Evaluation of Platelet Parameters as Prognostic Analysis in Cardiac Intensive Care Unit Patients
Received: 11-Jan-2017 / Accepted Date: 06-Mar-2017 / Published Date: 12-Mar-2017
Abstract
Objective: Platelet activation and consumption are common in critically ill patients and are associated with poorer prognosis. Inflammatory and thrombotic conditions may alter platelet size, which can be detected on routine blood cell analysis by evaluation of mean platelet volume. The aim of the present study was to investigate the evaluation of platelet parameters as a predictor of all-cause mortality in cardiac intensive care unit (ICU) patients. Methods: Platelet count and mean platelet volume were measured daily in cardiac ICU and were classified in three categories of thrombocytopenia, according to the average value of platelet count during hospitalization: mild (100-149 X 109/L), moderate (50-99 X 109/L) and severe (hematological disease, who have had previous use of steroids or chemotherapy, those that were readmitted after hospital discharge and patients who died in the first 24 hrs after admission. A correlation analysis was performed to identify independent predictors of mortality. Results: We included 165 patients (61 ± 16 years, 55.8% male, average length of stay in ICU was 10 ± 10 days). In total, 42 (25.4%) out of the 165 patients showed platelet count
Keywords: Cardiac intensive care unit; Daily platelet parameters; Mean platelet volume (MPV); Platelet count; Sequential organ failure assessment (SOFA); Acute physiology and chronic health evaluation II (APACHE II); Mortality
6560Abbreviations
ICU: Intensive Care Unit; APACHE II: Acute Physiology and Chronic Health Evaluation II; SOFA: Sequential Organ Failure Assessment; PLT: Platelet Count; MPV: Mean Platelet Volume; PDW: Platelet Distribution Width; P-LCR: Platelet Large Cells Ratio; EDTA: Ethylene Diamine Tetra Acetic Acid
Introduction
Thrombocytopenia is the most common hemostatic disorder in critically ill patients [1]. Thrombocytopenia is defined as a platelet count of <150,000/μL or a decrement of >50% from a previous measurement [2]. The causes of thrombocytopenia are numerous and varied, but basically they result from three processes: 1. Deficient platelet production, 2. Accelerated platelet destruction or increased consumption, 3. Abnormal distribution or dilution of platelets in the organism [3]. The incident thrombocytopenia (developing during the course of ICU stay) occurred in 13.0% to 44.1% of patients [4].
Most patients are exposed to heparin during their stay in the ICU and heparin-induced thrombocytopenia is often suspected, although rarely confirmed [5]. Other factors that have been associated with the development of thrombocytopenia in studies with high illness severity, sepsis and organ dysfunction [2]. The cause of a low platelet count in ICU may be difficult to determine and is often multifactorial [6].
Studies show that thrombocytopenia is associated with decreased survival in patients in ICU [7] and the decline in platelet count (PLT) during hospitalization in the ICU provides prognostic information [8].
Platelet parameters can be monitored through semi-invasive procedures for long periods. They help in diagnosis, early stage of disease, monitoring the progression and determining therapeutic results. The parameters include: PLT, mean platelet volume (MPV), platelet distribution width (PDW) and platelet large cells ratio (P-LCR) [9]. Among platelet indices, MPV is a potentially useful marker of platelet activity. The clinical importance of determining the MPV is related to the presence of increased platelet aggregation. The MPV has been linked to patients with coronary artery disease and severity of coronary atherosclerosis [10].
Prior studies have also demonstrated that platelet parameters are a prognostic indicator in general ICU, few data on patient admitted in the ICU acute cardiovascular disease exist. Therefore, the aim of the present study was to investigate the evaluation of platelet parameters as a predictor of all-cause mortality in ICU of the cardiac emergency unit to provide information that will allow anticipation of possible adverse outcomes.
Materials and Methods
Study Population and Protocol
An observational cohort, prospective and analytical study involving patients admitted to the cardiac ICU, with 10 beds, of the Cardiologic Emergency Unit (PROCAPE), a specialized tertiary care cardiovascular teaching hospital with 250 beds. The experimental design of this study has been approved by the Research Ethics Committee under number CAAE: 08412412.20000.5192, in Brazil Platform. All patients included in the study signed a free and informed consent form.
The study included patients admitted to the cardiac ICU of PROCAPE from May/2013 through January/2014 with clinical and/or surgical diseases. We excluded patients younger than 18 years, pregnant women, with cancer or hematological disease, who have had previous use of steroids or chemotherapy, those that were readmitted after hospital discharge and patients who died in the first 24 hrs after admission.
Demographic and clinical information were gathered from medical charts of patients, including age, period of observation, admission diagnosis in the cardiac ICU, severity of illness measured by APACHE II score [11], organic dysfunctions evaluated by the Sequential Organ Failure Assessment score (SOFA) [12] and laboratory data including platelet count and MPV. Patients were followed until hospital outcome,noting at this moment the length of stay in the cardiac ICU and in the hospital and the outcome (death or survival).
After the first 24 h of admission into the cardiac ICU, all patients had APACHE II and SOFA calculated. The SOFA score was also calculated on the 2nd and 3rd days of hospitalization in a cardiac ICU and later of 48/48 h until discharge from the cardiac ICU. Patients were classified in coronary (acute or chronic) [13,14] or not coronary (heart valve diseases, peri-miocardiopathies, cardiac arrhythmias). Patients were also classified into infected (sepsis) and uninfected obeying the criteria for systemic inflammatory response syndrome, plus an infectious focus documented or presumed (antibiotic use) [15].
Laboratory tests
PLT and MPV were performed by the automated method using the Sysmex XE-2100 device (Sysmex Europe GmbH, Norderstedt, Germany). Daily venous blood samples were collected in tubes containing anticoagulant ethylene diamine tetra acetic acid (EDTA), before 9 am until hospital discharge. Three categories of thrombocytopenia were defined: mild (100-149 X 109/L), moderate (50-99 X 109/L) and severe (<50 X 109/L) [1]. Each patient was classified in categories of thrombocytopenia using average daily PLT during the days of hospitalization.
Statistical analysis
Descriptive analysis was presented through absolute and relative frequencies of the main categorical variables. Quantitative analyses such as mean and standard deviations and comparison between groups were performed using chi-square tests (or Fisher's exact test when necessary) and numeric data were analyzed with t-Student tests. Kruskal-Wallis test was used for data with non-normal distribution. Hazard ratio between the variables platelet counts and mortality was calculated, and it was categorized through pre-defined cutoff point, diagnosis and outcome with respective 95% confidence intervals. Statistical significance level of p<0.05 was adopted. For the statistical analysis we used the SPSS (Statistical Program for Social Sciences) version 10.0 for Windows (SPPS Inc. Chicago, I11, USA).
Results
The study included 165 patients from a total of 212 (47 patients did not participate in the study due to the exclusion criteria: Neoplasia: 28, Death <24 hrs: 7, Chronic corticoid: 8, Refused: 2, Aged <18 years: 1, readmission: The mean age of these patients was 61 ± 16 years, 55.8% were male. The admission diagnosis in the ICU was coronary (48.8%) and non-coronary (51.2%), the majority (82.4%) coming mainly from the Cardiac Emergency (Table 1).
| Characteristics | Normal (n = 123) |
Mild (n = 24) |
Moderate (n = 15) |
Severe (n = 3) |
Total (n = 165) |
P |
|---|---|---|---|---|---|---|
| Sex | ||||||
| Male | 71 (57.7) | 12 (50.0) | 7 (46.7) | 2 (66.7) | 92 (55.8) | |
| Female | 52 (42.3) | 12 (50.0) | 8 (53.3) | 1 (33.3) | 73 (44.2) | .286 |
| Age (years) | 61 (±17) | 62 (±16) | 60 (±16) | 56 (±25) | 61 (±16) | .945 |
| Skin color | ||||||
| White | 49 (39.8) | 7 (29.2) | 6 (40.0) | 1 (33.3) | 63 (38.2) | |
| Black | 21 (17.1) | 3 (12.5) | 4 (26.7) | 0 (00.0) | 28 (17.0) | |
| Brown | 53 (43.1) | 14 (58.3) | 5 (33.3) | 2 (66.7) | 74 (44.8) | .714 |
| Origin | ||||||
| Emergency | 105 (85.4) | 17 (70.8) | 12 (80.0) | 2 (66.7) | 136 (82.4) | |
| Infirmary | 14 (11.4) | 5 (20.8) | 2 (13.3) | 1 (33.3) | 22 (13.3) | |
| TSRU | 4 (3.3) | 2 (8.3) | 1 (6.7) | 0 (00.0) | 7 (4.2) | .299 |
| Time of stay in the ICU (days) | 11 ± 11 | 7 ± 7 | 10 ± 9 | 3 ± 3 | 10 ± 10 | .303 |
| Median time of stay in the ICU (days) | 7 | 6 | 8 | 2 | 7 | .140 |
| Time of stay in the hospital (days) | 31 ± 30 | 32 ± 31 | 19 ± 14 | 8 ± 8 | 30 ± 29 | .575 |
| Median time of stay in the ICU (days) | 19 | 22 | 15 | 8 | 19 | .358 |
| Mortality | ||||||
| ICU | 45 (36.6) | 9 (37.5) | 10 (66.7) | 1 (33.3) | 65 (39.4) | .146 |
| Hospital | 14 (17.9) | 3 (20.0) | 2 (40.0) | 1 (50.0) | 20 (20.0) | .265 |
| APACHE II | 29.9 ± 9.5 | 22.0 ± 9.7 | 22.4 ± 8.5 | 33.7 ± 9.6 | 21.6 ± 9.5 | .131 |
| Median APACHE II | 21.0 | 21.0 | 21.0 | 32.0 | 21.0 | .225 |
| APACHE II score | ||||||
| < 25 points | 78 (63.4) | 14 (58.3) | 10 (66.7) | 0 (00.0) | 102 (61.8) | |
| ≥ 25 points | 45 (36.6) | 10 (41.7) | 5 (33.3) | 3 (100.0) | 63 (38.2) | .186 |
| SOFA | 4.5 ± 3.4 | 6.7 ± 3.9 | 9.6 ± 3.9 | 14.7 ± 5.3 | 5.4 ± 4.1 | <.001 |
| Median SOFA | 3.7 | 6.0 | 10.0 | 17.5 | 4.5 | <.001 |
| SOFA score | ||||||
| < 7 points | 97 (78.9) | 13 (54.2) | 3 (20.0) | 0 (00.0) | 13 (68.5) | |
| ≥ 7 points | 26 (21.1) | 11 (45.8) | 12 (80.0) | 3 (100.0) | 52 (31.5) | <.001 |
| VPM | 11.05 ± 0.99 | 10.93 ± 2.53 | 12.04 ± 0.68 | 12.10 ± 0.99 | 11.11 ± 1.34 | .085 |
| Median VPM | 11.03 | 11.34 | 11.94 | 12.10 | 11.12 | .002 |
| Sepsis | ||||||
| Yes | 67 (54.5) | 13 (54.2) | 9 (60.0) | 2 (66.7) | 91 (55.2) | |
| No | 56 (45.5) | 11 (45.8) | 6 (40.0) | 1 (33.3) | 74 (44.8) | .970 |
| Coronary patient | ||||||
| Yes | 65 (53.3) | 11 (45.8) | 3 (20.0) | 1 (33.3) | 80 (48.8) | |
| No | 57 (46.7) | 13 (54.2) | 12 (80.0) | 2 (66.7) | 84 (51.2) | .074 |
| Sepsis/Coronary | ||||||
| With sepsis and coronary | 26 (21.3) | 4 (16.7) | 1 (06.7) | 0 (00.0) | 31 (18.9) | |
| With sepsis and non-coronary | 40 (32.8) | 9 (37.5) | 8 (53.3) | 2 (66.7) | 59 (36.0) | |
| Without sepsis and coronary | 39 (32.0) | 7 (29.2) | 2 (13.3) | 1 (33.3) | 49 (29.9) | |
| Without sepsis and non-coronary | 17 (13.9) | 4 (16.7) | 4 (26.7) | 0 (00.0) | 25 (15.2) | .561 |
Table 1: Demographic and clinical characteristics of patients in intensive care in accordance with the PLT.
On the first day of hospitalization in the cardiac ICU, the mean total score of APACHE II was 21.6 ± 9.5 and the SOFA score was 5.4 ± 4.1, reflecting high severity of disease and the presence of severe organ dysfunctions in the study population. The average length of stay of the patients in the cardiac ICU was 10 ± 10 days and in the hospital, 30 ± 29 days. The total mortality was 39.4%, being higher in the cardiac ICU (Table 1).
The total average platelet count in the cardiac ICU admission was 160 ± 88 X 109/L and the total median value of MPV was 11.12 fl, being higher in patients with moderate and severe thrombocytopenia (11.94 and 12.10; P = 0.002) (Table 1).
In total, 42 out of 165 patients (25.4%) had platelet count <150 X 109/L during hospitalization. Mild, moderate and severe thrombocytopenia developed in 24 (14.5%) 15 (9.1%) and 3 (1.8%) patients, respectively. Thrombocytopenia was not associated with sepsis, length of stay in the hospital or in the cardiac ICU (Table 1).
Comparing the mean APACHE II scores and platelet count levels, an average value of APACHE II 33.7 ± 9.6 was observed among the severe thrombocytopenia group, but no significant differences were detected (P=0.131). In the analysis of SOFA score in relation to the profile of platelet count, the difference between means was statistically significant for patients with moderate and severe thrombocytopenia (P <0.001) (Table 1).
A proportionally inverse relationship between mortality and platelet count was observed, with statistical significance for moderate thrombocytopenia (HR 2.303; IC 95% 1.148–4.619; P=0.019), even with higher hazard ratio for severe thrombocytopenia group (HR 3.806; IC 95% 0.514–28.204) (Table 2).
| Number of platelets (X 109/L) | HR | IC 95% | P Value |
|---|---|---|---|
| None (≥ 150) | 1.000 | - | - |
| Mild (100 - 149) | 1.621 | 0.782 – 3.360 | 0.194 |
| Moderate (50 - 99) | 2.303 | 1.148 – 4.619 | 0.019 |
| Severe (< 50) | 3.806 | 0.514 – 28.204 | 0.191 |
Abbreviations: HR, hazard ratio; IC, Confidence interval.
Table 2: Thrombocytopenia and mortality.
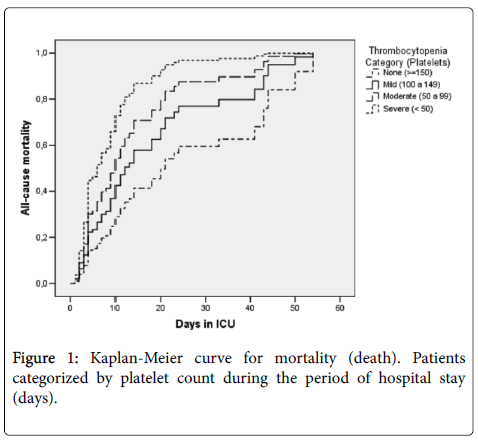
Figure 1 shows the Kaplan-Meier curve for different levels of thrombocytopenia categories, estimating that the more severe the thrombocytopenia, moderate to severe, the length of stay and mortality have an inverse behavior.
In the analysis with patients with thrombocytopenia, it was observed that increased PLT and drop of MPV was related to discharge outcome, in the case of patients hospitalized in the cardiac ICU (Table 3). The same behavior was found among patients admitted to the hospital ward after discharge of cardiac ICU (Table 4).
| Variables | Evolution ICU | Total | ||||
|---|---|---|---|---|---|---|
| Discharge | Death | |||||
| N | % | N | % | N | % | |
| Evaluation of PLT | ||||||
| Increase | 14 | 73.7% | 6 | 37.5% | 20 | 57.1% |
| Neutral | 0 | 0.0% | 1 | 6.3% | 1 | 2.9% |
| Decrease | 5 | 26.3% | 9 | 56.3% | 14 | 40.0% |
| Evaluation of MPV | ||||||
| Increase | 4 | 22.2% | 9 | 69.2% | 13 | 41.9% |
| Neutral | 2 | 11.1% | 0 | 0.0% | 2 | 6.5% |
| Decrease | 12 | 66.7% | 4 | 30.8% | 16 | 51.6% |
Abbreviations: PLT, Platelet Count; MPV, Mean Platelet Volume; ICU, Intensive Care Unit; Neutral: Constant values through period of hospital stay.
Table 3: Evaluation of PLT and MPV in patients with thrombocytopenia at the cardiac ICU.
| Variables | Hospital evolution | Total | ||||
|---|---|---|---|---|---|---|
| Discharge | Death | |||||
| n | % | n | % | n | % | |
| Evaluation of PLT | ||||||
| Increase | 11 | 78.6% | 3 | 60.0% | 14 | 73.7% |
| Decrease | 3 | 21.4% | 2 | 40.0% | 5 | 26.3% |
| Evaluation of MPV | ||||||
| Increase | 4 | 30.8% | 0 | 0.0% | 4 | 22.2% |
| Neutral | 2 | 15.4% | 0 | 0.0% | 2 | 11.1% |
| Decrease | 7 | 53.8% | 5 | 100.0% | 12 | 66.7% |
Abbreviations: PLT, Platelet Count; MPV, Mean Platelet Volume; Neutral: Constant values through period of hospital stay.
Table 4: Evaluation of PLT and MPV in patients with hospital thrombocytopenia.
Discussion
The main finding of this study was that the daily quantification of PLT and MPV are important to the prognosis in patients cardiac ICU. We demonstrated a positive association between thrombocytopenia and high level of MPV with prognosis, using gravity as parameters the APACHE II and SOFA scores in patients admitted to the cardiac ICU. In addition, our study showed that decrease of PLT and increase in the level of MPV after admission in cardiac ICU is associated with higher mortality, suggesting that PLT and MPV should be daily quantified.
Thrombocytopenia is common in ICU patients, on admission or during their stay in ICU [8]. In our study, the prevalence of thrombocytopenia was 25.4%. The incidence of mild (platelet count <150 X 109/L), moderate (50-99 X 109/L) and severe (<50 X 109/L) thrombocytopenia were 14.5%, 9.1% and 1.8%, respectively. In a study conducted in a medical-surgical ICU, the prevalence of thrombocytopenia was 26.2% and the incidence of mild, moderate and severe thrombocytopenia was 15.3%, 5.1% and 1.6%, respectively [1]. The cause of thrombocytopenia in critically ill patients can be difficult to determine and usually has a multifactorial origin. Basically, thrombocytopenia is incurred by lower production, increased consumption and destruction or sequestration of platelets [16]. In our study, the diagnosis of coronary artery disease upon admission to the ICU or sepsis detection did not influence significantly the development of thrombocytopenia.
Regarding the relationship between thrombocytopenia and mortality, in the hospital and in the ICU, it was observed significant difference in patients with moderate thrombocytopenia (RR 2,303; IC 95% 1,148 - 4,619; P=0.019), demonstrating greater risk of death, even the hazard ratio for patients with severe thrombocytopenia being higher (RR 3,806; IC 95% 0,514-28,204; p=0.191). Williamson et al. [1] found that mortality in the hospital and in the ICU is associated with moderate and severe thrombocytopenia. Boechat et al. [17] found that thrombocytopenia and temporal trends with a decrease >50% or not recovery is a poor prognosis in the group of septic patients.
While associating thrombocytopenia with the prognostic score for admission, median APACHE II, it was observed that the greater the severity of the patient on admission, the higher the incidence of severe thrombocytopenia, however, without statistically significant difference (P=0.225), similar results were obtained by Boechat et al. [17] for septic patients. When associating PLT and MPV with SOFA score, a statistically significant correlation (P<.001) was observed, indicating a relationship between organic dysfunction, thrombocytopenia and median increased MPV. To Vanderschueren et al. [6], thrombocytopenia is more than just one of the causes of death in the ICU, it is a marker of risk, regardless of disease severity or organ dysfunction number, reflecting a serious breakdown in homeostasis.
MPV is in evidence in literature for being a variable that represents the size and platelet activity and thrombocytes are involved in coronary ischemic events. Platelets with high MPV are metabolically and enzymatically more active and secrete more mediators [18]. These mediators may contribute to inflammation and atherogenesis, which may explain an association between MPV and severity of coronary atherosclerosis [19]. In our study, the median value of the MPV was 11.12 fL, being higher in patients with moderate and severe thrombocytopenia, 11.94 fL and 12.10 fL, respectively (P=.002). Slavka et al. [20] observed that patients with MPV ≥ 11.01 fL are at higher risk of death from ischemic heart disease, with risk ratios comparable to those reported in cases of obesity or smoking. In our study population, thrombocytopenic patients on admission that presented an increase of PLT and decrease on the level of MPV during the period of hospitalization were associated with discharge outcome.
Finally, the PLT and MPV are performed through methods that do not require advanced and expensive technology. Instead, they are performed through simple, reliable and economical methods. Thus, we suggest that PLT and MPV must be investigated in the daily assessment of the patient as important prognostic markers in critically ill patients. However, the use of measurement of platelet parameters composed of PLT, MPV, PDW, P-LCR may be more sensitive in the prognostic evaluation of cardiac patients.
Study Limitations
The main limitation of this study was that this study did not investigate the underlying mechanisms of thrombocytopenia in critically ill patients that can be associated with the presence of disseminated intravascular coagulation, medications or other causes. Furthermore, the non-separation of coronary patients between acute and chronic may be a confounding bias, especially in view of MPV.
We also think that probably there was no significant association between mortality in severe thrombocytopenia group due to the sample size in this population. Also, the platelet count is part of the SOFA score, but not the MPV, which could be a bias in the interpretation of the data.
Conclusion
Platelet parameter, including MPV in this study, is an important prognostic tool in the daily follow-up of patients admitted to a cardiac ICU. However, we suggest further studies with a larger sample of patients in order to rule out potential confounding factors.
Acknowledgment
We would like to thank Paulo Fernando Leite Filho for the computer system and the whole team of the 1st Coronary Unit and the Pernambuco Emergency Laboratory, Brazil.
References
- Williamson DR, Albert M, Heels-Ansdell D, Arnold DM, Lauzier F, et al. (2013) Thrombocytopenia in critically III patients receiving thromboprophylaxis: frequency, risk factors and outcomes. Chest 144: 1207-1215.
- Wang HL, Aguilera C, Knopf KB, Chen TMB, Maslove DM, et al. (2013) Thrombocytopenia in the intensive care unit. J of Intensive Care Unit 28: 268-280.
- Wittels EG, Siegel RD, Mazur EM (1990) Thrombocytopenia in the intensive care unit setting. J of Intensive Care Med 5: 224-240.
- Hui P, Cook DJ, Lim W, Fraser GA, Arnold DM, et al. (2011) The frequency and clinical significance of thrombocytopenia complicating critical illness: a systematic review. Chest 139: 271-278.
- Shalansky SJ, Verma AK, Levine M, Spinelli JJ, Dodek PM, et al. (2002) Risk markers for thrombocytopenia in critically ill patients: a prospective analysis. Pharmacotherapy 22: 803-813.
- Vanderschueren S, De Weerdt A, Malbrain M, VankersschaeverD, Frans E, et al. (2000) Thrombocytopenia and prognosis in intensive care. Crit Care Med 28: 1871-1876.
- Stephan F, Hollande J, Richard O, Cheffi A, Maier-Redelsperger M, et al. (1999) Thrombocytopenia in a surgical ICU. Chest 115: 1363-1370.
- Moreau D, Timsit JF, Vesin A, Garrouste-Orgeas M, de Lassence A, et al. (2007) Platelet count decline an early prognostic marker in critically III patients with prolonged ICU stays. Chest 131: 1735-1741.
- Cetin M, Bakirci EM, Baysal E, Tasolar H, Balli M, et al. (2014) Increased platelet distribution width is associated with ST-segment elevation myocardial infarction and thrombolysis failure. Angiology 65: 737-743.
- Murat SN, Duran M, Kalay N, Gunebakmaz O, Akpek M, et al. (2013) Relation between mean platelet volume and severity of atherosclerosis in patients with acute coronary syndromes. Angiology 64: 131-136.
- Knaus WA, Draper EA, Wagner DP, Zimmerman JE. (1985) APACHE II: a severity of disease classification system. Crit Care Med 13: 818-829.
- Vincent JL, De Mendonça A, Cantraine F, Moreno R, Takala J, et al. (1998) Use of the SOFA score to assess the incidence of organ dysfunction/failure in intensive care units: results of a multicenter, prospective study.Crit Care Med 26: 1793-1800.
- Hamm CW, Bassand JP, Agewall S, Bax J, Boersma E, et al. (2011) ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation: The Task Force for the management of acute coronary syndromes (ACS) in patients presenting without persistente ST- segment elevation of the European Society of Cardiology (ESC). Eur Heart J 32: 2999-3054.
- Fraker TD, Fihn SD, Gibbons RJ, Abrams J, Chatterjee K, et al. (2007) Chronic angina focused update of the ACC/AHA 2002 Guidelines for the Management of patients with Chronic Stable Angina: a Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines Writing Group to Develop the Focused Update of the 2002 Guidelines for the Management of Patients with Chronic Stable Angina. Circulation 116: 2762-2772.
- Dellinger RP, Levy MM, Rhodes A, Annane D, Gerlach H, et al. (2013) Surviving Sepsis Campaign: Internacional Guidelines for Management of Severe Sepsis and Septic Shock 2012. Intensive Care Med 39: 165-228.
- Drews RE, Weinberger SE (2000) Thrombocytopenic disorders in critically ill patients. Am J RespirCrit Care Med 162: 347-351.
- Boechart TO, Silveira MFBB, Faviere W, Macedo GL (2012) Thrombocitopenia in sepsis: an important prognosis factor. Rev Bras TerIntensiva 24: 35-42.
- Gawaz M, Langer H, May AE (2005) Platelets in inflammation and atherogenesis. J Clin Invest 115: 3378-3384.
- Gasparyan AY, Ayvazyan L, Mikhailidis DP, Kitas GO (2011) Mean Platelet volume a link between thrombosis and inflammation?. Curr Pharm Des 17: 47-58.
- Slavka G, Perkmann T, Haslacher H, Greisenegger S, Marsik C, et al. (2011) Mean platelet volume may represent a predictive parameter for overall vascular mortality and ischemic heart disease. Arterioscler Thromb Vasc Biol 31: 1215-1218.
Citation: Júnior JG de MM, Torres D de OC, Silva MCFC da, Santos ACO dos, Correia RM, et al. (2017) Evaluation of Platelet Parameters as Prognostic Analysis in Cardiac Intensive Care Unit Patients. Atheroscler open access 2: 106.
Copyright: © 2017 Junior JG de MM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Open Access Journals
Article Usage
- Total views: 4049
- [From(publication date): 0-2017 - Jul 01, 2025]
- Breakdown by view type
- HTML page views: 3126
- PDF downloads: 923