Bilateral Popliteal Arterial Emboli
Received: 22-May-2017 / Accepted Date: 16-Jun-2017 / Published Date: 21-Jun-2017
5982Case Report
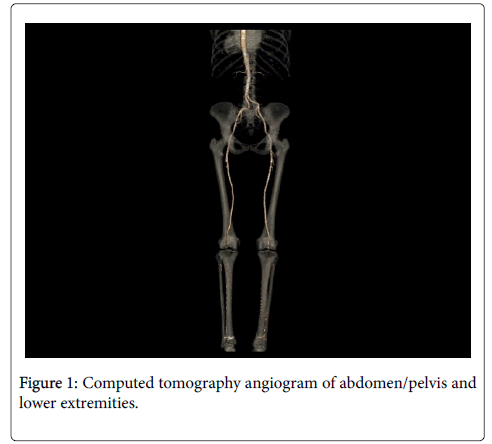
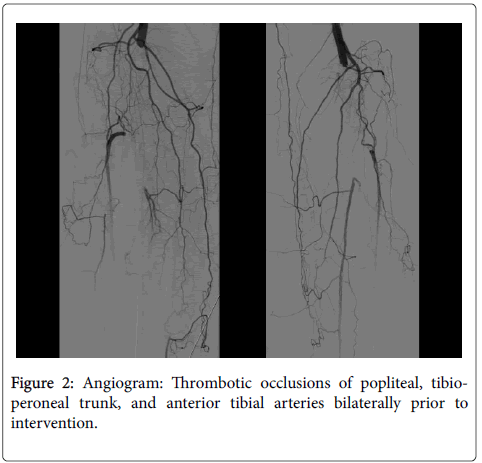
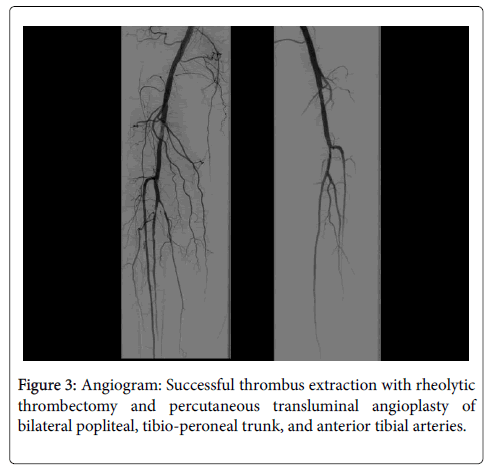
A 71 year-old woman with hypertension, rheumatic heart disease complicated by severe mitral stenosis, atrial fibrillation on chronic warfarin therapy who presented with bilateral calf pain. Two weeks prior to her presentation, her warfarin was held in anticipation for cataract surgery. A week later, she developed bilateral claudication pain after walking 20 feet that improved with rest. Her ankle-brachial index was 0.65 on the right side and 0.41 on the left side with pulse volume recording localizing lesions to bilateral popliteal region. Computed tomography angiogram of abdomen, pelvis and lower extremities demonstrated occluded popliteal arteries on both sides with variable degree of occlusions (Figure 1). Her diagnostic peripheral angiogram revealed non-obstructive disease in bilateral iliac, common femoral and superficial femoral arteries with thromboembolic occlusions in addition to organized thrombus of popliteal arteries, tibio-peroneal trunk and anterior tibial arteries (Figure 2). She underwent successful thrombus extraction with rheolytic thrombectomy and percutaneous transluminal angioplasty of bilateral popliteal arteries and their runoff vessels with significant improvement in vessel flow and in her symptoms of claudication (Figure 3). This is presumed to be an embolic phenomenon with her known atrial fibrillation and temporary cessation of her therapeutic anticoagulation.
Popliteal arterial embolism is an uncommon disease with high morbidity and mortality. In the setting of acute peripheral embolism, common presentation includes abrupt onset of pain and loss of pulses in the affected extremities. As the ischemia persists, tissue viability will depend on collateral flow while motor and sensory paralysis and muscle infarction can become irreversible in hours. Most common cause is thromboembolism from atrial fibrillation in about one quarter of the cases. Other causes include proximal aortic atherosclerosis, endocarditis, abdominal aortic aneurysms, aortic grafts, aortic dissection, paradoxical embolus, and iatrogenesis (intra-aortic balloon pump, valvuloplasty, and angiography). Treatment includes immediate anticoagulation to slow the formation and propagation of thrombus while allowing collateral circuit to form. Surgical treatment involves embolectomy via femoral or popliteal approach with and without bypass depending on preexisting atherosclerosis. In patients who do not have neurologic changes and can tolerate a delay in revascularization, selective intra-arterial thrombolysis should be considered.
When revascularization is successful, one should monitor for perfusion injury with limb swelling that might require fasciotomy for compartment syndrome. In the setting of nonviable tissue and irreversible limb ischemia, amputation should be carried out to avoid reperfusion related to the release of acidic and hyperkalemic venous blood from the infarcted extremity. In a surgical case series by Raut et al. at Massachusetts General Hospital from 1989 to 2000, 65 patients with 72 popliteal artery emboli were included with 82% of the patients presenting in an acute fashion and mostly with acute limb ischemia while the delayed presentation group had symptoms of claudication, rest pain, or gangrene. Most common identified etiology was atrial fibrillation in 17 of the 72 cases. Surgical embolectomy using popliteal approach was used in most of the cases leading to limb salvage rate of 88% and mortality of 10% with increased in mortality after amputation. Prior studies by Abbot et al. have demonstrated that shorter interval to treatment within 12 hour of onset of symptoms and post-operative anticoagulation resulted in increased limb salvage and lower mortality rates. This is the first case report of percutaneous approach of treating bilateral popliteal arterial embolism with rheolytic thrombectomy and percutaneous transluminal angioplasty [1-4].
References
- Rapp JH, Gasper W (2014) “Arteries.†Current Diagnosis & Treatment: Surgery (14th edn) New York, NY: McGraw-Hill.
- Oneglia C, Rusconi C (2001) “Left atrial appendage thrombus as a source of peripheral embolism.†Echocardiography 5: 389-390.
- Raut CP, Cambria RP, LaMuraglia GM, Brewster DC, Moncure AC (2004) “Surgical management of popliteal artery embolism at the turn of the millennium.†Annal of Vascular Surgery 1: 79-85.
- Abbott WM, McCabe C, Maloney RD (1984) “Embolism of the popliteal artery.†Surg Gynecol Obstet 159: 533-536.
Citation: Chyou AC, Kim LK, Feldman DV (2017) Bilateral Popliteal Arterial Emboli. Atheroscler Open Access 2: 112.
Copyright: © 2017 Chyou AC, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Open Access Journals
Article Usage
- Total views: 4089
- [From(publication date): 0-2017 - Aug 30, 2025]
- Breakdown by view type
- HTML page views: 3198
- PDF downloads: 891