Review Article Open Access
Closed Reduction & Percutaneous Fixation of Lisfranc Joints Injuries: Possibility, Technique & Results
Sherif Mohamed Abdelgaid*, Mahmoud Salah, Samir Abdulsalam and Farid AbdulmalakConsultant Orthopedic Surgeon, AL-Razi Orthopedic Hospital, Kuwait
- *Corresponding Author:
- Sherif Mohamed Abdelgaid
Consultant Orthopedic Surgeon
AL-Razi Orthopedic Hospital, Kuwait
Tel: 0096524898124, 0096599539270
E-mail: Sherifmaa@yahoo.com
Received Date: January 17, 2013; Accepted Date: April 29, 2013; Published Date: May 03, 2013
Citation: Abdelgaid SM, Salah M, Abdulsalam S, Abdulmalak F (2013) Closed Reduction & Percutaneous Fixation of Lisfranc Joints Injuries: Possibility, Technique & Results. Clin Res Foot Ankle 1:109. doi: 10.4172/2329-910X.1000109
Copyright: © 2013 Abdelgaid SM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Clinical Research on Foot & Ankle
Abstract
Introduction: Lisfranc joint injuries are the most common injuries of the midfoot. Injuries include (1) pure Lisfranc joint dislocations, (2) Lisfranc joint fracture dislocations, (3) combined Chopart-Lisfranc joint fracture dislocations, (4) complex Lisfranc joint fracture dislocations with entrapped tibialis anterior tendon and (5) segmental Lisfranc fracture dislocation with concomitant fracture metatarsal neck or head or dislocation of metatarsophalangeal joints. Treatment options vary from closed or open reduction followed by K. wires, screws or plate fixation or primary arthrodesis.
Material and Methods: 35 patients with 37 cases of Lisfranc’s joint injuries were treated in Al-Razi orthopedic hospital, Kuwait during the period from January 2006 to December 2010. Injuries were classified using Hardcastle classification. Closed reduction was tried first followed by percutaneous fixation with cannulated 3.5 mm screws for medial 3 joints & K wire fixation for lateral (4th & 5th) TMT joints. Closed reduction was failed in 5 cases and open reduction was performed.
Results: Functional results were assessed clinically using AOFAS Midfoot rating scale. The mean follow up period was 24 to 48 months (mean, 38 months). Excellent results were obtained in 15 cases 40.5%; results were good in 15 cases 46%; % fair results obtained in 3 cases 8% and poor results in 2 cases 5.5%.
Conclusion: The associated soft tissue injury with Lisfranc joint injury may interfere with surgical treatment of the injury increasing the risk of wound complications like wound dehiscence and deep infection. Early diagnosis of Lisfranc joint injuries allows closed or percutaneous reduction and fixation before massive soft tissue swelling. This minimally invasive treatment decreases the complication rate and allow early rehabilitation compared with the traditional method of open reduction. However open reduction is indicated in cases of complex Lisfranc injury with entrapped tibialis anterior tendon and in combined injury of Lisfranc joint with Chopart or metatarsophalangeal joints to avoid worse results associated with closed or percutaneous reduction in these types of injuries.
Keywords
Percutaneous - Lisfranc’s injury; Hardcastle classification
Introduction
Lisfranc joint dislocations or fracture dislocations are the most common severe injuries of the midfoot [1]. They account for 0.2% to 0.8% of all fractures [2]. The S shaped tarsometatarsal joint complex (Lisfranc joint) consists of the distal row of tarsal bones, the cuneiforms and the cuboid, which articulate with the bases of the five metatarsals. Lisfranc joint is divided into three columns; the medial column is formed by the base of the 1st metatarsal and the medial cuneiform, the middle column is formed by the 2nd & 3rd metatarsals and their respective cuneiforms and the lateral column is formed by the 4th & 5th metatarsals and the cuboid [3]. The base of the 2nd metatarsal, is recessed into a ‘mortise’ between the medial and lateral cuneiforms, and stabilizes the joint [4]. The main stabilizing structure of the tarsometatarsal joint is a Y-shaped interosseous ligament (Lisfranc’s ligament) extends to the plantar surface from the lateral aspect of the medial cuneiform to the medial aspect of the base of the second metatarsal. Together with the inter cuneiforms interosseous ligament, it is one of the most important structures involved in the stability of the joint and disruption in either of these ligaments will cause instability between the medial and middle columns. Inter-metatarsal and thin dorsal ligaments connect the 2nd, 3rd, 4th, & 5th metatarsals with no inter-metatarsal ligament between the bases of 1st & 2nd metatarsals [5].
The two major causes of Lisfranc’s joint injuries are low-energy like in certain types of sports-related injuries and high-energy as motor vehicle accident. Injuries are caused by a direct blow to the joint or by axial loading along the metatarsal bones, either with medially or laterally directed rotational forces [6]. In most cases an indirect trauma causes a longitudinal force to a plantar flexed foot ruptures the dorsal tarsometatarsal ligaments, and fractures the plantar aspect of the metatarsal bases. Additional forces may shift the metatarsals on the tarsus producing abduction and lateral displacement and leading to compression fractures of tarsal bones of Chopart joint (navicular and cuboid bones). The resultant Lisfranc’s joint injuries include pure Lisfranc joint dislocations, Lisfranc joint fracture dislocations or combined Chopart-Lisfranc joint fracture dislocations [7]. A rare type of Lisfranc injury is the segmental Lisfranc fracture dislocation with concomitant dislocation of the 1st metatarsophalangeal joint (floating metatarsal). Subtypes of these injuries include Lisfranc injury with fracture neck or head of lesser metatarsals or dislocation of metatarsophalangeal joints. The mechanism of segmental injury involves axial loading to the metatarsal heads with the foot plantar flexed and the toes dorsiflexed. This will create additional elements of torque, compression and rotation on the metatarsals & tarsal bones through tensioning its soft tissue attachments including plantar fascia & interosseous muscles and will generate various forms of osteo-articular and soft tissue damage [8-10]. Another type of unusual injuries is the so called, complex Lisfranc fracture dislocation characterized by the presence of Lisfranc fracture dislocation and a distance between the medial and middle cuneiform. It is better to categorize this injury as a separate type of Lisfranc joint injury due to its unique patho-anatomical and radiological features with the inherent irreducibility by closed means due to tibialis anterior tendon interposition between the cuneiform bones that blocks the reduction. The characteristic radiologic feature of this is a cuneiforms diastasis [11]. Several classification systems have been described for Lisfranc fracture dislocations. The most commonly used classification is the Hardcastle classification modified by Myerson et al. [12]: Type A refers to a total incongruity, B to a partial incongruity (B1 medial column and B2, affecting one or more tarsometatarsal joint of the middle or lateral column) and type C to a divergent injury with the 1st metatarsal displaced medially and the middle and lateral column laterally.
Treatment options vary from closed reduction, closed reduction and percutaneous pinning, open reduction and temporary screw fixation, screw fixation combined with external fixation and primary arthrodesis in severe fracture dislocations [13]. Indications for operative treatment includes: 1) Widening >4 mm of the space between first and second metatarsals in antero-posterior x-ray view. 2) Tarso- Metatarsal incongruence of >2 mm. 3) Entrapment of bony fragments in the joint. (e.g. fragment of 2nd metatarsal bone (M.T.B) base ). 4) Entrapment of soft tissue in a joint, (e.g., tibialis anterior tendon) the so-called complex dislocation [14]. Stavlas et al in 2010 performed a comprehensive review (257 patients in eleven articles)of clinical studies reporting on the management of Lisfranc fracture–dislocations. They concluded that Small fragment screw application (3.5- and 4.0 mm) seems to be the preferred method of management for the injuries in the joints of the medial and the middle column (first, second and third metatarsals), while K-wires can be used for the stabilization of the lateral column (fourth and fifth metatarsals) in case of instability. Screws may create postoperative discomfort or complications but it is not clear when and if they should be removed. Routine hardware removal, was described in four studies after a prespecified period of time (8-12 weeks), after completion of healing in two studies, it was suggested only if it caused problems (i.e. broken screws) in two studies, while in three others no recommendation about hardware removal was given. Regarding the type of hardware, screws were removed at eight weeks in 37 patients (14.4%) , at 12 weeks in 30 patients (11.6%) and at 16 weeks in 45 patients (17.5%). On the other hand, K-wires were usually removed after six to eight weeks [3].
Articular surface damage by single transarticular 3.5-mm screw varied from 2.0% to 4.8%. The amount of arthritis is directly proportional to the area of damage on the articular surface [15,16]. This did not seem to cause any problems [17,18]. Unlike transarticular screws, joint-spanning locking plates, do not cause further damage to the articular surfaces and theoretically less likely to contribute to posttraumatic arthritis. However a larger exposure is required for their insertion when compared with insertion of percutaneous screws [19].
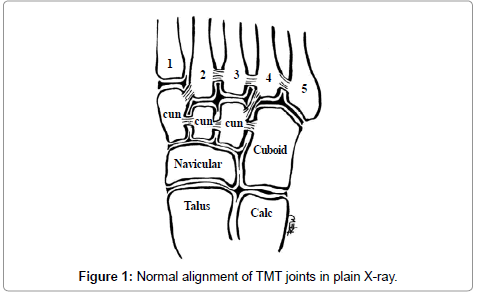
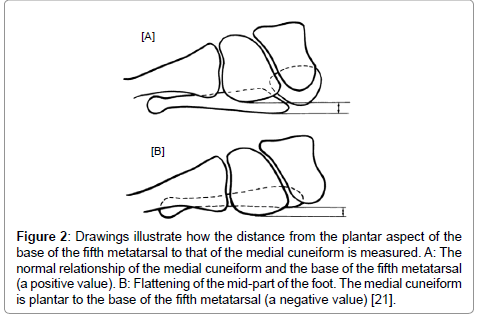
The quality of reduction is assessed through A.P, lateral and oblique views of the foot. The normal alignment of the midfoot includes that the lateral border of the base of the 1st metatarsal aligns with the lateral border of the 1st cuneiform, the medial border of the base of the 2nd metatarsal aligns with the medial border of the 2nd cuneiform, and the lateral border of the base of the 3rd metatarsal aligns with the lateral border of the 3rd cuneiform. The medial border of the base of the 4th metatarsal may align with the medial border of the cuboid; however, differences of 1 mm to 2 mm are not uncommon. The 5th tarsometatarsal relationship is more variable; if present, a notch on the articulating surface of the 5th metatarsal may align with the lateral aspect of the cuboid (Figure 1) [20]. In lateral weight-bearing radiographs the distance from the plantar aspect of the 5th metatarsal to that of the medial cuneiform is measured. Normally the medial cuneiform was dorsal to the fifth metatarsal (positive value). Abnormal negative value is assigned when the medial cuneiform is plantar to the fifth metatarsal (Figure 2) [21].
Figure 2: Drawings illustrate how the distance from the plantar aspect of the base of the fifth metatarsal to that of the medial cuneiform is measured. A: The normal relationship of the medial cuneiform and the base of the fifth metatarsal (a positive value). B: Flattening of the mid-part of the foot. The medial cuneiform is plantar to the base of the fifth metatarsal (a negative value) [21].
Aim
To assess the possibility and review the results of closed or percutaneous reduction of different types of Lisfranc joint injuries, followed by percutaneous fixation of the joints of the medial and the middle column (first, second and third metatarsals) by 3.5 mm cannulated screws and fixation of lateral column (fourth and fifth metatarsals) by K-wires. Routine K-wires removal at the end of the 6th week while the screws were removed only if they caused problems
Materials and Methods
From January 2006 to December 2010, a total of 37 cases of Lisfranc joint fracture-dislocation in 35 patients (two patients had bilateral injuries) were operated on at Al-Razi orthopedic hospital in Kuwait and available for study. Patients were 21 males and 14 females. The mean age was 36.5 years (range, 17–72 years). The mechanism of injury was Motor Vehicle Accident in 12 patients (M.V.A), Fall From Height (F.F.H) in 12 patients, sport related injury (mainly football playing) in 6 patients, fall of a heavy object in 3 patients and simple fall in two patients. Associated injuries were found in 13 patients. The study includes, 21 cases of Lisfranc fracture dislocations, 9 cases of pure Lisfranc dislocations, 3 cases of segmental Lisfranc fracture dislocation with fracture head metatarsals, 2 cases with combined Chopart-Lisfranc fracture dislocations and 2 cases with complex Lisfranc fracture dislocation In all cases, the injury was closed, and all cases (except one) were operated on within 48 hours from the time of injury and achieved a closed reduction except in 4 cases in which closed reduction was filled and open reduction was performed. Injuries were classified according to the modified Hardcastle classification system. Either with closed or open reduction, radiologic anatomical reduction of Lisfranc joint was achieved in all cases according to criteria reported by Foster et al. and Faciszewski et al. [20,21].
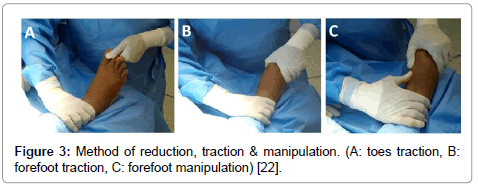
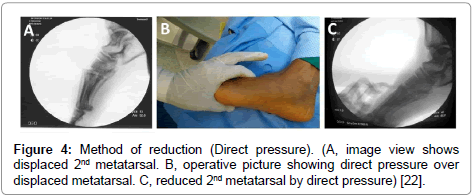
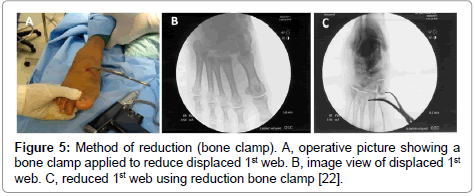
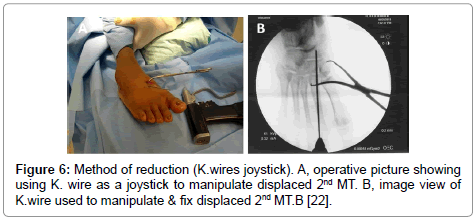
Surgical techniques: using the same technique reported by 3 of the authors in 2012 [22]. Under general or spinal anesthesia and without using a tourniquet, closed reduction was tried first by traction through the toes and counter- traction through the leg. This realigns the forefoot with the midfoot and regains the length of the foot. Then we applied forefoot varus or valgus stress to reduce varus or valgus deformity focusing on restoring articular congruity (Figure 3). Direct pressure was then applied to reduce the individual metatarsal in its anatomic position (Figure 4). Pointed bone reduction forceps was used to reduce the displaced bone, closing joint gap & temporary maintain the reduction (Figure 5). K. wire through the distal shaft of displaced metatarsal can be used as a joystick to manipulate the displaced metatarsal, then advanced through the base of the bone and crossing the joint in its articulation with cuneiform or cuboid bone (Figure 6). The medial column was fixed by 3.5 cannulated screws as follows:
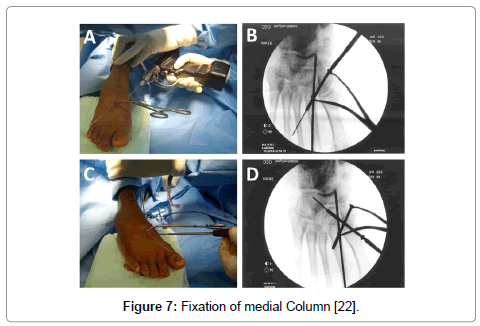
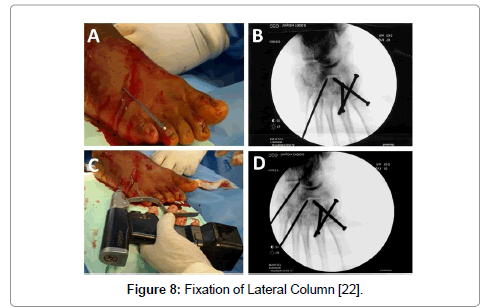
(1) One screw from medial cuneiform to the base of 2nd MTB (Figure 7A and B). (2) Additional stability can be obtained by insertion of one screw in crossing manner with first screw i.e. from the base of the 1st metatarsal (MT) to the intermediate cuneiform. (Figure 7C and D). (3) In cases of comminution of 2nd MT base, splinting of the base of the 2nd MTB by insertion of two screws, one from the base of 1st MT to medial cuneiform and 2nd screw from base of 3rd MT to the lateral cuneiform. Fixation of Lateral Column was done using one or two K. wires inserted through the base of 4th MT and/or 5th MT and directed proximally through the cuboid bone. Following fixation of medial and lateral column, stability of middle column was checked (Figure 8). Usually this joint became stable as it was splinted by the medial and lateral column but if instability was noticed we fixed the joint with one transarticular crossing screw. If closed reduction was failed, then open reduction was performed through two longitudinal incisions. One incision through the 1st web space to reduce the medial & middle columns and the 2nd incision through the 4th web space to reduce the lateral column. Then fractures were fixed as was done after closed reduction. Postoperative radiographs were assessed in anteroposterior, lateral and oblique views. Patients were followed up in the outpatient clinic initially in 2-week intervals up to 6 weeks, then every 6 weeks for 3 months, every 3 months for one year, and then every 6 months. Our protocol in postoperative follow up was: (1) Non weight bearing for 6 weeks. (2) Removal of K. wires at the end of 6th week. (3) Partial weight bearing was allowed for another 6 weeks. (4) Full weight bearing started at the end of the third month. (5) The results were evaluated using the functional criteria proposed by the AOFAS Midfoot Scale of American Orthopedic Foot and Ankle Society. (6) Forty five points were assigned to function, forty points to pain, and fifteen points to alignment (total hundred points). Excellent results equal 90–100 points, good results equal 75–89 points, fair results equal 60–74 points and poor results are less than 60 points [23] (7) Assessment of Lisfranc joint for osteoarthritic changes was done using the criteria of Paley & Hall scoring system (Table 1) [24].
| Grade 0 | Normal joint space with no evidence of degenerative cysts or subchondral sclerosis |
| Grade 1 | Osteophytes, subchondral sclerosis, and cysts without joint space narrowing |
| Grade 2 | Joint space narrowing |
| Grade 3 | Complete loss of joint space |
Table 1: Paley and Hall scoring system for subtalar osteoarthritic changes [21].
Results
The follow-up duration ranged from 24 to 48 months (mean, 38 months). Closed reduction was achieved in 32 cases (86.5% of cases). Open reduction was indicated in five cases with; complex fracture dislocation (2 cases) and combined Chopart-Lisfranc fracture dislocations (2 cases). The 5th case of open reduction was of a case of Lisfranc fracture dislocation type in which the diagnosis was late due to head trauma with coma and patient was operated in 2nd week. Unfavorable results occurred in cases of high injury trauma associated with ipsilateral foot injuries (Table 2 and 3). In the closed reduction group, excellent results were obtained in 13 cases, good results were obtained in 16 cases and fair results obtained in 3 cases. In the open reduction group, excellent results were obtained in 2 cases, good results in 1 case and poor results in 2 cases (Table 4). Results according to classification type showed that, satisfactory results were obtained in all cases with Type A (12 cases), 12 cases of 15 cases with type B and in 8 of 10 cases with type C (Table 5).
| Mechanism | Number of cases | % | Results | |||
|---|---|---|---|---|---|---|
| Excellent | Good | Fair | Poor | |||
| M.V.A | 12 | 32.5 | 4 cases | 5 cases | 1 case | 2 cases |
| F.F.H | 14 in 12 patients (2 bilateral) | 38 | 5 cases | 8 cases | 1 case | - |
| Sport | 6 | 16 | 3 cases | 2 Cases | 1 case | |
| Fall of heavy object | 3 | 8 | 2 Cases | 1 case | - | - |
| Simple fall | 2 | 5.5 | 1 case | 1 case | - | - |
Table 2: Results according to mechanism of injury.
| Associated injuries | Number of cases | Prognosis |
|---|---|---|
| Ipsilateral Femur | 1 | Good |
| Ipsilateral lateral Malleolus & 2nd, 3rd & 4th MT Heads | 1 | Fair |
| Ipsilateral Cuboid & 5th MT base | 1 | Excellent |
| Ipsilateral Chopart fractures (Cuboid & Navicular tuberosity) | 1 | Poor |
| Ipsilateral dislocated Chopart + fracture navicular & 3rd MT shaft | 1 | Excellent |
| Head injury with occipital & zygomatic bone fractures | 1 | Poor |
| Pelvis | 2 | Good |
| Contralateral acetabulum & os calcis | 1 | Good |
| Ipsilateral 2nd & 3rd MT Heads | 1 | Fair |
| Contralateral Tibial Plateau | 1 | Excellent |
| Ipsilateral 2nd MT shaft | 2 | Excellent |
Table 3: Cases with associated injuries and their prognosis.
| NO | Type of injuries | Classification | Method of fixation | AOFAS Score | Results |
|---|---|---|---|---|---|
| 1 | Lisfranc fracture dislocations | B2 | Closed | 100 | Excellent |
| 2 | Pure Lisfranc dislocations | B1 | Closed | 87 | Good |
| 3 | Pure Lisfranc dislocations | A | Closed | 87 | Good |
| 4 | Segmental Lisfranc fracture dislocation | C | Closed | 97 | Fair |
| 5 | Lisfranc fracture dislocations (extra-articular # cuboid)) | C | Closed | 64 | Poor Good |
| 6 | Pure Lisfranc dislocations | B2 | Closed | 88 | Good |
| 7 | Lisfranc fracture dislocations | B2 | Closed | 87 | Good |
| 8 | Segmental Lisfranc fracture dislocation | B1 | Closed | 85 | Good Fair |
| 9 | Combined Chopart-Lisfranc fracture dislocations | B2 | Closed | 59 | Poor |
| 10 | Complex Lisfranc fracture dislocation | C | Open | 85 | Good |
| 11 | Lisfranc fracture dislocations | B2 | Closed | 92 | Excellent |
| 12 | Pure Lisfranc dislocations | B 2 | Closed | 87 | Good |
| 13 | Lisfranc fracture dislocations | B 2 | Closed | 82 | Good |
| 14 | Lisfranc fracture dislocations | A | Closed | 70 | Good |
| 15 | Pure Lisfranc dislocations | A | Closed | 100 | Excellent |
| 16 | Lisfranc fracture dislocations | B 1 | Closed | 100 | Excellent |
| 17 | Lisfranc fracture dislocations | B 2 | Closed | 90 | Excellent |
| 18 | Pure Lisfranc dislocations | A | Closed | 97 | Excellent |
| 19 | Lisfranc fracture dislocations | C | Closed | 87 | Good |
| 20 | Pure Lisfranc dislocations | B 2 | Closed | 87 | Good |
| 21 | Lisfranc fracture dislocations | B 2 | Closed | 82 | Good |
| 22 | Combined Chopart-Lisfranc fracture dislocations | A | Open | 70 | Excellent |
| 23 | Lisfranc fracture dislocations | A | Closed | 100 | Good |
| 24 | Lisfranc fracture dislocations | B 1 | Closed | 100 | Excellent |
| 25 | Pure Lisfranc dislocations | B 2 | Closed | 90 | Good |
| 26 | Lisfranc fracture dislocations | A | Closed | 97 | Good |
| 27 | Lisfranc fracture dislocations | C | Closed | 87 | Excellent |
| 28 | Lisfranc fracture dislocations | B 2 | Closed | 87 | Good |
| 29 | Segmental Lisfranc fracture dislocation | B 2 | Closed | 82 | Fair |
| 30 | Lisfranc fracture dislocations | A | Open | 70 | Poor |
| 31 | Lisfranc fracture dislocations | A | Closed | 100 | Good |
| 32 | Complex Lisfranc fracture dislocation | B 1 | Open | 100 | Excellent |
| 33 | Lisfranc fracture dislocations | B 2 | Closed | 87 | Good |
| 34 | Lisfranc fracture dislocations | B 2 | Closed | 82 | Good |
| 9* | Combined Chopart-Lisfranc fracture dislocations | B2 | Open | 59 | Poor |
| 35 | Pure Lisfranc dislocations | A | Closed | 70 | Good |
| 36 | Lisfranc fracture dislocations | A | Closed | 100 | Good |
| 37 | Lisfranc fracture dislocations | B 1 | Closed | 100 | Excellent |
Table 4: Number of cases & results according to injury type.
| Type | Number of cases | % | Results | |||
|---|---|---|---|---|---|---|
| Excellent | Good | Fair | Poor | |||
| A | 12 | 32.5 | 5 Cases | 7 Cases | - | - |
| B | 15 | 40.5 | 7 Cases | 5 Cases | 2 Cases | 1 Case |
| C | 10 | 27 | 3 Case | 5 Cases | 1 Case | 1 Case |
Table 5: Number of cases & results according to modified Hardcastle type.
No infection or skin complications in all cases. Patients returned to normal activity on an average of 3.5 months. One of the five patients with poor had combined Lisfranc & Chopart fracture dislocation. The 2nd case with poor result had a head injury with occipital & zygomatic bone fractures. The three cases with fair results had associated ipsilateral multiple fracture metatarsal Heads. On follow up, 8 cases (21.5%) of the patients showed degenerative changes of secondary osteoarthritis during the 2nd and 3rd postoperative year. All cases were asymptomatic mild arthritic changes with only one case showed moderate degenerative changes (patient with Fracture dislocation of Lisfranc joint, head trauma, open reduction and poor outcome). 5 cases with mild arthritic changes are cases with pure dislocation of Lisfranc joint. The other two cases, one had segmental Lisfranc fracture dislocation and the 2nd was a combined Chopart-Lisfranc fracture dislocation case.
Discussion
Diagnosis and treatment of Lisfranc joint injuries especially Lisfranc joint fracture dislocations, are still problems in trauma care and influence the functional outcome of the entire foot in the mid and long-term follow-up [7]. The factors influencing the results of treatment for Lisfranc injuries include: (1) Initial degree of soft tissue injury. (2) Time from injury to operate. (3) The accuracy of reduction [25].
Early surgical treatment is very important in preventing and/ or treating any foot compartmental syndrome which is the most frequent and feared complication [26].
As a minimally invasive surgery, closed reduction & percutaneous screw fixation of Lisfranc fracture dislocation has the following advantages; decreased chance of wound breakdown and infection, faster recovery time, shorter hospital stay, decreased peri-operative morbidity, and early rehabilitation compared with traditional open procedures.
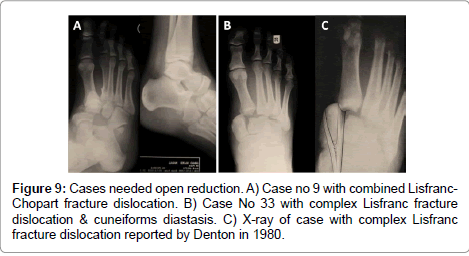
Using closed or percutaneous reduction followed by percutaneous fixation of Lisfranc joint injuries, our study showed a low complication rate with no cases of compartmental syndrome or infection. Percutaneous reduction was failed in 5 cases. Two of these cases were complex Lisfranc fracture dislocation with entrapped tibialis anterior tendon. This is matched with that was reported by Denton et al in 1980. Denton found that the complex Lisfranc fracture dislocation was irreducible by closed means and need open reduction [11] (Figure 9). Two of the cases needed open reductions were cases of combined Chopart-Lisfranc joint fracture dislocation with fractured navicular and cuboid bones. This matches what was reported by Richter in 2002 that combined Chopart- Lisfranc fracture dislocation results in a high degree of residual impairment and anatomic open reduction should be done to improve the final outcome [7]. The 5th case needed open reduction was a case of isolated Lisfranc fracture dislocation in comatose patient due to head trauma with occipital & zygomatic bone fractures. This patient diagnosed and operated in the 2nd post- injury week with poor final prognosis. This correlates with the findings reported by Pereira et al in 2008 that unfavorable functional results are directly proportional to the length of time elapsed between diagnosis and treatment (the longer the period of delay the lower the score) [27]. Our results showed 3 cases of fair results. All of these had associated ipsilateral fracture metatarsal heads. These findings point to the correlation between ipsilateral injury of Lisfranc& metatarsophalangeal joints and the worse results. Comminution and small size of head fragments in our cases directed our treatment to be focused mainly in anatomical reduction and fixation of Lisfranc joint component of this combined injury. This concept of treatment is matched with that was reported by Hekman in 1991. He said that if a closed reduction fail, one can accept healing in malaligned position and plan for a corrective osteotomy later if necessary [28]. Recently the worse results obtained in the three cases with this variant of Lisfranc injury changed our concept of its treatment to be similar to what is mentioned by Drosos et al in 2000. They said that anatomical reduction with an open approach of all components (TMT & MTP joints) of this type of injury lead to an excellent clinical and radiological result [29].
Regarding the post-traumatic osteoarthritis, our results highlight two important findings; 1) arthritic changes especially of mild type are radiologic findings not necessary implicate clinical symptoms, 2) patients with purely ligamentous injury (five of nine patients, 55.5% in our study) had a trend toward a higher prevalence of posttraumatic osteoarthritis compared with patients sustained combined ligamentous and osseous injuries (three of twenty eight patients 11% in our study). This finding is similar to that was reported by Kuo et al. [30]. However our results of post-traumatic osteoarthritis depend on midterm follow up and in future, the long-term of follow up may change the grade of radiologic & clinical findings and in turn alters the final scores.
Conclusion
Closed reduction and percutaneous fixation of Lisfranc joint injuries has the advantages of minimally invasive surgery, decrease the complication rate and allow early rehabilitation compared with the traditional method of open reduction. However open reduction is indicated from the start in cases of complex Lisfranc injury with entrapped tibialis anterior tendon since the closed reduction is usually filled with this injury. Also open reduction is indicated in cases of Lisfranc joint injuries combined with Chopart or metatarsophalangeal joint fracture dislocation to avoid worse results associated with failed closed or percutaneous reduction in these complicated injuries.
References
- Suren EG, Zwipp H (1989) [Dislocation fractures of the Chopart and Lisfranc joint]. Unfallchirurg 92: 130-139.
- Rosenberg GA, Patterson BM (1995) Tarsometatarsal (Lisfranc's) fracture-dislocation. Am J Orthop (Belle Mead NJ) Suppl: 7-16.
- Stavlas P, Roberts CS, Xypnitos FN, Giannoudis PV (2010) The role of reduction and internal fixation of Lisfranc fracture-dislocations: a systematic review of the literature. Int Orthop 34: 1083-1091.
- Berg JH, Silveri CP, Harris M (1998) Variant of the Lisfranc fracture-dislocation: a case report and review of the literature. J Orthop Trauma 12: 366-369.
- Sarafian SK. Syndesmology (1983) In: Sarafian SK (Ed) Anatomy of the foot and ankle: descriptive, topographic, and functional. (2nd Edn), Lippincott Williams & Wilkins, Philadelphia.
- Turchin DC, Schemitsch EH, McKee DM (1987) American Orthopedic Foot and Ankle Society. (AOFAS) mid-foot scoring scale. J Trauma 27: 343–348.
- Richter M, Thermann H, Huefner T, Schmidt U, Krettek C (2002) Aetiology, treatment and dislocations and fracture outcome in Lisfranc joint dislocations, Foot and Ankle Surgery 8:21-32.
- Myerson M (1989) The diagnosis and treatment of injuries to the Lisfranc joint complex. Orthop Clin North Am 20: 655-664.
- Kasmaoui H, Bousselmame N, Bencheba D, Boussouga M, Lazrek K, et al. (2003) The floating metatarsal. A rare traumatic injury. Acta Orthop Belg 69: 295-297.
- Leibner ED, Mattan Y, Shaoul J, Nyska M (1997) Floating metatarsal: concomitant Lisfranc fracture-dislocation and complex dislocation of the first metatarsophalangeal joint. J Trauma 42: 549-552.
- Denton JR (1980) A complex Lisfranc fracture-dislocation. J Trauma 20: 526-529.
- Myerson MS, Fisher RT, Burgess AR, Kenzora JE (1986) Fracture dislocations of the tarsometatarsal joints: end results correlated with pathology and treatment. Foot Ankle 6: 225-242.
- Trevino SG, Kodros S (1995) Controversies in tarsometatarsal injuries. Orthop Clin North Am 26: 229-238.
- Kuo RS, Tejwani NC, Digiovanni CW, Holt SK, Benirschke SK, et al. (2000) Outcome after open reduction and internal fixation of Lisfranc joint injuries. J Bone Joint Surg Am 82-82A: 1609-18.
- Panchbhavi VK (2004) Knee-stabilising device for lower limb orthopaedic procedures. Ann R Coll Surg Engl 86: 54-55.
- Alberta FG, Aronow MS, Barrero M, Diaz-Doran V, Sullivan RJ, et al. (2005) Ligamentous Lisfranc joint injuries: a biomechanical comparison of dorsal plate and transarticular screw fixation. Foot Ankle Int 26: 462-473.
- Arntz CT, Veith RG, Hansen ST Jr (1988) Fractures and fracture-dislocations of the tarsometatarsal joint. J Bone Joint Surg Am 70: 173-181.
- Yuen JS, Yung SW, Wong MK (2001) Open reduction and temporary rigid internal fixation of Lisfranc fracture-dislocations. Singapore Med J 42: 255-258.
- Thordarson DB, Hurvitz G (2002) PLA screw fixation of Lisfranc injuries. Foot Ankle Int 23: 1003-1007.
- Foster SC, Foster RR (1976) Lisfranc's tarsometatarsal fracture-dislocation. Radiology 120: 79-83.
- Faciszewski T, Burks RT, Manaster BJ (1990) Subtle injuries of the Lisfranc joint. J Bone Joint Surg Am 72: 1519-1522.
- Abdelgaid SM, Salah M, Abdel-Malak F, Closed reduction and percutaneous fixation of Lisfranc joint fracture dislocations, Kuwait Medical Journal 2012; 44 (3): 200-210.
- Kitaoka HB, Alexander IJ, Adelaar RS, Nunley JA, Myerson MS, et al. (1994) Clinical rating systems for the ankle-hindfoot, midfoot, hallux, and lesser toes. Foot Ankle Int 15: 349-353.
- Paley D, Hall H (1993) Intra-articular fractures of the calcaneus. A critical analysis of results and prognostic factors. J Bone Joint Surg Am 75: 342-354.
- Stavlas P, Roberts CS, Xypnitos FN, Giannoudis PV (2010) The role of reduction and internal fixation of Lisfranc fracture-dislocations: a systematic review of the literature. Int Orthop 34: 1083-1091.
- Ahmed S, Bolt B, McBryde A (2010) Comparison of standard screw fixation versus suture button fixation in Lisfranc ligament injuries. Foot Ankle Int 31: 892-896.
- Pereira C, Espinosa E, Miranda I, Pereira M, Canto R (2008) evaluation of the surgical treatment of Lisfranc joint fracture-dislocation. Acta Ortop Bras 16: 93-97.
- Heckman JD. Fractures and dislocations of the foot (1991) In: Rockwood CA, Green DP, Bocholt RW, (Eds) Rockwood and Green's Fractures in Adults. (3rd Edn) Lippincott, Philadelphia.
- Drosos GI, Gavalas NS, Papoutsidakis AN (2000) Concomitant Lisfranc fracture-dislocation and displaced neck fractures of the lesser metatarsals: a case report. Foot and Ankle Surgery 6: 49-54
- Kuo RS, Tejwani NC, Digiovanni CW, Holt SK, Benirschke SK, et al. (2000) Outcome after open reduction and internal fixation of Lisfranc joint injuries. J Bone Joint Surg Am 82-82A: 1609-18.
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 22515
- [From(publication date):
July-2013 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 17647
- PDF downloads : 4868