Research Article Open Access
Current Attitudes and Practices among Pregnant Women toward Influenza Immunization
| Sharon Puchalski*, Cheryl Hollema and Brenda Marshall | |
| William Paterson University of New Jersey, Wayne, NJ, United States | |
| Corresponding Author : | Sharon Puchalski William Paterson University of New Jersey, Wayne, NJ, United States Tel: 1-201-602-0290 E-mail: puchalskis1@wpunj.edu; sjprnc@aol.com |
| Received: July 01, 2014; Accepted: July 22, 2015; Published: July 27, 2015 | |
| Citation: Puchalski S, Hollema C, Marshall B (2015) Current Attitudes and Practices among Pregnant Women toward Influenza Immunization. J Preg Child Health 2:184. doi:10.4172/2376-127X.1000184 | |
| Copyright: © 2015 Puchalski S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Pregnancy and Child Health
Abstract
Pregnant women are more vulnerable to severe illness and complications due to influenza infection. The Advisory Committee on Immunization Practices and the American College of Obstetrician and Gynecologists recommend that all women who are pregnant during influenza season receive the inactivated influenza vaccine, regardless of trimester. The Centers for Disease Control (2015) reported that only 52.2% of women pregnant during influenza season stated that they had received the influenza immunization. Prenatal visits represent an ideal time for the APN to discuss immunization history and recommend and educate about the importance of influenza immunization during pregnancy and to help reach the Healthy People 2020 goal of 80% of pregnant women to receive the influenza vaccine. The purpose of this study was to explore pregnant women’s knowledge, attitudes, and behaviors toward influenza immunization and examine vaccination coverage in this population. The purposive, convenience sample was comprised of 60 pregnant women who were recruited from a private obstetrician and gynecologist practice. Fifty-seven percent of pregnant women did not receive the influenza immunization. Maternal age, race/ethnicity, education, and health insurance are independent from the women’s decision to receive the influenza vaccination. Women who believed in the efficacy (x2 (1) = 16.587, p < 0.05) and safety (x2(1) = 12.219, p < 0.05) of the vaccination were more likely to get vaccinated then those who didn’t. Influenza vaccination rates in pregnant women remain low. Understanding pregnant women’s knowledge, attitudes, and practices related to influenza immunization can help to improve vaccination coverage rates among pregnant women.
| Keywords |
| Pregnancy; Influenza; Immunization |
| Introduction |
| Pregnant women are more vulnerable to severe cases of influenza than the general population, however the Center for Disease Control and Prevention (CDC) reported that only 11% of women received the influenza vaccine during the 2008-09 influenza season [1-3]. Estimates provided from the CDC document an overall range of flu-associated deaths from 3,000 – 49,000 [4] (CDC, 2015). Influenza immunization can reduce morbidity and mortality among pregnant women and also reduces risk to neonates [5-7]. Among adult populations, pregnant women have the lowest coverage rates [8]. Maternal prenatal vaccination data falls below the Healthy People 2020 goal of 80% influenza vaccination coverage for pregnant women. Despite the ACIP (2011) and ACOG (2014) guidelines, only 44% of women surveyed in 2010-2011 flu season, 46.4% in 2011-2012, 50.5% in 2012-2013 season, and 52.2% in the 2013-2014 influenza season received the influenza immunization [9-11]. |
| Significance |
| Immunization signifies an imperative public health approach to disease prevention and health promotion [12]. According to the Advisory Committee on Immunization Practices (ACIP) of the CDC (2011) and ACOG (2010), all pregnant women are recommended to have the inactivated influenza vaccination at any time during the pregnancy [5,12]. Women’s access to healthcare during pregnancy represents an ideal time for Advanced Practice Nurses (APNs) to discuss immunization history, educate women about the importance of immunization, and recommend influenza immunization [12]. |
| Among healthy individuals, pregnant women and their healthy infants are more likely to develop serious complications related to influenza including premature labor and delivery [1]. Due to changes in the immune system, heart, and lungs during pregnancy, pregnant women infected with influenza virus are at increased risk of hospitalization, serious medical complications, and adverse pregnancy outcomes [13,14]. Healthy People (2020) reported 200,000 hospitalizations and 36,000 deaths each year resulting from influenza [15]. Increasing vaccination coverage of pregnant women offers significant preventative benefits to the woman and an indirect protection to her unborn child [16]. Evidence-based research supports the benefit of immunization for pregnant women and APN’s can take a lead role in educating patients and recommending vaccination. Individuals continue to contract this vaccine preventable infectious disease [17]. A preventative service, such as influenza immunization, is a critical public health intervention to improve maternal-child health [15]. |
| Purpose |
| The purpose of this study was to explore pregnant women’s knowledge, attitudes, and behaviors toward influenza immunization and their vaccination decisions. |
| Theoretical Framework |
| The Health Belief Model (HBM) utilizes six main constructs to explain health-seeking behavior. The HBM examines how people perceive the seriousness of a disease, their susceptibility of contracting that disease, benefits in preventing the disease, barriers to taking preventative action, factors that encourage action, and their ability to perform an action [18]. In the context of a health-related behavior, such as immunization, the HBM designates the desire to avoid illness and the belief that a specific health action will prevent illness. |
| Literature Review |
| Databases and electronic sources were evaluated utilizing a literature search strategy to identify peer reviewed journal articles, websites, and various public health authorities noting key terms to identify relevant literature. Medline, PubMed, Scopus, Science Direct, CINAHL, CDC, and the Cochrane Library were selected to review and synthesis literature regarding the following key words: influenza, influenza immunization, pregnancy, and vaccine safety. |
| Influenza virus is transmitted either directly or indirectly by infected respiratory droplets and is an acute and sometimes prolonged infectious illness [17]. The influenza viruses, considered orthomyxoviruses, are highly changeable, pathogenic viruses and in uncomplicated cases may cause fever/chills, sore throat, cough, headache, myalgia, fatigue, and rhinorrhea [7,12,19]. However, influenza viruses may lead to complications that are reported in databases as pneumonia and influenza, respiratory illness, cardiopulmonary outcomes, and death [20]. Influenza infection poses a health threat that to pregnant women and infants. Influenza continues to be a significant cause of morbidity and mortality among pregnant women. An increase in incidence among pregnant women, 2 to 3 fold higher than the general population has been reported [21]. Influenza immunization is an effective primary intervention to lessen the burden of influenza infection in the general population and specifically during pregnancy [6]. |
| Provider and patient barriers to vaccine uptake among pregnant women and strategies to optimize influenza vaccination in this population have been addressed [21,22]. Barriers reported in the study included safety concerns, lack of knowledge about influenza, and lack of access to care. A previous study examined predictors of pregnant women choosing to receive the influenza vaccination and cited attitudes toward influenza vaccination that included perceived protection of self/infant, anticipated regret, and safety concerns [5,23]. Reviewing international literature, pregnant women have concerns regarding the safety of the vaccine for themselves and their fetus causing ambivalence toward immunization [24]. |
| Multiple studies have been reviewed and cited comparable barriers including “safety concerns”, “not usual practice”, and “financial reasons” to vaccine uptake among pregnant women [20]. In addition, pregnant women’s awareness of influenza’s potential to cause serious illness and also report suboptimal influenza immunization coverage among pregnant women citing emotions and attitudes can be major barriers to vaccination coverage [16]. |
| Materials and Methods |
| A descriptive, exploratory design using a self-administered questionnaire examined attitudes, knowledge and behaviors of pregnant women in northern New Jersey. A purposive, convenience sample comprised of sixty pregnant women was recruited from a private OB/ GYN practice, after receipt of institutional review board approval. All pregnant women, while at the private practice, were invited by the RN to participate in the survey. Inclusion criteria included any patient from this practice who was pregnant, between the ages of 18 to 49 years, who could speak and understand English. Exclusion criteria: non English speaking patients. |
| The study used the 13 item CDC developed Internet Panel Survey, which addressed influenza vaccination coverage and knowledge, attitudes and behaviors related to end-of-season influenza vaccination among pregnant women [13]. The questions on the survey were selected from a pretested list of standard questions. In establishing reliability and validity, the questionnaire has been evaluated and revised to cover topics that have been comprehensively researched and has been compared to estimates from a known valid data source [13]. Content validity was established by having a panel of three obstetrician-gynecologists and three OB-GYN nurse educators review the questionnaire and minor changes were incorporated in the final version. |
| Four items elicited demographic information including maternal age (years), race/ethnicity, maternal education, and health insurance. Two items examined past history of influenza vaccination, receipt of influenza vaccination, as well as the reason for not receiving immunization. Seven items focused on the participant’s attitudes about influenza immunization. Implementation of the survey included utilizing a paper and pencil questionnaire that was administered in the OB-GYN office prior to or after an appointment. |
| Data Analysis |
| SPSS-19 was utilized for statistical analysis. Descriptive results (demographics) were reported as frequencies and percentages. Chi-square test of association between influenza vaccination and each descriptive statistic (age, race/ethnicity, education, and health insurance) were calculated. Influenza immunization knowledge, attitudes and behavior (vaccination coverage) among pregnant women will provide estimates of influenza vaccination coverage among pregnant women in the OB-GYN office for the 2012–2013 influenza seasons. And lastly, the reasons why pregnant women did not receive the influenza immunization were reported. The CDC Internet Panel Survey (2012) has categorized the responses: safety concern, concern about side effects of vaccine, and concern the vaccination would give me the flu; efficacy of vaccine/severity of the flu (don’t think the vaccine is effective, I do not need the vaccination, I don’t get very sick or can treat it; health reason; psychosocial reason; tangible barrier; and other reason [13]. |
| Results |
| Demographic characteristics |
| Demographic characteristics of the sample of pregnant women surveyed in this study Ninety-six percent of the pregnant women surveyed were between the ages of 25-49. Seventy percent of the respondents were white. Of the 60 women who participated in the survey, 93.3% had completed a college degree or more than college degree. Almost all of the participants (98.3%) had health insurance. The sample population mostly represented 25-49 year old pregnant women, predominantly White, non-Hispanic women, with a college degree, and health insurance. |
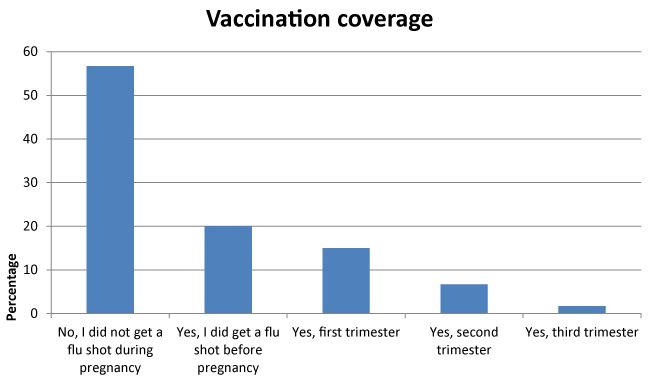
| Vaccination coverage |
| Fifty-seven percent of pregnant women (n = 34) participating in the survey choose not to be immunized. Among the forty-three percent (n = 26) receiving the influenza immunization. 20% received the immunization before pregnancy, 15% during the first trimester, 6.7% during the second trimester, and 1.7% during the third trimester (Figure 1). |
| Chi Square test of independence with vaccination and specific demographics |
| Sixty percent of White (non-Hispanic) women with a college degree or more, who had private health insurance declined influenza immunization. Eighty-three percent of Hispanic women, 50% of Black (non-Hispanic) women and 30% of those women who self-identified as other also declined influenza immunization. A chi-square test of independence was calculated comparing the result of ethnicity with vaccination (X2 (2) = 3.180, p > 0.05), indicating that ethnicity is independent from the women’s decision to receive the vaccination. |
| When education was factored into vaccination rates, approximately forty percent of those with college or more than college were vaccinated as compared to a 75% vaccination rate for women with less than college education. A chi-square test of independence was calculated comparing the result of education with vaccination (X2 (2) = 1.752, p > 0.05), indicating that education is independent from the women’s decision to take a vaccination in this sample. |
| A chi square test was calculated for age and vaccination (X2 (1) = 1.582, p > 0.05) and health insurance coverage and vaccination (X2 (2) =2.314, p > 0.05), maternal age and health insurance coverage are independent from the women’s decision to get vaccinated in this sample. |
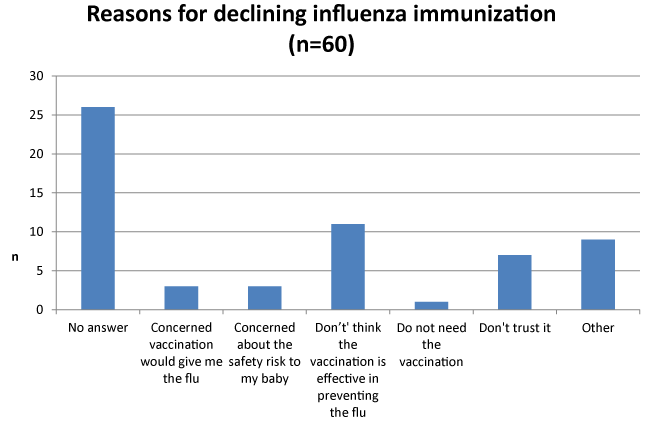
| Why women decline influenza immunization? |
| Fifty-six percent of women (n = 34) who reported not receiving the influenza immunization were asked to choose from a list of factors that possibly influenced their decision to decline vaccination. The most frequent response (18%) “I don’t think the vaccination is effective in preventing the flu.” The other most commonly selected reasons to decline the influenza immunization were “other” (15%), “don’t trust it” (11%), “concerned the vaccination would give her the flu” (5%), and “concerned about the safety risk to my baby” (5%). |
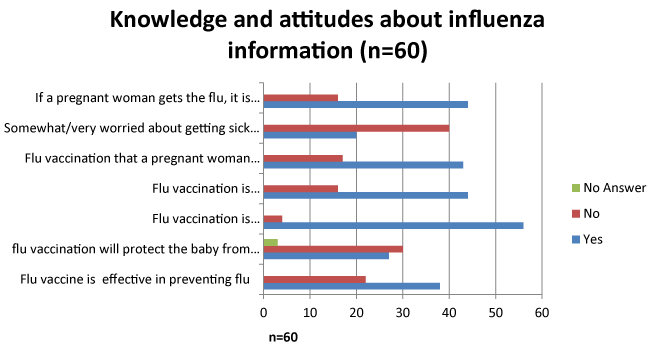
| Forty-five percent women (n = 27) agree/strongly agreed that by receiving the flu vaccine, their baby would be protected from getting influenza after birth. Ninety-three percent of the women (n = 56) believe that influenza immunization is somewhat/very/completely safe for most adult women. Fewer women (73%) believe that immunization is somewhat/very/completely safe for pregnant women. Approximately three-quarters of women believe that receiving the influenza immunization is somewhat/very/completely safe for her baby and also believe that if she contracts influenza, that it is somewhat/very likely to harm the baby. One third of women reported being somewhat/very worried about getting sick from this season’s influenza (Figure 2). |
| The vaccination coverage rate among pregnant women in this study (44%) was slightly lower than the national CDC (2011-2012) survey among pregnant women (47%) (13). Ninety-three percent of the respondents believe that the flu vaccine is somewhat/very effective for adult women but were less certain that the vaccine was effective for pregnant women (73%). Sixty-seven percent of the women surveyed were not worried about getting sick from the flu with, some women believing that the influenza immunization would not be effective in preventing the flu. Others indicated that they still did not trust the vaccine (12%). |
| Knowledge and Attitudes of efficacy and safety of vaccine with likelihood of vaccination |
| Sixty-three percent of the sample believed that the flu vaccine was somewhat/very effective in preventing the flu. A chi-square test of independence was calculated comparing the attitude of efficacy of vaccination to likelihood of vaccination (X2 (1) = 16.587, p < 0.05). Women who believed in the efficacy of the vaccination were more likely to get vaccinated then those who didn’t (Figure 3). |
| Forty two percent of the sample believed that the flu vaccine was safe for pregnant women to take. A chi-square test of independence was calculated comparing the attitude of safety of vaccination during pregnancy to likelihood of vaccination (X2 (1) = 12.219, p < 0.05). Women who believed the vaccine was safe to take during pregnancy were more likely to get vaccinated then those who did not. |
| Discussion |
| Perceived susceptibility and severity and the decision to vaccinate |
| One of the tenets of the HBM is perceived susceptibility, if a person believes him/herself to be susceptible and if that susceptibility could lead to negative health outcomes, the person is more likely to take preventive steps toward health [25]. Data indicated that when pregnant women perceived that they, and/or their infants, are at low risk of contracting influenza, they were less likely to receive the immunization. Sixty-seven percent of the women surveyed believed that they were at no risk of getting the flu, with fifty- six percent choosing not to be vaccinated. This data supports the HBM model. This study found that seventy-three percent of pregnant women believe if they get the flu, that it is likely to harm the baby; however, less than half of the women surveyed received the influenza vaccination. |
| Perceived barriers and the decision to vaccinate |
| This study explored the perceived barriers to influenza immunization by pregnant woman. When the pregnant woman did not perceive the efficacy of the flu vaccine they were less likely to get the vaccination. The most frequently selected reason for not getting the flu shot during pregnancy was a belief that the vaccination was not effective in preventing the flu and not trusting the vaccination. Twentyseven percent of pregnant women did not perceive the flu vaccine to be safe for themselves and for their babies. One-third of women were somewhat/very worried about getting sick from this season’s flu vaccination. |
| Perceived benefits and the decision to vaccinate |
| Pregnant women participating in this study who indicated that they perceived the vaccine to be an effective way to prevent the flu were more likely to get the flu vaccine (63%). The perceived benefit of staying healthy and preventing a negative health outcome was a positive determinant in their choice for vaccination. |
| Improving preventive behaviors in at risk populations |
| The blueprint for increasing preventative behaviors in populations has been provided through increasing the knowledge of perceived benefits and decreasing the barriers [25]. This model has been demonstrated to be effective in multiple public health research studies [26]. Morbidity and mortality rates increase as a result of influenza infection. Improving influenza immunization coverage among pregnant women is a critical public health intervention to improve maternal-child health [15]. The results from this study are consistent with previous CDC (2015) findings, demonstrating that half of pregnant women choose not to receive the influenza immunization [4]. |
| The importance of disease prevention through immunization must be emphasized to advance the health of pregnant women. Monitoring vaccination coverage rates, addressing reasons for not receiving the vaccination and educating pregnant women are necessary to improve coverage rates and protect pregnant women from complications related to influenza. The present survey revealed that some pregnant women did not think that the vaccination is effective in preventing the flu. Furthermore, some pregnant women had safety concerns about influenza immunization. Healthcare providers must understand how and why women make decisions to accept or refuse the influenza immunization, employ cues to action, and educate accordingly. |
| Limitations |
| The small convenience sample of pregnant women from a private suburban practice, with basic homogeneity of ethnicity, education and insurance coverage prevents generalization of the findings. The survey was adapted from a CDC study, but the questions provided responses that were not clearly indicative of level of susceptibility and/or severity therefore making the determination of the level of susceptibility, severity or intention difficult to assess. |
| Implications for Practice |
| Reducing barriers and increasing benefits are effective methods of changing preventive behaviors in large populations. Lack of knowledge and misinformation can affect health-related behaviors. Illness and serious complications may occur if pregnant women contract influenza. Healthcare providers can address the knowledge gap and educate pregnant women. Educating pregnant women about the importance of influenza immunization can help to increase women’s knowledge, attitude, and practice in health promotion and disease prevention. Effective information from a reliable trusted source may increase the patient’s knowledge of the flu vaccine’s safety and effectiveness to maternal and infant health. Healthcare providers, during prenatal visits, may provide information and the recommendation to receive the flu vaccine. |
References
- Fortner KB, Kuller JA, Rhee EJ, Edwards KM (2012) Influenza and tetanus, diphtheria, and acellular pertussis vaccinations during pregnancy. Obstetrics and Gynecology 67: 251-257.
- Saleeby E, Chapman J, Morse J, Bryant A (2009) H1N1 influenza in pregnancy: Cause for concern. Obstetrics and Gynecology 114: 885-891.
- Zaman K, Roy E, Arifeen SE, Rahman M (2008) Effectiveness of maternal influenza immunization in mothers and infants. New England Journal of Medicine 359: 1555-1564.
- Centers for Disease Control (2015) Estimating Seasonal Influenza-Associated Deaths in the United States: CDC Study Confirms Variability of Flu (2015, March 18).
- Centers for Disease Control and Prevention (2011) Estimating seasonal influenza-associated deaths in the United States.
- Coonrod, DV, Jimenez B, Sturgeon AN, Drachman D (2012) Influenza vaccine coverage among pregnant women in a public hospital system during the 2009-2010 pandemic influenza season. Influenza Research and Treatment.
- Hubka TA, Wisner KP (2011) Vaccinations recommended during pregnancy and breastfeeding. Journal of the American Osteopath Association, (111), Supplement 10: S23-S30.
- Lu P, Bridges CB, Euler GL, Singleton JA (2008) Influenza vaccination of recommended adult populations, U.S., 1989-2005. Vaccine 28: 1786-1793.
- Grohskopf L, Shay D, Shimabukuro T, Sokolow L, Keitel W, et al. (2013) Prevention and Control of Seasonal Influenza with Vaccines: Recommendations of the Advisory Committee on Immunization Practices —United States, 2013–2014.
- American Congress of Obstetricians and Gynecologists (2014) Influenza Vaccination during Pregnancy.
- Ding H, Black C, Ball S, Donahue S, Izrael D, et al. (2014) Influenza Vaccination Coverage among Pregnant Women — United States, 2013–14 Influenza Season.
- American College of Obstetricians and Gynecologists (2010) Immunization for women: Seasonal influenza (flu) for ob-gyns.
- Centers for Disease Control and Prevention (2012) Influenza Vaccination Coverage among Pregnant Women — 29 states and New York City, 2009–10 season. Morbidity and Mortality Weekly Report 61: 113-118.
- Ponnampalan S, Khalil A, O’Brien P (2011) Swine flu and pregnant women: Advice, prevention and management. British Journal of Midwifery 19: 76-80.
- Healthy People (2002) Objectives for influenza vaccination
- Centers for Disease Control and Prevention (2011) Influenza vaccination coverage among pregnant women---United States, 2010—11 influenza season. Morbidity and Mortality Weekly Report, August 19, 2011, 60: 1078-1082.
- Mersereau P, Layton C, Smith L, Kendrick J, Mitchell E, et al. (2012) Prenatal care providers and influenza prevention and treatment: Lessons from the field.Maternal and Child Health Journal 16: 479-485.
- United States Department of Health and Human Services (2005) Theory at a Glance: A guide for health promotion practice. National Institute of Health: 16-18.
- Prisco M (2002) Update your understanding of influenza. Nurse Practitioner 27: 32-41.
- Skowronski DM, De Serres G (2009) Is routine influenza immunization warranted in early pregnancy? Vaccine 27, 4754-4770.
- ShavelVI, Moniz MH, Gonik B, Beigi RH (2012) Influenza immunization in pregnancy: Overcoming patient and health care provider barriers. American Journal of Obstetrics and Gynecology, 107, S67-S74.
- Tucker-Edmonds BM, Coleman J, Armstrong K, Shea J (2011) Risk perceptions, worry, or distrust: What drives pregnant women’s decisions to accept the H1N1 vaccine? Maternal and Child Health Journal 15: 1203-1209.
- Thompson M, Williams J, Naleway A, Li DK, Chu S, et al. (2011) The pregnancy and influenza project:Design of an observational case-cohort study to evaluate influenza burden and vaccine effectiveness among pregnant women and their infants. American Journal of Obstetrics and Gynecology, 204, S69-76.
- Schindler M, Blanchard-Rohner G, Meier S, Martinez de Tejada B, Siegrist, CA, et al. (2012) Vaccination against seasonal flu in Switzerland: The indecision of pregnant women encouraged by healthcare professionals. Revue d'Epidemiologicet de SantePublique60: 447-453.
- Rosenstock IM, Strecher VJ, Becker MH. (1988) Social learning theory and the health belief model. Health Education Quarterly 15: 175-183.
- Carpenter CJ (2010) A meta-analysis of the effectiveness of the health belief model variables in predicting behavior. Health Communication 25: 661-669.
Figures at a glance
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 |
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 14868
- [From(publication date):
August-2015 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 10129
- PDF downloads : 4739
