Case Report Open Access
Does Combining Body Weight Support Treadmill Training with Thera- Band�?® Improve Hemiparetic Gait?
| Diana Veneri* | |
| Physical Therapy Department, University of Hartford, West Hartford, CT, USA | |
| Corresponding Author : | Diana Veneri Physical Therapy Department, University of Hartford 200 Bloomfield Avenue, West Hartford, CT 06117, USA Tel: (860)768-4542 E-mail: veneri@hartford.edu |
| Received March 26, 2012; Accepted April 27, 2012; Published April 30, 2012 | |
| Citation: Veneri D (2012) Does Combining Body Weight Support Treadmill Training with Thera-Band® Improve Hemiparetic Gait? J Nov Physiother 2:114. doi: 10.4172/2165-7025.1000114 | |
| Copyright: © 2012 Veneri D. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
Introduction: The purpose of this case report was to explore the use of Thera-Band® Elastic Band in combination with body weight support treadmill training during locomotor training of a person with chronic stroke. Methods: Inclusion and exclusion criteria were established and Institutional Review Board approvals were obtained. During treadmill training, the Thera-Band® was configured around the participant’s hemiparetic leg in a figure-8 fashion and attached to the harness of the body weight support. The purpose of the Thera-Band® was to assist with hip and knee flexion and ankle dorsiflexion during swing and proper foot placement during stance, avoiding excessive inversion. The locomotor training protocol consisted of thirty minutes of training at ten-minute intervals with five-minute rest periods in between, three times per week for a total of ten weeks. Outcome measures included fast gait speed, spatiotemporal variables of gait, endurance and strength of ankle eversion. Data collection occurred at baseline, during weeks five and ten of the training protocol and at six weeks follow-up (week sixteen). Results: All 90 training trials were completed. Mean gait speed increased from .625m/s at baseline to 1.10m/s at week sixteen. Gait distance increased from 191m at baseline to 367m at week 16; ankle eversion strength increased from 4.67 ± 0.45 to 5.90 ± 0.59 force/Kg. GAITRite data demonstrated a more symmetrical gait pattern, with a more equal step length and stance time when comparing the left and right limbs, and an increased stride length bilaterally. Discussion: The results of this case report with one participant demonstrated significant improvement in the fast walking speed, gait endurance, gait symmetry and spatiotemporal gait variables and ankle eversion strength. Several limitations and suggestions for further research were identified.
| Introduction |
| Body weight support treadmill training (BWSTT) is a treatment modality used for gait recovery of persons with stroke [1,2]. Patients with hemiparesis are able to walk with more normal gait kinematics, EMG timing and improved symmetry during BWSTT [3,4]. Manual assistance during BWSTT is sometimes necessary to properly align the trunk and advance and guide the lower extremity (LE) through a more normal gait trajectory, and provide stability during stance, particularly for those with severe weakness or spasticity [5,6]. The need for manual assistance can be problematic; it can require more than one individual to administer [7,8], it is difficult to consistently and adequately control the joint to produce kinematically correct steps [8-10], it can be exhausting and can place the physical therapist (PT) assisting the LE in a non-ergonomic position [7-10]. |
| The author hypothesized that the elastic properties of Thera-Band® Elastic Band (Thera-Band®) might lend well to assisting a hemiparetic LE through the gait cycle during BWSTT. Different colors of Thera- Band® were trialed to determine which band color offered the appropriate amount of resistance; enough to adequately assist the limb without interfering with either phase of gait. The middle of a piece of green Thera-Band®, approximately 78 inches in length (197cm), was placed under the shoe of the participant’s forefoot, crossed in front of the ankle and behind the knee in a figure-8 configuration. The two ends of the Thera-Band® were tied to a metal ring on the harness of the BWS near the participant’s upper anterior thigh area (Figure 1). The purpose of the Thera-Band® was to assist with hip and knee flexion and ankle dorsiflexion during swing and proper foot placement during stance. Since the overhead harness is fixed and the Thera-Band® is attached to it, as the treadmill draws the limb back, swing and forward progression of the limb are assisted. |
| A single subject case report was conducted to determine whether use of Thera-Band® during BWSTT could substitute for the participant’s AFO and need for manual assistance [11]. The study was conducted at a university research laboratory. The participant was a 54 year-old woman with right hemiparesis resulting from embolic stroke ten months prior. The participant ambulated with a large based quad cane and custom ankle foot orthoses. She was independent with household mobility and most activities of daily living, supervision for showers and required minimal assistance on uneven surfaces and elevations. Because of excessive abnormal tone, the participant’s foot was inverted without the AFO; the configuration of the Thera-Band® was modified for the participant with an additional medial to lateral wrap around the forefoot to draw the foot towards eversion. The 10- week training protocol was successfully administered and the primary objective was accomplished. However, it could not be concluded if improvements in secondary outcome measures of gait, strength and balance were a direct result of the training protocol, as the participant received a Botox injection to her spastic plantarflexors during week two of the protocol [11]. Therefore, the purpose of this second case report was to determine whether the combined interventions of BWSTT and Thera-Band® could be transferred to the clinical setting and result in measureable changes in gait speed, endurance, symmetry and temporal-spatial gait parameters, and strength of ankle eversion. |
| Materials and Methods |
| Physical therapists at a local outpatient rehabilitation hospital advertised the study, which sought a person with a single incidence of stroke with hemiparesis, and referred potential participants. Inclusion criteria included a minimum Functional Ambulatory Category (FAC) score of four, which indicates independent gait abilities on level surfaces with assistance for elevations and uneven terrain [12]. Physical therapy services were completed at least three months prior to the start of the training protocol as not to influence the study. If the participant had an exercise regimen before the start of the training protocol, he was encouraged to continue at the same frequency and intensity. Exclusion criteria included having a pre-existing medical condition that could interfere with the participant’s ability to successfully complete the training protocol. Informed consent from the participant and IRB approval from the university and hospital institution were obtained. |
| Participant profile |
| The participant was a 62 year-old male having experienced a cardio- embolic stroke nine months prior to the start of the study; his residual right hemiparesis involved the upper extremity (UE) more than the LE. He was retired and lived alone in an apartment with assistance from his family for his Instrumental Activities of Daily Living Skills (IADL). He ambulated limited community distances (~700’ at a time) with modified independence (Functional Independence Measure (FIM) of 6), as he used an AFO to prevent falls. It was decided during the preliminary screening session by the participant to discharge his AFO completely. During this screening, average fast gait speed was 0.619m/s using the Ten Meter Walk Test (10MWT) compared to a comfortable gait speed of 0.443m/s. A Mini Mental State examination was used to verify the participant’s ability to carry out two-step commands; the participant scored a 26/30 on the 11-item test, indicating no cognitive impairment [13]. The subject participated in a supervised community fitness program 4-5 days/week. His hourlong routine consisted of 10 minutes of cardiovascular work, UE and LE resistive exercises using equipment and standing balance activities in the parallel bars. |
| Outcome measures |
| The 10MWT was used to determine fast gait speed [14], since it has been shown to be a valid and reliable measure in individuals with stroke [15,16]. The Six-Minute Walk Test (6MWT) was utilized to measure gait endurance [17], and has excellent test-retest reliability [18,19]. Hand-held dynamometry (HHD) was used to measure ankle eversion strength; HHD is a valid and reliable measure of muscle strength [20,21]. GAITRite was performed to provide information about gait symmetry and spatiotemporal gait variables. The GAITRite system has strong concurrent validity and test- retest reliability, is portable and objectively assesses gait in the clinical setting [22]. Data collection occurred at baseline, during weeks five and ten of the training protocol and at six weeks follow-up (Week 16). |
| The five trials of the 10MWT and HHD were averaged for each data collection period. Scores were generated with percentage of improvements calculated for gait speed, endurance and strength. Results of the 10MWT and HHD were further assessed using the two standard deviation score. The key to the two standard deviation band method is the computation of the standard deviation for the baseline data. Statistical significance is computed directly from the standard deviation of the scores [23]. If at least two successive observations during the intervention phase fall outside the two standard deviation band, a statistically significant change in client performance has occurred across the two phases. This score could not be applied to the 6MWT because only one trial was performed during each data collection period. Additional comparisons were made with values for Minimal Detectable Change (MDC) and Minimally Clinically Important Difference (MCID) for the 10MWT and 6MWT. The MDC is defined as the amount of change in a variable that must be achieved to reflect a true difference. It is the smallest amount of difference that passes the threshold of error for a specific instrument and measure. The MCID is the smallest difference in a measured variable that signified an important rather than trivial difference in a participant’s condition [24]. |
| Training protocol |
| The subject participated in 30 minutes of training divided into three-ten minute blocks separated by five minute rest periods, three times a week for ten consecutive weeks [25,26]. The treatment intervention included BWSTT using LiteGait Model #LG360E with Thera- Band® configured around the hemiparetic LE as previously described (Figure 1). The Thera-Band® had to be tight enough to adequately assist the participant, but not too tight as to cause discomfort. The PT used visual analysis to determine the position of the foot to be the first metatarsal head in line with the tibia when applying the Thera- Band® to ensure consistent application. Initial fast treadmill speed was 0.22m/s without the Thera-Band®. With the Thera-Band®, speed was increased to 0.31m/s. Increasing gait speed was continuously encouraged and occurred with participant consent and when the new speed could be maintained throughout the training trial. |
| Body weight support was initially set at 30%, since using more would significantly reduce the activity of weight-bearing muscles in the hemiparetic LE [4]. The BWS was decreased by increments of 5 or 10%. This was done when the participant was observed demonstrating proper upper body alignment, good limb kinematics during the swing phase of gait [2,27] and felt comfortable. A safety lanyard was attached to the participant during all training. Since the participant admitted that he was apprehensive about locomotor training on a treadmill, he was allowed to hold the handrail. Vital signs were recorded before and after each training interval and included heart and respiratory rate, blood pressure (BP), and percent of oxygen saturation. The training trial was terminated at the request of the participant or if the exercise heart rate exceeded 116 beats per minute. The maximum exercise heart rate was calculated using the Karvonen Formula [28] incorporating both the participant’s age, resting heart rate and an exercise intensity of 60 percent; this was done to establish safe parameters for exercise intensity. |
| Results |
| All 90 training trials were completed. The participant reluctantly agreed to reduce BWS from 30% to 20% at session #53, to 15% at session #77 and finally to 10% at session #85. Changing the % BWS im-pacted treadmill speed; the participant trained at 0.85m/s with 20% BWS, and at 0.67m/s with 10% BWS. Mean fast gait speed increased from. 625m/s at baseline to 1.10m/s at week sixteen using the 10MWT, indicating a 76% improvement. With the 6MWT, the participant increased his gait distance from 191m at baseline to 367m at week 16, reflecting a 92% improvement; ankle eversion strength increased from 4.67 to 5.90 force/Kg, demonstrating a 27% improvement (Table 1). GAITRite data demonstrated a more symmetrical gait pattern, with a more equal step length and stance time when comparing the left and right limbs, and an increased stride length bilaterally (Table 2). The physical therapist administering the protocol stated that the Thera- Band® was easy to use and that she did not have to physically assist the patient at any time during locomotor training. |
| Discussion |
| Initial estimates of small meaningful change (0.2) for persons with stroke are near 0.06m/s for gait speed and 20m for distance; initial estimates for substantial meaningful change (0.5) are near 0.1 m/s and 49m for gait speed and distance, respectively [24]. Using these figures, the subject in this study experienced substantial meaningful change with respect to fast gait speed and distance. This improvement in fast gait speed is similar to the results of other BWSTT studies [25-27,29,30]. Using the two standard deviation rule [23], a gait speed to 0.67m/s would be significant for the 10MWT. The participant improved his gait speed to 1.10m/s at follow-up, indicating a significant change in gait speed. Minimal detectable change (MDC) was also achieved for the 6 MWT. Minimally clinically important differences (MCID) were achieved for the 10 MWT and 6 MWT (Table 3). When comparing treadmill speed among studies of participants with chronic stroke, studies with similar starting speeds did not progress as much, but study durations were shorter [31,32]. The subject in this study was able to double his treadmill speed, starting at 0.7 mph and progressing to 1.5 mph. It is possible that the additional intervention of Thera-Band® allowed the participant to progress his treadmill speed a bit faster. Since this protocol used training durations of 10 minutes, training at faster treadmill speeds should result in improved gait endurance and perhaps strength. Treatment interventions used in combination with BWSTT with the goal of increasing treadmill speed should be explored. |
| Hand-held dynamometry is not a typical outcome measure for studies using BWSTT for persons with stroke. Given the use of Thera- Band®, the researchers were curious about potential strength gains. Since gains were noted with ankle eversion, it seems that investigation of other muscle groups would be plausible. |
| Physical therapists should consider the spirit of this project and question the possibility of combining existing treatment interventions creatively; there is evidence to support the combined interventions of BWSTT and electrical stimulation to improve ambulation [33,34]. Coupling treatment interventions can solve a clinical problem and/or lead to improved function faster. Given the nature of healthcare and shorted lengths of stays and treatment durations, it is essential that treatment time maximizes patient function in the shortest time possible. While further study is necessary to develop and understand the effects of combining BWSTT and Thera-Band®, implications for clinical practice may be that Thera-Band® can replace the need for manual assistance. Implications research may be that subjects may be able to train faster, for longer periods of time and perhaps with better kinematics. |
| Limitations |
| There was no specific progression protocol for increasing gait speed or reducing BWS. The participant limited changes in treadmill speed and % BWS due to periodic elevated BP readings, despite assurance from his primary care physician. Use of the handrail during the training protocol may have affected the results. Use of the handrail increases single limb support and improves gait symmetry, but arm swing is a normal component of gait [6]. The participant was highly motivated to improve his functional status; therefore, it is not known if the same results would occur in persons with less motivation. The researchers neglected to measure the moment arm during dynamometry and were unable to compute torque. Because the protocol combined treatment modalities, it is not possible to know to what extent each modality contributed to the results i.e. BWSTT or Thera-Band®. The results of this case report included only one participant and cannot be generalized to all persons with chronic stroke. |
| Suggestions for Further Research |
| Increasing the study sample size will better validate the results. Since it is known that time matters with regard to neural plasticity, conducting similar studies with persons with acute stroke may yield different outcomes [35]. The protocol could be further developed to determine specific dosage parameters, treatment progression and weaning schedule. Another suggestion could be a crossover design study using BWSTT with and without Thera-Band® .Lastly, kinematic analysis and surface EMG would better qualify muscular activity during training. |
| Conclusions |
| The results of this case study indicated that the combined interventions of BWSTT and Thera-Band® could improve gait speed, endurance, gait symmetry, temporal-spatial gait parameters, and strength of ankle eversion. These results suggest that combining BWSTT and Thera-Band® has the potential to improve motor performance in subjects with stroke. Further investigation with a large sample is necessary to examine the effectiveness of combining BWSTT and Thera- Band® in people with stroke. |
| Acknowledgements |
| The author would like to thank and acknowledge the local investigators at Mount Sinai Rehabilitation Hospital in Hartford, Connecticut and the student research group who conducted the training protocol. |
References
- Sullivan KJ, Knowlton BJ, Dobkin BH (2002) Step training with body weight support: effect of treadmill speed and practice paradigms on poststroke locomotor recovery. Arch Phys Med Rehabil 83: 683-691.
- Barbeau H, Visintin M (2003) Optimal outcomes obtained with body-weight support combined with treadmill training in stroke subjects. Arch Phys Med Rehabil 84: 1458-1465.
- Hesse S, Konrad M, Uhlenbrock D (1999) Treadmill walking with partial body weight support versus floor walking in hemiparetic subjects. Arch Phys Med Rehabil 80: 421-427.
- Hesse S, Uhlenbrock D, Sarkodie-Gyan T (1999) Gait pattern of severely disabled hemiparetic subjects on a new controlled gait trainer as compared to assisted treadmill walking with partial body weight support. Clin Rehabil 13: 401-410.
- Hesse S, Werner C, von Frankenberg S, Bardeleben A (2003) Treadmill training with partial body weight support after stroke. Phys Med Rehabil Clin N Am 14: S111-123.
- Chen G, Patten C, Kothari DH, Zajac FE (2005) Gait deviations associated with post-stroke hemiparesis: improvement during treadmill walking using weight support, speed, support stiffness, and handrail hold. Gait Posture 22: 57-62.
- Freivogel S, Mehrholz J, Husak-Sotomayor T, Schmalohr D (2008) Gait training with the newly developed 'LokoHelp'-system is feasible for non-ambulatory patients after stroke, spinal cord and brain injury. A feasibility study. Brain Inj 22: 625-632.
- Hornby GT, Campbell DD, Zemon DH, Kahn JH (2005) Clinical and Quantitative Evaluation of Robotic-Assisted Treadmill Walking to Retrain Ambulation After Spinal Cord Injury. Top Spinal Cord Inj Rehabil 11: 1-17.
- Mayr A, Kofler M, Quirbach E, Matzak H, Fr�?¶hlich K, et al. (2007) Prospective, blinded, randomized crossover study of gait rehabilitation in stroke patients using the Lokomat gait orthosis. Neurorehabil Neural Repair 21: 307-314.
- Westlake KP, Patten C (2009) Pilot study of Lokomat versus manual-assisted treadmill training for locomotor recovery post-stroke. J Neuroeng Rehabil 6: 18.
- Veneri D (2011) Combining the treatment modalities of body weight support treadmill training and Thera-Band: a case study of an individual with hemiparetic gait. Top Stroke Rehabil 18: 402-416.
- Werner C, Lindquist AR, Bardeleben A, Hesse S (2007) The influence of treadmill inclination on the gait of ambulatory hemiparetic subjects. Neurorehabil Neural Repair 21: 76-80.
- Folstein MF, Folstein SE, McHugh PR (1975) "Mini-mental state". A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12: 189-198.
- Collen FM, Wade DT, Bradshaw CM (1990) Mobility after stroke: reliability of measures of impairment and disability. Int Disabil Stud 12: 6-9.
- Richards CL, Malouin F, Dean C (1999) Gait in stroke: assessment and rehabilitation. Clin Geriatr Med 15: 833-855.
- Salbach NM, Mayo NE, Higgins J, Ahmed S, Finch LE, et al. (2001) Responsiveness and predictability of gait speed and other disability measures in acute stroke. Arch Phys Med Rehabil 82: 1204-1212.
- Kosak M, Smith T (2005) Comparison of the 2-, 6-, and 12-minute walk tests in patients with stroke. J Rehabil Res Dev 42: 103-107.
- Flansbjer UB, Holmb�?¤ck AM, Downham D, Patten C, Lexell J (2005) Reliability of gait performance tests in men and women with hemiparesis after stroke. J Rehabil Med 37: 75-82.
- Eng JJ, Dawson AS, Chu KS (2004) Submaximal exercise in persons with stroke: test-retest reliability and concurrent validity with maximal oxygen consumption. Arch Phys Med Rehabil 85: 113-118.
- Bohannon RW (1997) Discriminant Construct Validity of Hand-Held Dynamometry and Manual Muscle Testing in a Home Care Setting. J Phys Ther Sci 9: 57-61.
- Bohannon RW (1999) Intertester reliability of hand-held dynamometry: a concise summary of published research. Percept Mot Skills 88: 899-902.
- Bilney B, Morris M, Webster K (2003) Concurrent related validity of the GAITRite walkway system for quantification of the spatial and temporal parameters of gait. Gait Posture 17: 68-74.
- Ottenbacher K (1986) Evaluating clinical change: Strategies for occupational and physical therapists. Williams & Wilkins, Baltimore, USA.
- Perera S, Mody SH, Woodman RC, Studenski SA (2006) Meaningful change and responsiveness in common physical performance measures in older adults. J Am Geriatr Soc 54: 743-749.
- Miller EW, Quinn ME, Seddon PG (2002) Body weight support treadmill and overground ambulation training for two patients with chronic disability secondary to stroke. Phys Ther 82: 53-61.
- Flom-Meland C, Herring A, Olson AS, Perkerewicz S, Runyan A (2005) Gait recovery. Rehab Manag 18: 18, 20-21.
- Sullivan K, Klassen T, Mulroy S (2006) Combined task-specific training and strengthening effects on locomotor recovery post-stroke: a case study. J Neurol Phys Ther 30: 130-141.
- Hill DC, Ethans KD, MacLeod DA, Harrison ER, Matheson JE (2005) Exercise stress testing in subacute stroke patients using a combined upper- and lower-limb ergometer. Arch Phys Med Rehabil 86: 1860-1866.
- Mudge S, Rochester L, Recordon A (2003) The effect of treadmill training on gait, balance and trunk control in a hemiplegic subject: a single system design. Disabil Rehabil 25: 1000-1007.
- Lindquist AR, Prado CL, Barros RM, Mattioli R, da Costa PH, et al. (2007) Gait training combining partial body-weight support, a treadmill, and functional electrical stimulation: effects on poststroke gait. Phys Ther 87: 1144-1154.
- Yen CL, Wang RY, Liao KK, Huang CC, Yang YR (2008) Gait training induced change in corticomotor excitability in patients with chronic stroke. Neurorehabil Neural Repair 22: 22-30.
- Peurala SH, Tarkka IM, Pitk�?¤nen K, Sivenius J (2005) The effectiveness of body weight-supported gait training and floor walking in patients with chronic stroke. Arch Phys Med Rehabil 86: 1557-1564.
- Kleim JA, Jones TA (2008) Principles of experience-dependent neural plasticity: implications for rehabilitation after brain damage. J Speech Lang Hear Res 51: S225-239.
Tables and Figures at a glance
| Table 1 | Table 2 | Table 3 |
Figures at a glance
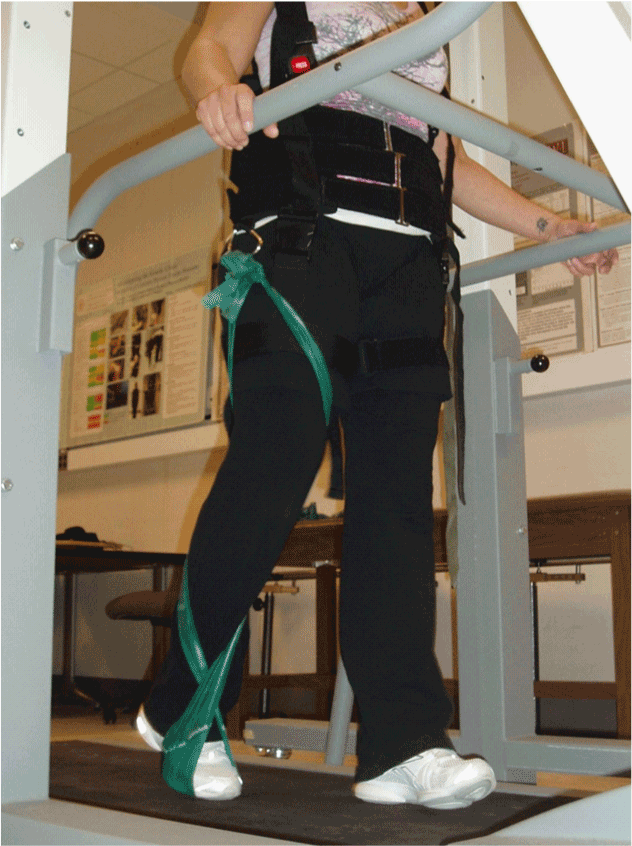 |
| Figure 1 |
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 14994
- [From(publication date):
September-2012 - Sep 03, 2025] - Breakdown by view type
- HTML page views : 10317
- PDF downloads : 4677
