Research Article Open Access
Ethnic Differences in Inflammatory Bowel Diseases
Souad Bouhadan* and Tom G Moreels
Antwerp University Hospital, Department of Gastroenterology & Hepatology, Wilrijkstraat 10, 2650 Edegem-Antwerp, Belgium
- *Corresponding Author:
- Souad Bouhadan
Department of Gastroenterology & Hepatology
Antwerp University Hospital, Wilrijkstraat 10
2650 Edegem-Antwerp, Belgium
Tel: +3238213324
Fax: +3238214478
E-mail: souad.bouhadan@uza.be
Received date: January 23, 2014; Accepted date: February 20, 2014; Published date: February 25, 2014
Citation: Bouhadan S, Moreels TG (2014) Ethnic Differences in Inflammatory Bowel Diseases. J Gastroint Dig Syst 4:173. doi:10.4172/2161-069X.1000173
Copyright: © 2014 Bouhadan S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
have investigated all first and second degree immigrants from our IBD patient cohort. In Antwerp – Belgium there is an important Moroccan immigrant population since the 1960s. Phenotype differences were assessed between Moroccan and Caucasian immigrants. We looked at age at diagnosis, sex, disease location and behavior (Montreal classification), extraintestinal manifestations, need for anti-TNFα treatment and surgery. Our single-center results suggest that first and second degree Moroccan immigrants with IBD suffer predominantly from Crohn’s disease with a more severe phenotype characterized by penetrating disease leading to higher rates of CD-related surgery and need for anti-TNFα treatment. In addition, extraintestinal manifestations tend to be more prevalent in the Moroccan immigrant population. Possible explanations are discussed.
Keywords
Inflammatory bowel diseases; Immunological factors; Anti-TNFα treatment
Introduction
Inflammatory bowel diseases include ulcerative colitis (UC) and Crohn’s disease (CD). The etiology of IBD is not fully understood and is influenced by environmental, genetic and immunological factors. The geographic variation of IBD is well known [1]. The highest prevalence rates are reported in North America and Northern Europe, whereas the prevalence rates are much lower in eastern European and Asian populations [2,3]. It has been shown that higher incidence rates of IBD are associated with westernization [4]. People who immigrate to westernized countries have a higher risk for developing IBD [5]. The prevalence of IBD is also different among ethnic groups of immigrant populations [6,7]. Nguyen et al. showed a higher prevalence of IBD in Non-Hispanic whites compared with Non-Hispanic blacks [8]. The same study showed a higher ratio of IBD hospitalizations and IBDrelated mortality in Non-Hispanic blacks compared with Non-Hispanic whites. This suggests a different IBD phenotype among ethnic groups.
Based on this assumption, we have investigated the clinical phenotype of CD in first and second degree Moroccan immigrants in comparison to Caucasian immigrants in the Antwerp University Hospital.
Materials and Methods
Patients in this retrospective study were selected from the continuously updated IBD cohort from the Antwerp University Hospital, which started in 2005. The cohort consists of both patients who were diagnosed with IBD within our hospital and patients who were diagnosed with IBD in other centers and referred for treatment. Patients not attending our IBD clinic for more than 2 years were considered lost to follow-up and were not included. In addition, pediatric Crohn’s disease patients (<18 years) are followed in the Pediatric department and are not included either. When selecting Moroccan patients, all first and second degree immigrants were considered. Non-Moroccan Caucasian immigrant patients are a diverse group of East-European (Bulgarian, Albanian,…) and Middle-East (Turkish, Israelites,…) immigrants.
Phenotype differences were assessed between Moroccan and Caucasian immigrants. We looked at age at diagnosis, sex, disease location and behavior, according to the Montreal classification (Table 1). We also assessed smoking habits, extra intestinal manifestations, need for anti-TNFα treatment and the need for surgery. Chi-square statistics were used for analysis using SPSS for Windows. Differences were considered statistically significant at p<0,05.
Results
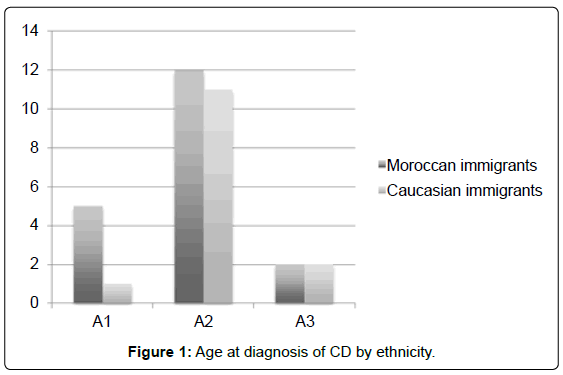
From the active IBD cohort, 50 immigrant patients were withheld. 33 cases of CD (66%) and 17 cases of UC (34%). Of the 33 CD patients, the Moroccan immigrants accounted for 58% of the patients and the Caucasian immigrants for 42% (p=0.03). The male/female ratio was inverse between the two groups: 47/53% in the Moroccan group vs 64/36% in the Caucasian group. The mean age at diagnosis was comparable in Moroccan (28 ± 12 years) and Caucasian immigrants (30±15 years), however Moroccan patients tended to be younger at diagnosis (Figure 1).
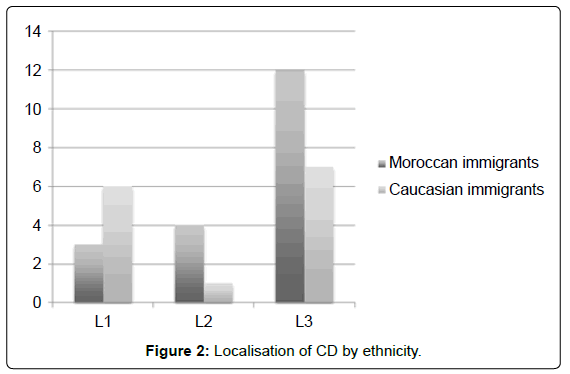
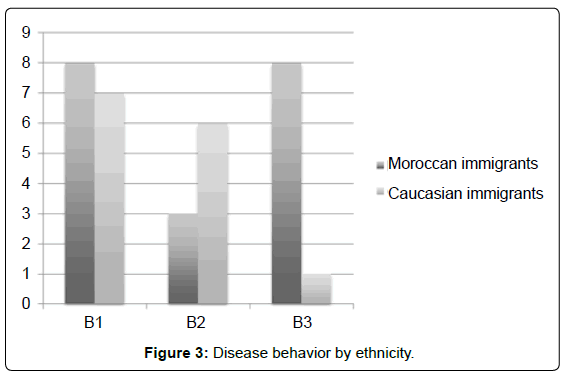
The majority of immigrant patients had ileocolonic (L3) disease (Figure 2). Moroccan patients tended to have more penetrating (B3) disease: 42% vs 7% (p=0.053) (Figure 3). The penetrating phenotype was seen in 8 out of 19 Moroccan patients. Caucasian CD patients mostly had the inflammatory phenotype (Figure 3).
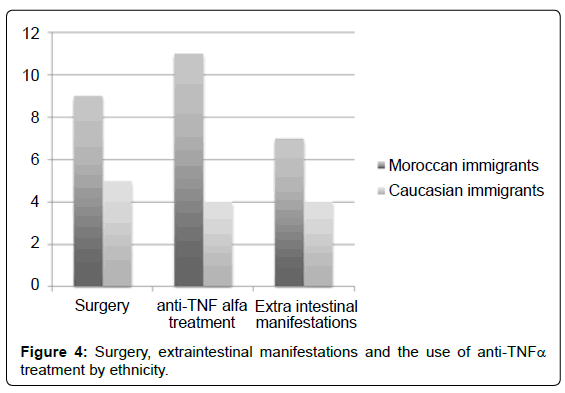
Moroccan immigrants underwent CD-related surgery more often, 47% vs 35% (p=0.530). They were also treated more often with anti-TNFα therapy, 57% vs 29% (p=0.095) and they suffered more extraintestinal manifestations, 36% vs 27% (p=0.1) (Figure 4). Although there was a tendency towards more serious disease in Moroccan CD patients, results did not reach statistical significance, possibly due to the small sample size. There were no differences in smoking habits.
Discussion
It is known that genetic and environmental factors play a role in the etiology of IBD [1]. The incidence of IBD varies among different regions [1]. Emigration to industrialized countries creates a higher risk of developing IBD [5,9].
In this study we analyzed a multiethnic IBD population in the Antwerp University Hospital.
Belgium comprises a large population of Moroccans. In 2010 nearly 82 000 inhabitants had the Moroccan nationality on a total of nearly 11 million [10]. There is no information on the prevalence of IBD in Morocco. An epidemiological study on the incidence of IBD in Brussels showed the same incidence of CD among Moroccan immigrants compared to the native population [11]. Joossens et al. investigated a large Moroccan family in which the father developed CD after moving from Morocco to Belgium [12]. Four of his eight children also developed CD. They found no explanation by the known genetic and environmental risk factors.
We report a higher prevalence of CD in Moroccan patients compared to Caucasian immigrants in our active IBD cohort. Moreover, Moroccan CD patients tend to have more severe disease, illustrated by their younger age at diagnosis, more penetrating disease and more CD-related surgery, use of anti-TNFα treatment and extraintestinal manifestations. Several hypotheses can be put forward to explain these ethnic differences in IBD.
Genetic differences may account for phenotypic differences in CD. However, large-scale genetic consortium research in IBD has not shown specific genetic defects in Moroccan IBD patients [12]. Second, although in Belgium social security is available for all tax payers, Moroccans may have suboptimal access to healthcare with delayed diagnosis and treatment. Cultural and socioeconomic differences may play a role. Third, the Antwerp University Hospital is a tertiary referral center concentrating more severe CD patients. The lower prevalence of mild disease could be explained by the fact that patients with less severe disease are not referred to our center. However, this also accounts for Caucasian immigrants with CD. There is no reason to assume that Moroccan patients have a different referral behavior as compared to non-Moroccan immigrants or autochtone Crohn’s disease patients. Otherwise it is not impossible that the Moroccans have a more severe course of CD. Malaty et al. found that the rate of fistulizing CD among Hispanics was double that of Black and Caucasian Americans [6]. Our results are preliminary and a larger multicenter study in Antwerp is planned in order to confirm our findings and to determine possible underlying explanations. Future research will focus upon larger immigrant population cohorts, with more differentiated ethnicities to be compared with each other and with native Belgian IBD patient cohorts.
We conclude that these single-center results suggest that first- and second- degree Moroccan immigrants with IBD predominantly suffer from CD with a more severe phenotype characterized by penetrating disease leading to higher rates of CD-related surgery and need for anti-TNFα treatment. In addition, extraintestinal manifestations tend to be more prevalent in the Moroccan immigrant population. Further study is needed to confirm these findings and to explain why Moroccan immigrants seem to have more severe CD.
References
- Ng SC, Bernstein CN, Vatn MH, Lakatos PL, Loftus EV Jr, et al. (2013) Geographical variability and environmental risk factors in inflammatory bowel disease. Gut 62: 630-649.
- Yang SK, Yun S, Kim JH, Park JY, Kim HY, et al. (2008) Epidemiology of inflammatory bowel disease in the Songpa-Kangdong district, Seoul, Korea, 1986-2005: a KASID study. Inflamm Bowel Dis 14: 542-549.
- Shivananda S, Lennard-Jones J, Logan R, Fear N, Price A, et al. (1996) Incidence of inflammatory bowel disease across Europe: is there a difference between north and south? Results of the European Collaborative Study on Inflammatory Bowel Disease (EC-IBD) Gut 39: 690–697.
- Carr I, Mayberry JF (1999) The effects of migration on ulcerative colitis: a three-year prospective study among Europeans and first- and second- generation South Asians in Leicester (1991-1994). Am J Gastroenterol 94: 2918-2922.
- Barreiro-de Acosta M, Alvarez Castro A, Souto R, Iglesias M, Lorenzo A, et al. (2011) Emigration to western industrialized countries: A risk factor for developing inflammatory bowel disease. J Crohns Colitis 5: 566-569.
- Malaty HM, Hou JK, Thirumurthi S (2010) Epidemiology of inflammatory bowel disease among an indigent multi-ethnic population in the United States. ClinExpGastroenterol 3: 165-170.
- Mangat BK, Evaschen C, Lee T, Yoshida EM, Salh B (2011) Ethnic variation in the annual rates of adult inflammatory bowel disease in hospitalized patients in Vancouver, British Columbia. Can J Gastroenterol 25: 73-77.
- Nguyen GC, Chong CA, Chong RY (2013) National estimates of the burden of inflammatory bowel disease among racial and ethnic groups in the United States. J Crohns Colitis.
- Satsangi J, Silverberg MS, Vermeire S, Colombel JF (2006) The Montreal classification of inflammatory bowel disease: controversies, consensus, and implications. Gut 55: 749-753.
- A statistical overview of the Belgian population.
- Van Gossum A, Adler M, De Reuck M, Devis G, Fiasse R, et al. (1996) Epidemiology of inflammatory bowel disease in Brussels' area (1992-1993). ActaGastroenterolBelg 59: 7-9.
- Joossens M, Simoens M, Vermeire S, Bossuyt X, Geboes K, et al. (2007) Contribution of genetic and environmental factors in the pathogenesis of Croh n's disease in a large family with multiple cases. Inflamm Bowel Dis 13: 580-584.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 14445
- [From(publication date):
April-2014 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 9827
- PDF downloads : 4618