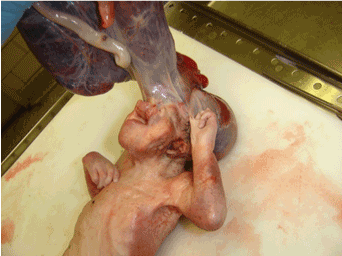
| The parents were non-consanguineous, and there was no family history of any congenital anomalies. She had no antenatal complications. Ultrasonogram done at 14 and 23 weeks gestation showed a fetus with multiple congenital anomalies. She delivered a 950 gram female still born infant at 26 weeks gestation by spontaneous delivery. The infant demonstrated the following anomalies (Figure 1) absence of skull superior to the base of the skull, absence of face above the mouth, rudimentary buccal mucosa with cleft lip and palate, and polydactyly in the right hand with a rudimentary extra digit between the 3th and 4th digit. This hand was attached to the face by fibrous tissues. The left hand was clenched and the thumb amputated. There was a circumferential constrictor band above the right ankle and bilateral rocker bottom feet. Karyotyping showed normal female 46 XX chromosomes. The placenta weighed 290 grams and was fused with the membranes covering the brain. Histopathological examination of the placenta showed perivillous fibrin and focal calcifications, severe acute chorionitis, and a three vessel umbilical cord. A postmortem full body X-ray was also done. |
| Case 2 |
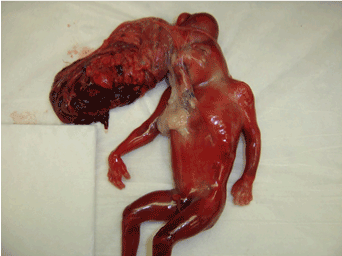
| 23 year old G6P5 Hispanic mother had regular antenatal care during this pregnancy and tested negative for hepatitis B and HIV antibodies and was immune to rubella. The parents were non-consanguineous, and there was no family history of any congenital anomalies. She had no antenatal complications. Ultrasonogram done at 14 weeks gestation showed a fetus with multiple congenital malformations. The pregnancy was electively terminated at 20 weeks gestation and she delivered 350 grams, still born male fetus by spontaneous delivery. The fetus demonstrated the following anomalies (Figure 2) multiple cephalocele, meningomyelocele with cranial vault defect, mutilation of facial features including absence of eyes and nose, rudimentary ears with absence of auditory meatuses, and ectopis cordia with Truncus Arteriosus. Karyotyping showed normal male 46 XY chromosomes. The placenta weighed 80 grams and was fused by membranes to the superior part of the skull and the anterior chest wall. Histopathological exam of the placenta showed focal intervillous fibrin membranes without pathological changes and a three vessel umbilical cord. A postmortem full body X-ray was also done. |
| Case 3 |
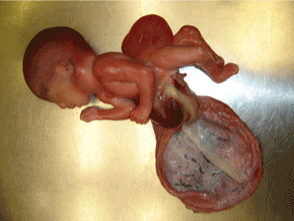
| 26 year old G4P3 African American mother had regular antenatal care during this pregnancy and tested negative for hepatitis B and HIV antibodies and was immune to rubella. The parents were nonconsanguineous, and there was no family history of any congenital anomalies. She had no antenatal complications. Ultrasonogram done at 14 weeks gestation showed a fetus with multiple congenital malformations. She delivered 475 grams, still born male fetus at 20 weeks gestation by spontaneous delivery. The fetus demonstrated the following anomalies (Figure 3) omphalocele, lumbar meningocele, severe lumbar scoliosis associated with lordosis, disarticulation of the symphysis pubis associated with 180 degree malrotation of the bilateral lower limbs, malformation of the lower pelvic organs and external genitalia with imperforate anus, rocker bottom feet and malformed left foot. Placental amniotic membrane demonstrated destructive adhesion to the abdomen with partial exposure of some of the abdominal organs. Karyotyping showed normal male 46 XY chromosomes. The umblical cord length was 35 cms which is normal for a fetus as 20 weeks gestation. The placenta weighed 110 grams and had there were adhesions between the amnion and abdomen. Histopathological examination of the placenta showed inter and intravillous fibrin and hemorrhages, membranes without pathological changes, and a three vessel umbilical cord. A postmortem full body X-ray was also done. |
| Discussion |
| The malformations in the three cases described illustrate the wide range of defects seen in ABS. These defects are so varied that the pathogenesis of this condition cannot be explained by a single mechanism. The mechanisms invoked include amniotic disruption, vascular disruption, embryonic dysplasia, and disorganization. |
| Amniotic disruption (exogenous) theory |
| Theory of Torpin (1965) [3] supports the exogenous nature of defects that result from rupture of the amniotic sac. Torpin proposed that once the amnion is ruptured and the fetus lies outside amniotic cavity, mesodermal bands emanate from the chorionic side of amnion which entrap various parts of the fetus and disturb normal development. Early rupture would lead to more severe malformations (eg. craniofacial and visceral) whereas later rupture would lead to milder forms. All three cases presented show a combination of craniofacial and visceral abnormalities and hence would represent an early rupture of the amniotic sac as a proposed mechanism. |
| Vascular disruption theory (VDT) |
| VDT proposed by Van Allen [4] implies that various congenital malformations may result from vascular disruption. Vascular disruption is described as events that negatively influence normal embryonic blood supply during embryogenesis, interrupt normal morphogenesis, or destroy previously existing structures. VDT is supported by experimental animal studies [5,6] where puncturing the amniotic cavity or ligating umbilical blood vessels has produced defects similar to those seen in ABS. The presence of multiple visceral abnormalities in cases 2 and 3 support the vascular disruption theory. |
| Embryonic dysplasia theory (endogenous) theory |
| In 1930, Streeter [7] suggested that fetal disruptions result from imperfect histogenesis. Based on thorough macroscopic and microscopic examination of constrictions in 16 cases, he concluded that structures mistaken for amniotic bands are residua of localized area of defective tissue. McKenzie [8] supported this theory and further added that defective tissue at the site of constrictions reflects an abnormal distribution of areas of cell death, a physiological feature in normal embryogenesis (programmed cell death). Histopathological studies of the constriction were not performed in this case series, but histopathological studies of the placenta in all three cases showed focal necrosis with intravillous fibrin and necrosis. |
| Genetic Disorganization (Ds) theory |
| Ds was first suggested as the cause of an ABS-like phenotype by Donnai and Winter [9]. They reported a series of cases, primarily spontaneous abortuses and stillbirths, with ABS-like findings, including limb amputations and body- wall defects. These cases and others reviewed by Robin and Nadeau [10] also manifested strikingly unusual findings, including mirror-image limb duplications, ectopic extra limbs, and finger-like skin projections. In some cases, these skin tags have been interpreted as digits amputated by amniotic bands that have been reimplanted [11]. The fetus in case 1 had an extra digit and an amputated thumb, supporting this theory. |
| As skin papillae are seen in no other disorder, Donnai and Winter [9] concluded that these cases represented the human homolog of Ds. The Ds gene has yet to be identified. It is a gain-of function mutation that causes malformations through a two hit mechanism [12]. However, unlike the classic retinoblastoma two-hit model [13], the ‘‘second hit’’ for Ds is thought not to arise in the other Ds allele. Rather, the second hit is thought to be another factor, genetic, environmental, or stochastic. It is the nature and timing of the second hit that determines the type of birth defect. Chromosome studies were performed in all three cases and showed normal karyotype. |
| Conclusion |
| Analysis of the four cases indicates that the phenotypic manifestations of amniotic band syndrome cannot be explained in totality by any one of the above mechanisms. Rather a combination of amniotic disruption, vascular disruption, embryonic dysplasia and genetic disorganization play a role in the development of the syndrome. |
References
- Garza A, Cordero JF, Mulinare J (1988) Epidemiology of the early amnion rupture spectrum of defects. Am J Dis Child 142: 541-544.
- Lindenau KF, Evers G (1974) An unusual case of bilateral and symmetric amniogenic indentations. Padiatr Grenzgeb 13: 61-65.
- Torpin R (1965) Amniochorionic mesoblastic fibrous strings and amnionic bands: Associated constricting fetal malformations or fetal death. Am J Obstet Gynecol 91: 65-75.
- Van Allen MI (1981) Fetal vascular disruptions: mechanisms and some resulting birth defects. Pediatr Ann 10: 219-233.
- Kino Y (1975) Clinical and experimental studies of the congenital constriction band syndrome, with an emphasis on its etiology. J Bone Joint Surg Am 57: 636-643.
- Kennedy LA, Persaud TV (1977) Pathogenesis of developmental defects induced in the rat by amniotic sac puncture. Acta Anat (Basel) 97: 23-35.
- Streeter GL (1930) Focal deficiency in fetal tissues and their relation to intrauterine amputation. Contrib Embryol 33:41.
- McKenzie J (1975) Amniotic bands. British Society for Developmental Biology, Symposium 2: The early development of mammals. Cambridge: University Press.
- Donnai D, Winter RM (1989) Disorganisation: a model for 'early amnion rupture'? J Med Genet 26: 421-425.
- Robin NH, Nadeau JH (2001) Disorganization in mice and humans. Am J Med Genet 101: 334-338.
- Rayan GM (2001) Ectopic implantation of constriction band intrauterine digital amputation. Plast Reconstr Surg 107: 1000-1002.
- Crosby JL, Varnum DS, Nadeau JH (1993) Two-hit model for sporadic congenital anomalies in mice with the disorganization mutation. Am J Hum Genet 52: 866-874.
- Knudson AG Jr (1971) Mutation and cancer: statistical study of retinoblastoma. Proc Natl Acad Sci U S A 68: 820-823.
Figures at a glance
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 |
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 22529
- [From(publication date):
October-2014 - Jul 15, 2025] - Breakdown by view type
- HTML page views : 17833
- PDF downloads : 4696
