Case Report Open Access
Amoebic Enterocolitis Mimicking Crohns Disease - Case Report
Jan M. Vrolijk*
Department of Hepatology, Gastroenterology and Clinical Pathology, Rijnstate Hospital Arnhem, The Netherlands
- *Corresponding Author:
- Jan M. Vrolijk
Department of Hepatology
Gastroenterology and Clinical Pathology
Rijnstate Hospital Arnhem
The Netherlands
Tel: +3188880880
E-mail: jvrolijk@rijnstate.nl
Received date: October 12, 2015; Accepted date: April 27, 2016; Published date: April 29, 2016
Citation: Vrolijk JM (2016) Amoebic Enterocolitis Mimicking Crohn’s Disease - Case Report. J Gastrointest Dig Syst 6:422. doi:10.4172/2161-069X.1000422
Copyright: © 2016 Vrolijk JM. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
To demonstrate the pitfalls in the diagnosis of intestinal amoebiasis we describe a case of amoebic enterocolitis with an atypical clinical presentation. In a patient with repeated rectal blood loss and no diarrhea, colonoscopy showed discontinuous ulcerative enterocolitis of the ileocecal region. Because of a high suspicion of Crohn’s disease a recipe of Entocort 9mg daily was handed out to him. Histological examination of the biopsies revealed the causative trophozoites of Entamoeba hystolitica, and the patient was then successfully treated with Metronidazole. Presumptive diagnosis based on a lesion’s appearance could be important for initial therapy but only objective data enable definitive diagnosis and specific therapy.
Keywords
Crohn’s disease; Amoebic enterocolitis
Introduction
A challenge that clinicians face on a daily basis is deciding when they have sufficient information to make a diagnosis. Clinical medicine is filled with scenarios in which ruling out a condition that mimics another disorder is important.
The lack of a pathognomonic diagnostic test for Crohn’s disease makes this condition susceptible for being frequently misdiagnosed. The current case provides a very good example: the need to consider infections that may mimic inflammatory bowel disease.
Case Report
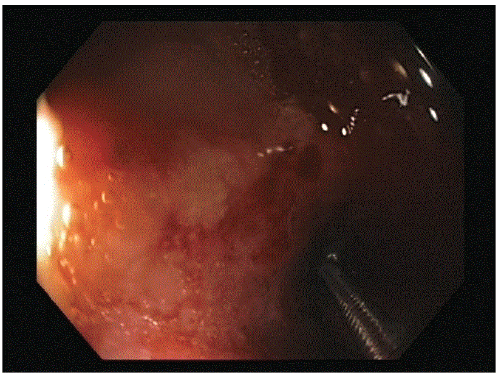
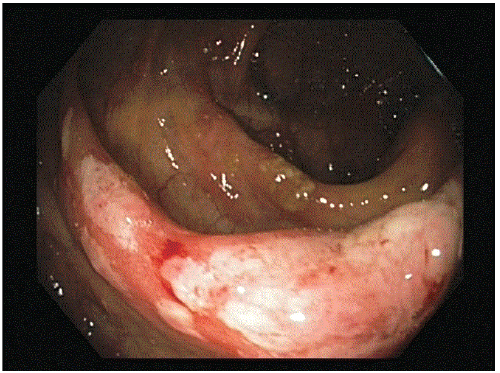
A 53 year-old man was referred by his general practitioner to our endoscopy unit for a colonoscopy because of recent rectal blood loss. Besides that, his bowel habits were unchanged. Colonoscopy showed multiple, discontinuous aphtous ulcers with overlying exudate located in the otherwise normal terminal ileum (Figure 1a) and generalized ulceration, atrophy and edema of the ileocecal valve (Figure 1b). In the ascending, transverse, descending en sigmoid colon no abnormalities were seen. Multiple biopsy samples were taken and because of the suspicion of Crohn’s disease an appointment for the outpatient clinic was made. A recipe for Entocort 9 mg daily was written and handed to him.
On his visit at the outpatient clinic one week later he presented without any significant problem. He did not have abdominal pain, diarrhoea, weight loss, anorexia or fever and his family history was unremarkable. Fortunately he had lost the recipe and therefore had not been able to start the prescribed medication yet. In the last two years he had been traveling to Thailand, Singapore and Sumatra where he had met his current girl friend who accompanied him on his visit. Clinical examination was besides generalized adipositas (length 187 cm, weight 105 kg), unremarkable. Laboratory investigations were normal.
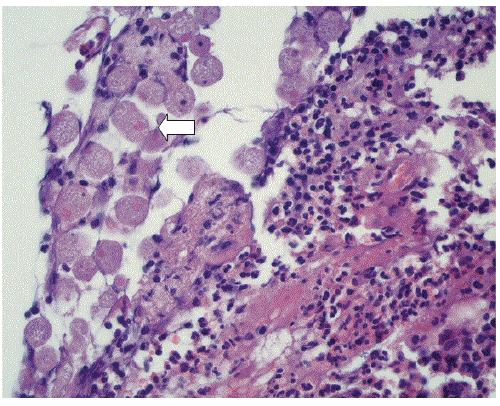
Histological examination of the biopsies taken at colonoscopy demonstrated trophozoites of Entamoeba histolytica (Figure 2). The patient was treated with antibiotics including metronidazole 500 mg t.i.d. for 10 days, and recovered without further difficulty. An ultrasound examination of the liver showed no cysts or other abnormalities.
Two months later he visited the outpatient clinic again because of a change in bowel habits and the suspicion of blood in his feces. A second colonoscopy was made to exclude recurrence of disease. No abnormalities were seen and the taken biopsies proved without any abnormalities. The diagnosis “post infectious irritable bowel syndrome” was discussed on the outpatient clinic.
Discussion
Amoebiasis is an ubiquitous parasitic infection, with a prevalence as high as 50% in the Indian subcontinent, Southern and Western Africa and South America [1]. The prevalence in the western countries is not known, still amebiasis is encountered anywhere from USA to Northern Europe. Amoebic infections are acquired via the oral-fecal, oral-anal, and oral-genital routes.
Intestinal amoebiasis is the most common form of amoebic infection. Most infected individuals carry the trophozoites asymptomatically within the lumen of the ascending colon and shed the cysts in their stools. Symptomatic patients typically present with a several – week history of cramping abdominal pain, weight loss, and watery or bloody diarrhea. The insidious onset with fever and bloody stools absent in most cases, make the diagnosis difficult. Complications of intestinal amoebiasis include massive hemorrhage, peritonitis secondary to perforation, paralytic ileus, intestinal fistulae and abscesses, stricture and intussusception. Ameboma’s are localized chronic, granulomatous masses containing multiple small abscesses commonly occurring in the wall of the coecum of ascending colon and can be mistaken for carcinoma. Fulminant colitis is an unusual complication of amebic infection and carries a mortality of 50%.
In developing countries the diagnosis is most commonly made by identifying cysts or motile trophozoites on a saline wet mount of stool specimen. The drawbacks of this method include its low sensitivity and false positive results owing to the presence of noninvasive Entamoeba species such as E. dispar and E. moshkovskii infection. The diagnosis should be based on the detection in stool of E. histolytica – specific antigen or DNA and by the presence of antiamebic antibodies in the serum. Both the serum indirect hemaglutination antibody (IHA) and the enzyme-linked immunosorbent assay (ELISA) are highly sensitive (90-100%) and turn positive within 7-10 days of infection. Unfortunately the serologic tests are unable to distinguish between active or prior invasive infection since antibodies can remain detectable for as long as 20 years [1,2].
The diagnosis can also be made by examination of colonic mucosal biopsy specimens obtained endoscopically. Histopathological findings associated with amebic colitis include diffuse, nonspecific mucosal thickening, focal ulceration with or without amoebae. The amoeba parasites are lying on top of the ulcera, sometimes extending in the submucosa. The ingested erythrocytes help to distinguish true parasites from swollen and degenerated epithelial cells.
Nitroimidazoles, particularly metronidazole is the mainstay of the therapy for invasive amoebiasis. In the rare case of fulminant amoebic colitis it is prudent to add broad-spectrum antibiotics to treat intestinal bacteria that may spill into the peritoneum; surgical intervention is required for acute abdomen, gastrointestinal bleeding, or toxic megacolon. In 40-60% of the patients receiving nitroimidazole parasites can persist in the intestine. Therefore, nitroimidazole treatment should be followed by paromomycin or the second-line agent diloxanide furoate to cure luminal infection.
Conclusion
In previous reports of unsuspected amoebic colitis presenting as inflammatory bowel disease, misdiagnosis, delay in antibiotic treatment and institution of immunosuppressive therapy have resulted in serious morbidity and mortality [2-6]. Even if in our patient no serious complications occurred, it is imperative to exclude amoebic colitis prior to undertaking steroid therapy, especially in patients with a history of travel to or residence in areas with endemic E. histolytica.
In conclusion, amoebiasis is no longer an exotic disease. Think of it especially in world travelers and patients presenting as inflammatory bowel disease with no response to immunosuppressive therapy [7].
References
- Haque R, Huston CD, Hughes M (2003) Amebiasis. N Engl J Med 348:1565-1573.
- Haque RR, Mollah NU, Ali IKM, Alam K, Eubanks A, et al. (2000) Diagnosis of amebic liver abscess abd intestinal infection with the Tech Lab Entamoeba histolytica II antigen detection and antibody tests. J Clin Microbiol 38:3235-3239.
- Mendonca HL Jr, Vieta JO, Korelitz BI (1977) Perforation of the colon in unsuspected amebic colitis: report of two cases. Dis Colon Rectum 20:149-153.
- Ishida H, Inokuma S, Murata N, Hashimoto D, Satoh K, et al. Fulminant amoebic colitis with perforation successfully treated by staged surgery: a case report. J Gastroenterol 38:92-96.
- Goulet CJ, Mosseley RH (2005) The unturned stone. N Engl J Med 352:489-494.
- Gupta SS, Singh O, Shukla S, Raj MK (2009) Acute fulminant necrotizing amoebic colitis: a rare and fatal complication of amoebiasis: a case report. Cases J2:6557.
- Abbas MA, Mulligan DC, Ramzan NN, Blair JE, Smilack JD, et al. (2000) Colonic perforation in unsuspected amebic colitis. Dig Dis Sci 45:1836-1841.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 12476
- [From(publication date):
April-2016 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 11570
- PDF downloads : 906