Case Report Open Access
An Unusual Presentation of Cholecystoduodenal Fistula: Massive Upper Gastrointestinal Bleeding
Yael Feferman*, Vyacheslav Bard, Nimrod Aviran, Michael stein, Hanoch Kashtan and Eran SadotThe Department of Surgery, Rabin Medical Center, Campus Beilinson, Petach Tiqva, Israel
- *Corresponding Author:
- Yael Feferman
The Department of Surgery
Beilinson Hospital, Jabotinsky 39
Petach Tiqva, Israel
Tel: +972-3-9376208
Fax: +972-3-9376251
E-mail: yaelfef@gmail.com
Received date: July 4, 2015 Accepted date: July 24, 2015 Published date: July 30, 2015
Citation: Feferman Y, Bard V, Aviran N, Stein M, Kashtan H, et al. (2015) An Unusual Presentation of Cholecystoduodenal Fistula: Massive Upper Gastrointestinal Bleeding. J Gastrointest Dig Syst 5: 314. doi:10.4172/2161-069X.1000314
Copyright: © 2015 Feferman Y et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License; which permits unrestricted use; distribution; and reproduction in any medium; provided the original author and source are credited
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
Background: Cholecystodoudenal fistula (CDF) as a cause of severe upper gastrointestinal bleeding (UGIB) is a rare event that has few reported cases. Methods: Here we discuss the case of an 86-year-old male who presented with UGIB due to a CDF. Results: The patient was diagnosed promptly and underwent successful emergent operation. Discussion and Conclusion: The following is a discussion of the case, accompanied by a brief review of enterobiliary fistulas. Physicians involved in the management of patients with UGIB should entertain the possibility of a biliary-enteric fistula as a possible cause, particularly in patients with risk factors for gallstone disease. Computed Tomography (CT) might enable prompt diagnosis.
Abstract
Background: Cholecystodoudenal fistula (CDF) as a cause of severe upper gastrointestinal bleeding (UGIB) is a rare event that has few reported cases.
Methods: Here we discuss the case of an 86-year-old male who presented with UGIB due to a CDF.
Results: The patient was diagnosed promptly and underwent successful emergent operation.
Discussion and Conclusion: The following is a discussion of the case, accompanied by a brief review of entero-biliary fistulas. Physicians involved in the management of patients with UGIB should entertain the possibility of a biliary-enteric fistula as a possible cause, particularly in patients with risk factors for gallstone disease. Computed Tomography (CT) might enable prompt diagnosis.
Keywords
Fistula; Biliary-enteric; Cholecystoduodenal; Upper gastrointestinal hemorrhage
Introduction
Cholecystoenteric fistulas are rare complication of gallstone disease, with a reported incidence of 3-5% in patients with cholelithiasis. CDF is the most common biliary-enteric fistula [1-4]. Clinical presentation is variable and may include a history of pain in the right upper quadrant and/or epigastrium, jaundice, and flatulent dyspepsia that is aggravated with the intake of fried food [3].
Massive UGIB, caused by CDF, is rare with only few cases reported in the literature [5-13]. Demonstrating the fistula as the cause of bleeding is difficult, and the majority of non-obstructive biliary-enteric fistulas cases will be found incidentally only in the operating room.
We report the 10th English- language published case of a CDF that presented with hemorrhagic shock due to massive UGIB [5-13]. The inconclusive Esophagogastroduodenoscopy (EGD) findings led us to perform an abdominal CT and the combination of these two modalities made the diagnosis of bleeding from CDF.
Case Report
An 86-year-old male presented to the emergency room with vomiting of coffee-ground content and melena. His comorbidities included hypertension, chronic renal failure, osteoporosis and gout. He had no past surgical history. Two months prior, he was admitted to an outside hospital due to similar presentation. He underwent EGD which did not reveal any source of active bleeding and he was therefore discharged with proton pump inhibitors (PPI) treatment.
During his later admission he was afebrile and pale. Abdominal physical examination was normal. Digital rectal examination demonstrated melena. Hemoglobin level declined from a baseline of 13 g% to 7.4 g%.
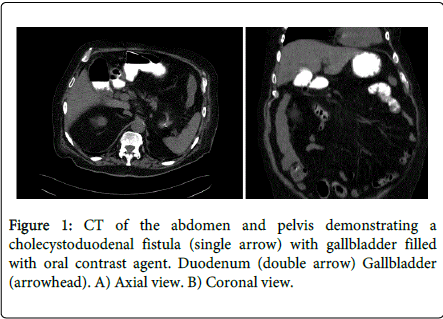
An urgent EGD was performed which revealed a large ulcer located at the posterior wall of the duodenal bulb, encircling about 2/3rd of its diameter. Fistula tract was suspected at the inferior part of the ulcer. Following the examination, the patient became hemodynamically unstable with blood pressure dropped to 77/40 mmHg. Resuscitation with vasopressors and blood products was initiated. Later, abdominal CT demonstrated contrast material in the gallbladder and CDF was diagnosed (Figure 1a and 1b).
A working diagnosis of UGIB secondary to CDF was made and the patient was taken to the Operating room. On exploration through a midline incision, partially gangrenous gallbladder was identified, adherent to the duodenum. A necrotic CDF was observed. A retrograde cholecystectomy was preformed and the duodenum was repaired primarily with suturing in two layers. A 3 mm laceration at the lateral right aspect of the common bile duct was identified. It was repaired primarily using single PDS sutures. A feeding jejunostomy with longitudinal Witzel technique was performed. Pathology findings of the specimen were consistent with a marginal ulcer located at the CDF. The postoperative course included aspiration pneumonia and the patient was discharged to rehabilitation center on post operative day 23.
Discussion
Biliary-enteric fistulas are rare, with a reported incidence of 3-5% in patients with cholelithiasis, and 0.15-4.8% in patients undergoing biliary surgery. The most common communication is cholecystoduodenal (61% to 77%), followed by cholecystocolonic (14% to 17%) and cholecystogastric (6%). Biliary tract fistulas are categorized into spontaneous and post-operative types. Spontaneous biliary-enteric fistulas are produced by gallstones (90%), peptic ulcer disease (6%) and malignancy or trauma (4%) [1-4].
The etiology of biliary-enteric fistulas is yet to be clearly established. According to Glenn et al., [1] following stone formation in the gallbladder, an acute inflammatory process with obstruction of the cystic duct results in adhesion of the gallbladder to the contiguous viscus, usually duodenum. Recurrent episodes of such inflammation result in the destruction of the wall of the gallbladder and the adjacent viscus, ultimately resulting in erosion and fistula formation. Raiford et al., [14] hypothesized that mechanical pressure due to a gallstone results in erosion of the tissues in the gallbladder wall with necrosis until a fistula forms with the contiguous viscus.
There are no specific clinical symptoms or signs that can lead to the diagnosis of a biliary-enteric fistula [15]. Symptoms are nonspecific and similar to those of any chronic biliary-tract disease. The majority of patients with biliary-enteric fistulas have a history of prolonged gallstone disease. Physical findings are unremarkable; however, a vague fullness can sometimes be palpated in the right upper abdominal quadrant which represents the fistula and adhesions [16]. Other presenting symptoms include: Jaundice, right upper quadrant and/or epigastric pain, and flatulent dyspepsia that is aggravated with the intake of fried food [3]. Possible consequences of biliary-enteric fistulas are ascending cholangitis, particularly when the colon is involved; gallstone ileus; weight loss and “malabsorption syndrome”; carcinoma, and rarely gastrointestinal hemorrhage [16].
Diagnosis of biliary-enteric fistulas is traditionally performed using Barium meal examination. However, it can demonstrate the communication between the duodenum and biliary tract, only when the fistula is relatively large. In some cases cholecystoduodenal fistulas can be demonstrated by a deformity of the duodenal bulb. Although ultrasound and CT examinations are not always diagnostic, the presence of an internal biliary fistula can be suggested in some cases by the findings of pneumobilia, an atrophic gallbladder, and biliary stones [4]. CT scans, in particularly, allows visualization of the fistulas, air in the bile duct and contraction of the gallbladder, and differentiates between cholecysto-enteric and choledocho-enteric fistulas [17].
However, in a study which investigated the role of Helical CT in diagnosis of gallstone ileus and related conditions, direct CT visualization of a biliary-enteric fistula was found in only 12.5% of cases [18].
As the majority of non-obstructive biliary-enteric fistulas cases are found incidentally in the operating room, if one is not aware of the disturbed anatomic features, operation is likely to be difficult and dangerous. In cases of UGIB with inconclusive finding of EGD, the possibility of a bleeding marginal ulcer with CDF should be considered. Direct CT visualization of a biliary-enteric fistula is important to establish diagnosis.
Bleeding from the biliary tract occurs most commonly into the duodenum and is manifested by hematemesis or melena. Non traumatic massive hemorrhage, caused by CDF, is rare. A thorough search of the medical literature revealed only 10 English-language published reported cases of CDF as a cause of severe UGIB (Table 1). Whitman and associates [19] collected reports of 100 patients with bleeding which originated in the biliary tract as a cause of major gastrointestinal hemorrhage. Of those, more than half occurred due to rupture of an aneurysm of the hepatic or cystic artery into the biliary tract. Most cases of severe bleeding manifested primarily by hematemesis. Only slight melena occurred in some cases [19].
| Author | Year of publication | Age | Gender | Treatment method | Outcomes |
| Corry [11] | 1968 | 81 | Female | Cholecystectomy, cystic artery ligation, extending the duodenal perforation across the pylorus into the antrum, closure with Heineke-Mikulicz pyloroplasty. | - |
| Schenken and Adamson [10] | 1970 | - | - | - | - |
| Harte [5] | 1984 | - | - | - | - |
| Hjelmqvist [9] | 1985 | - | - | - | - |
| Kochhar [8] | 1988 | - | - | Surgical treatment, No details | Surgical treatment was successful |
| Lee [12] | 2003 | 60 | Male | After failure of Endoscopic treatment - open cholecystectomy | No post operative complication, histology of gallbladder cancer |
| Changku [7] | 2005 | 50 | Male | Cholecystectomy was performed after the duodenal fistula was resected and repaired | The postoperative course was uneventful. Seven month follow-up without any recurrence of bleeding |
| Kosugi [6] | 2006 | 66 | Female | Cholecystectomy, cystic artery ligation, omental patch on the duodenum | Discharged on the 53rd postoperative day. Three months after surgery, endoscopy revealed a persisting duodenal opening without any symptoms |
| Mohammed [13] | 2013 | 44 | Female | Conservatively treatment with antibiotics and elective open cholecystectomy with repair of the CDF | - |
Table 1: Clinical features of previous English-language publications of cases with UGIB as the presenting symptom of CDF [5-13].
Upper gastrointestinal hemorrhage associated with biliary fistula has previously been reported as the presenting symptom in Bouveret’s syndrome, which is characterized by the formation of gastric outlet obstruction due to gallstone in the duodenum [20]. This is a rare clinical condition, with few cases reported in the literature [21]. Bleeding usually arises secondary to ulceration of the duodenal bulb, caused by the impacted stone. In the case reported here, the inconclusive EGD findings led us to perform an abdominal CT and the combination of these two modalities enabled the diagnosis of bleeding CDF.
Conclusion
Physicians involved in the management of patients with UGIB should entertain the possibility of a biliary-enteric fistula as the cause, particularly if the patient has risk factors for gallstone disease. We believe that this case highlights the importance of CT imaging as a complementary tool to an EGD study in patients with UGIB and unusual endoscopic findings.
References
- Glenn F, Reed C, Grafe WR (1981) Biliary enteric fistula. Surg Gynecol Obstet 153: 527-531.
- Angrisani L, Corcione F, Tartaglia A, Tricarico A, Rendano F, et al. (2001) Cholecystoenteric fistula (CF) is not a contraindication for laparoscopic surgery. Surg Endosc 15: 1038-1041.
- Chowbey PK, Bandyopadhyay SK, Sharma A, Khullar R, Soni V, et al. (2006) Laparoscopic management of cholecystoenteric fistulas. J Laparoendosc Adv Surg Tech A 16: 467-472.
- Yamashita H, Chijiiwa K, Ogawa Y, Kuroki S, Tanaka M (1997) The internal biliary fistula--reappraisal of incidence, type, diagnosis and management of 33 consecutive cases. HPB Surg 10: 143-147.
- Harte PJ, Hyland JM, Browne HJ (1984) Acute upper gastro-intestinal haemorrhage in a patient with choledochoduodenal fistula. Ir Med J 77: 353-354.
- Kosugi S, Tani T, Kurosaki I, Hatakeyama K (2006) Gallstone ileus with cholecystoduodenal fistula presenting massive upper gastrointestinal hemorrhage. J Gastroenterol Hepatol 21: 624-625.
- Changku J, Shaohua S, Zhicheng Z, Shusen Z (2005) Upper gastric tract bleeding due to cholecystoduodenal fistula: a case report. Hepatogastroenterology 52: 1372-1374.
- Kochhar R, Krishna PR, Gupta NM, Mehta SK (1988) Massive gastrointestinal bleeding due to cholecystoduodenal fistula. Case report. Acta Chir Scand 154: 471-472.
- Hjelmqvist B, Borgström A, Zederfeldt B (1985) Major gastrointestinal haemorrhage as a complication of cholecystoduodenal fistula in gallstone disease. Report of three cases. Ann Chir Gynaecol 74: 6-8.
- Schenken JR, Adamson JR (1970) Fatal gastrointestinal tract hemorrhage: a complication of ulcerative cholecystitis, cholelithiasis, and cholecystoduodenal fistula. Am J Clin Pathol 53: 423-424.
- Corry RJ, Mundth ED, Bartlett MK (1968) Massive upper-gastrointestinal tract hemorrhage. A complication of cholecystoduodenal fistula. Arch Surg 97: 531-532.
- Lee SB, Ryu KH, Ryu JK, Kim HJ, Lee JK, et al. (2003) Acute acalculous cholecystitis associated with cholecystoduodenal fistula and duodenal bleeding. A case report. Korean J Intern Med 18: 109-114.
- Mohammed N, Godfrey EM, Subramanian V (2013) Cholecysto-duodenal fistula as the source of upper gastrointestinal bleeding. Endoscopy 45 Suppl 2 UCTN: E250-251.
- Raiford TS (1961) Intestinal obstruction due to gallstones. (Gallstone ileus). Ann Surg 153: 830-838.
- LeBlanc KA, Barr LH, Rush BM (1983) Spontaneous biliary enteric fistulas. South Med J 76: 1249-1252.
- Piedad OH, Wels PB (1972) Spontaneous internal biliary fistula, obstructive and nonobstructive types: twenty-year review of 55 cases. Ann Surg 175: 75-80.
- Shimono T, Nishimura K, Hayakawa K (1998) CT imaging of biliary enteric fistula. Abdom Imaging 23: 172-176.
- Lassandro F, Romano S, Ragozzino A, Rossi G, Valente T, et al. (2005) Role of helical CT in diagnosis of gallstone ileus and related conditions. AJR Am J Roentgenol 185: 1159-1165.
- Whitman EJ, Buie LA Jr, Huizenga KA, Waugh JM (1960) Cystic artery--cystic duct fistula: an unusual cause of gastrointestinal hemorrhage; report of case. Proc Staff Meet Mayo Clin 35: 551-554.
- Jones TA, Davis ME, Glantz AI (2001) Bouveret's syndrome presenting as upper gastrointestinal hemorrhage without hematemesis. Am Surg 67: 786-789.
- Nabais C, Salústio R, Morujão I, Sousa FV, Porto E, et al. (2013) Gastric outlet obstruction in a patient with Bouveret's syndrome: a case report. BMC Res Notes 6: 195.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 16789
- [From(publication date):
August-2015 - Aug 17, 2025] - Breakdown by view type
- HTML page views : 12089
- PDF downloads : 4700