Case Report Open Access
Extraskeletal Osteochondroma of the Heel: A Case Report
Bilgin Y, Karademir G*, Anarat B and Salduz AIstanbul University, Istanbul Faculty of Medicine, Istanbul, Turkey.
- *Corresponding Author:
- Dr. Karademir G
Istanbul University, Istanbul Faculty of Medicine
Istanbul, Turkey
Tel: 269724111
E-mail: dr@gokhankarademir.com
Received Date: October 08, 2015; Accepted Date: October 24, 2015; Published Date: November 02, 2015
Citation: Bilgin Y, Karademir G, Anarat B, Salduz A (2015) Extraskeletal Osteochondroma of the Heel: A Case Report. J Orthop Oncol 1:101. doi:10.4172/2472-016X.1000101
Copyright: © 2015 Bilgin Y, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Orthopedic Oncology
Abstract
Osteochondroma is the most common benign bone tumor and usually occurs in the metaphyseal region of the long bones around the knee. This is acartilage-capped bony tumor, which out growths on the surface of the bone. Extraskeletal osteochondroma is a variant of extraskeletal chondromas that are uncommon soft-tissue cartilaginous tumors. This report describes thecase of a 56-year-old woman with an extraskeletal osteochondroma of the heel.
Keywords
Extraskeletal osteochondroma; Soft-tissue chondroma; Foot; Heel
Introduction
Osteochondroma are present approximately 10–15% of all bone tumors [1]. Usually represent as cartilage capped tumor around the knee such as proximal tibia and distal femur. Extraskeletal osteochondromas also seen rarely. Peak occurrence is during the 3rd and 6th decades [2]. Extraskeletal osteochondromas are often benign tumors and local excision is known as the Standard treatment if tumor is symptomatic [3]. With only few data on literature, treatment choice may depends on the risk of malignant transformation. This article presents a case of an extraskeletal osteochondroma arising of heel.
Case Report
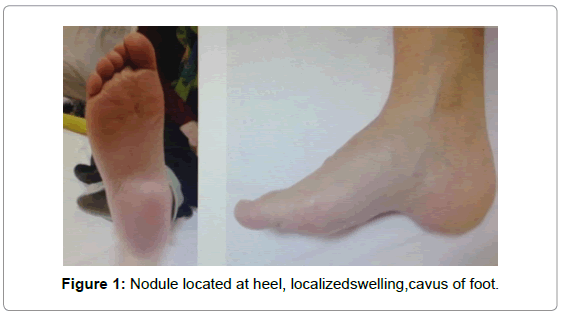
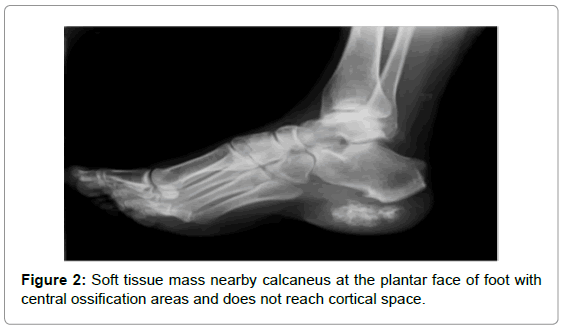
A 56-year-old woman was admitted with gradually increasing right heel pain, recent swelling and difficulty walking. Patient’s pain had been present for 5 years and have increased over the last 3 months. She had been treated with physical therapy with a diagnosis of calcaneal spurs for a year. Clinical examination revealed a nodule measuring 5×2 cm, localized swelling in the heel, cavus of foot, and tenderness to palpation located on the heel of right foot (Figure 1). X-ray showed soft tissue mass near by calcaneus at the plantar face of foot (Figure 2), which has central ossification are asand does not reach cortical space. Routine laboratory tests were within normal limits. Magnetic resonance imaging (MRI) showed a mass lesion has seen approximately 46×23 mm hypointense (centrallyisointense) in T1 weighted images and heterogeneous hiperintense in T2 weighted images.
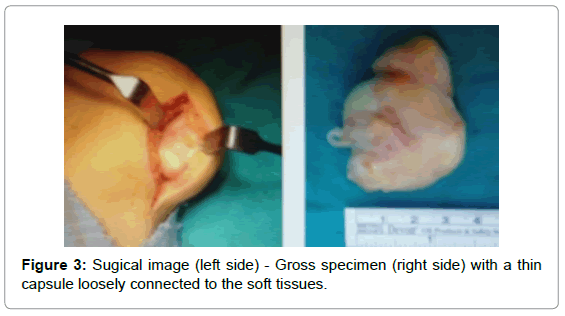
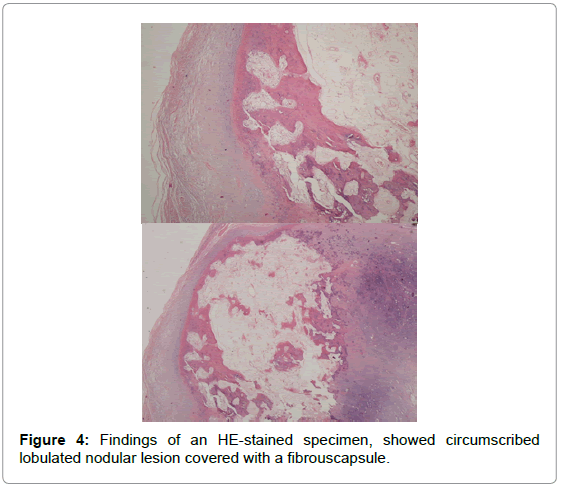
Excisional biopsy planned for this mass on plantar face with prediagnosis of ostechondroma and heterotopic ossification. The tumor was completely resected under general anesthesia (Figure 3), revealing a yellowish mass with a thin capsule loosely connected to the soft tissues around heel but without any adhesion to the bone. Histologic examination showed benign osteochondromatous lesion, circumscribed lobulated nodular lesion covered with a fibrouscapsule (Figure 4). The layers from outside to inside; Fibrous capsule, mature hyaline cartilage, central ossification area. After removal of mass, patient relieved. Recurrence didn’thappen 18 months followup.
Discussion
Extraskeletal osteochondromas, are slow growing solitary nodules of hyaline cartilage seen rarely [4]. It presents as cartilage covered bone mass in soft tissue. Hands, spesifically fingers is the most common site for this tumor, foot comes the second. Also researches showed widerange of locations for extraskeletal osteochondromas [3] in 2013 [4]. In 2010 reported similar cases in the plantar aspect of foot [5].
in 2008 reported single case of osteochondroma in infrapatellar fat pad [6]. In 2012 showed one in elbow joint [7]. In 2010 reported an extraskeletal osteochondroma near hip joint in a pediatric patient [8]. In 2006 reported a ostechondroma in thenape of the neck.
There is couple theories for developement of heel pad osteochondromas, some researchers come up with idea that it might develops as metaplasia of plantaraponeurosis [4,8]. Also, Singh et al. said it can form as seperation from calcaneal osteochondroma in one of their case report [4].
An extraskeletal osteochondroma often presents with central calcification or ossification are as that are not reaching cortex of bone in radiologic images. Other cases in literature shows MRI is the best for seeing the borders of the mass clearly, which is important for distinguish it from malignant tumors. On MRI, extraskeletal osteochondrom aappears as intermediate intensity on T1-weighted images, whereas it appears as a high signal intensity on T2- weighted images [9].
The differential diagnosis includes myositis ossificans, tumoral calcinosis, extraskeletal osteosarcoma, synovial chondromatosis, soft tissue osteochondromas and extraskeletal osteosarcoma, pseudomalignant osseous tumor and an ossifying fibromyxoid tumor [10]. Mature ossification is usually associated with benign lesion.
There is 1-2% malignant transformation risk in classic osteochondromas [11,12]. Similar to our case report, there was no malignant transformation or recurrence at this sporadic cases [3]. In 2013 reported lesion with 6×3×3 cm size, no recurrence had developed by 5 month follow-up [13]. In 2013 reported a large extraskeletal osteochondroma of heel with 10×8 cm size, followed up by 30 months and stil no recurrence or malignant formation had occured. Even so it is hard to discuss about malignant transformation as there is only few cases reported, and most of them are without follow up. For this reason, like other osteochondromas, conditions as large mass, cartilage cap thicker than 1-2 cm, rapid growth and new onset of pain which increases the risk of malign transformation in extraskeletal osteochondromas and it should be considered for excision [12,14,15].
Conclusion
Osteochondromas, is the most common benign tumor of bone and rarely seen extraskeletally. It has been reported that they have low risk of malignant degeneration. We think, no surgical treatment is needed as long as these osteochondromas does not have risk factors for malignant transformation and stay asymptomatically, otherwise surgical excision should be the choice of treatment.
References
- Dahlin DC, Unni KK (1986)Bone Tumors. (4thedtn),Charles C Thomas Publication, Springfield.
- Dahlin DC, Salvador AH (1974) Cartilaginous tumors of the soft tissues of the hands and feet. Mayo ClinProc49:721–726.
- Estil JC Jr, Yeo ED, Kim HJ, Cho WT, Lee JJ (2013) Alargeextraskeletalosteochondromaof the foot. J FootAnkleSurg52:663-665.
- Singh R, Jain M, Siwach R, Sen R, Rohilla RK, et al. (2010) Soft-tissue osteochondroma of the heel pad: a case report and review of literature. FootAnkleSurg 16:e76-e78.
- Lim SC, Kim YS, Kim YS, Moon YR (2003) Extraskeletal osteochondroma of buttock. J KoreanMedSci18:127–130.
- Narula R, Arya A, Verma L, Singh S (2012) Soft TissueOsteochondromain Elbow Joint: A case report. MalaysOrthop J6:53-56.
- Liu ZJ, Zhao Q, Zhang LJ (2010)Extraskeletalosteochondromanear the hip: a pediatric case. J Pediatr Orthop B 19:524-528.
- Singh R, Sharma AK, Magu NK, Kaur KP, Sen R (2006) Extraskeletalosteochondromain the nape of the neck: a case report. J OrthopSurg (Hong Kong)14: 192-195.
- Kransdorf MJ, Meis JM (1993) From th earchives of the AFIP. Extraskeletal osseous and cartilaginous tumors of the extremities. Radiographics13:853-884.
- Turhan E, Doral MN, Atay AO, Demirel M (2008) Agiantextrasynovialosteochondromain the infrapatellar fat pad: end stage Hoffa'sdisease. ArchOrthopTraumaSurg128: 515-519.
- Nakanishi H, Araki N, Mukai K, Ohno H, Matsui Y (2001) Soft-tissueosteochondromain the calcaneal pad: a case report.J FootAnkleSurg40:396-400.
- Batra S, Garg B, Arora S (2013) Largesofttissueosteochondromaof the heel: a case report and literature review.MusculoskeletSurg97:255-258.
- Malik R, Kapoor N, Malik R (2004) Transformation of solitary osteochondroma calcaneumtochondrosarcoma—a casereport. Indian J PatholMicrobiol 47: 42–43.
- Sheff JS, Wang S (2005) Extraskeletalosteochondromaof the foot. JfootAnkleSurg44:57-59.
- Weiss SW, Goldblum JR (2007) Cartilaginous soft tissue tumors. In: Enzinger and Weiss's Soft Tissue Tumors (5thedtn) St. Louis: Mosby 1017–1036.
Relevant Topics
- 3D Printing in Limb-Sparing Surgery
- Adamantinoma
- Aneurysmal Bone Cysts
- Chondrosarcoma
- Chordomas
- Cryosurgery
- Enchondroma
- Ewing’s Sarcoma
- Fibrous Dysplasia
- Giant Cell Tumor of Bone
- Immunotherapy for Osteosarcoma
- Liquid Biopsy in Orthopedic Oncology
- Malignant Osteoid
- Metastatic Bone Cancer
- Molecular Profiling of Bone Tumors
- Multilobular Tumour of Bone
- Orthopaedic Oncology
- Osteocartilaginous Exostosis
- Osteochondrodysplasia
- Osteoma
- Osteonecrosis
- Osteosarcoma
- Primary Bone Tumors
- Sarcoma
- Secondary Bone Tumours
- Targeted Therapy in Bone Sarcomas
- Tumours of Bone
Recommended Journals
Article Tools
Article Usage
- Total views: 15484
- [From(publication date):
December-2015 - Jul 12, 2025] - Breakdown by view type
- HTML page views : 14536
- PDF downloads : 948