Case Report Open Access
Ceftriaxone-Associated Cholelithiasis in Adult Patients with Bacterial Meningitis
| Hideto Nakajima*, Shin Ota, Takahiko Hirose, Takafumi Hosokawa, Shimon Ishida and Fumiharu Kimura | ||
| Department of Internal Medicine I, Osaka Medical College, Takatsuki, Osaka, Japan | ||
| Corresponding Author : | Hideto Nakajima Division of Neurology Department of Internal Medicine I Osaka Medical College, Takatsuki Osaka 569-8686, Japan Tel: +81-72-683-1221 Fax: +81-72-683-1801 E-mail: in1045@poh.osaka-med.ac.jp |
|
| Received August 01, 2014; Accepted August 26, 2014; Published August 30, 2014 | ||
| Citation: Nakajima H, Ota S, Hirose T, Hosokawa T, Ishida S, Kimura F (2014) Ceftriaxone-Associated Cholelithiasis in Adult Patients with Bacterial Meningitis. J Infect Dis Ther 2:161. doi: 10.4172/2332-0877.1000161 | ||
| Copyright: © 2014 Nakajima H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | ||
Related article at Pubmed Pubmed  Scholar Google Scholar Google |
||
Visit for more related articles at Journal of Infectious Diseases & Therapy
Abstract
Ceftriaxone is known to induce gallstones and intrabiliary debris as the adverse effects. Ceftriaxone-related cholelithiasis occurs mainly in children treated with a high dosage of ceftriaxone for severe infections and has been rarely reported in adults. Here we report two cases of bacterial meningitis, with cholelithiasis complication developed during ceftriaxone treatment. A 65 year old man and a 66 year old man were treated with long-term (3 weeks) administration of high-dose ceftriaxone (4 g/day) for bacterial meningitis. Both patients had renal dysfunction, which may have affected gallstone formation. In one patient, gallstones spontaneously disappeared after discontinuing ceftriaxone treatment. However, the other patient needed the drainage by endoscopic retrograde cholangiopancreatography. These events are associated with elevated doses of ceftriaxone and require particular attention in the elderly and patients with renal dysfunction.
| Introduction |
| Ceftriaxone, a third-generation cephem antibiotic, has a broad spectrum of antimicrobial activity against gram-positive and gram-negative bacteria and is a major antibacterial drug used for the treatment of bacterial meningitis [1,2]. The adverse effects of ceftriaxone include cholecystitis, cholangitis, and pancreatitis, which have been reported to be involved in the formation of gallstones and intrabiliary debris, facilitated by a component of the drug formulation [3,4]. These occur mainly in children treated with high dosage of ceftriaxone for severe infections and have been rarely reported in adults [5,6]. Here we report two cases of bacterial meningitis, with cholelithiasis complication developed during ceftriaxone treatment. |
| Keywords |
| Bacterial meningitis; Ceftriaxone; Cholelithiasis |
| Case Reports |
| Case 1 |
| The patient was a 65 year old man who had been previously treated by a physician for hypertension and hyperlipidemia. In October 2012, the patient was brought to the same physician for emergency medical care due to restlessness and delirium, following fever, headache, and lower back pain, which occurred the day before. High inflammatory reactivity and liver/kidney dysfunctions were noted in blood tests. The patient was treated with intravenous meropenem and methylprednisolone for suspected sepsis and showed improvement in fever and disturbed consciousness. However, the patient presented with nuchal rigidity and was referred to us 7 days later for suspected meningitis. No yellowing of the bulbar conjunctiva or abnormal thoracoabdominal findings was noted. The patient was alert. Apart from nuchal rigidity, negative Kernig’s sign, and hearing loss in the left ear, no other cranial nerve disorder or motor paralysis was noted. The pathological reflex was negative. |
| In the general blood tests, the white blood cell count increased to 17,000/mm3, albumin of 2.3 g/dL, GOT of 65 U/mL, GPT of 33 U/mL, BUN of 34.3 mg/dL, and creatinine of 1.49 mg/dL indicated hypoalbuminemia, impaired liver and kidney functions. Furthermore, CRP increased to 36.75 mg/dL. In the cerebrospinal fluid tests performed following the initiation of antibiotic therapy, the cell count was 58/mm3 (mononuclear cells, 97%; polymorphonuclear cells, 3%), protein level increased to 434.8 mg/dL, glucose level reduced to 13 mg/dL, and Streptococcus pneumoniae DNA was detected by PCR. The symptoms improved temporarily by treatment with meropenem, but fever and lower back pain recurred and the inflammatory reaction increased again. The antibiotic regimen was thus changed to ceftriaxone (4 g/day) combined with vancomycin and ampicillin, and the symptoms and laboratory findings improved thereafter (Figure 1). |
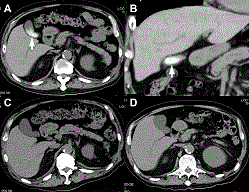
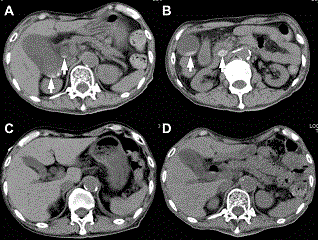
| During the course of the treatment, no abdominal pain and increase in biliary enzymes were observed. However, abdominal CT performed on the 21st day after the initiation of ceftriaxone treatment revealed biliary sludge and calculi in the gallbladder, which were absent on CT performed upon admission and spontaneously disappeared on CT performed on the 35th day after discontinuing ceftriaxone treatment. |
| Case 2 |
| The patient was a 66 year old man who had diabetes at the age of 41 years, diabetic nephropathy at the age of 63 years, and chronic renal failure. At the end of October 2012, the patient was admitted to the hospital due to traumatic acute subdural hematoma, where pulmonary congestion and pleural effusion were detected. The next day, the patient was transferred to our hospital, where he underwent emergency dialysis. The patient developed fever (38°C), headache, and nausea on the 7th day after the transfer. Nuchal rigidity was noted, and the patient was referred to us for suspected meningitis. No yellowing of the bulbar conjunctiva or abnormal thoracoabdominal findings was noted. The patient was alert. Nuchal rigidity was positive, and no cranial nerve disorder or motor paralysis was detected. Dialysis was continued and the blood test findings included BUN of 56 mg/dL, creatinine of 5.9 mg/dL, CRP of 8.4 mg/dL, albumin of 1.9 g/dL, and HbA1c of 7.6%. In the cerebrospinal fluid tests, the cell count was 256/mm3 (mononuclear cells, 46%; polymorphonuclear cells, 54%), protein level elevated to 74.3 mg/dL, and glucose level reduced to 39 mg/dL. A bacterial culture test was performed, but the causative bacteria could not be identified. |
| Initially, the patient was presumed to have bacterial meningitis or herpes simplex encephalitis and was treated with acyclovir and ceftriaxone (4 g/day). Thereafter, the patient showed improvements in symptoms and cerebrospinal fluid findings. However, fever and impairment of consciousness were observed on the 20th day after the initiation of ceftriaxone treatment, and inflammatory reactivity and the level of hepatobiliary enzymes increased. The patient was diagnosed with obstructive cholangitis on the basis of abdominal CT findings that showed stones in the gallbladder and common bile duct (Figure 2). Ceftriaxone treatment was discontinued, and the patient recovered upon drainage by endoscopic retrograde cholangiopancreatography (ERCP). |
| A routine thoracoabdominal CT scan was performed to evaluate chronic renal failure and pulmonary congestion upon admission, and no gallstones were found. However, abdominal CT performed on the 20th day after the initiation of ceftriaxone treatment revealed stones in the gallbladder and common bile duct. After ERCP drainage and discontinuation of ceftriaxone, the stones in the gallbladder and common bile duct shrunk and eventually disappeared (Figure 2). |
| Discussion |
| Ceftriaxone is a third-generation cephem antibiotic with a broad antibacterial activity against aerobic and anaerobic gram-positive and gram-negative bacteria. It is widely used for bacterial infections, particularly for biliary infection and meningitis, because of its efficient migration to the bile and cerebrospinal fluid. Ceftriaxone is characterized by a high rate of biliary excretion, which accounts for approximately 40% of excretion, whereas the remaining 60% of the drug is excreted in the urine [7,8]. In patients with renal dysfunction, biliary elimination is increased slightly. Therefore, it has been thought that dosage of this drug did not need to be reduced in patients with chronic kidney disease [9]. The half-life of ceftriaxone in blood is 7-8 h in healthy adults, but has been reported to increase to 13.5 h in the elderly and to 21.4 h in the elderly with renal dysfunction [10]. |
| The concentration of excreted ceftriaxone in bile is 20- to 150-folds higher than that in the serum, and the drug readily binds to calcium to form biliary sludge [3]. Biliary sludge reportedly emerges in 3-22 days (mean, 9 days) after the initiation of ceftriaxone administration and disappears in 2-63 days (mean, 15 days) after discontinuation [6]. In most cases, the biliary sludge formed disappears spontaneously following the discontinuation of ceftriaxone or water administration; this is sometimes referred to as biliary pseudolithiasis [9]. However, this condition requires attention, because the sludge can develop to gallstones and cause complications such as acute cholecystitis and obstructive cholangitis, and an endoscopic procedure or surgery becomes necessary in some cases [11,12]. |
| While some studies have reported that ceftriaxone-associated biliary sludge and calculi caused colic attack, cholecystitis, and pancreatitis, others have reported that ceftriaxone-associated biliary sludge and calculi remained predominantly asymptomatic and were found in 25%-46% of the patients when they were actively subjected to abdominal ultrasonography after ceftriaxone treatment [13-16]. Therefore, it is conceivable to conclude that ceftriaxone-induced biliary sludge remains unnoticed in many patients. |
| Cholelithiasis caused by the administration of ceftriaxone has been reported to occur mainly in children, with incidence rates varying between 10% and 40%. Therefore, high-dose or bolus administration of ceftriaxone, dehydration, hypoalbuminemia, calcium-containing transfusion material, and complication with renal diseases in the elderly and children are associated with an increased risk of developing ceftriaxone-induced cholelithiasis [17]. The two patients presented in this report were under long-term (3 weeks) administration of high-dose ceftriaxone (4 g/day) for bacterial meningitis treatment, and were under conditions that facilitated the formation of gallstones. Both the patients indicated in this report had renal dysfunction, which must have increased the half-life of ceftriaxone in blood. These conditions may have affected gallstone formation. Although the biliary pseudolithiasis disappears spontaneously after discontinuation of ceftriaxone in most cases, we should be aware of this adverse effect of ceftriaxone to adjust a drug dose. It would be advisable to evaluate an abdominal ultrasound or CT in every patient being treated with ceftriaxone who presents suggestive signs of acute biliary tract obstruction, especially in patients with renal dysfunction. |
| Conclusion |
| In the treatment of bacterial meningitis involving an increased dose of ceftriaxone, adequate attention should be paid to the emergence of biliary sludge and calculi as a possible adverse effect in the elderly and patients with renal dysfunction. |
References
- Begg N, Cartwright KA, Cohen J, Kaczmarski EB, Innes JA, et al. (1999) Consensus statement on diagnosis, investigation, treatment and prevention of acute bacterial meningitis in immunocompetent adults. British Infection Society Working Party. J Infect 39:1-15.
- Heyderman RS, Lambert HP, O'Sullivan I, Stuart JM, Taylor BL, et al. (2003) Early management of suspected bacterial meningitis and meningococcal septicaemia in adults.J Infect 46: 75-77.
- Park HZ, Lee SP, Schy AL (1991) Ceftriaxone-associated gallbladder sludge. Identification of calcium-ceftriaxone salt as a major component of gallbladder precipitate. Gastroenterology 100:1665-1670.
- Shaffer EA (2001) Gallbladder sludge: what is its clinical significance?CurrGastroenterol Rep 3: 166-173.
- Schaad UB, Tschäppeler H, Lentze MJ (1986) Transient formation of precipitations in the gallbladder associated with ceftriaxone therapy.Pediatr Infect Dis 5: 708-710.
- Schaad UB, Wedgwood-Krucko J, Tschaeppeler H (1988) Reversible ceftriaxone-associated biliary pseudolithiasis in children.Lancet 2: 1411-1413.
- Brogard JM, Blickle JF, Jehl F, Arnaud JP, Paris-Bockel D, et al. (1988) High biliary elimination of ceftriaxone in man.Int J ClinPharmacolTherToxicol 26: 167-172.
- Shiffman ML, Keith FB, Moore EW (1990) Pathogenesis of ceftriaxone-associated biliary sludge. In vitro studies of calcium-ceftriaxone binding and solubility.Gastroenterology 99: 1772-1778.
- Heim-Duthoy KL, Caperton EM, Pollock R, Matzke GR, Enthoven D, et al. (1990) Apparent biliary pseudolithiasis during ceftriaxone therapy.Antimicrob Agents Chemother 34: 1146-1149.
- Joynt GM, Lipman J, Gomersall CD, Young RJ, Wong EL, et al. (2001) The pharmacokinetics of once-daily dosing of ceftriaxone in critically ill patients.J AntimicrobChemother 47: 421-429.
- Robertson FM, Crombleholme TM, Barlow SE, Verhave M, Brown D (1996) Ceftriaxone choledocholithiasis.Pediatrics 98: 133-135.
- Famularo G, Polchi S, De Simone C (1999) Acute cholecystitis and pancreatitis in a patient with biliary sludge associated with the use of ceftriaxone: a rare but potentially severe complication. Ann Ital Med Int 14:202-204.
- Kim YS, Kestell MF, Lee SP (1992) Gall-bladder sludge: lessons from ceftriaxone.J GastroenterolHepatol 7: 618-621.
- Schaad UB, Tschäppeler H, Lentze MJ (1986) Transient formation of precipitations in the gallbladder associated with ceftriaxone therapy.Pediatr Infect Dis 5: 708-710.
- Ozturk A, Kaya M, Zeyrek D, Ozturk E, Kat N, et al. (2005) Ultrasonographic findings in ceftriaxone: associated biliary sludge and pseudolithiasis in children.ActaRadiol 46: 112-116.
- Biner B, Oner N, Celtik C, Bostancioğlu M, Tunçbilek N, et al. (2006) Ceftriaxone-associated biliary pseudolithiasis in children.J Clin Ultrasound 34: 217-222.
- Palanduz A, Yalçin I, Tonguç E, Güler N, Oneş U, et al. (2000) Sonographic assessment of ceftriaxone-associated biliary pseudolithiasis in children.J Clin Ultrasound 28: 166-168.
Figures at a glance
 |
 |
|
| Figure 1 | Figure 2 |
Relevant Topics
- Advanced Therapies
- Chicken Pox
- Ciprofloxacin
- Colon Infection
- Conjunctivitis
- Herpes Virus
- HIV and AIDS Research
- Human Papilloma Virus
- Infection
- Infection in Blood
- Infections Prevention
- Infectious Diseases in Children
- Influenza
- Liver Diseases
- Respiratory Tract Infections
- T Cell Lymphomatic Virus
- Treatment for Infectious Diseases
- Viral Encephalitis
- Yeast Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 16522
- [From(publication date):
October-2014 - Aug 18, 2025] - Breakdown by view type
- HTML page views : 11834
- PDF downloads : 4688
