Research Article Open Access
Comparison of Aggressive and Traditional Postoperative Rehabilitation Protocol after Rotator Cuff Repair: A Meta-analysis
| Tsun-Shun Huang, Shwu-Fen Wang and Jiu-Jenq Lin* | |
| School and Graduate Institute of Physical Therapy, College of Medicine, National Taiwan University, 100 Taipei, Taiwan | |
| Corresponding Author : | Jiu-Jenq Lin School and Graduate Institute of Physical Therapy College of Medicine, National Taiwan University, Taiwan E-mail: jiujlin@ntu.edu.tw |
| Received July 02, 2013; Accepted July 27, 2013; Published July 30, 2013 | |
| Citation: Huang TS, Wang SF, Lin JJ (2013) Comparison of Aggressive and Traditional Postoperative Rehabilitation Protocol after Rotator Cuff Repair: A Metaanalysis. J Nov Physiother 3:170. doi:10.4172/2165-7025.1000170 | |
| Copyright: © 2013 Huang TS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
Introduction: In addition to size/location of tear, surgical technique, and fixation methods, a well-programmed rehabilitation protocol is also critical to successful tendon healing and satisfactory shoulder functional outcome for patients with rotator cuff repair (RCR). To date, the progression of rehabilitation is still debated.
Purpose: The aim of this meta-analysis is to analyze the effects of a post-operative aggressive protocol versus those of a traditional rehabilitation protocol. Methods: We searched the database of PubMed, Ovid MEDLINE, CINAHL, Cochrane library, and CEPS and finally included 6 articles that met our selection criteria.
Results: The aggressive postoperative rehabilitation protocol results in more improvement in ROM and shoulder function than the traditional protocol, but it also entails a greater risk of un-healing or re-tearing of the rotator cuff tendon.
Conclusion: Although the aggressive postoperative rehabilitation protocol has positive effects for patients with RCR, factors influencing the risk of un-healing/re-tearing of the tendon should be further investigated. These factors are important to consider in the design of a post-operative program for patients with RCR.
| Keywords |
| Rotator cuff repair; Rehabilitation; Aggressive; Range of motion; Function |
| Introduction |
| Rotator cuff tears are a common cause of shoulder pain and dysfunction, with a prevalence of 13% in subjects aged 50 years and one of 50% after the age of 80 [1]. Nonoperative treatment can be applied to patients with small incomplete tears. When conservative treatment options have failed, surgical repair of the rotator cuff is recommended. One problem with the surgical approach is that the capacity for healing of tendon to bone varies. The rate of recurrent tears after repair ranges from 16% for non-retracted tears in young subjects to 94% for massive tears [2,3]. With rapidly advancements in surgical techniques such as open repair, mini-open repair, and arthroscopic repair, optimal rehabilitation following rotator cuff repair has become more important and challenging [4]. The size and location of tear, surgical technique and fixation methods, and a wellprogrammed rehabilitation protocol are key factors for successful tendon healing and satisfactory shoulder functional outcome. |
| The postoperative rehabilitation protocols for duration of immobilization, passive/active motion, and aggressive post-operative treatment are still under debate. An aggressive rehabilitation protocol is defined as early use of passive or active range of motion exercise, increased dosage of a rehabilitation protocol, an accelerated or intensive rehabilitation protocol, or combined pre-operative rehabilitation [1,5-7]. Early passive movement after surgery is recommended to prevent postoperative stiffness. Raab et al. (1996) demonstrated that early continuous passive motion after repair resulted in faster improvement in range of motion (ROM) and pain relief. Other authors, however, have reported that immobilization for 4 to 6 weeks after rotator cuff repair may promote tendon healing [8-11]. Additionally, early motion after repair had negative effects on rotator cuff healing, such as a higher unhealed rate and even rotator cuff retearing [3]. On the other hand, one recent study found no negative impact from early active motion in week 4 after surgery [12]. Recently, improvements in surgical techniques have also improved the possibility of an early or aggressive post-operative treatment protocol. |
| From the literature, no consensus has been reached on a standard rehabilitation protocol for patients with RCR. So far, no systemic reviews or meta-analysis of the differences between an aggressive rehabilitation protocol and the traditional protocol have been reported. The objective of the present meta-analysis is to analyze the effects of a post-operative aggressive protocol versus those of the traditional rehabilitation protocol on shoulder range of motion, shoulder function, and the risk of rotator cuff tendon un-healing or re-tearing in patients with RCR. |
| Methods |
| Search strategy |
| Two physical therapists performed the initial review independently. Databases including PubMed, Ovid MEDLINE, Cumulative Index to Nursing and Allied Health Literature (CINAHL), Cochrane library, and Chinese electronic periodical service (CEPS) were searched. Additionally, a hand search of the references of the papers found was performed. Initially, PubMed was searched using the keywords “rotator cuff repair”. That phrase was paired with “aggressive”, “early”, “progressive”, or “accelerated”, all of which are related to the meaning of aggressive, and with “physical therapy”, “rehabilitation”, “exercise”, or “motion”, all of which were related to the meaning of intervention. These steps were then repeated for the other databases. All searches were limited to studies on humans. |
| Studies were included if they were published between 2000 and December 2012 and met the following criteria: (1) they were randomized controlled trials that compared the effects of an aggressive post-operative rehabilitation protocol versus those of a traditional protocol, (2) the participants in the studies received rotator cuff repair, (3) the studies used at least 1 of the following outcome measures: pain, shoulder range of motion, shoulder function, or status of anatomic structure of rotator cuff tendon, and (4) they were published in English with the full text. Studies were excluded if the participants had confirmed cervical radiculopathy, autoimmune disease, and metastatic disease or if the studies did not provide the mean and standard deviations or 95% confidence interval for at least 1 of the outcome measures. |
| Methodological Quality Evaluation |
| Each article included in the present study was evaluated by 2 physical therapists using the Physiotherapy Evidence Database (PEDro) scale [13]. The PEDro is often used to assess the quality of intervention type of randomized controlled trials with adequate reliability and validity [14,15]. It is composed of 11 questions, each of which is scored yes or no, with 1 point gain for each affirmative response. The first question, which is used to investigate the internal validity, is not calculated in the total score, so the maximum score is 10 points. Evaluators answer affirmatively only if the information is explicitly stated in the studies. The following ranges were used to qualify the methodological quality: a score of 9 to 10 points was excellent-quality study; 6 to 8 points was good-quality study; 4 to 5 points was fair-quality study; lower than 4 points was poor-quality study. |
| Statistical analysis |
| In this meta-analysis, we used Review manager software (v5.2 Cochrane IMS) to integrate the results of different studies. The experimental group was the aggressive post-operative rehabilitation protocols, and the control group was the traditional rehabilitation protocol. For all continuous variables, the differences of mean and standard deviations were used to calculate the standardized mean differences (SMDs), also called the standardized effect size. For categorical variables, the odds ratio was demonstrated. Before we combined all studies to calculate the total SMDs, we used the I2 test to estimate the homogeneity between the studies. In this study, homogeneity refers to the similarity of SMDs in different studies. Higher values indicate lower homogeneity between studies, and generally, lower than 25% indicates high homogeneity. The results of homogeneity determined the calculation methods of SMDs. The fix-effect model was used to combine SMDs in the high homogeneity condition, and the random-effect model was used in the low homogeneity condition. The aim of choosing the correct model was to estimate the total SMDs appropriately. If the total SMDs and the range of 95% CI were not equal to zero, the aggressive protocol had a significant difference from the traditional protocol. Cohen demonstrated that the effect size of 0.2 to 0.3 is a small effect, 0.3 to 0.8 is a medium effect, and more than 0.8 is a large effect [16]. If the total SMDs and the range of 95% CI were across zero, it indicated that there were no significant differences between the aggressive protocol and the traditional protocol. |
| Results |
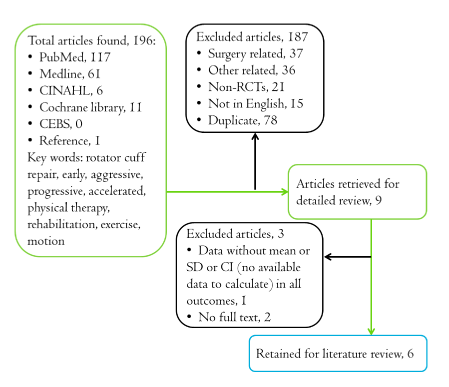
| Figure 1 presents the flowchart of the literature search. The initial search of all the databases turned up 196 articles. Of those, 187 articles were eliminated based on their titles and abstracts because they were non-related articles on the effects of surgery, they were not randomized-controlled trials or in English, or duplicates from different databases. The remaining 9 articles were examined to confirm they contained the full text. Two articles lacked the full text, and one article did not have the mean value and SD or 95% CI in all outcome measures, making it impossible to calculate for SMDs. In the end, 6 articles were retained for meta-analysis. Four of the articles investigated the effects of early post-operative passive ROM exercise and those of a traditional protocol; [1,6,15,17] one investigated the differences between increased dosages of passive ROM exercise, which added continuous passive motion (CPM) and a traditional protocol; [17] and one article investigated the effects of early postoperative active ROM exercise and pre-operative exercise (aggressive rehabilitation protocol) compared to those of a traditional protocol [18]. The characteristics of the included studies are presented in Table 1. The quality scores of the PEDro scores for each question are presented in Table 2. The overall mean PEDro score was 4.50, with an SD of 0.55. All articles were fair-quality studies. |
| Outcome Measures |
| Range of motion (ROM) |
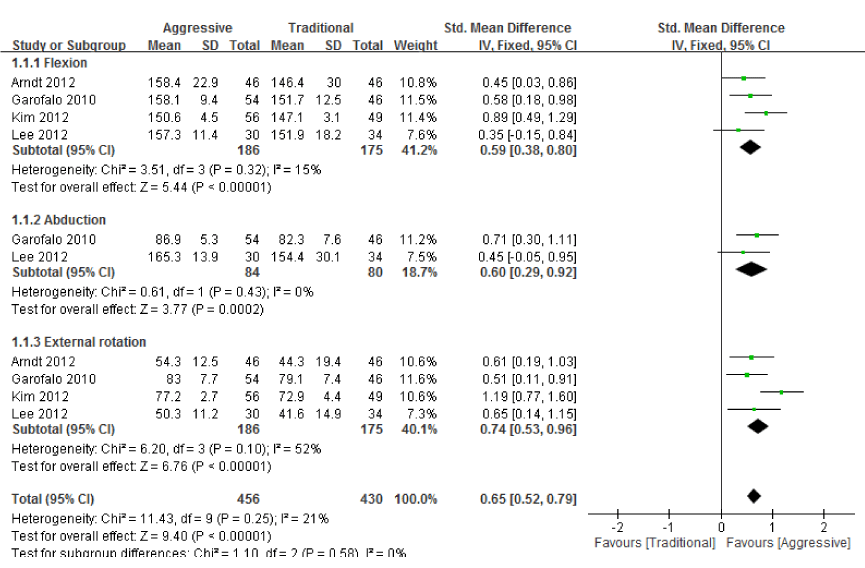
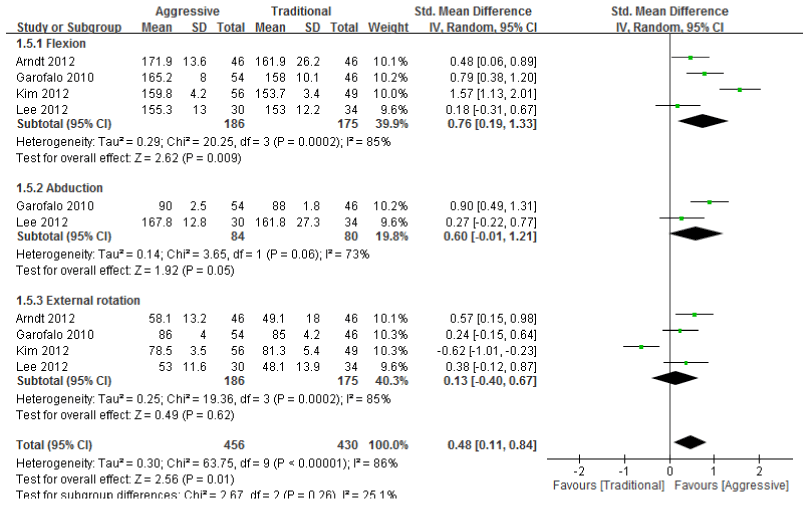
| Four articles included ROM as an outcome and compared the effects of an aggressive rehabilitation protocol to those of a traditional protocol on ROM, including flexion, abduction, and external rotation at 6 months and 1 year after surgery [1,11,15,17]. The outcome of external rotation was only investigated in 2 studies [11,17]. Combining the results of these 4 studies at 6 months after surgery by using the fixed-effects model yielded an SMD of 0.59 (95% CI: 0.38~0.80) in ROM of flexion, an SMD of 0.60 (95% CI: 0.29~0.92) in ROM of abduction, and an SMD of 0.74 (95% CI: 0.53~0.96) in ROM of external rotation. The total SMDs combining 3 outcomes of ROM were 0.65 (95% CI: 0.52~0.79), with the positive values in favor of aggressive rehabilitation protocol (p<0.00001). Figure 2 shows the SMDs of individual studies. I2=0.21 indicates that 21% of the variation was due to heterogeneity between studies. The data of 1 year after surgery were combined using random-effects model, yielding an SMD of 0.76 (95% CI: 0.19~1.33) in ROM of flexion, an SMD of 0.60 (95% CI: -0.01~1.21) in ROM of abduction, and an SMD of 0.13 (95% CI: -0.40~0.67) in ROM of external rotation. The total SMDs combining 3 outcomes of ROM were 0.48 (95% CI: 0.11~0.84), which indicated that the aggressive protocol resulted in more improvement in overall ROM than traditional protocol did (p=0.01), although parts of the ROM (abduction and external rotation) had no significant difference (p=0.05 and 0.62, respectively). The random-effects model was used due to high I2 range from 73% to 85%. Figure 3 shows individual study SMDs. We combined 3 outcomes of ROM with meta-analysis, represented as overall ROM of a patient. |
| Shoulder function |
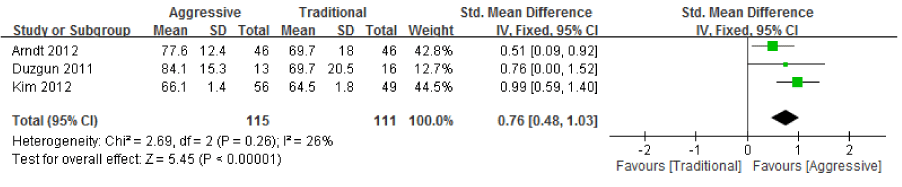
| Three articles included function as an outcome and compared the effects of an aggressive rehabilitation protocol to traditional protocol on shoulder function [1,8,19]. The time points of postoperative follow-up in all studies were different. Two articles used the constant shoulder score, but one used the Disability of the Arm, Shoulder, and Hand score (DASH). As a result, we investigated the general effect on shoulder function. Because higher DASH scores indicate more disability, we translated DASH scores by using full scores (100) minus patients’ received scores. After processing, the data could be combined with the constant shoulder score to represent overall shoulder function. Figure 4 shows individual study SMDs. Combining the results of these 3 studies using a fixed-effects model yielded the overall SMDs of 0.76 (95% CI: 0.48~1.03), indicating that the aggressive protocol led to greater improvement in shoulder function than did the traditional protocol (p<0.00001). |
| Anatomy structure |
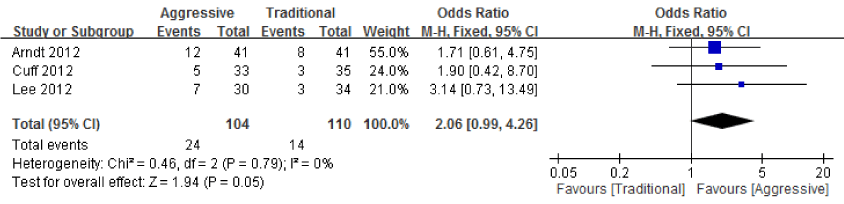
| Finally, we combined 3 articles to analyze the risk of aggressive protocols as compared to traditional protocols in terms of rotator cuff un-healing and re-tear rates by using the fixed-effects model [1,6,20,21]. The time points of post-operative follow-up in all studies were different. Figure 5 shows individual study SMDs. Combining the results of these 3 studies using a fixed-effects model yielded the overall odds ratio of 2.06 (95 % CI: 0.99~4.26), which indicated that aggressive protocols entailed greater risk of rotator cuff un-healing and higher re-tear rates than did traditional protocols. |
| Discussion |
| This meta-analysis included 6 RCTs that compared the effects of aggressive rehabilitation protocols and traditional protocols in patients after rotator cuff repair. The results showed that the aggressive rehabilitation protocol first, was superior to the traditional protocol in the outcomes of overall ROM at 6 months and 1 year after repair, and second, led to greater improvement in shoulder function. Previous studies have demonstrated that postoperative shoulder stiffness, the most frequent complication after arthroscopic rotator cuff repair, is correlated to increased pain, poor shoulder function, and worse quality of life [1]. Additionally, it is also correlated to adhesive capsulitis, pseudotenodesis of the deltoid, and complex regional pain syndrome, which leads to soft tissue contracture, tightness, and adhesion [20,22]. Early motion after operation can avoid immobilization-related stiffness. |
| Despite the several advantages of aggressive rehabilitation after surgery, it should be noted that an aggressive rehabilitation protocol may entail higher risks of rotator cuff un-healing and a higher retear rate than the traditional protocol. In this review, the differences between the two protocols were nearly significant. Several animal model studies have demonstrated that immobilization reduces tendon load-to-failure/stiffness and allows better tendon to bone healing. Over-activity may lead to inflammation and increase the production of scar tissue with lower biomechanical loads [13,18,23-30]. As a result, several studies indicated that avoiding early motion may have potential benefits in an effort to protect repaired tendons. |
| Only 2 of the 6 articles had an outcome of pain score, so metaanalysis could not be performed. Düzgün et al. showed significant pain reduction during activity at week 5 and week 16 compared to a standard protocol. Garofalo et al. also showed significant pain reduction at 2.5 months but no significant differences at 6 or 12 months after surgery. However, some of the non-included articles showed controversial results on pain reduction. Kim et al. and Lee et al. also demonstrated no difference in pain level between groups at 3, 6, and 12 months after surgery. Klintberg et al. showed that early active movement beginning in week 3 did not lead to inflammation and even could reduce pain [16]. According to the results of several studies; the effect of reducing pain within 3 to 4 months after surgery was demonstrated in an aggressive protocol. |
| Because rotator cuff un-healing and re-tearing need revision, which is functionally debilitating for the patients, multiple factors affecting post-operative rehabilitation protocols need to be controlled. These factors are listed in the following text [12]. The first factor is the surgical approach. Progression from an open procedure to a mini-open procedure and then to arthroscopic techniques leads to decreasing deltoid injury and minimizes post-operative pain. The second factor is the size of the tear, which varies from partial thickness to full thickness, and from small (<1 cm), medium (1~3 cm), and large (3~5 cm) to massive (>5 cm). Many researchers agree that the size of a tear is correlated to functional outcomes. Thus, the progression for rehabilitation should be slower in patients with larger tears [28,31]. The third factor is the fixation methods. The strength of fixation increases progressively from single-row to double-row and suture bridge technique [14,24]. In addition to the above 3 factors supported by the data of our review, other factors including (4) quality of tendon, muscular tissue, and bone, (5) mechanism of failure of the rotator cuff, such as traumatic or gradual tear, (6) immediate repair or delayed repair [2] and (7) different muscles and tendons; and number of tears should also be taken into consideration to determine the progression of rehabilitation. Furthermore, the characteristics of the patients, including age, level of activity, lifestyle habits, general health, and history of systemic disease such as diabetes mellitus, should also be carefully considered in designing a rehabilitation protocol [4,32]. |
| Several limitations to our analysis should be noted. First, because so few articles with variable outcome measures and time points of follow-up, only 4 articles at most could be combined to analyze each outcome. Second, the data of some studies did not fit normal distributions and could not be calculated by the software. Third, in terms of methodology, all articles were only of fair quality. This may threaten the validity of our analysis. |
| To our knowledge, this is the first article to examine the effect of an aggressive post-operative rehabilitation protocol versus a traditional rehabilitation protocol. The concept of aggressive rehabilitation includes early motion and increased dosage in passive or active motion. An aggressive rehabilitation protocol has both advantages and disadvantages. In recommending such treatment, several factors should be carefully considered. Generally, with a physician’s approval, aggressive rehabilitation can result in early recovery of shoulder ROM and function. The passive ROM exercise can be started 1 day after surgery, and active ROM exercise may follow several days later. A traditional or conservative protocol, however, is more appropriate for patients with specific characteristics such having large to massive tears, receiving invasive surgical techniques such as open repair, using less stable fixation methods such as single-row repair, having surrounding soft tissues of poor quality, being older and having a sedentary life style, and other systemic diseases. For these patients, passive ROM exercise can begin 4 weeks after surgery, and active ROM exercise can be added 6 to 8 weeks after surgery. High quality RCT trials are still needed for intervention protocols, long-term follow-up, and standard outcome measurements. |
| Conclusion |
| This meta-analysis found that the aggressive postoperative rehabilitation protocol leads to greater improvement in ROM and shoulder function than does the traditional protocol, but also that it entails higher risk of unhealing or re-tearing of the rotator cuff tendon. Any post-operative program for patients with rotator cuff repair must be designed with careful consideration of the several factors that influence the rehabilitation protocol. |
References |
|
Tables and Figures at a glance
| Table 1 | Table 2 |
Figures at a glance
 |
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 | Figure 5 |
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 18466
- [From(publication date):
July-2013 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 13584
- PDF downloads : 4882
