Make the best use of Scientific Research and information from our 700+ peer reviewed, Open Access Journals that operates with the help of 50,000+ Editorial Board Members and esteemed reviewers and 1000+ Scientific associations in Medical, Clinical, Pharmaceutical, Engineering, Technology and Management Fields.
Meet Inspiring Speakers and Experts at our 3000+ Global Conferenceseries Events with over 600+ Conferences, 1200+ Symposiums and 1200+ Workshops on Medical, Pharma, Engineering, Science, Technology and Business
Editorial Open Access
Environmental Risk Factors for Anterior Encephaloceles: 15 Years' Experience at a Tertiary Centre in India
| Hemonta Kr Dutta1* and Debasish Borbora2 | |
| 1Department of Pediatric Surgery, Assam Medical College & Hospital, Dibrugarh 786002, Assam, India | |
| 2Department of Biotechnology, Gauhati University, Guwahati 781014, Assam, India | |
| Corresponding Author : | Hemonta Kr Dutta Department of Pediatric Surgery Assam Medical College & Hospital Dibrugarh, Assam, India Tel: 91 9435031257 E-mail: hemontdut@gmail.com |
| Received February 23, 2015; Accepted February 24, 2015; Published February 26, 2015 | |
| Citation: Dutta HK, Borbora D (2015) Environmental Risk Factors for Anterior Encephaloceles: 15 Years’ Experience at a Tertiary Centre in India. J Preg Child Health 2:e109. doi: 10.4172/2376-127X.1000e109 | |
| Copyright: © 2015 Dutta HK, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Pregnancy and Child Health
| Keywords |
| Anterior encephalocele; Sincipital encephalocele; Congenital malformations; Risk factors; Assam |
| Introduction |
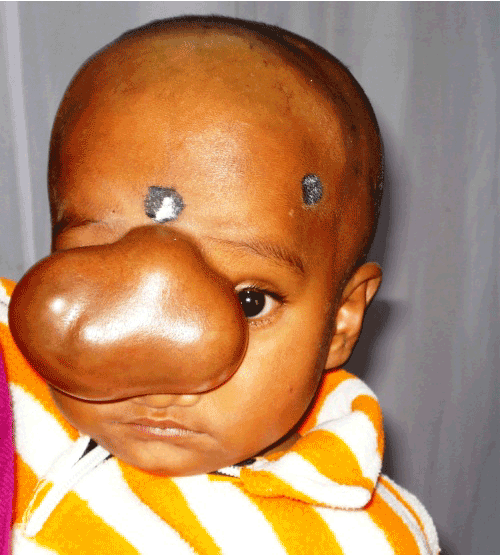
| Anterior encephaloceles (AE) are rare forms of neural tube defects (NTD) which are characterized by the herniation of brain tissue through a congenital defect in the skull. Based on their location they are subdivided into sincipital and basal. Sincipital encephaloceles are further classified into nasofrontal, nasoethmoidal, and nasoorbital. Although sporadic in the western world, the condition is frequent in few Southeast Asian countries like Myanmar and Malaysia [1]. In India however, this malformation is seen frequently among the tea garden communities of Assam [2,3]. As NTD show marked ethnic and geographic variations, the role of environmental factors causing these malformations could be significant. Accordingly, WHO has outlined maternal diabetes, alcohol abuse, antenatal X-irradiation, aminopterin and hallucinogen ingestion as known risk factors of NTD. Tea garden communities in Assam are socioeconomically backward and they are exposed to various chemicals used in tea gardens. So this study was conducted among patients attending Assam Medical College & Hospital (AMCH), a tertiary health care centre in Assam (Northeast India) to identify possible environmental risk factors of AE. |
| Materials and Methods |
| A retrospective chart review of patients with AE who were born at or referred to AMCH between January 1999 and December 2013 was performed to evaluate various lifestyle and environmental risk factors which may contribute to the disease. This study was approved by the institutional ethical committee and consent was obtained from all participating parents. Parental BMI (kg/m2) was classified according to the criterions suggested by WHO for the Asian populations. In case of children, the BMI-for-age percentile was used to interpret ‘Weight Status Categories’. |
| Results |
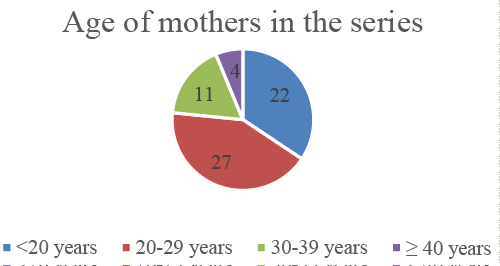
| 64 patients were treated at the Pediatric surgery department during the 15 years period. The number of female cases was marginally higher than the males at a ratio of 1.2:1 with a mean age of 36 months (1 month-14 years). 40 children had naso-ethmoidal, 20 children had naso-frontal and 4 had naso-orbital encephaloceles (Figure 1). Of the 64, 61 (95.3%) cases were of the tea garden community with either one or both parents of 58 children reportedly engaged as manual workers in the tea gardens. Families of all the 64 children were socio economically weak, living in hutments either in the midst or in the vicinity of tea gardens. In the present series, 22 patients were born to mothers aged < 20 years and 4 were born to mothers aged >39 years, indicating that advanced maternal age accounted for 40.6% of the cases (Figure 2). Advanced Multi-parity among the mothers was frequent with 56.3% having a parity ≥3 and 17.2% having a parity >5 (Figure 3). History of past abortions was reported in 15 mothers. 30 mothers never received folate supplementation during pregnancy. Of the 34 who received folate supplementation, only 2 women received it during the 1st trimester of pregnancy. 35.9% of the mothers had BMI <18.5. 53.1% of the mothers were anemic with the level of hemoglobin <10 gm% and in 65.6% mothers serum albumin level was <3.5gm/dl. In our series, 12 babies were born to consanguineous parents. 4 of them were first cousins and 6 were second cousins. |
| Discussion |
| These study reports of a high incidence of anterior encephalocele in Assam which after stratification clearly indicates that majority of the cases came from the tea garden community. The tea garden communities are quite distinct from other communities of Assam. And within this impoverished community, our study observes several lifestyle and environmental risk factors that could predispose children to AE. |
| The use of weedicides and pesticides is widespread in tea gardens. Pesticides such as organophosphates and pyrethrins are known to cause neurotoxicity by inhibiting acetylcholine activity [4]. In utero exposure to some pesticides can lead to psychomotor developmental delay in the child [5]. Studies have also associated parental exposure to pesticides with the risk of NTD [6-8]. In the present series, one or both the parents of 58 children reported exposure to various agricultural pesticides and weedicides. Male members were mostly involved in spraying of pesticides. It was also significant to note that families of all the 64 children lived in hutments either in the midst or in the vicinity of tea gardens and it is likely that the water and food they consume could also be contaminated with pesticides. |
| Advanced maternal age was also a distinct risk factor in this study. According to Vaughan et al. children born to mothers aged ≤17 years and ≥40 years were at a greater risk of having a congenital anomaly [9]. A systematic review analyzing risk factors associated with stillbirth in high-income setting also concluded that maternal age >35 years is a major modifiable risk factor [10]. Similar observations were also reported during independent studies conducted by Suphapeetiporn et al. and Mashuda et al. [1,11]. In the present series too, 22 children were born to mothers aged < 20 years and 4 to mothers aged >40 years. This is in corroboration with finding by Taksande et al. from Maharashtra [12] and Grover et al. from Shimla [13]. Previous studies have associated grand multipara with the risk of congenital malformations [13,14,11] but in their systematic review Shah et al. did not observe any association between grand multiparity, great grand multiparity and pregnancy outcomes [15]. In this study however, 56% of the mothers had parity of 3 or more and 17% had parity more than 5, indicating a possible association. We believe that advanced maternal age along with multiparity could result in unfavorable intrauterine environment causing AE among the newly born. |
| Maternal nutrition is a modifiable risk factor associated with adverse birth outcomes, particularly in developing economies/lowincome populations [16]. In the present series, 35% of the mothers had BMI <18.5, 53.1% were anemic and 65.6% mothers had serum albumin levels <3.5gm/dl. These figures clearly indicate that low socio economic status had a bearing on the mother’s diet during pregnancy which might have affected the growing fetus. It is known that supplementing 4 mg folic acid per day for at least one month prior to conception to 3 months post conception reduces the risk of recurrence of NTD by 70% [17], but in the present series, mother of 30 children reportedly did not receive folate supplementation during pregnancy and 32 mothers consumed folic acid only after 3 months of pregnancy. |
| In this report, 61 cases were from the tea garden community of which 12 were born to consanguineous parents. As the association of birth defects with consanguinity is known [18], intrafamilial marriages within this community could explain for the high incidence of AE as it increases the prevalence of homozygotes for autosomal recessive genetic disorders. The study concludes that low socioeconomic status, pesticides exposure, advanced maternal age, increasing parity and maternal malnutrition may contribute to the occurrence of AE. Although there were no clustering of AE cases in this present study, 90% of the patients hailed from the 6 upper Assam districts, where density of the tea gardens are one of the highest in the world. |
| Acknowledgements |
| We wish to thank the participants as well as the staff and students at Assam Medical College and Hospital for their active cooperation during the course of the study. |
| Conflict of Interest |
| None declared |
| Contribution of Authors |
| The study was designed by Dr. Hemonta Kumar Dutta. Both the authors contributed substantially towards the collection, compilation and interpretation of data. |
| Funding |
| None |
References
- Suphapeetiporn K, Mahatumarat C, Rojvachiranonda N, Taecholarn C, Siriwan P, et al. (2008) Risk factors associated with the occurrence of frontoethmoidal encephalomeningocele. Eur J Paediatr Neurol 12: 102-107.
- Dutta HK, Deori P (2010) Anterior encephaloceles in children of Assamese tea workers. J Neurosurg Pediatr 5: 80-84.
- Dutta HK, Bhattacharyya NC, Sarma JN, Giriraj K (2010) Congenital malformations in Assam. J Indian Assoc Pediatr Surg 15: 53-55.
- Gupta, R. C. and D. Milatovic (2012). "Toxicity of organophosphates and carbamates." by Marrs TC. Royal Society of Chemistry, Cambridge, UK: 104-136.
- Horton MK, Rundle A, Camann DE, Boyd Barr D, Rauh VA, et al. (2011) Impact of prenatal exposure to piperonyl butoxide and permethrin on 36-month neurodevelopment. Pediatrics 127: e699-706.
- El-Helaly, M., K. Abdel-Elah, A. Haussein and H. Shalaby (2011). "Paternal occupational exposures and the risk of congenital malformations--a case-control study." Int J Occup Med Environ Health24(2): 218-227.
- Ren A, Qiu X, Jin L, Ma J, Li Z, et al. (2011) Association of selected persistent organic pollutants in the placenta with the risk of neural tube defects. Proc Natl Acad Sci U S A 108: 12770-12775.
- Desrosiers, T. A., C. C. Lawson, R. E. Meyer, D. B. Richardson, J. L. Daniels, M. A. Waters, E. van Wijngaarden, P. H. Langlois, P. A. Romitti, A. Correa, A. Olshan and S. National Birth Defects Prevention (2012). "Maternal occupational exposure to organic solvents during early pregnancy and risks of neural tube defects and orofacial clefts." Occup Environ Med69(7): 493-499.
- Vaughan DA, Cleary BJ, Murphy DJ (2014) Delivery outcomes for nulliparous women at the ext
- Flenady V, Koopmans L, Middleton P, Frøen JF, Smith GC, et al. (2011) Major risk factors for stillbirth in high-income countries: a systematic review and meta-analysis. Lancet 377: 1331-1340.
- Mashuda, F., A. Zuechner, P. L. Chalya, B. R. Kidenya and M. Manyama (2014). "Pattern and factors associated with congenital anomalies among young infants admitted at Bugando medical centre, Mwanza, Tanzania." BMC Res Notes7: 195.
- Taksande A, Vilhekar K, Chaturvedi P, Jain M (2010) Congenital malformations at birth in Central India: A rural medical college hospital based data. Indian J Hum Genet 16: 159-163.
- Grover N (2000) Congenital malformations in Shimla. Indian J Pediatr 67: 249-251.
- Shechter Y, Levy A, Wiznitzer A, Zlotnik A, Sheiner E (2010) Obstetric complications in grand and great grand multiparous women. J Matern Fetal Neonatal Med 23: 1211-1217.
- Shah PS; Knowledge Synthesis Group on Determinants of LBW/PT births (2010) Parity and low birth weight and preterm birth: a systematic review and meta-analyses. Acta Obstet Gynecol Scand 89: 862-875.
- Abu-Saad K, Fraser D (2010) Maternal nutrition and birth outcomes. Epidemiol Rev 32: 5-25.
- Steegers-Theunissen RP, Boers GH, Trijbels FJ, Finkelstein JD, Blom HJ, et al. (1994) Maternal hyperhomocysteinemia: a risk factor for neural-tube defects? Metabolism 43: 1475-1480.
- Sheridan E, Wright J, Small N, Corry PC, Oddie S, et al. (2013) Risk factors for congenital anomaly in a multiethnic birth cohort: an analysis of the Born in Bradford study. Lancet 382: 1350-1359.
Figures at a glance
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 |
Post your comment
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 13912
- [From(publication date):
April-2015 - Aug 17, 2025] - Breakdown by view type
- HTML page views : 9344
- PDF downloads : 4568
