Case Report Open Access
Dry Gangrene Of The Glans Penis In A Patient With Bilateral Foot Ulcers And Severe Vascular Disease: A Case Report
Jeremy T Smith* and Eric M BlumanBrigham Foot and Ankle Center, Faulkner Hospital, Suite 56, 1153 Centre Street, Boston, MA 02130,USA
- *Corresponding Author:
- Jeremy T. Smith, MD
Brigham Foot and Ankle Center
Faulkner Hospital
Suite 56, 1153 Centre Street
Boston, MA 02130, USA
Tel: 617-983-7295
Fax: 617-983-7201
E-mail: jsmith42@partners.org
Received date January 01, 2013; Accepted date July 20, 2013; Published date July 23, 2013
Citation: Smith JT, Bluman EM (2013) Dry Gangrene of the Glans Penis in a Patient with Bilateral Foot Ulcers and Severe Vascular Disease: A Case Report. Clin Res Foot Ankle 1:114. doi: 10.4172/2329-910X.1000114
Copyright: © 2013 Smith JT, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Clinical Research on Foot & Ankle
Abstract
Orthopaedic surgeons, particular foot and ankle surgeons are frequently asked to assist with the treatment of patients with lower extremity ulcerations and infections related to diabetes and/or vascular disease. The case report presents the history and clinical images of a patient with diabetes and multiple medical co-morbidities who presented with bilateral lower extremity ulcerations and dry gangrene of the glans penis. This case is presented because it is a striking example of the end-organ effects of diabetes and associated vascular disease.
Introduction
Orthopaedic surgeons, particular foot and ankle surgeons are frequently asked to assist with the treatment of patients with lower extremity ulcerations and infections related to diabetes and/or vascular disease. According to the United States Centers for Disease Control and Prevention, more than 25 million patients in the United States had diabetes in 2010 [1], and this number has very likely increased since that time. Foot problems are very prevalent in patients with diabetes with approximately 30% of all hospital admissions in diabetics related to problems with the feet [2].
In the United States, patients with diabetes account for more than 60% of all nontraumatic lower extremity amputations [1]. The causes of these amputations are often multifactorial, including neuropathy, infection, ischemia, and ulceration [3,4] As the duration of diabetes lengthens in an individual patient, so does the risk of developing peripheral vascular disease [5]. The care of a patient with a lower extremity diabetic ulceration is often complicated by medical co-morbidities. These include, but are not limited to, peripheral vascular disease, cardiac disease, chronic renal insufficiency, immunocompromise, and poor nutrition.
Case Report
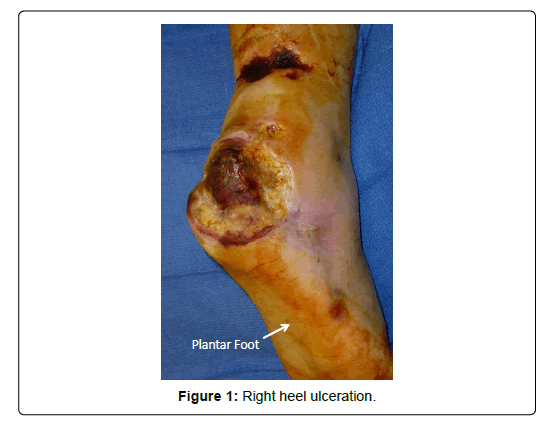
A 47-year-old man presented to the orthopaedic service with bilateral foot ulcers. He had previously had a left midfoot amputation and now presented with a wound dehiscence and recurrent osteomyelitis. He also had a full-thickness ulceration of the right heel with calcaneal osteomyelitis (Figure 1). Treatment for his lower extremity ulcers required a left revision midfoot amputation and a right below knee amputation.
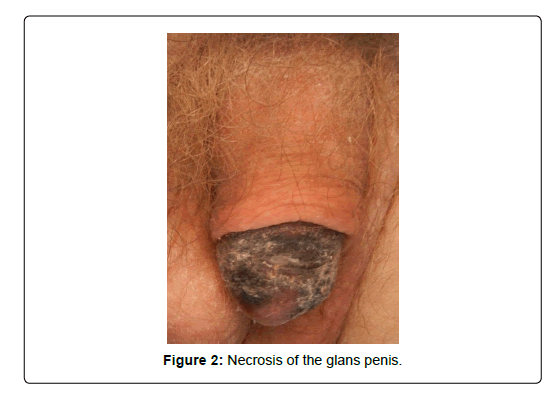
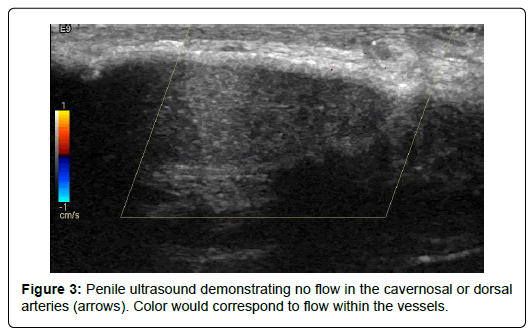
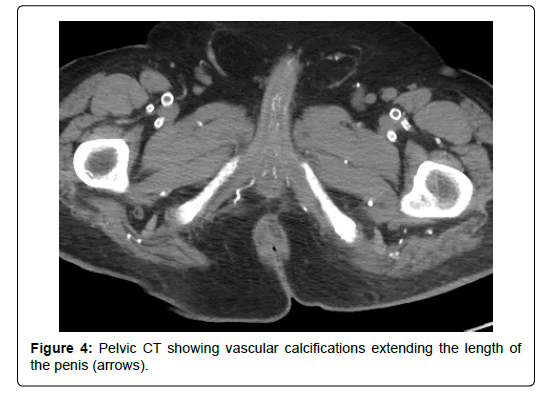
His medical history included diabetes mellitus, end-stage renal disease treated with hemodialysis, and peripheral vascular disease. While undergoing treating for his lower extremity ulcerations, he reported pain in his penis. Physical examination revealed a circumcised penis with dry gangrene of the glans (Figure 2). The urology service was consulted and a penile ultrasound demonstrated no flow in the cavernosal or dorsal arteries (Figure 3). A computed tomography scan of the pelvis showed vascular calcifications extending the length of the penis (Figure 4). This patient’s penile necrosis was treated non-surgically with observation. He ultimately underwent auto-amputation of the glans penis with meatal stenosis, requiring placement of a suprapubic tube.
Discussion
The case report presents the history and clinical images of a patient with diabetes and multiple medical co-morbidities who presented with bilateral lower extremity ulcerations and dry gangrene of the glans penis. This case is presented because it is a striking example of the endorgan effects of diabetes and associated vascular disease.
Dry gangrene of the glans penis is usually caused by vascular disease [6]. Blood supply to the skin of the penis is from the femoral artery and then the superficial external pudendal arteries. The deeper structures of the penis are supplied from three branches of the internal pudendal artery, the bulbourethral artery, the dorsal artery, and the cavernosal artery. The terminal branches of the dorsal artery supply the glans penis. Figure 3: Penile ultrasound demonstrating no flow in the cavernosal or dorsal arteries (arrows). Color would correspond to flow within the vessels. Figure 4: Pelvic CT showing vascular calcifications extending the length of the penis (arrows). Submit
Glans necrosis has been described previously in case reports [7,8] and a series of seven patients with diabetes [9]. In addition to vascular disease, causes of penile glans necrosis include calciphylaxis, thromboembolic disease, penile strangulation from priapism, paraphimosis, or constrictive devices [8]. Glans necrosis of the penis has been associated with a high mortality rate, as high as 57% within six months, largely because of the severe associated vascular disease [10].
Our approach for treating a lower extremity diabetic ulceration involves alleviating mechanical pressure due to contractures and external compression, addressing the patient’s vascular status and nutritional status, and treating infection if present. In addition, we regularly involve our colleagues in Internal Medicine, Endocrinology, Vascular Surgery, Infectious Disease, Nephrology, Rehabilitation, and Prosthetics. In the case of the patient presented here, we also involved our Urology colleagues. This case clearly illustrates the importance of a multi-team approach to caring for diabetic patients with foot pathology.
References
-
Centers for Disease Control and Prevention (2011) National diabetes fact sheet, 2011.
- Coughlin MJ, Mann RA, Saltzman CL (2007) Surgery of the foot and ankle. (8thedn), Mosby, Philadelphia PA.
- Holewski JJ, Moss KM, Stess RM, Graf PM, Grunfeld C (1989) Prevalence of foot pathology and lower extremity complication in a diabetic outpatient clinic. J Rehabil Res Dev 26: 35-44.
- Pecoraro RE, Reiber GE, Burgess EM (1990) Pathways to diabetic limb amputation. Basis for prevention. Diabetes Care 13: 513-521.
- Medvei VC (1982) History of Endocrinology. MPT Press, Lancaster.
- Gillitzer R, Franzaring L, Hampel C, Pahernik S, Bittinger F, et al. (2004) Complete gangrene of penis in a patient with arterial vascular disease. Urology 64: 1231.e 4-e6.
- Sorensen MD, Long LO, Wessells H, Kuan JK (2007) Monckeberg’s calciphylaxis with necrosis of the glans penis: a case presentation. Hemodial Int 11: 300-302.
- Vijayan P (2009) Gangrene of the penis in a diabetic male with multiple amputations and follow up. Indian J Urol 25: 123-125.
- Stein M, Anderson C, Ricciardi R, Chamberlin JW, Lerner SE, et al. (1994) Penile gangrene associated with chronic renal failure: report of 7 cases and review of the literature. J Urol 152: 2014-2016.
- Weiner DM, Lowe FC (1996) Surgical management of ischaemic penile gangrene in diabetics with end stage atherosclerosis. J Urol 155: 926–929.
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 22058
- [From(publication date):
July-2013 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 17350
- PDF downloads : 4708