Case Report Open Access
Computerized Behavioral Activation Treatment for Maternal Depression Delivered in an Obstetric Clinic: A Case Study
| Julia Huston*, Jennifer Kuhn, Chelsea Sage-Germain and Amy Damashek | |
| Department of Psychology, Western Michigan University, Kalamazoo, MI 49008, USA | |
| Corresponding Author : | Julia Huston Department of Psychology Western Michigan University Kalamazoo, MI 49008, USA Tel: 740-603-2328 E-mail: julia.c.konkler@wmich.edu |
| Received: January 07, 2016; Accepted: February 02, 2016; Published: February 06, 2016 | |
| Citation: Huston J, Kuhn J, Sage-Germain C, Damashek A (2016) Computerized Behavioral Activation Treatment for Maternal Depression Delivered in an Obstetric Clinic: A Case Study. J Preg Child Health 2:216. doi:10.4172/2376-127X.1000216 | |
| Copyright: © 2016 Huston J, et al., This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Pregnancy and Child Health
Abstract
Purpose Depression affects a significant number of pregnant and postpartum mothers, especially low-income women. The presence of depressive symptoms during and immediately after pregnancy has been found to negatively affect both mothers and their children. Effective and accessible psychosocial treatment alternatives to antidepressant medications are needed to accommodate patient preferences and avoid potential risks to infant development. However, low-income depressed mothers face many barriers to accessing care. Computer-based treatment delivered in obstetric clinics may bypass some of these barriers and allow depressed pregnant and postpartum mothers greater access to effective treatment. Methods Presented is the clinical case of a low-income 22-year-old pregnant woman experiencing depressive symptoms. The patient successfully completed a 10-session computerized behavioral activation treatment program that was delivered in her obstetric clinic. Results Clinical outcomes revealed a decrease in depressive symptoms and an increase in quality of life. These gains were present at the end of treatment and were maintained at the three-month follow-up. Additionally, the patient responded positively to the treatment program and reported a high level of satisfaction. Conclusion These results suggest that computerized treatments delivered in familiar medical settings could accommodate patient preferences, remove some barriers to care, and allow for a streamlined referral process from physicians to mental health care providers, thus improving the accessibility of treatment for low-income mothers suffering from depression.
| Keywords |
| Maternal depression; Behavioural activation; Computerized treatment |
| Introduction |
| Depression is one of the most prevalent and disabling mental health disorders in the United States, and most people who suffer from depression receive inadequate care or no treatment at all [1]. Women of childbearing age are at high risk for depression; estimates indicate that 10-15% of women suffer from Major Depressive Disorder during and immediately after pregnancy, and an even greater number of women suffer from sub-clinical symptomatology [2-4]. For some women, the experience of perinatal depression leads to a chronic and recurring course of depression [5]. Minority mothers and young mothers of low socioeconomic status are particularly at risk for experiencing prenatal and postpartum depression [6]. |
| The prenatal and postpartum periods are critical developmental periods for both mother and child, and depression can cause significant interference. Some mothers may have impairment in their ability to participate in appropriate prenatal or infant care and may experience thoughts of hurting their babies or engage in negative parenting behaviors [7]. Maternal depression can also negatively affect children by increasing the likelihood of health complications including preterm birth, neonatal mortality, and later cognitive deficits and psychopathology [8-16]. |
| Due to the serious nature of the possible negative effects of depression for both mothers and their children, effective and accessible treatment for pregnant and postpartum women experiencing depression is essential. Effective evidence-based pharmacological and non-pharmacological treatments exist [17,18]; however, the majority of pregnant women suffering from major depression are receiving no treatment at all [2,3,5,19]. |
| Psychotropic medication is one treatment option, and is currently the most commonly used intervention for depression in primary care settings [18]. Antidepressant medications have been associated with negative health outcomes for the developing foetus (e.g., spontaneous abortion, fetal growth changes, preterm birth, and neurobehavioral changes), although studies are often unable to disentangle the effects of antidepressant medications from the effects of other medications or the effects of depression itself [20,21]. Additionally, research has revealed concerns among mothers about the stigma and potential side effects of long-term psychotropic medication use [5,19]. Thus, many women may choose to avoid or discontinue previously used antidepressant medications during pregnancy and while breastfeeding which may place them at increased risk for experiencing a relapse in their depression symptoms [3,14,22]. Thus, alternative options to psychotropic medications are needed. |
| Psychosocial interventions may be a preferable treatment alternative for many women who are pregnant or breastfeeding [5,19]. Despite the fact that several efficacious psychosocial treatments for depression exist [17], research has shown that the majority of pregnant and postpartum women, especially low income women, do not receive services because they do not follow up on referrals to outpatient mental health care [3,23,24]. |
| Many women indicate a preference for receiving treatment for depression during pregnancy or the postpartum period at their obstetric (OB) clinic [5]. It is not uncommon for mental health issues like depression to be treated in a medical setting; currently more than half of all cases of depression are diagnosed and treated in primary care practices [1,18]. Research has shown that when treatment is delivered in primary care or home settings, patients are more likely to adhere to treatment and to show improved outcomes [25,26]. It is possible that these findings may also extend to care delivered in obstetric clinics. |
| However, even when psychosocial treatment is delivered in a primary care setting, there are still numerous barriers to treating lowincome women including both attitudinal (e.g., inadequate knowledge, negative views of therapy, lack of support, fear of being stigmatized or perceived negatively, reluctance to disclose personal information) and logistical barriers (e.g., lack of transportation, financial resources, child care, time) [5,19,27]. Additionally, there are barriers to providing effective, evidence-based treatment for depression in primary care settings, including time and cost constraints as well as a deficit in trained professionals [18]. |
| Advances have been made with regard to developing accessible psychosocial interventions for depressed populations, especially in the form of computer-based interventions. There is preliminary evidence for the effectiveness of cognitive behavioral therapies delivered in nonconventional ways, including phone or computer-based interventions, in reducing depression symptoms and increasing patient satisfaction [18]. A growing body of literature continues to demonstrate the clinical effectiveness and feasibility of computer and web-based interventions for depression across populations diverse in terms of ages, depression level, and comorbid health problems [28]. Moreover, web and computer-based cognitive behavioral therapies are recommended by the practice guidelines issued by the joint taskforce of the American College of Obstetrics and American Psychiatric Association for the treatment of depression during pregnancy in cases in which there are barriers to accessing other treatment services (e.g., few behavioral therapists in a patient's area, patient has monetary limitations) [21]. |
| Computerized interventions for depression may take many forms and include a variety of different treatment techniques. Behavioral activation may be particularly well-suited for computerized treatment because of its relatively simple implementation and overall effectiveness [29]. Additionally, behavioral activation may be particularly appropriate for broad dissemination due to evidence supporting it as a parsimonious evidence-based treatment for depression [30]. There is evidence that brief behavioral activation treatment for depression delivered in primary care settings produces high client satisfaction ratings and large effect sizes on measures of depression and quality of life [18]. |
| Behavioral activation is based on the behavioral model of depression; the goals are to reduce avoidance behaviors (e.g., excessive sleeping) and increase engagement in reinforcing behaviors that are consistent with one’s individual values (e.g., spending time with family) [26,29-31]. Recent research has revealed the effectiveness of an online behavioral activation treatment accompanied by phone support that includes modules specifically adapted to the concerns of postpartum women. This treatment produced clinically significant improvement in depression scores for over 60% of participants [4]. However, the study did not examine the effects of the intervention with pregnant women. Thus, research is needed to examine the effectiveness of computerbased behavioral activation for pregnant women. |
| Building a Meaningful Life Through Behavioral Activation (BAML) is a computer-based, interactive treatment based on behavioral activation therapy. BAML has been shown to be effective in significantly reducing depression and improving quality of life in a sample of 15 adults from the general population in an initial open trial [29]. However, the intervention has not been tested specifically with pregnant or postpartum women. The following case study presents clinical outcomes from a pregnant woman who completed the BAML program delivered in an obstetric clinic. The case was selected from an ongoing research study on the efficacy of BAML with pregnant and postpartum women. In the larger research study, there have been approximately 60 women referred for depression treatment, 20 of whom indicated a desire to participate in the BAML treatment program. Of those who attended an initial assessment session, five women did not meet eligibility criteria and 11 women were found eligible to participate in the study. Eight of the eligible participants attended one or more BAML treatment sessions. To date, the participant discussed in the current paper is the only participant who completed the entire BAML treatment program. This case study provides a strong rationale for continuing to address barriers to care in order to increase access to the BAML treatment program, given the promising results that were obtained with the participant discussed in the current case study. This research study was approved by both hospital and university based Human Subjects Institutional Review Boards and was performed in accordance with relevant ethical standards. |
| Materials and Methods |
| Participant |
| The client treated in this report, Jenny (name changed to maintain confidentiality), was recruited as part of a research study, as described above, and chose the BAML program from among several alternative community treatment options for depression. Her history and presenting complaints include only information that was collected as part of the study’s assessment protocol, therefore we have only limited information about her history. |
| When she began participating in the current study, Jenny was a 22- year-old Caucasian female who was two months pregnant with her first child. Jenny’s pregnancy was not an intentional pregnancy. She had never been married and did not currently have a live-in partner or spouse. However, she did have a boyfriend, who was the father of her child. She was in the process of completing a trade school education and preparing to graduate. She was also employed part-time in the food service industry and worked about 20 hours each week. Jenny lived with her mother and reported an annual gross household income between $10,000 and $14,999. She was in good health, and had limited social support from her mother and boyfriend. |
| Jenny learned about her option to participate in BAML through the social worker at her hospital-based obstetric clinic. The obstetric clinic uses the Edinburgh Postnatal Depression Scale (EPDS) [32,33] to screen pregnant and post-partum women for symptoms of depression. Women scoring higher than 12 may meet criteria for depression and are therefore referred to the social worker to discuss community treatment referral options. After scoring a 14 on the EPDS, Jenny was given a list of community treatment resources for depression, including information about the current research study utilizing BAML. She indicated that she was interested in learning more about the study and was then contacted by a graduate research assistant (GRA). After obtaining additional information from the GRA, Jenny indicated that she was interested in participating and agreed to attend an initial screening session to see if she qualified. |
| During the initial assessment, Jenny reported experiencing many symptoms of depression. She reported both difficulty sleeping and excessive sleeping, sluggishness and reduced energy, decreased appetite (slight weight loss), difficulty making routine decisions and getting things done (especially at work), little desire to get out of bed or engage in any activity, depressed mood, and feelings of guilt. She also endorsed some suicidal ideation. A complete suicide assessment was conducted, and Jenny was not found to be at risk for hurting herself. Her current major depressive episode began shortly after she found out that she was pregnant and worsened with the onset of winter weather. |
| Jenny first began experiencing symptoms of depression when she was in junior high school. Over the years her depressive symptoms came and went, but she reported that they always worsened during the winter months. Jenny also had a history of substance abuse. She drank heavily as a teenager and was involved in the legal system for engaging in underage drinking. As a result, she underwent substance abuse treatment and attended Alcoholics Anonymous meetings. Jenny stopped binge drinking about three years before her contact with the present treatment regimen, but continued to engage in light drinking until she learned that she was pregnant. Additionally, Jenny engaged in occasional recreational marijuana use prior to becoming pregnant. |
| Initial assessment session |
| Jenny participated in an initial assessment session to determine if she was eligible to participate in the computerized treatment program. At this initial assessment session Jenny completed the informed consent document, a demographic questionnaire, the Patient Health Questionnaire-9 (PHQ-9) [34], the Quality of Life Scale (QoLS) [35], and the Structured Clinical Interview for DSM-IV (SCID-I) [36]. |
| Demographic questionnaire |
| The demographic questionnaire was used to gather basic information about Jenny. The 13-item measure included questions about Jenny’s age, ethnicity, education level, marital status, employment status, socioeconomic status, and the number of children in her home. |
| PHQ-9 |
| The PHQ-9 is a 9-item questionnaire designed to measure depression levels in medical settings. It takes less than 5 minutes to complete and has been found to have diagnostic validity and utility [34]. Jenny received a score of 20 on her initial PHQ-9, indicating severe depression. Additionally, she indicated that her depression symptoms were making it very difficult to function in her daily life. |
| QoLS |
| The QoLS is a 16-item measure, with higher scores indicating higher quality of life. Research has shown adequate reliability and validity for this measure [37]. Jenny’s score on the QoLS was 42 out of a possible 112 points. |
| SCID-I |
| The clinical version of the SCID-I was administered as a semistructured interview to determine if Jenny met the inclusion criterion for participating in the study, which was a current diagnosis of Major Depressive Disorder or Dysthymic Disorder. The SCID-I was also used to determine whether Jenny met any of the exclusion criteria. The complete modules were administered for Mood Episodes, Psychotic and Associated Symptoms, and Alcohol and Other Substance Use Disorders. The SCID-I revealed that Jenny met criteria for Major Depressive Disorder, recurrent, moderate. She did not meet criteria for current psychosis, Bipolar Disorder, or current substance abuse or dependence (exclusion criteria). Jenny met criteria for past alcohol abuse but this did not exclude her from participating in the study. The SCID-I has been shown to be a reliable diagnostic tool for major DSM IV disorders [36]. |
| Case Conceptualization |
| Jenny’s depressive symptoms caused significant functional impairment in many domains of her life resulting in impaired social, academic, and employment functioning. Additionally, Jenny’s depressive symptoms may have put her infant at risk of experiencing a variety of health complications, as well as later cognitive, emotional, and behavior problems [8-16]. Her symptoms also made it more likely that she would have difficulty engaging in positive parenting behaviors such as engagement, social communication, and enthusiasm [7]. |
| Jenny faced several life challenges that might have made it difficult for her to access services in a traditional mental health setting, such as a lack of financial resources, limited social support and inconsistent access to transportation. She was able to schedule many of her computerized treatment sessions to coincide with her regularly scheduled medical appointments at her obstetric clinic, which made services more accessible. It is also possible that because treatment was offered free-of-charge, it was made more accessible. While this is unlikely to be replicated in a real-world setting, we believe that computerized treatments could be delivered at a much lower cost than traditional therapy sessions which require the one-on-one attention of a highly trained mental health professional for extended periods of time. Some monitoring is necessary with the BAML program, particularly in case of suicidality or technical issues. However, while many OB clinics might be able to support computer-delivered care using the staff already in place, to provide similar face-to-face therapy sessions would likely require major changes. For example, although a social worker was available at Jenny’s OB Clinic, her role was not to provide face-to-face therapy, but rather to connect patients with external community supports. Additionally, there was only one social worker available to coordinate care for the entire patient population. Computerized treatments also have the potential to be streamed directly to patients in their homes or in local libraries or computer labs, which could further reduce cost and transportation barriers for some individuals. |
| BAML, the computerized treatment program that was administered in the current study, is based on a behavioral model of depression. Lewinsohn’s behavioral model describes depression as the result of an individual’s loss of contact with stable sources of positive reinforcement in his/her environment, which results in a loss of meaning in life [38]. Positive reinforcement occurs when the introduction of a stimulus following a behavior increases the likelihood of the behavior occurring again in the future. Negative reinforcement, on the other hand, occurs when the removal of a stimulus following a behavior increases the likelihood of the behavior occurring again in the future [39]. Environments low in positive reinforcement and high in negative reinforcement can elicit avoidance behavior, which can contribute to the maintenance of depression [40]. From this functional perspective, depression is a natural response to life stressors and difficult environments [39]. |
| The behavioral model can be used to explain the emergence and maintenance of Jenny’s depressive symptoms. Jenny had recently discovered that she was pregnant, which resulted in many physical and psychological changes in her life. Jenny was working part time and going to school, so most of her time and energy was devoted to those activities. Jenny began experiencing fatigue, achiness, and nausea as a result of her pregnancy, making it difficult for her to get things done and engage in the few enjoyable activities for which she had previously had time and energy (e.g., exercise, spending time with friends, spending time outside). The winter weather worsened her mood and made transportation even more of a barrier for her. Jenny did not have many friends or other supportive individuals in her life, and as a result of her pregnancy she reported greater isolation and tension within the few close relationships that she did have. In combination, these factors resulted in a loss of contact with stable sources of positive reinforcement in several areas of Jenny’s life, and she began experiencing symptoms of depression. Jenny began feeling sad and guilty. She had trouble getting out of bed, making decisions, and completing daily tasks and activities. She also had difficulty sleeping and eating normally. These depressive symptoms made it more difficult for Jenny to obtain reinforcement, and so her depression continued to worsen. |
| The behavioral model of depression has clear treatment implications. If loss of contact with sources of positive reinforcement is the cause of depression, then treatment should focus on establishing contact with old and new sources of positive reinforcement and building the skills needed to maintain contact with these sources of reinforcement [38]. Behavioral activation therapy is an evidence-based treatment for depression that seeks to re-establish meaning in an individual’s life by reinstating contact with diverse and stable sources of positive reinforcement [39]. The BAML treatment program attempts to reactivate patients and get them reengaged in their environments so that they are able to come into contact with old and new sources of positive reinforcement. BAML assists clients in identifying their values and facilitates engagement in meaningful and reinforcing activities that are values-consistent. Through renewed contact with varied and stable sources of positive reinforcement, it is hypothesized that life becomes more meaningful, and symptoms of depression decrease. |
| Intervention |
| The BAML program (version used in the present investigation) consists of 10 sessions delivered approximately once per week, each lasting approximately one hour. Sessions begin with a video introduction by a narrator, who guides users through homework review and self-report of mood. Participants input symptom ratings each time they access the program, and progress is reviewed throughout treatment. After users view the introduction and complete self-report measures, users access session content that is delivered via video recordings of licensed community therapists. During each BAML session, users are able to choose one of four potential therapists of varying age, gender, and race to guide them through the program content via videos. All session content is predetermined and identical between therapists, so choice of therapist does not influence receipt of treatment. Concepts are explained using videos of actors playing the roles of various patient examples, and through the use of voice-over narration, rich graphics, and text. Users interact with the program by answering multiple choice questions as they progress through the sessions. The narrator ends each session by summarizing key concepts and reminding users of their between session homework [29]. Homework includes practice with key concepts introduced in each session. Specifically, each week participants are asked to track their daily activities and moods. Additional homework activities include engaging in values clarification exercises and identifying and scheduling values-consistent activities. During each weekly session participants input information about their homework completion and depressive symptoms from the previous week directly into the BAML program and then receive individualized feedback tailored to their responses. The BAML program stores all participant data entered during treatment sessions. BAML requires very little (if any) support from a live provider. Some monitoring is required, particularly in the event of suicidality or technical issues. However, the necessary time commitment and involvement from a live provider is approximately five minutes per session and thus is much less than would be required for a regular outpatient therapy session. |
| The first five BAML sessions, considered to be the therapeutic dose of treatment, introduce the concepts of behavioral activation. Users are then instructed to practice these concepts in their everyday lives. Users learn to track their behavior, notice relationships between behavior and mood, clarify their values, and schedule activities that align with their identified values. The latter five sessions are made up of minilessons, the selection and delivery of which are tailored to each user based on the results of a questionnaire that assesses their individual needs. Lessons involve a range of topics, including how to get organized, how to look for a job, or how to appropriately deal with anger [29]. There are 16 such mini lessons in total and the program delivers two to three mini lessons in each of the five final sessions, in order of relevance to the user, based on their reported concerns. |
| Weekly and Post-Treatment Assessments |
| The PHQ-9 was administered at the beginning of each of the 10 BAML treatment sessions to monitor changes in depression levels throughout the course of treatment. During the final treatment session, Jenny also completed another QoLS and a modified Client Satisfaction Questionnaire [29,41-43] to assess her level of satisfaction with the BAML program. At the three-month follow-up, which was conducted as a phone interview, Jenny again completed the PHQ-9 and the QoLS. |
| Jenny completed the initial assessments, all 10 computerized treatment sessions, and the three-month follow-up assessment. The BAML treatment spanned the majority of Jenny’s pregnancy; she was two months pregnant when she attended her initial assessment session in January, she was five months pregnant when she completed the final BAML session in April, and she completed her three month follow-up phone session 10 days before her due date in July. A GRA conducted the initial and follow up assessments, and was present for all treatment sessions. For each treatment session, Jenny came to the obstetric clinic and completed a BAML treatment module in a private room on a laptop provided by the research study. During treatment sessions, the GRA gave Jenny the PHQ-9, and then remained present only to answer any questions that Jenny might have about the program, trouble shoot computer issues, or intervene in the case of suicidality. GRA interaction with Jenny during treatment sessions averaged only five minutes per session. |
| Results |
| Jenny was extremely reliable, motivated, and engaged throughout treatment. She regularly attended sessions and completed her homework assignments. Some of the values-based activities that Jenny reported engaging in over the course of treatment were riding her bike, spending time with friends (e.g., going to lunch with them) and attending a prenatal yoga class. |
| See Figure 1 for a depiction of changes in Jenny’s depression scores throughout treatment. At the initial assessment session, Jenny’s depression score on the PHQ-9 was a 20, indicating severe depression and significant functional impairment. At the final treatment session her depression score had dropped to a 9, indicating only mild depression and some functional impairment. The depressive symptoms that Jenny was still endorsing most strongly at the end of treatment (e.g., trouble sleeping, appetite concerns, lack of energy) were physiological in nature and could have also been related to her pregnancy. Jenny’s QoLS score at the initial assessment session was a 42 out of a possible 112 points and by the final treatment session her QoLS score had doubled to 84 out of a possible 112 points. |
| In addition to showing improvement in her level of depression and her quality of life at the end of treatment, Jenny reported being very satisfied with the treatment. On the 19-item satisfaction questionnaire, Jenny used a 1 (strongly agree) to 5 (strongly disagree) scale to rate a variety of statements about the BAML program (e.g., “As a result of completing BAML, I deal more effectively with daily problems”, “The computerized treatment for depression was easy to use”, “The computerized treatment for depression fit my individual needs”). Jenny’s average rating of the computerized treatment program was 1.32, indicating that overall she was very satisfied with the BAML program. Additionally, she gave all of the individual components of the treatment program (e.g., videos, therapists, work completed during sessions, homework, staff support, and written information) a rating of 5 on a 1 (useless) to 5 (useful) scale. In addition to providing the above quantitative feedback, Jenny also provided qualitative feedback about her satisfaction with the treatment provided. Jenny reported that she “found many perks to treatment through computerized methods.” She also reported that she found the homework and the interactive questions asked throughout the treatment sessions helpful. Additionally, Jenny commented: “the people that I met and the people on the computer program helped me to feel like I am not wrong for feeling how I feel, that it is okay. And I cherish that. I hope this program can reach many more people feeling how I did.” |
| Three months after the final treatment session, Jenny completed the follow-up assessments via phone interview. At this time, Jenny’s PHQ-9 depression score was an 8, indicating mild depression and some functional impairment. Again, the symptoms endorsed most strongly were physiological in nature (e.g., trouble sleeping, lack of energy) and could have been related to the fact that she was eight months pregnant. Additionally, her QoLS score was a 78 out of a possible 112 points. Neither of these scores differed greatly from those reported during the final treatment session, and both scores show a great deal of improvement from Jenny’s PHQ-9 and QoLS scores during the initial assessment session (see Figure 1 for PHQ-9 scores). |
| Discussion |
| Access and barriers to care |
| Jenny did not always have access to transportation for her treatment sessions. Fortunately, she lived close enough to the obstetric clinic where treatment sessions were conducted to walk or ride her bike if needed. She was also often able to schedule her treatment sessions around her other pregnancy-related visits, which reduced transportation and time barriers. The treatment provided to Jenny was free, so there were no monetary barriers to her receiving treatment. Additionally, Jenny did not have any other children, so a lack of childcare was not a barrier to her receiving treatment. |
| Treatment implications of the case |
| The present case provides preliminary evidence that delivering a computerized treatment program in an obstetric setting may be efficacious for pregnant women experiencing symptoms of depression. A growing body of evidence supports the use of computerized treatments for depressive symptoms [28,29], but the efficacy of computerized treatment has not yet been well-established for specific sub populations, including depressed pregnant and postpartum mothers. |
| Jenny responded positively to the treatment program and reported a high level of satisfaction with BAML. Clinical outcomes revealed a decrease in depressive symptoms and an increase in quality of life. These gains were present at the end of treatment and were maintained at the three-month follow-up. Additionally, Jenny attended sessions regularly and completed her homework. These results suggest that delivering computerized treatment in an obstetric setting may be an effective way to bypass some of the barriers that many low-income depressed mothers face in trying to access effective care. The use of BAML in an obstetric creates the potential for a “warm hand-off” between medical and mental health providers, thus easing the transition for clients and offering an alternative to the standard referral process. Additionally, the potential to group obstetric and mental health appointments together creates the possibility of further reducing transportation and time burdens. |
| Though Jenny did face some barriers to accessing care, there are several other common barriers that Jenny did not face. She did not have any other children, so childcare was not a barrier for her. She also did not suffer from any co-morbid mental health disorders, though she did have a history of alcohol abuse. It is unknown how well Jenny would have adhered to treatment, and how much clinical improvement in depression symptoms and quality of life she would have experienced, had any other common stressors been present in her life at the time of her participation in the current research project. In fact, many of these barriers have gotten in the way of other potential participants initiating and/or completing the BAML treatment program as delivered in the current study. Therefore, there is need for additional research investigating additional possibilities for overcoming remaining barriers so that evidence-based treatments can continue to be made more accessible to low income pregnant women. |
| Physicians are often the first professionals to come into contact with the mental health concerns of their patients, with half of all cases of depression being seen first in primary care practices [1]. Within the traditional model, physicians provide patients with referrals to outpatient mental health providers. However, there are many barriers and limitations to the traditional referral model, including stigma, delayed access to services, and the lack of follow-up by many patients [3,5,19,23,27]. Additionally, many women experiencing depression during and after pregnancy prefer to receive treatment in their obstetric clinic rather than in an outpatient therapy setting [5]. |
| Computerized treatments delivered in familiar medical settings create the possibility of accommodating patient preferences, removing some barriers to care, and allowing for a streamlined referral process from physicians to mental health care providers, thus improving the accessibility of treatment. The ease of use, cost-effectiveness, and transportability of computerized treatments allows for the possibility of easy implementation in primary care or obstetric settings. The staff demands for computerized treatment are minimal and much less costly than one on one therapy with specialized mental health providers. Personnel requirements for the delivery of computerized treatment could be fulfilled by existing medical or mental health staff and would not necessarily require additional specialized staff members. Ideally, computerized treatment sessions could be scheduled around existing medical visits thus allowing patients to avoid having to make separate trips for medical and mental health appointments. Computerized treatments also have the potential to be streamed directly into patients’ homes or to public libraries or other public computer lab facilities, further expanding the accessibility of treatment. Attitudinal barriers may also be overcome by implementing treatment in this way. Women who may be reluctant to disclose personal information to a treatment provider may feel more secure working with a computer. There is less risk of stigmatization; women may fear going to a mental health clinic and being recognized, but being recognized in a medical center may be less scary, and would not necessarily lead others to the conclusion that the patient suffers from mental health issues. Programs like BAML may therefore offer a much needed extension of evidence-based behavioral treatment for depression. The existing evidence for the effectiveness and acceptability of computer based treatments supports the notion that they allow patients to overcome some barriers to treatment. |
| Recommendations for future research |
| More research investigating the efficacy of computerized treatments generally and for specific populations, including depressed pregnant and postpartum women, is greatly needed. Additionally, more research is needed to identify and address the many remaining barriers that low income and minority pregnant and postpartum women face in accessing affordable and efficacious treatment for depressive symptoms. The data presented in this case study provides preliminary evidence to suggest that a computerized treatment program for depression delivered in an obstetric setting may be effective in reducing depressive symptoms and increasing quality of life for pregnant women. It also provides preliminary evidence of high consumer satisfaction with computerized treatment. The delivery of computerized treatment in obstetric and primary care settings has the potential to reduce some of the barriers to care that are commonly faced by low income pregnant women, and should be investigated further. However, additional accommodations may need to be made to bypass many of the other barriers to care that are commonly faced by low-income populations. Among these might be use of a web-based version that does not require office visits, thus relieving some of the transportation, childcare, and scheduling pressures encountered by many low-income patients. Additionally, options for more long term follow-up care following computerized treatment programs, both within primary care and OB clinics and externally in the community, should be investigated. |
References
- Wang PS, Lane M, Olfson M, Pincus HA, Wells KB (2005) Twelve month use of mental health services in the united states: Results from the national comorbidity survey replication. Archives of General Psychiatry 62: 629-640.
- Gavin NI, Gaynes BN, Lohr KN, Meltzer-Brody S, Gartlehner G, et al. (2005) Perinatal depression: a systematic review of prevalence and incidence.Obstet Gynecol 106: 1071-1083.
- Muzik M, Marcus SM, Flynn HA (2009) Psychotherapeutic treatment options for perinatal depression: Emphasis on maternal-infant dyadic outcomes. Journal of Clinical Psychiatry 70: 1318-1319.
- Mahen HA, Richards DA, Woodford J, Wilkinson E, McGinley J, et al. (2014) Netmums: A phase II randomized controlled trial of a guided internet behavioural activation treatment for postpartum depression. Psychological Medicine 44: 1675-1689.
- Goodman JH (2009) Women's attitudes, preferences, and perceived barriers to treatment for perinatal depression.Birth 36: 60-69.
- Rich-Edwards JW, Kleinman K, AbramsA, Harlow BL, McLaughlin TJ, et al (2006) Sociodemographic predictors of antenatal and postpartum depressive symptoms among women in a medical group practice. Journal of Epidemiology and Community Health 60: 221-227.
- Lovejoy MC, Graczyk PA, O'Hare E, Neuman G (2000) Maternal depression and parenting behavior: a meta-analytic review.Clin Psychol Rev 20: 561-592.
- Dayan J, Creveuil C, Marks MN, Conroy S, Herlicoviez M, et al. (2006) Prenatal depression, prenatal anxiety, and spontaneous preterm birth: a prospective cohort study among women with early and regular care.Psychosom Med 68: 938-946.
- Diego MA, Field T, Hernandez-Reif M (2005) Prepartum, postpartum and chronic depression effects on neonatal behavior. Infant Behavioral Development 28: 155- 164.
- Diego MA, Field T, Hernandez-Reif M, Cullen C, Schanberg S, et al. (2004) Prepartum, postpartum, and chronic depression effects on newborns.Psychiatry 67: 63-80.
- Field T, Diego M, Dieter J, Hernandez-Reif M, Schanberg S, et al. (2004) Prenatal depression effects on the fetus and the newborn. Infant Behavioral Development 27: 216- 229.
- Field T, Diego M, Hernandez-Reif M, Figueiredo B, Schanberg S, et al. (2008) Chronic prenatal depression and neonatal outcome.Int J Neurosci 118: 95-103.
- Hay DF, Pawlby S, Sharp D, Asten P, Mills A, et al. (2001) Intellectual problems shown by 11-year-old children whose mothers had postnatal depression.J Child Psychol Psychiatry 42: 871-889.
- Nulman I, Koren G, Rovet J, Barrera M, Pulver A, et al. (2012) Neurodevelopment of children following prenatal exposure to venlafaxine, selective serotonin reuptake inhibitors, or untreated maternal depression.Am J Psychiatry 169: 1165-1174.
- Pawlby S, Sharp D, Hay D, O'Keane V (2008) Postnatal depression and child outcome at 11 years: the importance of accurate diagnosis.J Affect Disord 107: 241-245.
- Rahman A, Iqbal Z, Bunn J, Lovel H, Harrington R (2004) Impact of maternal depression on infant nutritional status and illness: a cohort study.Arch Gen Psychiatry 61: 946-952.
- Hollon SD, Ponniah K (2010) A review of empirically supported psychological therapies for mood disorders in adults.Depress Anxiety 27: 891-932.
- Wolf NJ, Hopko DR (2008) Psychosocial and pharmacological interventions for depressed adults in primary care: a critical review.ClinPsychol Rev 28: 131-161.
- Dennis C, Chung-Lee L (2006) Postpartum depression help-seeking barriers and maternal treatment preferences: A qualitative systematic review. Birth: Issues in Perinatal Care 33: 323-331.
- Flynn HA, Blow FC, Marcus SM (2006) Rates and predictors of depression treatment among pregnant women in hospital-affiliated obstetrics practices. General Hospital Psychiatry 28: 289-295.
- Yonkers KA, Wisner KL, Stewart DE, Oberlander TF, Dell DL, et al. (2009) The management of depression during pregnancy: A report from the American Psychiatric Association and the American College of Obstetricians and Gynecologists. General Hospital Psychiatry 31: 403-413.
- Cohen LS, Altshuler LL, Harlow BL, Nonacs R, Newport DJ, e al. (2006) Relapse of major depression during pregnancy in women who maintain or discontinue antidepressant treatment. JAMA: Journal of the American Medical Association 295: 499-507.
- Smith MV, Shao L, Howell H, Wang H, Poschman K, et al. (2009) Success of mental health referral among pregnant and postpartum women with psychiatric distress.Gen Hosp Psychiatry 31: 155-162.
- The Urban Institute, Depression in low-income mothers of young children: Are they getting the treatment they need, Washington, DC: McDaniel, Lowenstein C.
- Segre LS, Brock RL, O’Hara MW (2014) Depression treatment for impoverished mothers by point-of-care providers: A randomized controlled trial. Journal of Consulting and Clinical Psychology
- Yawn BP, Dietrich AJ, Wollan P, Bertram S, Graham D, et al. (2012) TRIPPD: A practice-based network effectiveness study of postpartum depression screening and management. Annals of Family Medicine 10:320-329.
- Leis JA, Mendelson T, Perry DF, Tandon SD (2011) Perceptions of mental health services among low-income, perinatal African-American women.Womens Health Issues 21: 314-319.
- Richards D, Richardson T (2012) Computer-based psychological treatments for depression: a systematic review and meta-analysis.Clin Psychol Rev 32: 329-342.
- Spates CR, Kalata AH, Ozeki S, Stanton CE, Peters S (2013) Initial open trial of a computerized behavioral activation treatment for depression.Behav Modif 37: 259-297.
- Dimidjian S, Barrera M Jr, Martell C, Muñoz RF, Lewinsohn PM (2011) The origins and current status of behavioral activation treatments for depression.Annu Rev Clin Psychol 7: 1-38.
- Mazzucchelli T, Kane R, Rees C (2009) Behavioral activation treatments for depression in adults: A meta-analysis and review. Clinical Psychology: Science and Practice 16: 383-411.
- Cox JL, Holden JM, Sagovsky R (1987) Detection of postnatal depression. Development of the 10-item Edinburgh Postnatal Depression Scale.Br J Psychiatry 150: 782-786.
- Murray D, Cox JL (1990) Screening for depression during pregnancy with the Edinburgh Depression Scale (EPDS). Journal of Reproductive and Infant Psychology 8: 99-107.
- Spitzer RL, Kroenke K, Williams JB (1999) Validation and utility of a self-report version of PRIME-MD: the PHQ primary care study. Primary Care Evaluation of Mental Disorders. Patient Health Questionnaire. JAMA 282: 1737-1744.
- Flanagan JC (1978) A research approach to improving our quality of life. American Psychologist 3: 138-147.
- First MB, Gibbon M, Spitzer RL, Williams JB (1996) User’s guide for the Structured Clinical Interview for DSM-IV Axis I Disorders. Washington, DC: American Psychiatric Press.
- Burckhardt CS, Anderson KL (2003) The Quality of Life Scale (QOLS): reliability, validity, and utilization.Health Qual Life Outcomes 1: 60.
- Hopko DR, Mullane CM (2008) Exploring the relation of depression and overt behavior with daily diaries.Behav Res Ther 46: 1085-1089.
- Kanter JW, Busch AM, Rusch LC (2009) Behavioral activation: The CBT distinctive features series, New York: Routledge.
- Ferster CB (1973) A functional anlysis of depression. Am Psychol 28: 857-870.
- Fischer J Corcoran K (2007) Measures for clinical practice and research, New York, Oxford University Press.
- Larsen DL, Attkisson CC, Hargreaves WA, Nguyen TD (1979) Assessment of client/patient satisfaction: development of a general scale. Eval Program Plann 2: 197-207.
- McMurty S, Hudson W (2007) Client Satisfaction Inventory, Measures for clinical practice and research, New York, NY: Oxford University Press.
Figures at a glance
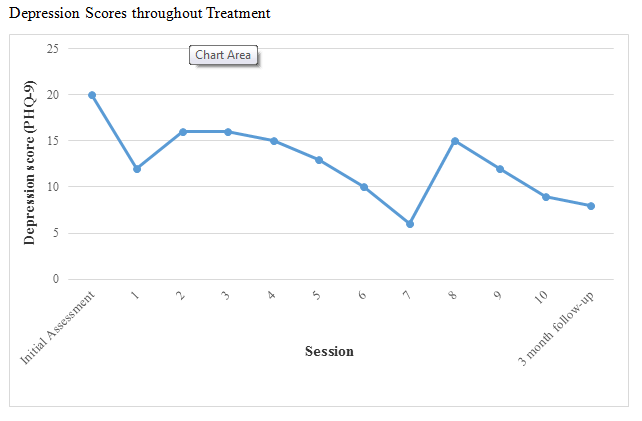 |
| Figure 1 |
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 11649
- [From(publication date):
February-2016 - Aug 17, 2025] - Breakdown by view type
- HTML page views : 10672
- PDF downloads : 977
