Dynamic Lumbar Stabilization with Peek Rod/Titanium to Prevent Adjacent Disc Pathology
Received: 24-Nov-2016 / Accepted Date: 27-Dec-2016 / Published Date: 07-Jan-2017
Keywords: Lumbar; syndrome; intervertebral; discectomy; Biomechanical; ligament; degenerative; Titanium; stenosis; etiopathogeny
79069Introduction
Over the last decades segmental spinal fusion has become the standard surgical procedure for lumbar degenerative spondyloarthropathy [1]. Its evolution towards the most modern instrumentation techniques has achieved a very high percentage of success in spinal fusion in the lumbar region [2]. This varies between 72 and 91%, depending on the technique used. But the success of lumbar fusion has been seen to be accompanied by the appearance of what is known as adjacent segment disease [3]. These pathological changes, which may appear in the disc above or below the fusion as degenerative disc disease [4-7], segmental instability or spinal stenosis, have high prevalence and reoperation rates. Spinal fusion resulting in the increase of intradiscal pressure (IDP) on the adjacent segment has been pointed at as being the etiopathogeny of this syndrome.
Method
The sample comprises 50 patients who were operated on between January and December 2014. They age range was between 28 and 45, 38 of whom were male and 12 female.
Pre and post-surgical Oswestry questionnaire was carried out, resulting in figures, which varied from 56.8% to 21.4% respectively. Pre and post-surgical simple x-ray studies have been analysed. Possible Modic and intervertebral disc rehydration changes have also been evaluated. We used the standard surgical approach via the lumbar midline until we identified the articular capsule endeavouring not to damage the same [8]. When it was necessary to carry out a discectomy the habitual procedure was followed until the neural elements were uncovered. This was followed by the placement of screws in the transverse facet angle. The pathology intervened was determined based on the classification of the degenerative pathology established by GDubois [9], based on what is known as the Kirkaldy-Willis degenerative cascade dating from 1978 (Table 1).
| Phase | Instability |
|---|---|
| Phase 1 | Spondylarthritis + disc primary |
| Phase 2 | Disc prolapse + Phase 1 |
| Phase 3 | Discopathy + Phase 1 |
| Phase 4 | Funtional Instability + Phase 3 |
| Phase 5 | One level stenosis + Phase 4 |
| Phase 6 | Multi-level stenosis + Phase 4 |
| Phase 7 | Structural Deformities |
Table 1: Phases of instability.
The pathology corresponds to degenerative disc disease, spinal stenosis and lumbar instability. The most frequent pathology operated on was degenerative discopathy (Table 2).
| Pathology | No. of Cases |
|---|---|
| Disc Degenerative | 35 |
| Canal stenosis | 10 |
| Lumbar instability | 5 |
Table 2: Pathology involved.
Result
In the 50 cases treated using this method, we have, in general, observed a notable improvement of the patients' symptoms. Based on our experience we can say that sciatica symptoms disappear in 80% of cases, absence of lower back pain in 70% and a sufficient reduction of the said symptoms to enable the majority to carry out a normal active life, progressing from a 56.8% in the pre-surgery Oswestry questionnaire to an a post-surgery evaluation of 21.4%. There has been recuperation of work activity in 46 cases, i.e., 82%. Logically, reincorporation becomes more compromised depending on how demanding the work activity is (Table 3).
| Type of Work | Measure of activity |
|---|---|
| Mild | 10 |
| Moderate | 25 |
| Heavy | 15 |
Table 3: Work activity.
Discussion
1995 saw the first implant of a dynamic neutralization system for the treatment of a degenerative disc disease. In 1998 they published the first results from 50 cases and, in 2000, their update on 150 cases. In these works, apart from presenting the technique, the authors describe their indications, based on the classification they themselves have established for degenerative lumbar spine disease according to the Kirkaldy-Willis criteria, excluding primary disc pathology, hypomobile disc disease and structural deformities [4,10,11].
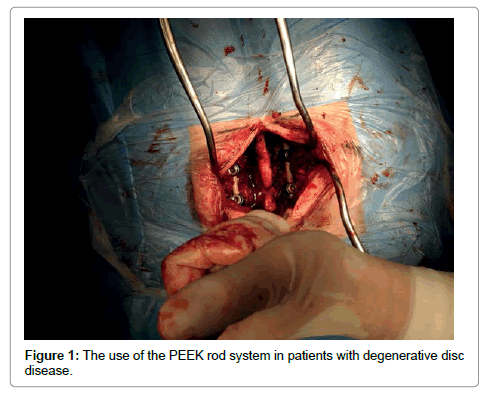
Our series represents a statistical number comparable to the results obtained by other authors, by prescribing the use of the PEEK rod system in patients with degenerative disc disease (Figure 1), although we have also included mono-segmental degenerative slipped discs in the same.
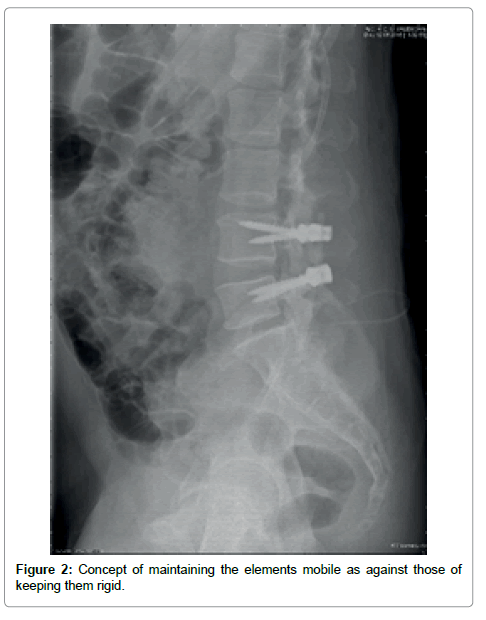
The main advantage compared to instrumented fusion precisely lies in the fundamental concept of maintaining the elements mobile as against those of keeping them rigid (Figure 2).
Conclusion
The short term results seem to be encouraging as regards dynamic stabilization systems using pedicle screws and semi-rigid rods and it obvious that long term clinical trials are necessary to analyse how efficient they are in comparison to traditional fusion procedures [10-13].
Biomechanical studies of the adjacent segment allow the same to be protected by means of the use of semi-rigid PEEK cages, which means that it would be a good alternative means of protection given that it is not necessary to involve the ligament or the pedicles of the segment adjacent to the fusion.
References
- Sénégas J (2002) Mechanical supplementation by non-rigid fixation in degenerative intervertebral lumbar segments: The Wallis system. Eur Spine J 11: S164-S169.
- Redaelli A, Caserta S, La Maida GA, Misaggi B, Per oni D, et al. (2002) Elastic stabilization alone or combined with rigid fusion in spinal surgery: A biomechanical study and clinical experience are based on 82 cases. Euro Spine J 11: S192–S197.
- Yang JY, Lee JK, Song HS (2008) The impact of adjacent segment degeneration on the clinical outcome after lumbar spinal fusion. Spine 33: 503-507.
- Kumar MN, Jacquot F, Hall H (2001) Long-term follow-up of functional outcomes and radiographic changes at adjacent levels following lumbar spine fusion for degenerative disc disease. Eur Spine J 10: 309-313.
- Okuda S, Iwasaki M, Miyauchi A, Aono H, Morita M, et al. (2004) Risk factors for adjacent segment degeneration after PLIF. Spine 29: 1535-1540.
- Ghiselli G, Wang JC, Bhatia NN, Hsu WK, Dawson EG (2004) Adjacent segment degeneration in the lumbar spine. J Bone Joint Surg Am 86: 1497-1503.
- Harrop JS, Youssef JA, Maltenfort M, Vorwald P, Jabbour P, et al. (2008) Lumbar adjacent segment degeneration and disease after arthrodesis and total disc arthroplasty. Spine 33: 1701-1707.
- Kim YS, Zhang HY, Luna BJ, Parque KW, Ji KY, et al. (2007) Nitinol bar dynamicrodstabilizationsystem and memoryloopsNitinol in surgicaltreatmentfor lumbar disc disorders: Short-term follow-up. Neurosurg Focus 22: E10.
- Dubois G (1999) Dynamic neutralization, a new concept for restabilization of the spine. Neuroradiology J 12: 175-176.
- Maserati MB, Tormenti MJ, Panczykowski DM, Bonfield CM, Gerszten PC (2010) The use of a hybrid dynamic stabilization and fusion system in the lumbar spine: preliminary experience. Neurosurg Focus 28: E2.
- Putzier M, Hoff E, Tohtz S, Gross C, Perka C, et al. (2010) Dynamic stabilization adjacent to single-level fusion: part II. No clinical benefit for asymptomatic, initially degenerated adjacent segments after 6 years follow-up. Eur Spine J 19: 2181-2189.
- Aota Y, Kumano K, Hirabayashi S (1995) Post fusion instability at the adjacent segments after rigid pedicle screw fixation for degenerative lumbar spinal disorders. J Spinal Disord 8:464-473.
- Cheh G, Bridwell KH, Lenke LG, Buchowski JM, Daubs MD, et al. (2007) Adjacent segment disease following lumbar/thoracolumbar fusion with pedicle screw instrumentation: A minimum 5-year follow-up. Spine 32: 2253-2257.
Citation: Arrotegui I (2017) Dynamic Lumbar Stabilization with Peek Rod/Titanium to Prevent Adjacent Disc Pathology. J Med Imp Surg 2: 111.
Copyright: © 2017 Arrotegui I. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Usage
- Total views: 5218
- [From(publication date): 0-2017 - Sep 01, 2025]
- Breakdown by view type
- HTML page views: 4322
- PDF downloads: 896