Research Article Open Access
Cardiorespiratory Repercussions of Hot Tub (Ofur�?´) in Preterm Newborns with Low Birth Weight: A Cross-Sectional Study
Roberta Lins Gonçalves1*, Joaquim de Azevedo Machado Junior2, Mayara Elisa Meneguini2, Valéria Padilha Ataíde2, Sheila Maria Serrão Gama3, Marcos Giovanni Santos Carvalho4 and Fernanda Figueroa Sanchez51Physical Therapist (PT), Federal University of Amazonas (UFAM), Brazil
2PT, Residence Program in Physical Therapy in Neonatal Intensive Care, UFAM, Brazil
3PT, Neonatal Intensive Care Unit, Balbina Mestrinho Maternity, Secretaria de Estado de Saúde do Amazonas - Manaus (AM), Brazil
4PT, Coordinator at Neonatal Intensive Care Unit, Balbina Mestrinho Maternity, Secretaria de Estado de Saúde do Amazonas - Manaus (AM), Brazil
5PT, Federal University of Amazonas – UFAM, Manaus-AM, Brazil
- *Corresponding Author:
- Mrs. Roberta Lins Gonçalves, PhD
UFAM Campus, Universitário Senador Arthur Virgílio Filho-Faculdade de Educação
Física e Fisioterapia-FEFF-UFAM. Av Rodrigo Otávio Jordão Ramos, 3000
Campus setor sul-Japiim-Manaus, Amazonas, Brazil, Cep: 69.077-000
Tel: +55(031)999584724
Fax: (92)33054092
E-mail: betalinsfisio@yahoo.com.br
Received date: August 07, 2017; Accepted date: August 14, 2017; Published date: August 19, 2017
Citation: Gonçalves RT, Machado Junior JDA, Ataíde MEMVP, Gama SMS, Carvalho MGS, et al. (2017) Cardiorespiratory Repercussions of Hot Tub (Ofurô) in Preterm Newborns with Low Birth Weight: A Cross-Sectional Study. J Nov Physiother 7:361. doi: 10.4172/2165-7025.1000361
Copyright: © 2017 Gonçalves RT, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
Background: According to the World Health Organization preterm birth is the most common direct cause of newborn mortality. Preterm birth and being small for gestational age which are the reasons for low-birth-weight (LBW), are also important indirect causes of neonatal deaths. LBW contributes to 60% to 80% of all neonatal deaths. In addition to the high mortality rate preterm newborns (PTNB), especially LBW, there are many barriers to the normal development. In this way, some practices have been adopted to favor the humanized assistance to the baby and his family. The hot tub, known in Brazil as ofurô, has been use in Brazil as a form of aquatic physiotherapy with the purpose of contributing to the reduction of stress, length of hospital stay and favoring the weight gain of PTNB with LBW. It consists of immersing the PTNB in hot tub in warm water up to shoulder height to simulate the sensation of the mother's uterus. However, there are few studies evaluating the repercussions of the subject. Objective: To evaluate the cardiorespiratory repercussions heart rate, respiratory rate, oxygen pulse saturation and the pain of PTNB submitted to the hot tub were observed. Methodological design: A prospective cross-sectional study was carried out in an intermediate care unit of Manaus, Amazonas, Brazil, between Months from March to November 2016. Twenty-one PTNB which have undergone to the hot tub were observed in three moments: before (moment 1), during (moment 2) and after (moment 3) hot tub. Categorical variables were evaluated by frequency, percentages, and the numerical by means of mean, median and standard deviation. 0.05 of significance was adopted. Results: The hot tub did not present cardiorespiratory changes in the PTNB analyzed and did not cause pain or stress or any type of intercurrence. Clinically there was a favorable response to conduct. It was possible to observe that the PTNB during the hot tub remained calm and relaxed, and in many situations, they presented sleepiness and yawning demonstrating well-being with the conduct. Conclusion: The hot tub did not present cardiorespiratory alterations in the low birth weight PTNB analyzed and did not cause pain, stress, or any kind of intercurrence, being a safe conduct in this regard.
Keywords
Modalities of physical therapy; Newborn; Humanization of care; Prematurity; Hydrotherapy
Introduction
According to the World Health Organization (WHO) preterm birth is the most common direct cause of newborn mortality. Preterm birth and being small for gestational age which are the reasons for low-birthweight (LBW), are also important indirect causes of neonatal deaths. LBW contributes to 60% to 80% of all neonatal deaths. The global prevalence of LBW is 15.5%, which amounts to about 20 million LBW infants born each year, 96.5% of them in developing countries [1,2].
In addition to the high mortality rate PTNB, especially LBW, there are many barriers to the normal development. Some barriers are intrinsic to the conditions of diseases, affecting multiple organs and systems; others, however, can be extrinsic to it and related to the noisy, enlightened and stressful environment of neonatal intensive care units (NICUs).
To end preventable newborn morbidity and mortality, every newborn need skilled care at birth with evidence-based practices delivered in a humane, supportive environment. Good quality of care requires appropriate use of effective clinical and non-clinical interventions, strengthened health infrastructure and optimum skills and attitude of health providers, resulting in improved health outcomes and positive experience [2]. Moreover, quality of care is considered a key component of the right to health, and the route to equity and dignity for baby [2].
In this way, some practices have been adopted to favor the humanized assistance to the baby and his family with measures that potentially reduce stress, pain, excessive manipulation and that favor the interaction between the baby and his family. So it has been with the hot tub, adapted from the immersion bath developed in the Netherlands in 1977 by doctors and nurses as a way to mimic the sensation and the stimuli experienced in the maternal uterus, allowing the relaxation, the sensation of safety and body limit that are important for the sensory organization. Physiologic responses and behavioral state changes associated with the adjunctive use hydrotherapy in developmental intervention for neonates been described [3-6].
Recently in Brazil the hot tub has been used as a form of aquatic physiotherapy or hydrotherapy an adjunct to an individualized intervention program [6-11]. Your goal is to provide a moment of pleasure for PTNB, especially those of LBW, clinically stable favoring the humanization of care and the improvement of baby´s quality of life (QoL). It is based on properties of heated water in a controlled environment with the expected outcome of reduction of pain, stress and to promote weight gain [6-11].
The therapeutic effects related to the simple immersion in the heated water and to the practice of exercises have been demonstrated, especially with respect to the improvement of blood circulation and muscle relaxation, including respiratory muscles, increased venous return, decreased sensibility in the nerve terminals, consequently of pain and HR [12-15]. It has also been demonstrated that the aquatic environment provides an increase in vital capacity and favors the development of motor coordination [14-16]. Immediately after immersion, as a consequence of the action of hydrostatic pressure, approximately 700 ml of blood is displaced from the lower limbs to the chest region, causing an increase in the venolymphatic return, resulting in a 60% increase in the central volume. Intrathoracic pressure increases from 0.4 mmHg to 3.4 mmHg and right atrial pressure increases from 14.0 mmHg to 18.0 mmHg. Central venous pressure increases from 2.0 to 4.0 mmHg to 3.0 to 16.0 mmHg. Cardiac output (blood volume × heart rate) increases associated with a decrease of approximately 10 beats per minute of HR.
However, studies of the hot tub are still scarce. The lack of standardization makes it difficult to compile and analyze the research results, both with regard to the expected outcomes and the safety related to its cardiorespiratory effects. In view of the above, the objective of the present study was to evaluate the cardiorespiratory repercussions and pain presented by PTNB during and after the hot tub.
Methods
The study was approved by the Ethics Committee of Federal University of Amazonas-UFAM (No. CAAE 54698616.2.0000.5020). From March to November 2016 twenty-one PTNB of low weight (1,250 kg to 2,500 kg) which have undergone to the hot tub in the NICU of the Balbina Mestrinho Maternity (BMM) in Manaus, Amazonas, Brazil were observed in three moments: before (moment 1), during (moment 2) and after (moment 3). In the BMM NICU the hot tub is routine for the care of PTNB with LBW, clinically stables and who are in a weight gain program. Clinical stability was considered when: the underlying disease was resolved, the baby did not need to use vasoactive amines to maintain homeostasis, the heart rate (HR) and arterial pressure (BP) were within the normal range, and do not to present fever, open wound, contagious rash, infectious disease, severe cardiovascular disease, history of uncontrolled seizures, use of peripheral venous access, hypotension, or severe hypertension.
Instruments and Procedures
Was used a standard transparent plastic tub with capacity of 9 liters filled with 6 liters of water. The bucket was placed on a bench support routinely used by the nursing staff and sanitized with chlorhexidine and 70% alcohol. The water temperature was prepared between at 36.8° and 37.4°C.
The PTNB was placed in the tub without nappies and contained in a flexor pattern through the winding with diaper towel. After the flexor pattern winding and the water volume and temperature check the first measurement of the cardiorespiratory variables was performed and the NIPS (Moment 1). The following parameters were evaluated in three moments: Moment 1: five minutes before starting the hot tub; (Moment 2): with five minutes of hot tub and (Moment 3): five minutes after the withdrawal of the PTNB of immersion: peripheral oxygen saturation (SO2), HR, and respiratory rate (RR). At moment 1 and at moment 3 was evaluated pain as the fifth vital sign. For this was used a Neonatal Infant Pain Scale (NIPS), as shown in Table 1. The NIPS is a scale composed of six questions: a physiological (FR) and five behavioral indicators (facial expression, upper and lower limb movements, crying and state of alertness), being scored from 0 to 7 being considered as pain scores greater than or equal to four [12].
| NPS | 0 point | 1 point | 2 points |
|---|---|---|---|
| Facial expression | Relaxed. | Contracted. | - |
| Cry | Absent. | Mumbling. | Vigorous. |
| Breathing | Relaxed. | Different than basal. | - |
| Arms | Relaxed. | Flexed/strerched. | - |
| Legs | Relaxed. | Flexed/stretched. | - |
| Alestness | Sleeping/Calm. | Uncomfortable. | - |
| Source: Arias and Guinsburg, 2012 [13]. | |||
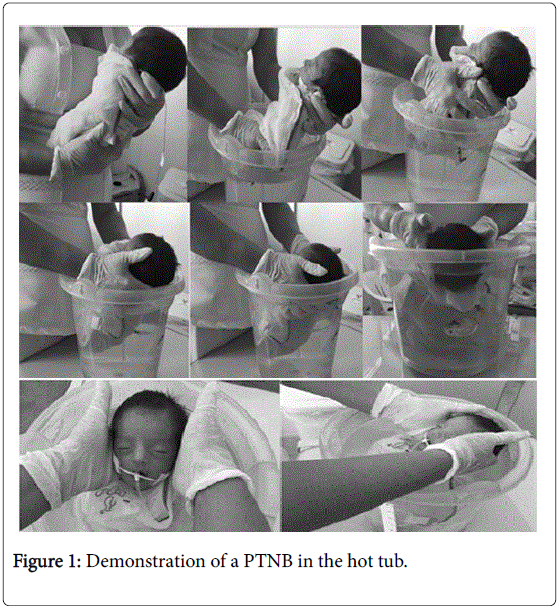
Table 1: Neonatal Infant Pain Scale (NIPS).
In order to collect the SO2 and HR variables the Dixtal® Brand device was used with the sensor positioned on the right foot of the PTNB, fixed with the manufacturer's own material and adapted with insulation for submersion readings. The RR was evaluated for one (1) minute, counting the thoracic respiratory movements.
The hot tub was performed for 10 minutes as shown in Figures 1 and 2. The PTNB was slowly immersed in the bucket in an upright posture, feet down, facing the physiotherapist, until the water was at shoulder height [13]. Physiotherapist held the PTNB with one hand in the neck and the other in the sacral region to fit it in the bottom of the bucket as if seated [12]. During the immersion, the physiotherapist associated slow, safe and coordinated movements within the water. After 10 minutes, the PTNB was slowly taken out the bucket, remained contained with a dry towel, and cuddled in the lap of the mother or caregiver for 5 minutes, during which time the cardiorespiratory variables were reassessed, as well as NIPS (Moment 3). No hygiene was performed during hydrotherapy.
All statistical analyzes were performed with software R 3.3.1 with several packages. For categorical variables, frequency and percentages were used. For the numerical variables, mean, median and standard deviation (SD) were used. The Wilcoxon test (for two categories) and Friedman (for more than 2 categories) were used to evaluate if there was a difference between the variables analyzed at moments 1, 2 and 3. The level of significance was α ≤ 0.05.
Results
Twenty-one (21) PTNB were included in the study.
None of them used supplemental oxygen, antibiotics, anticonvulsants, sedatives or analgesics. The main characteristics of PTNB were described in Table 2.
| Variables | N = 21 |
|---|---|
| Age. Chronological (days of life) | |
| Mean (SD) | 20.3 (11.5) |
| Weight (grams) | |
| Mean (SD) | 1742,3 (182,4) |
| Type of Birth | |
| Cesarean n (%) | 15 (71.4) |
| Vaginal n (%) | 6 (28.6) |
| SEX | |
| Female | 9 (42.9) |
| Male | 12 (57.1) |
| Gestacional Age (weeks at birth) | |
| Mean (SD) | 31.4 (3.3) |
Table 2: Characteristics of the PTNB included in the study.
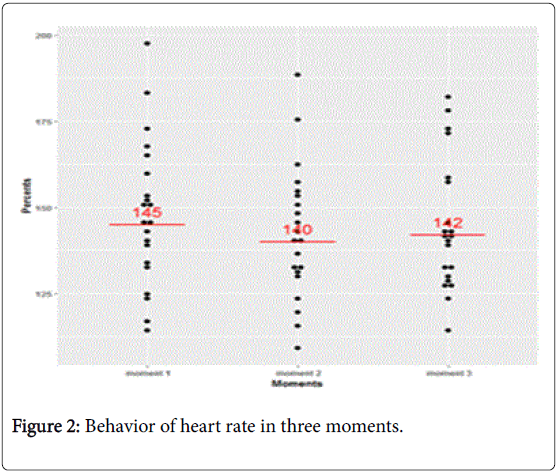
In Figure 2, it is possible to observe the behavior of HR individually in all three moments. The Table 3 presents the variables analyzed in the various moments demonstrating that there was no statistical difference in any of them. There were no intercurrences related to the hot tubs in the PTNB analyzed.
| Variables | Mean | SD | SE | Median | P value |
|---|---|---|---|---|---|
| HR moment 1 | 158,70 | 23,56 | 7,45 | 157,0 | 0.5418 |
| HR moment 2 | 140,30 | 17,99 | 5,69 | 138,5 | |
| HR moment 3 | 144,25 | 22,54 | 7,97 | 137,5 | |
| RR moment 1 | 42,10 | 8,85 | 2,80 | 46 | 0.266 |
| RR moment 2 | 43,40 | 9,47 | 2,99 | 44,5 | |
| RR moment 3 | 44,10 | 17,99 | 5,69 | 43,5 | |
| SpO2 moment 1 | 96,70 | 0,82 | 0,26 | 97,00 | 0.254 |
| SpO2 moment 2 | 95,30 | 1,77 | 0,56 | 96,00 | |
| SpO2 moment 3 | 95,50 | 2,73 | 0,96 | 96,00 | |
| NIPS Before | 1,80 | 2,44 | 0,77 | 1 | 0.4004 |
| NIPS Later | 2,40 | 2,37 | 0,75 | 3 | |
| Note: P value of the Friedman Test. Standartdesviation (SD), Standart error (SE). Heart rate (HR) data are presented in beats per minute, those of the respiratory rate (RR) in respiratory incursions per minute and those of the peripheral oxygen saturation (SpO2) in percentage. The NIPS scale goes from 0-7. Source: MBM, Manaus (Am), 2016. | |||||
Table 2: Variables analyzed according to the moment.
Discussion
Increased survival of increasingly PTNB in NICUs poses challenges to health professionals. These challenges go beyond continuous monitoring and advanced support for life preservation. They include attention to the quality of care (QoC) aimed at neuropsychomotor and affective development, functionality and QoL of these babies that are in a hostile environment and so different from the intrauterine environment [1].
WHO vision defines QoC as the extent to which health care services provided to individuals and patient populations improve desired health outcomes. In order to achieve this, health care needs to be safe, effective, timely, efficient, equitable, and people-centered [2]. This includes evidence-based practices for routine and emergency care [2].
In Brazil, the hot tub is part of the humanization of care strategy of PTNB with LBW clinically stables and who are in a weight gain program. However, is still low-researched. Although centered on the premise of baby well-being, it does not present consistent scientific evidence of its effectiveness, efficiency, or even safety. In the present study was demonstrated that there was stability of the cardiorespiratory variables analyzed during and shortly after the hot tub in PTNB with LBW without adverse effects demonstrating that it is a safe conduct.
Pereira et al. [15] carried out a randomized clinical trial with 184 healthy newborns (NB) with the objective of evaluating the thermal and cardiorespiratory adaptations during the immersion bath and shower in the first hours of life. Were compared in both types of bath HR, RR, and temperature. They demonstrated that the immersion bath promoted positive thermal and cardiorespiratory adaptations when compared to the shower bath. The immersion bath led to the reduction in HR (-0.83 ± 11.00 bpm) and RR (-1.98 ± 16.17 beats/min). However, different from the present study, they evaluated infants with normal gestational age and birth weight (gestational age ≥ 37 weeks, birth weight between 2500-3500 g) and in the immersion bath they performed corporal hygiene. In the present study, there was a reduction in HR (-8.4 ± 5.57 bpm), without no statistic change. However, in addition to the population being different, the large variability of the values between the PTNB and the small number of included individuals may have influenced these results. Clinically there was favorable responses to conduct. It was possible to observe that the PTNB during the hot tub remained calm and relaxed, and in many situations, they presented sleepiness and yawning demonstrating wellbeing with the conduct.
Evidence has shown that pain and stress cause physiological changes in cardiorespiratory, immune, hormonal and behavioral NB leading to the loss of homeostasis [3]. Barker and Rutter [15] reported that an NB in NICU can be submitted to more than 300 invasive procedures in the period of one week and emphasizes that the more immature the NB, the more procedures the same will be submitted. Another study described that in the first 24 hours of life PTNB are submitted to about 130 to 234 manipulations and among them, many of them are painful [17].
The environment of the NICU is stressful for the PTNB due to noise, strong lights and constant manipulation. However, the identification of pain and stress in this population is often difficult or devalued [12]. Many health professionals use behaviors such as crying and facial expression of the NB for pain. However, apart from crying, facial and body expression, physiological changes are parameters for assessing the presence of pain in this population and should be monitored in order not to underestimate pain. In this way, multidimensional scales such as NIPS are more adequate to assess pain in NB because they associate behavioral responses with physiological responses, making the approach more complete [12].
Although the hot tub is theoretically indicated for PTNB with pain and stress it was possible to observe that this conduct is also performed in PTNB without pain, since none of the PTNB included in this study had pain when starting the hot tub. It is possible that for this reason there was no significant change in this parameter after the hot tub. This conduct is used as a strategy of humanization of care, aiming a moment of pleasure to the PTNB and his mother or responsible, unlike the stressful environment of the NICU.
Conclusion
The hot tub did not present cardiorespiratory alterations in the low birth weight PTNB analyzed and did not cause pain, stress, or any kind of intercurrence, being a safe conduct in this regard. More research are needed to evaluate the repercussions of the hot tub in both cardiorespiratory variables and its capacity to achieve the desired outcomes, such as reducing pain and stress and favoring weight gain in this population.
References
- Mahoney MC, Cohen MI (2005) Effectiveness of Developmental Intervention in the Neonatal Intensive Care Unit: Implications for Neonatal Physical Therapy. PediatrPhysTher 17:194-208.
- Tunc alp, Were WM, MacLennan C, Oladapo OT, Gulmezoglu AM, et al. (2015) Quality of care for pregnant women and newborns-the WHO vision. BJOG 122:1045-1049.
- Sweeney JK (1983) Neonatal hydrotherapy an adjunct to developmental intervention in an intensive care nursery setting. PhysOccupTherPediatrpp: 39-52.
- Sweeny JK, Heriza CB, Blanchard Y (2009) Neonatal Physical Therapy. Part I: Clinical Competencies and Neonatal Intensive Care Unit Clinical Training Models. PediatrPhysTher21: 296-307.
- Sweeny JK, Heriza CB, Blanchard Y, Dusing SC (2010) Neonatal Physical Therapy. Part II: Practice Frame works and Evidence-based practice guidelines. PediatrPhysTher 22: 2-16.
- Tobinaga WCO, Marinho CL, Abelenda VLB, Sá PM, Lopes AG (2016) Short-Term Effects of Hydrokinesiotherapy in Hospitalized Preterm Newborns. Rehabil Res and Pract2016: Article ID 9285056.
- Gonçalves RL, Carvalho MGS, Franco FFS, Meneghini MEF, Machado Junior JA, et al. (2017) Hydrotherapy with hot tub as a physiotherapy modality in the humanized hospital setting in neonatology. In: Brazilian Association of Cardiorespiratory Physiotherapy and Physical Therapy in Intensive Care; Martins JA, Andrade LB, Ribeiro SNS, organizers. PROFISIO Updating Program in Pediatric and Neonatal Physiotherapy: Cardiorespiratory and Intensive Therapy: Cycle 6. Porto Alegre: ArtmedPanamericanapp: 59-90.
- Perini C, Seixas MC, Catão ACSM, Silva GD, Almeida VS, et al. (2014) Banho de ofurôemrecém-nascidos no alojamentoconjunto: um relato de experiência Rev PesquiCuidFundam (Online) 6: 785-792.
- Reibscheid M (2012)Banho de ofurôpropriedadesterapêuticas [Informativo]. Pediatriaemfoco [Internet].
- Oliveira RM, Silva AVS, Silva LMS, Silva APAD, Chaves EMC, et al. (2011)Implementação de medidaspara o alívio de doremneonatospelaequipe de enfermagem. Esc Anna Nery15:277-283.
- Ministério da Saúde (Brasil) (2007) Norma de atençãohumanizadaaorecém-nascido de baixo peso: MétodoCanguru. Brasília: Ministério da Saúde.
- Arias MCC, Guinsburg R (2012) Differences between: uni-and multidimensional scales for assessing pain in term newborn infants at the bedside. Clinics 67: 1165-1170.
- Ataíde VP, Barbosa JSV, Carvalho MGS, Neves SMSG, Franco FFS, et al. (2016) Ofurôemrecém-nascidospré-termo de baixo peso: relato de experiência. AssobrafirCiênciaago 7: 13-22.
- Getz M, Hutzler Y, Vermeer A (2006) Effects of aquatic interventions in children with neuromotor impairments: a systematic review of the literature. ClinRehabil 20: 927-936.
- Pereira AS, Fonseca Filho GG, Passos JOS, Almeida VA, Aquino CMR, et al. (2017) Thermal and cardiorespiratory newborn adaptations during hot tub bath: a randomized clinical trial. Int Arch Med10: 1-6.
- Barker DP,Rutter N (1995) Exposure to invasive procedures in neonatal intensive care unit admissions. Arch Dis Child Fetal Neonatal Ed72: F47-F48.
- Santos LM, Pereira MP, dos Santos LFN, de Santana RCB (2012)Avaliação da dor no recém-nascidoprematuroemUnidade de TerapiaIntensiva. Rev Bras Enferm65: 27-33.
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 3910
- [From(publication date):
October-2017 - Jul 30, 2025] - Breakdown by view type
- HTML page views : 3002
- PDF downloads : 908