Research Article Open Access
Clinicoepidemiological Profile and Predictors of Mortality in LBW Babies:A Hospital Based Observational Study
Ishtiyaq Q*, Aijaz AM and Qazi I
Department of Pediatrics, G.B Panth Childrens Hospital, Srinagar, Jammu and Kashmir, India
- *Corresponding Author:
- Ishtiyaq Q
Department of Pediatrics
G.B Panth Childrens Hospital
Srinagar, Jammu and Kashmir, India
Tel: 917006872230
Fax: +278615107002
E-mail: iqadri80@gmail.com
Received Date: December 09, 2016; Accepted Date: December 19, 2016; Published Date: December 26, 2016
Citation: Ishtiyaq Q, Aijaz AM, Qazi I (2016) Clinicoepidemiological Profile and Predictors of Mortality in LBW Babies: A Hospital Based Observational Study. Neonat Pediatr Med 2: 119. doi: 10.4172/2572-4983.1000119
Copyright: © 2016 Ishtiyaq Q, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Neonatal and Pediatric Medicine
Abstract
Introduction: Low birth weight has a significant impact on the survival of a newborn. Low birth weight babies are at risk for a number of serious clinical problems and as such contribute to overall neonatal mortality and morbidity. Aims: The aim was to study the clinicoepidemiological profile and predictors of mortality in low birth weight babies in resource limited settings. Materials and methods: This was a prospective observational study conducted from July 2013 to May 2015. The study group included neonates admitted in NICU having birth weight less than 2500 gms. Newborns with congenital or chromosomal anomalies were excluded from the study. Data was collected regarding various epidemiological and clinical parameters and entered as per a preset proforma. Results and inference: Total of 100 eligible LBW newborns were studied. Incidence of LBW admission was found to be 17.3%. There were 26 deaths among LBW neonates. Birth weight, gestational age, mechanical ventilation, shock on admission, NEC, sepsis, and CRIB score were found to have a statistically significant association with mortality.
Keywords
LBW babies; Mortality risk factors; Sepsis; Shock; Mechanical ventilation; Crib score
Introduction
Low birth weight has been defined by the World Health Organization (WHO) as weight at birth of less than 2500 grams (5.5 pounds) [1]. This practical cut-off for international comparison is based on epidemiological observations that infants weighing less than 2500 grams are approximately 20 times more likely to die than heavier babies [2]. India, the most populous country in South Asia shares a very high prevalence of low birth weight babies (LBW). The incidence of low birth weight in India has been reported to range from 21% to 33% as compared to 4.5% in industrially developed countries [3]. Survival of LBW infants is a rising trend more so in developed countries. However LBW neonatal deaths continue to constitute a major part of infant mortality rate in developing countries. A number of indicators like birth weight, gestational age, apgar score, antenatal steroids, gender and CRIB score have been evaluated in low birth weight neonates for predicting mortality in different studies. However there is paucity of studies done in evaluating low birth weight neonates with reference to risk factors associated with their mortality and there epidemiological characteristics in our resource limited settings.
Materials and Methods
This study was conducted in the neonatal I.C.U Skims Soura. The sample consisted of all those neonates admitted in NICU, who were born as LBW. The cut off weight for including the neonates in the study was taken as birth weight of less than 2500 gms. All those neonates who were born with congenital malformations or chromosomal anomalies were not included in the study. Eligible candidates were followed up to 28 days of postnatal life. A detailed history was collected about the baby as well as the mother. Relevant data regarding course of events during the gestational period was sought.
A detailed general physical and systemic examination was performed. Gestational age was recorded according to LMP and by new Ballards scoring. A CRIB score was assigned to each baby based on gender, gestational age, presence or absence of congenital malformations, base excess on admission, minimum and maximum Fio2 requirement during first 12 hours of admission. During the NICU stay monitoring for common neonatal problems like sepsis, meningitis, hypoglycaemia, hyperglycaemia, hypocalcaemia, polycythaemia, jaundice, hypoxia/acidosis, necrotizing enterocolitis, feed intolerance, hypothermia etc. was done. Investigations were done as required according to the condition of the neonate. The daily examination, complications and investigations during the NICU stay were entered as per the preset proforma. The study collected data about the outcome of NICU stay during first 28 days of life. The neonatal outcome was studied and various risk factors were assessed with regard to their statistical significance in predicting mortality in LBW neonates.
Results
There were a total of 866 admissions during the study period. 150 were LBW neonates. The incidence of LBW admission was 17.3%. Out of 150 LBW neonates, 50 neonates did not meet the inclusion criteria, and hence were excluded from the study. 55 neonates from the study sample were females (55%) and 45 were males (45%). The number of neonates born at term in the study population was 44 and those admitted as preterm were 56. 80 neonates were born by vaginal delivery and 20 were born by LSCS. 81 neonates were born at a hospital and 19 were born at home. The number of neonates whose mothers had antenatal visits was 78 and 22 mothers had not visited any antenatal clinic during pregnancy. From the study population 74 patients were low birth weight (LBW), 13 were very low birth weight (VLBW) and 13 were extremely low birth weight (ELBW). The number of appropriate for gestational age (AGA) neonates was 53 and the number of small for gestational age (SGA) neonates was 47. The mean gestational age of the study population was 34.70 weeks with standard deviation of 4.82. Minimum gestational age was 24 weeks and maximum gestational age was 40 weeks. The mean birth weight was 1.80 kg with a standard deviation of 0.56. Minimum birth weight recorded in the study was 0.50 kg while as maximum was 2.42 kg. Mean Apgar score at one minute was 5.69 with standard deviation 1.47. Mean Apgar score at 5 minutes was 7.11 with standard deviation of 1.22. Mean Crib score was 4.08 with minimum score of 0 and maximum score of 15. Mean maternal age was 27.41 years with standard deviation of 3.97. Minimum age was 20 years and maximum was 35 years (Table 1).
| Clinical Problems | Frequency |
|---|---|
| RDS | 36 |
| Shock | 34 |
| Hypoglycemia | 33 |
| Sepsis | 27 |
| NNJ | 24 |
| Apnea | 19 |
| Coagulopathy | 17 |
| NEC | 14 |
| Meningitis | 9 |
| MAS | 9 |
| Birth asphyxia | 7 |
| Seizures | 6 |
| Polycythemia | 4 |
Table 1: Clinical problems encountered and their frequency.
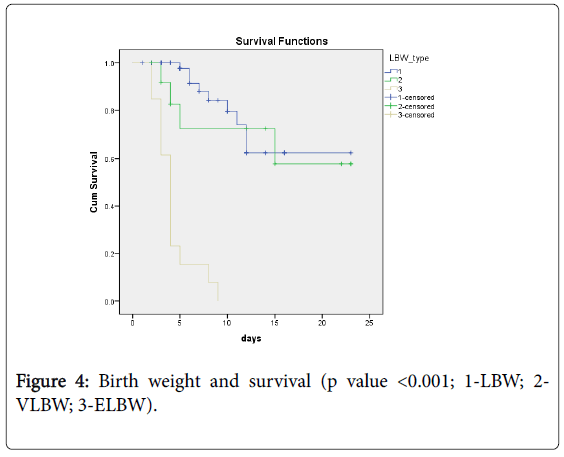
There were 26 deaths in the study group. 65 LBW neonates were discharged and nine 9 died. Out of 13 VLBW neonates 9 were discharged and 4 died. Whereas within 13 ELBW neonates there were no survivors with a 100% mortality. The differences were statistically significant (p<0.001).
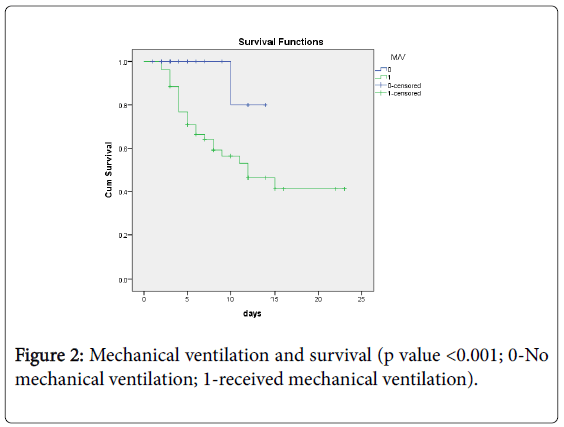
52 neonates received mechanical ventilation out of which 27 were discharged and 25 died. Whereas within 48 neonates who did not, 47 were discharged and only 1 died. The difference between these two groups was statistically significant (p<0.001).
34 patients had shock out of which twenty five 25 died and nine 9 survived. Within 66 neonates without shock 65 survived and only 1 patient died. This difference was also statistically significant (p<0.001).
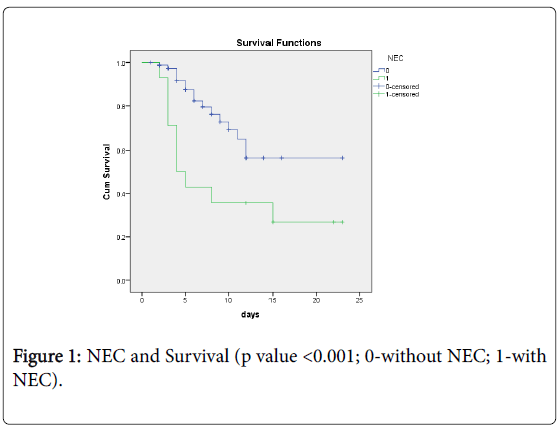
14 neonates developed NEC out of which four 4 were discharged and 10 died. Among 86 patients that did not develop NEC 76 survived and 16 died. The difference was again statistically significant (p<0.001).
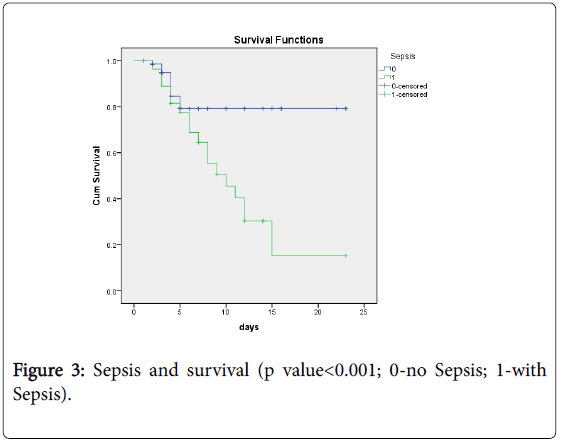
Among 73 patients who were sepsis free 64 survived and 9 died, while as among 27 patients having sepsis 10 survived and 17 died. This difference was statistically significant (P<0.001).
Also there was a statistically significant difference in Crib score between neonates (Table 2) who died and those neonates who survived (P Value-0.001).
| Group | Median | Min | Max |
|---|---|---|---|
| Survived 2 | 0 | 6 | 3 |
| Died | 10 8 | 15 | 4.5 |
Table 2: CRIB Score and survival.
Kaplan Meier survival curves till discharge were made for independent predictors of mortality. Survival analysis showed a statistical significant difference in survival between LBW neonates, who had risk factors under study (Sepsis, mechanical ventilation, NEC and low birth weight) with those who did not have these risk factors (Figures 1-4).
Discussion
LBW contributes significantly to neonatal mortality in our country. While as incidence of LBW as well as mortality among LBW neonates have significantly come down in developed countries, these variables are still high in developing countries.
The mortality rate in our study was 26% which is in between mortality rates of developing and developed countries. Ezeaka, et al. [4] studied outcome of LBW babies in Logos Nigeria and found a mortality of 23.2%, which is similar to the mortality found in our study. Brito, et al. [5] also found a mortality of 23% in his study. One study by Njuguna FM, et al. [6] from Kenya demonstrated a mortality rate of 51.6% among LBW neonates. It is a reflection of differences in quality of medical care, health care facilities and infrastructure.
The difference between mortality among LBW, VLBW and ELBW neonates was found to be statistically significant as was found in a number of other studies conducted by Gera, et al., Basu, et al., Terzic, et al., Dong, et al., Mukhyopadhyay, et al. [7-11]. This observation is consistent with our clinical understanding that survival decreases as birth weight decreases. In our study there were 13 ELBW neonates and mortality was 100% in this group. However most of neonates [12] in this group consisted of those with extreme prematurity with severe RDS. Neonates with extreme prematurity pose a significant challenge with respect to survival. They need intensive care and treatment of associated complications in high dependency units with provision of facilities like high frequency ventilation, NO and ECMO. However our NICU was lacking these facilities as is the case with most level III NICUs in our country.
The study found that mechanically ventilated LBW neonates had significantly high mortality in comparison to non-ventilated neonates. Mukhyopadhyay et al. [11] found similar results in a study that aimed at predicting mortality and major morbidity in extremely low birth weight neonates. Study by Chye, et al. [12] also found mechanical ventilation as a risk factor predicting mortality in LBW infants. Those neonates who need mechanical ventilation are usually very sick. Also neonates on mechanical ventilation are exposed to ventilator associated problems like barotrauma, ventilator associated pneumonia, unintended respiratory alkalosis, impairment of hepatic, renal and cardiac functions. As a result these, neonates are at increased risk for adverse outcome. Premature LBW neonates requiring mechanical ventilation are particularly vulnerable to adverse effects of invasive ventilation. In our study higher mortality among LBW neonates receiving mechanical ventilation could be attributed to this reason. Therefore our study suggests that the need to start mechanical ventilation in a sick LBW neonate should be clearly established before putting the neonate on mechanical ventilation and the neonate extubated as soon as feasible.
We studied the impact of shock on admission to NICU and it was found that neonates with shock on admission had a higher mortality as compared to those who did not have shock on admission. Out of 34 patients with shock on admission 20 were later on found to have sepsis also. The association of shock with adverse outcome in LBW neonates was found in other studies also. For example studies done by Kermorvant-Duchemin, et al. [13], Mukhyopadhyay, et al. [11] showed similar results. However our study was different in that we studied impact of shock on admission only. Development of shock later on during course of hospital stay was not taken into consideration.
Sepsis had a significant impact on mortality of LBW neonates in our study. Among 27 patients who developed sepsis 17 died and 10 survived. 15 of these 17 neonates who died also had shock on admission, while as among the rest of 10 patients with sepsis only 5 had shock on admission. Similarly among 34 patients who had shock on admission 20 patients had sepsis. These results show that shock and sepsis are closely related in sick LBW neonates. And the combined impact of shock and sepsis together on mortality was more significant than either one alone.
Necrotising enterocolitis was one more variable that was studied as a risk factor for neonatal mortality and it was found that there is a statistically significant difference in mortality between those neonates who had NEC and those who did not. A total of 14 neonates developed NEC, out of which 10 died and 4 survived. All of the 4 neonates who survived were term neonates with LBW and had stage I of NEC. Rest of the neonates with NEC was premature and progressed to advanced stages of NEC.
Our study found that CRIB score was a significant predictor of mortality risk. It is an easy to use clinical score to assess the risk of severity of illness in LBW babies as it consists of variables that are part of initial assessment of a sick neonate. In our study the median CRIB score for survived group was 2 and median CRIB score for expired group was 10. The difference was statistically significant. Terzic, et al. [9] and Brito, et al. [5] also had similar results while assessing mortality in very low birth weight babies. However our study studied usefulness of CRIB score in all admitted LBW babies.
Conclusion
Birth weight, mechanical ventilation, shock on admission, sepsis, NEC and CRIB score are important predictors of mortality in LBW neonates admitted in ICU.
References
- Kramer MS (1987) Determinants of LBW, Methodological assessment and mete-analysis. WHO Bull 65: 663-737.
- WHO (2004) Low Birth Weight: Country, Regional and Global Estimates. Geneva.
- UNICEF (1997) The progress of nations, New York, United Nations Children's Fund.
- Ezeaka VC, Ekure EN, Iroha EO, Egri-Okwaji MT (2004) Outcome of low birth weight neonates in a tertiary health care centre in Lagos, Nigeria. Afr J Med Med Sci 33: 299-303.
- Brito AS, Matsuo T, Gonzalez MR, de Carvalho AB, Ferrari LS (2003) CRIB score, birth weight & gestational age in neonatal mortality risk evaluation. Rev Saude Publica 37: 1-9.
- Njuguna FM, Kiptoon P, Nyandiko W (2014) An assessment of the overall mortality of low birth weight neonates at the new birth units of the Moi teaching & referral hospital in Eldoret, Kenya. European Journal of Biology & Medical Science Research 2: 63-71.
- Gera T, Ramji S (2001) Early predictors of mortality in very low birth weight neonates. Indian Pedaitrics 38: 596-602.
- Basu S, Rathore P, Bhatia BD (2008) Predictors of mortality in very low birth weight neonates in India. Singapore Med J 49: 556-560.
- Terzic S, Heljic S (2012) Assessing mortality risk in very birth weight infants. Med Arh 66: 76-79.
- Dong Y, Guang Y, Jia-lin Y (2012) Changes in perinatal care & predictors of In-hospital mortality for very low birth weight preterm infants. Iran J Pediatr 22: 326-332.
- Mukhopadhyay K, Louis D, Mahajan R, Kumar P (2013) Predictors of mortality & major morbidities in extremely low birthweight neonates. Indian Pediatrics 50: 1119-1123.
- Chye JK, Lim CT (1999) Very low birth weight infants- mortality & predictive risk factors. Singapore Med J 40: 565-570.
- Kermorvant-Duchemin E, Laborie S, Rabilloud M, Lapillonne A, Claris O, et al. (2008) Outcome and prognostic factors in neonates with septic shock. Pediatr Crit Care Med 9: 186-189.
Relevant Topics
- About the Journal
- Birth Complications
- Breastfeeding
- Bronchopulmonary Dysplasia
- Feeding Disorders
- Gestational diabetes
- Neonatal Anemia
- Neonatal Breastfeeding
- Neonatal Care
- Neonatal Disease
- Neonatal Drugs
- Neonatal Health
- Neonatal Infections
- Neonatal Intensive Care
- Neonatal Seizure
- Neonatal Sepsis
- Neonatal Stroke
- Newborn Jaundice
- Newborns Screening
- Premature Infants
- Sepsis in Neonatal
- Vaccines and Immunity for Newborns
Recommended Journals
Article Tools
Article Usage
- Total views: 4193
- [From(publication date):
December-2016 - Aug 25, 2025] - Breakdown by view type
- HTML page views : 3174
- PDF downloads : 1019