Research Article Open Access
Failed Agility™ LP Total Ankle Replacement Salvaged with Tibio-Talo-Calcaneal Arthrodesis and Vascularized Pedicled Medial Malleolus and Fibula Onlay Bone Grafts
Thomas S Roukis*
Orthopaedic Center, Gundersen Health System, South Avenue, La Crosse, Wisconsin
- Corresponding Author:
- Thomas S Roukis
Orthopaedic Center, Gundersen Health System
Mail Stop: C02-006, 1900 South Avenue
La Crosse, Wisconsin 54601-5467
Tel: 608-775-9673
Fax: 608-775-6707
E-mail: tsroukis@gundersenhealth.org
Received Date: July 08, 2016; Accepted Date: August 03, 2016; Published Date: August 12, 2016
Citation: Thomas SR (2016) Failed Agility™ LP Total Ankle Replacement Salvaged with Tibio-Talo-Calcaneal Arthrodesis and Vascularized Pedicled Medial Malleolus and Fibula Onlay Bone Grafts. Clin Res Foot Ankle 4:195. doi:10.4172/2329-910X.1000195
Copyright: © 2016 Thomas S Roukis. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Clinical Research on Foot & Ankle
Abstract
Controversy exists regarding the most predictable salvage for failed total ankle replacement. Revision total ankle replacement with soft-tissue release/reconstruction or explantation with tibio-talo-calcaneal arthrodesis with bulk structural allograft are the most commonly performed approaches. Tibio-talo-calcaneal arthrodesis with bulk structural allograft has a high complication rate; however, augmentation with vascularized pedicled onlay bone grafts may improve osseous union and functional limb salvage. This manuscript presents the revision of a failed Agility™ LP total ankle replacement system with severe >45° varus ankle deformity that was salvaged with tibio-talocalcaneal arthrodesis, bulk femoral head structural allograft and vascularized pedicled medial malleolus and fibula onlay bone grafts. At short-term 1.5-years follow-up the patient had a well-balanced and painless foot/ankle and return of a functional lower limb.
Keywords
Ankle mal-alignment; Complications; Deformity; Musculotendinous imbalance; Total ankle arthroplasty
Introduction
The concept and technique of performing a tibio-talo-calcaneal arthrodesis with bulk structural allograft fixated using a retrograde compression intramedullary nail as a salvage procedure for failed total ankle replacement is not new.
However, when compared with primary tibio-talo-calcaneal arthrodesis [1,2] a higher complication rate exists with nonunion occurring in >50%, infection in 20% and below-knee amputation in nearly 20% [3-7].
One reason for the high incidence of complications may be that the fibula is nearly universally resected with this procedure. Instead, vascularized pedicled bone graft augmentation of these salvage arthrodesis procedures to treat failed total ankle replacement seems a logical choice to enhance union rate and functional limb salvage.
The specific options for vascularized pedicled bone grafting about the ankle are the distal fibula supplied by the musculo-periosteal branches of the peroneal artery [8] and the medial malleolus supplied by the cortico-periosteal branches of the tibial artery [9].
However, to date, only 1 case involving tibio-talo-calcaneal arthrodesis stabilized with a retrograde intramedullary locked compression nail and a vascularized pedicled fibular onlay bone graft secured with multiple screws has been published [10].
The author presents a case involving a failed Agility™ LP total ankle replacement system (DePuy Synthes Joint Reconstruction, Warsaw, IN) with severe >45° varus ankle deformity that was corrected with explantation and tibio-talo-calcaneal arthrodesis stabilized with a retrograde intramedullary compression nail, bulk femoral head structural allograft and vascularized pedicled medial malleolus and fibula onlay bone grafts.
Case Study
A 50-year old man sustained a closed head injury in 2007 when he was struck by a car while riding his bicycle and subsequently developed chronic right ankle instability even on flat ground.
He trialed symptomatic relief measures and structural control measures that failed to relieve his symptoms or improve his function.
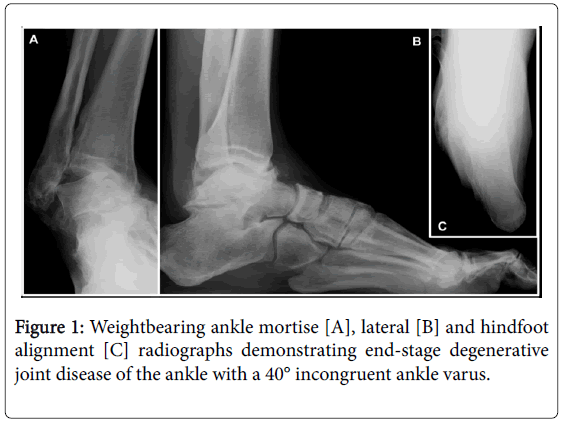
Clinical exam revealed grossly lateral ankle instability correctable to neutral with valgus stress. Weightbearing radiographs confirmed endstage ankle degenerative joint disease and a 40° incongruent ankle varus (Figure 1).
He declined an ankle arthrodesis and instead underwent an Agility™ LP TAR system size 4 tibial component, size 4 LP talar component and neutral 0-mm polyethylene insert with deltoid ligament release and peroneus brevis tendon lateral ankle stabilization through the distal tibio-fibular syndesmosis anchored underneath the lateral side plate [11] in 2008.
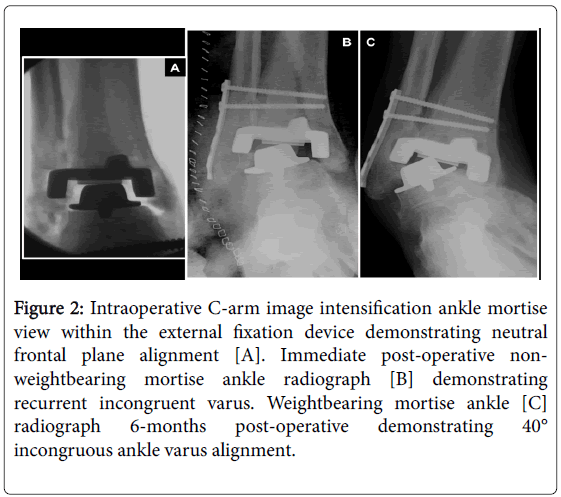
At the time of surgery the ankle was corrected to neutral with the external fixation device (Figure 2A).
However, after removing the external fixation device the ankle recoiled into varus and the post-operative films demonstrate this (Figure 2B).
During early follow-up ankle varus progressed until it worsened beyond the pre-operative value (Figure 2C).
Figure 2: Intraoperative C-arm image intensification ankle mortise view within the external fixation device demonstrating neutral frontal plane alignment [A]. Immediate post-operative nonweightbearing mortise ankle radiograph [B] demonstrating recurrent incongruent varus. Weightbearing mortise ankle [C] radiograph 6-months post-operative demonstrating 40° incongruous ankle varus alignment.
Based on his poor outcome he never returned for follow-up visits until he presented to the author in November 2013 as part of the authors total ankle replacement surveillance program.
He could only comfortably ambulate in plastic clog shoes due to pressure about the lateral ankle deformity.
Clinical examination demonstrated that the ankle was rigidly fixed in 46° varus with no frontal or sagittal plane mobility evident and global pain with ankle movement.
He had an obvious cavus foot posture with varus heel originating from the ankle and his lower leg muscle strength was graded at 5/5 to manual stress except for the peroneus brevis that appeared absent.
Multiple weightbearing views of the right ankle including sagittal plane stress views demonstrated no meaningful dorsiflexion or plantarflexion and heel varus of 42°.
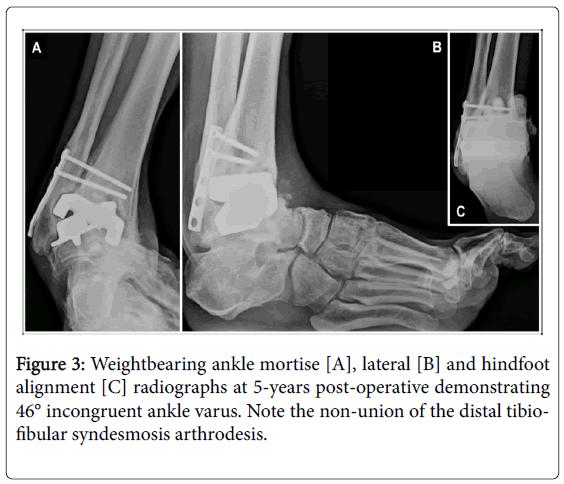
The tibial and talar components were rigidly mal-aligned in 46° varus with the lateral wing of the talar component eroded into in the fibula (Figure 3).
The syndesmosis fixation was intact but only partially united.
Based on the severity of his dysfunction and varus contracture the potential for a meaningful revision without major complication would decrease until he would either have to live with the condition, use supportive aides at all times or undergo a below-knee amputation amputation.
He did not desire amputation as a primary treatment and did not want to continue to live with his current limited functional status.
Based on the above, the author discussed the only meaningful option being explantation of the Agility™ LP prosthesis and deep hardware with posterior tibial tendon intramuscular recession lengthening [12], tibio-talo-calcaneal arthrodesis with a bulk femoral head structural allograft fixated with a retrograde locked intramedullary nail augmented with vascularized pedicled medial malleolus and fibula only bone grafts.
The revision surgery was performed in December 2014.
Surgical Procedures
After a validated surgical preparation of his lower leg [12], the initial operative intervention began with harvesting of bone marrow aspirate/ graft from the lateral calcaneus [13].
Intramuscular recession lengthening of the posterior tibial tendon [14] was then performed.
To do this a linear incision was made at the medial aspect of the operative lower extremity slightly inferior to the junction of the middle and distal one-thirds of the lower leg overlying the posterior-medial border of the tibia.
The incision was deepened to the junction of the posterior tibial musculotendinous junction that was verified with manual traction on the posterior tibial tendon that was then transected within the muscle belly.
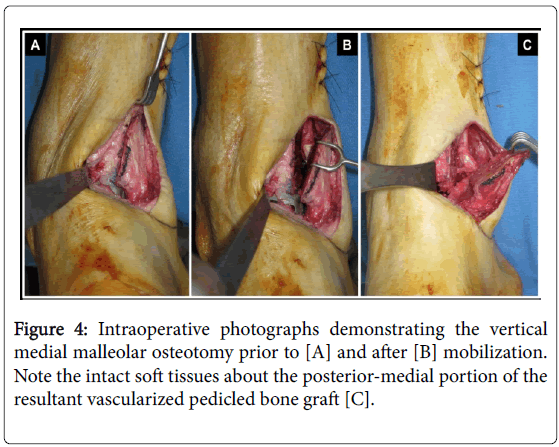
Next, the medial malleolus underwent vertical osteotomy with maintenance of the periosteum and posterior-medial soft-tissues to preserve its cortico-periosteal arterial supply [15] (Figure 4).
The prior lateral ankle skin incision was incised with additional length proximally and distally to minimize tension on the soft-tissue envelope during bone preparation.
The proximal incision was extended along the posterior–lateral edge of the fibula to the junction of the middle and distal one-thirds of the leg.
Controlled, layered dissection was carried down to the lateral side plate and screw fixation that were removed with maintenance of the periosteum overlying the remainder of the fibular shaft and lateral malleolus intact.
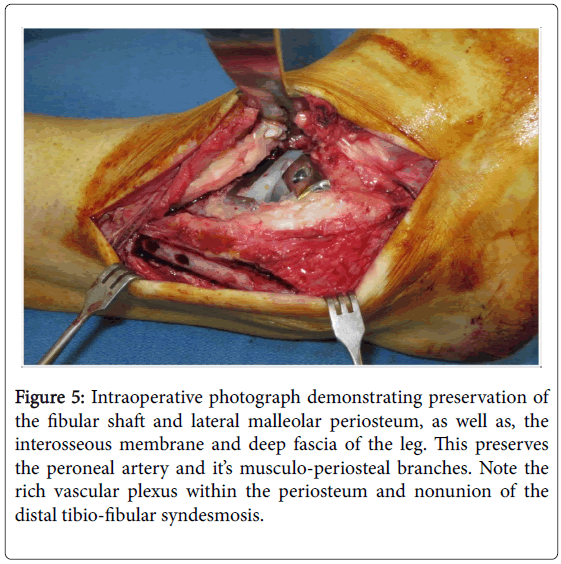
The interosseous membrane and deep fascia between the anterior and lateral muscle compartments of the leg were left intact to preserve the peroneal artery and it’s musculo-periosteal branches (Figure 5).
Figure 5: Intraoperative photograph demonstrating preservation of the fibular shaft and lateral malleolar periosteum, as well as, the interosseous membrane and deep fascia of the leg. This preserves the peroneal artery and it’s musculo-periosteal branches. Note the rich vascular plexus within the periosteum and nonunion of the distal tibio-fibular syndesmosis.
The distal inferior tibiofibular syndesmosis nonunion was freed from anterior-to-posterior to release the fibrous connections between the tibia and fibula.
The adjacent sides of the tibia distal-lateral tibia, as well as, medial aspect of the fibular shaft and lateral malleolus were resected of cortical bone to expose the cancellous bone substrate for later arthrodesis as part of the vascularized pedicled fibular onlay bone graft.
The fibula was then mobilized posterior-lateral to allow direct visualization of the failed total ankle replacement components.
The retained prosthetic components were wedged together in a varus posture as expected from the pre-operative radiographs and clinical examination.
The tibial component was firmly bonded to the adjacent bone requiring this to be cut free.
The polyethylene insert was then removed and revealed a deep groove consistent with severe edge loading.
Much polyethylene particular wear debris was appreciated in and around the joint and this was removed in its entirety.
The talar component was firmly bonded to the adjacent bone requiring this to be cut free.
Segments of avascular tibia and talus were then resected until only viable cancellous bone substrate was appreciated on direct visualization followed by fenestration with a 2-mm drill.
To perform the retrograde intramedullary compression nail insertion, the foot was placed in a functional position at the ankle and subtalar joints [16] and maintained with an intramedullary guide wire.
The position, alignment and osseous apposition were verified with direct visualization and intraoperative C-arm image intensification.
During withdrawal of the serial reamers the evacuated intramedullary tibial reaming’s should be collected as they exit the tibia, as well as, from the reamer blades and saved for later bone graft use.
Due to the massive bone void encountered following explantation of the failed Agility LP total ankle replacement, a bulk structural femoral head allograft was employed.
After completing sizing, the bulk allograft was soaked in sterile saline impregnated with Bacitracin solution (Pfizer, Inc., New York, NY) for 15-minutes time.
The area of the bulk allograft intended for direct contact with the host bone was then fenestrated with a 2-mm drill and these same surfaces were firmly packed with a mixture of calcaneal bone marrow aspirate and tibial reaming’s harvested during the intramedullary nail preparation process.
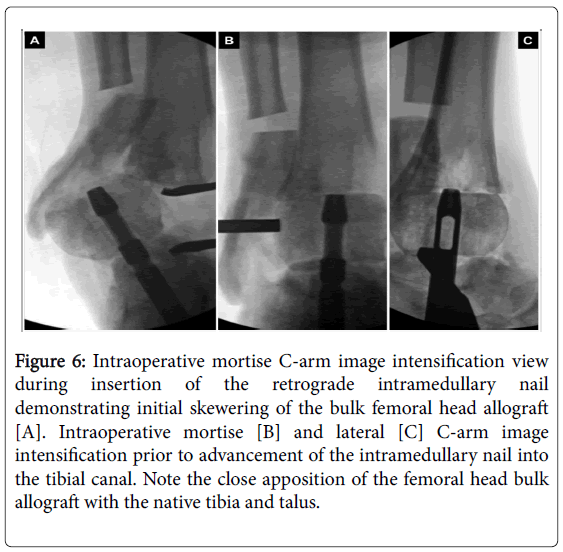
The bulk allograft was then skewered over the intramedullary nail during insertion and compressed between the tibia and talus (Figure 6).
Figure 6: Intraoperative mortise C-arm image intensification view during insertion of the retrograde intramedullary nail demonstrating initial skewering of the bulk femoral head allograft [A]. Intraoperative mortise [B] and lateral [C] C-arm image intensification prior to advancement of the intramedullary nail into the tibial canal. Note the close apposition of the femoral head bulk allograft with the native tibia and talus.
Definitive fixation consisted of a retrograde delivered, power reamed, modern tibio-talo-calcaneal arthrodesis intramedullary nail with internal compression capability secured with locking screws through the tibia, talus/bulk allograft and calcaneus.
Once the intramedullary nail was inserted and locked in place, the vascularized pedicled medial malleolus onlay graft was then secured to the underlying tibia and bulk femoral head allograft with a compression screw and washer. Next, the vascularized fibular onlay bone graft was then completed.
The first step involved removing a segment of fibular shaft 1-cm in length at the most proximal visualized portion of the fibula by releasing the investing deep fascia from the fibular shaft with care taken to protect the peroneal artery that is in close proximity within the anterior muscle compartment.
The 1-cm segment of bone was removed and a sharp curved osteotome was utilized from proximal-to-distal to release the deep investing fascia off of the posterior-lateral fibular shaft.
Next, a sterile Doppler probe was employed to identify the peroneal artery and it’s distal course, as well as, the dominant musculoperiosteal perforating arteries feeding the distal fibula.
Release of the deep investing fascia off of the posterior-medial and posterior-lateral portions of the fibular shaft was then performed.
Immediately prior to inset, the visualized peroneal artery and musculo-periosteal branches are bathed in lidocaine 2% HCl solution (BDI Pharma, Columbie, SC) to resolve any arterial spasm common following manipulation during dissection.
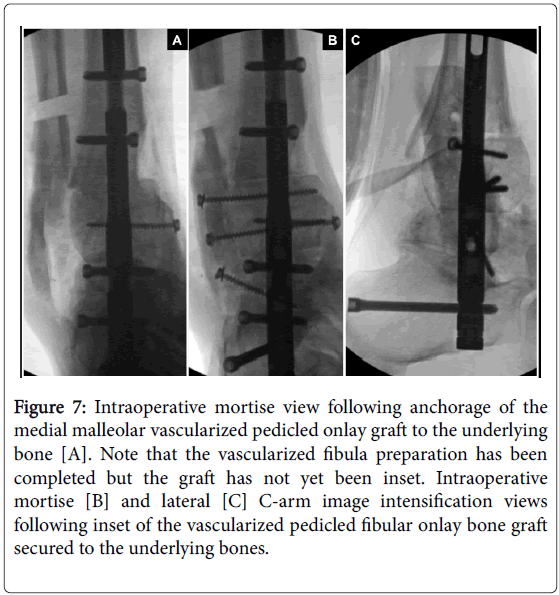
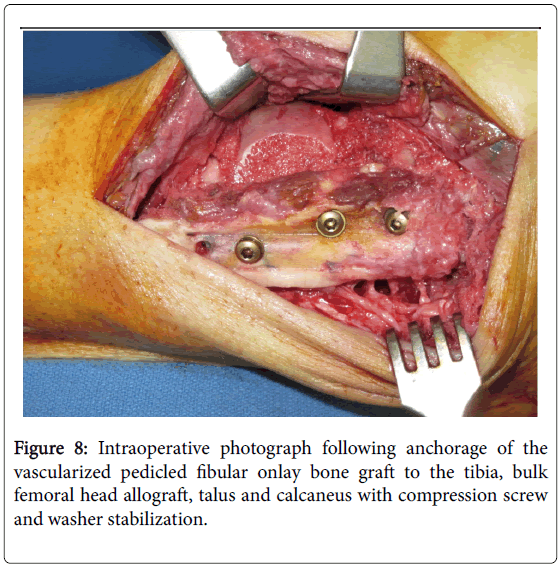
The fibular shaft was then carefully mobilized distally so that it is in direct contact with the distal tibia, medial surface of the fibular malleolus and lateral aspects of the bulk allograft, talus and calcaneus. The fibular graft was then stabilized with a bone clamp and secured onto the adjacent bone segments with multiple compression screws with washers oriented in the direction of greatest bone stock (Figures 7 and 8).
Figure 7: Intraoperative mortise view following anchorage of the medial malleolar vascularized pedicled onlay graft to the underlying bone [A]. Note that the vascularized fibula preparation has been completed but the graft has not yet been inset. Intraoperative mortise [B] and lateral [C] C-arm image intensification views following inset of the vascularized pedicled fibular onlay bone graft secured to the underlying bones.
Final intraoperative C-arm image intensification views were taken to assess for proper length, orientation and alignment of the metallic fixation and close osseous apposition of all osseous surfaces.
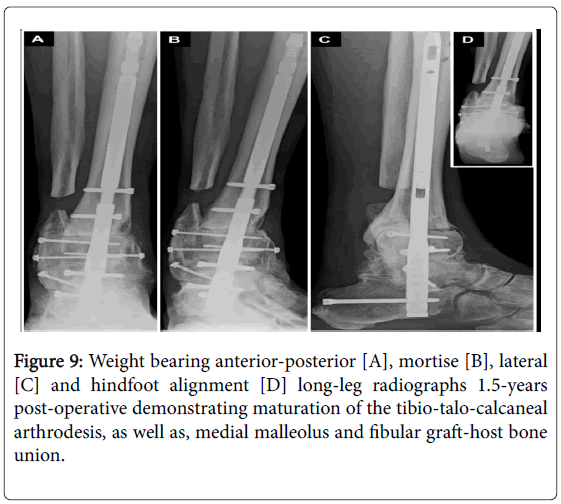
The soft-tissues were closed in layers over a closed-suction drain sewn in place. A standard post-operative protocol for revision of failed total ankle replacement was employed as previously described [17]. At 1.5-years follow-up the ankle/hindfoot was stable to manual stress and weight bearing radiographs demonstrated no change in position/ alignment with osseous union appreciated to all interfaces except the distal tibia-bulk femoral head allograft site that had persistent gap appreciated without evidence of impending failure. At the time of most recent follow-up the patient had no pain, ambulated without a brace or modified shoes and returned to his desired physical activities (Figure 9).
Discussion
Controversy exists regarding the most predictable salvage for failed total ankle replacement [18-20]. Revision total ankle replacement with soft-tissue release/reconstruction or explantation with tibio-talocalcaneal arthrodesis with bulk structural allograft are the most common procedures performed. Although in a constant state of evolution, there are limits to performing revision total ankle replacement and most efficacious treatment strategy remains elusive [21]. Tibio-talo-calcaneal arthrodesis stabilized with retrograde intramedullary nail fixation is associated with a high incidence of complications including nonunion requiring revision, hardware failure requiring removal, and in catastrophic situations, below-knee amputation [1,2]. The incidence of complication is even higher when performed with bulk structural allograft and with hostile soft-tissues such as encountered with failed total ankle replacements [3-7]. Since the vascular anatomy of the fibula/lateral malleolus and medial malleolus are robust, their use as vascularized pedicled onlay bone grafts based on intact musculo-periosteal branches of the peroneal artery and cortico-periosteal branches of the tibial artery, respectively, may enhance osseous union without the complexity involved with free vascularized bone transplantation. However, harvest and inset of the vascularized onlay bone grafts discussed does remain technically difficult and should only be undertaken by foot and ankle surgeons experienced performing these procedures. The world literature on this topic and with these techniques is unfortunately limited and further prospective studies should be undertaken.
Conclusion
A case involving a failed Agility™ LP prosthesis with severe >45° varus ankle deformity that was salvaged with tibio-talo-calcaneal arthrodesis secured with a retrograde intramedullary compression nail, bulk femoral head structural allograft and vascularized pedicled medial malleolus and fibula onlay bone grafts. At short-term 1.5-years follow-up the patient had a well-balanced and painless foot/ankle and return of a functional lower limb.
Financial Disclosure
None.
Conflict of Interest
None.
References
- Jehan S, Shakeel M, Bing AJF, Hill SO (2011) The success of tibiotalocalcaneal arthrodesis with intramedullary nailing: A systematic review of the literature. ActaOrthopBelg77:644-651.
- Franceschi F, Franceschetti E, Torre G, Papalia R, Samuelsson K, et al. (2016) Tibiotalocalcaneal arthrodesis using an intramedullary nail: A systematic review. Knee Surg Sports TraumatolArthrosc 24:1316-1325.
- Jeng CL, Campbell JT, Tang EY, Cerrato RA, Myerson MS (2013) Tibiotalocalcaneal arthrodesis with bulk femoral head allograft for salvage of large defects in the ankle. Foot Ankle Int 34:1256-1266.
- DeVries JG, Berlet GC, Hyer CF (2013) Predictive risk assessment for major amputation after tibiotalocalcaneal arthrodesis. Foot Ankle Int 34:846-850.
- Bussewitz B, DeVries JG, Dujela M, McAlister JE, Hyer CF, et al. (2014) Retrograde intramedullary nail with femoral head allograft for large deficit tibiotalocalcaneal arthrodesis. Foot Ankle Int 35:706-711.
- Donnenwerth MP, Roukis TS (2013) Tibio-talo-calcaneal arthrodesis with retrograde compression intramedullary nail fixation for salvage of failed total ankle replacement: A systematic review. ClinPodiatr Med Surg 30:199-206.
- Gross C, Erickson BJ, Adams Jr SB, Parekh SG (2015) Ankle arthrodesis after failed total ankle replacement: A systematic review of the literature. Foot Ankle Spec8:143-151.
- Liwen D, Futian L, Juan J, Guocheng Z (2000) Transplantation of fibula with vascular pedicle for fusion of ankle in leprotic drop-foot. Indian J Lepr 72:431-436.
- Sakai K, Doi K, Kawai S (1991) Free vascularized thin corticoperiosteal graft. PlastReconstSurg 87:290-298.
- Roukis TS, Kang RB (2016) Vascularized pedicled fibula onlay bone graft augmentation for complicated tibiotalocalcaneal arthrodesis with retrograde intramedullary nail fixation: A case series. J Foot Ankle Surg 55:857-867.
- Coetzee JC (2010) Surgical strategies: Lateral ligament reconstruction as part of the management of varus ankle deformity with ankle replacement. Foot Ankle Int 31:267-274.
- Roukis TS (2010) Bacterial skin contamination prior to and after surgical preparation of the foot, ankle, and lower leg in patients with diabetes and intact skin versus patients with diabetes and ulceration: A prospective controlled therapeutic study. J Foot Ankle Surg 49:348-356.
- Roukis TS, Hyer CF, Philbin TM, Berlet GC, Lee TH (2009) Complications associated with autogenous bone marrow aspirate harvest from the lower extremity: An observational cohort study. J Foot Ankle Surg 48:668-671.
- Roukis TS (2013) Tibialis posterior recession for balancing varus ankle contracture during total ankle replacement. J Foot Ankle Surg 52:686-689.
- Doets HC, van der Plaat LW, Klein JP (2008) Medial malleolar osteotomy for the correction of varus deformity during total ankle arthroplasty: Results in 15 ankles. Foot Ankle Int 29:171-177.
- Roukis TS (2006) Determining the insertion site for retrograde intramedullary nail fixation of tibiotalocalcaneal arthrodesis: A radiographic and intraoperative anatomical landmark analysis. J Foot Ankle Surg 45:227-234.
- Schweinberger MH, Roukis TS (2010) Effectiveness of instituting a specific bed protocol in reducing complications associated with bed rest. J Foot Ankle Surg 49:340-347.
- Deleu P-A, Bevernage BD, Maldague P, Gombault V, LeemrijseTh (2014) Arthrodesis after failed total ankle replacement. Foot Ankle Int 35:549-557.
- Rahm S, Klammer G, Benninger E, Gerfer F, Farshad M, et al. (2015) Inferior results of salvage arthrodesis after failed ankle replacement compared to primary arthrodesis. Foot Ankle Int 36:349-359.
- Kamrad I, Henricsson A, Karlsson MK, Magnusson H, Nilsson JA, et al.(2015) Poor prosthesis survival and function after component exchange of total ankle prostheses: An analysis of 69 cases in the Swedish Ankle Registry. ActaOrthop 86:407-411.
- Roukis TS (2014) Strategies for revision total ankle replacement. J Orthop Trauma Rehab 18:59-68.
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 15392
- [From(publication date):
September-2016 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 14453
- PDF downloads : 939