Research Article Open Access
Fear of Heights and Visual Height Intolerance in Children 8 10 Years Old
Doreen Huppert1,2* and Thomas Brandt1,2
1Institute of Clinical Neurosciences, University of Munich, Germany
2German Center for Vertigo and Balance Disorders, University of Munich, Germany
- *Corresponding Author:
- Doreen Huppert
Institute of Clinical Neurosciences
and German Center of Vertigo and
Balance Disorders University
of Munich, Marchioninistr 15
81377 Munich, Germany
Tel: +49 89 4400 72380
Fax: +49 89 4400 78883
E-mail: doreen.huppert@med.uni-muenchen.de
Received Date: March 06, 2015; Accepted Date: July 07, 2015; Published Date: July 13, 2015
Citation: Huppert D, Brandt T (2015) Fear of Heights and Visual Height Intolerance in Children 8–10 Years Old. J Child Adolesc Behav 3:219.doi: 10.4172/2375-4494.1000219
Copyright: © 2015 Huppert D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Child and Adolescent Behavior
Abstract
Objective: To evaluate the prevalence, symptoms, spontaneous course, and behavioral consequences of visual height intolerance in children in comparison to adults. Methods: Survey in three primary schools on the frequency of visual height intolerance in 455 children aged 8 to 10 years. Individual structured interviews of 90 susceptible children and 54 of their parents. Results: The prevalence of visual height intolerance in children amounted to 34%; there was no gender preponderance. The condition began at a mean age of 5.9 years and rarely showed a tendency to generalize with respect to trigger stimuli. Triggers and symptoms were similar to those in adults. Avoidance behavior was reported by less than one third of the children, and there was only minimal subjective impairment of life quality. The condition was not perceived to be a disease or an individual weakness. Frequency and severity had already spontaneously improved in nearly one half of the children by the time of the survey. Conclusion: More than one third of prepubertal girls and boys exhibited susceptibility for visual height intolerance which - in contrast to the adult-onset type of the condition – appeared to take a benign spontaneous course.
Keywords
Fear of heights; Visual height intolerance; Primary school children; Epidemiology; vertigo
Introduction
Acrophobia or fear of heights is a specific phobia according to the Diagnostic and Statistical Manual of Mental Disorders (DSM-V) [1]. Its life-time prevalence ranges from 3.1 to 6.4% [2-4]. There is a continuum of severity ranging from acrophobia to a less distressing visual height intolerance (vHI), to which the categorical distinction of a specific phobia does not apply, but which may also cause medically relevant restrictions [4-6]. In a cross-sectional epidemiological study on 3,517 individuals representative of the general populationthe lifetime prevalence of vHI was found to be 28% [7]. It was higher in women (32%) than in men (25%) and increased with age. The main symptoms of vHI are fearfulness, a queezy-stomach feeling, subjective postural instability with to-and-fro vertigo, inner agitation, and vegetative symptoms as well as weakness in the knees, palpitations, sudden sweating, light-headedness, and tremor. Climbing a tower is the first and most common precipitating stimulus followed by hiking, climbing a ladder, walking over a bridge, looking out a window or from a balcony on an upper floor, and climbing stairs. The range of precipitating height stimuli broadens over time in more than 50% of afflicted persons. The most frequent reaction to vHI is to avoid the triggering stimuli (>50%). This strategy may have a considerable impact on quality of life [8]. Initial attacks occur most often (30%) in the second decade, but can manifest throughout life. A total of 16% of the afflicted adults reported that vHI began in childhood before the age of 10 years; they represent 4.5% of the general population.Epidemiological studies on children are available for anxiety disorders and specific phobias, especially fear of the dark, spider phobia, and medical phobias as well as fear of heights [9-11]. However, there were no epidemiological studies that focused on the frequency and phenomenology of vHI in prepubertal children.
Our study on 455 children aged 8 to 10 years addressed the main questions of frequency, phenomenology, the typical triggers of vHI in childhood in comparison to those in adulthood, and of how children perceive their susceptibility with respect to their self-efficacy belief relative to their peers. Further issues were the coping strategies of children and how vHI affects their daily activities and family life, and the disorder’s spontaneous course after first manifestation. One of the hypotheses was that vHI in childhood is less severe than in adulthood with a more favourable spontaneous course.
Method
Interviews were conducted in three primary schools; 455 unselected children (244 boys, 211 girls) aged 8 to 10 years (mean age=9 years) participated. In a first step, we (DH, TB) interactively discussed the topic of vHI separately with each class in groups of 17 to 23 pupils for about 20 minutes. Only the two authors were involved in all discussions and interviews in order to maintain a consistent standard and augment the representative character of the study. This procedure allowed us not only to personally evaluate frequency, but also to explain any questions that the children did not clearly understand. We preferred this to just asking volunteers to fill out a questionnaire. The group interview proceeded as follows. To slowly approach the subject,we first asked the children if they had already been in high places, for example, in the mountains when climbing, high houses, towers, on bridges, etc., and what feelings they had had in these situations. After the children had expressed their sensations, the interviewers gave a general description of trigger situations and the symptoms of vHI determined in the study in adults. The children could ask questions at any time if they did not understand something or make additional statements. At the end of this discussion the interviewers asked who of the children had already experienced visual height intolerance, an unpleasant feeling caused by visual exposure to heights. Those children who indicated that they had experienced symptoms of vHI were selected for an individual, structured interview in a second step. One might suspect that group interviews tend to produce false negatives. However, both interviewers had the strong impression that in the relaxed atmosphere of the interview the children were not too shy to speak about their symptoms before a group since they did notconsider their feelings at height shameful (see results). The authors DH and TB conducted these individual structured interviews separately. They included questions about the age at first manifestation, typical symptoms, trigger situations, possible traumatic or triggering events before the first manifestation, distress and restrictions in daily activities, self-efficacy belief, individual forms of compensational behavior, whether or not the condition was confided to the parents, associated disorders and other anxieties apart from heights, and the spontaneous course since first manifestation. There was a list of each of these items, for example, the trigger situations and symptoms. If children responded to only a few items of the different questions, the interviewers made sure to ask all items according to the list.
Afterwards the parents were interviewed using a structured telephone survey about their perception of vHI in their children, for example, about constraints in daily life or sporting activities, behavioural problems, fearfulness, and questions on the family history of vHI and of migraine in children and parents.
The study was approved by the Bavarian State Ministry of Education after a written application providing detailed information about methodology, objectives, practicability, feasibility as regards the age of the children and the normal operation of the school, data protection, and benefit from a medical point of view. Parents had to give their written consent to the research and to publication of the results after being informed in writing. The children were also asked about their willingness to participate in the study. The headmaster and teachers gave their approval and helped organize the local inquiry. The study received written permission from the Local Ethics Committee and has been performed in accordance to the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.The software Excel 2007 was used for the statistical data evaluation.
Results
Survey of the children
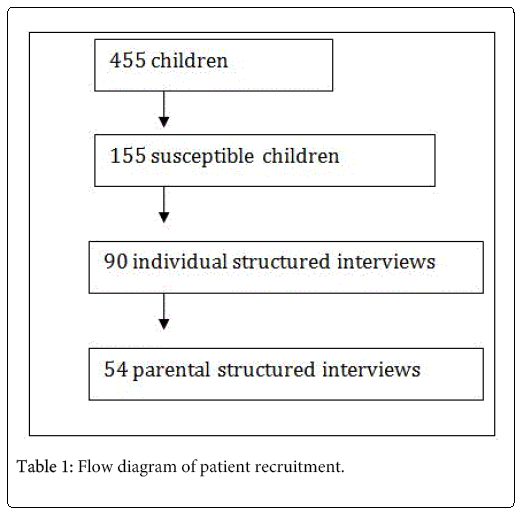
Frequency: Of 455 primary school children 155 (81 boys; 74 girls) were found to be susceptible to vHI. Thus, the overall frequency was 34%. The gender distribution of vHI was nearly equal. In accordance with the written agreement of their parents ninety-three of the 155 children (mean age 9 years; 53 boys, 40 girls) took part in the individual structured interviews. Three boys were eliminated from the group of 93 children after the interviews because of relevant visual or locomotor handicaps. One can assume that this subsample is representative of the original group of 155 pupils that reported instances of vHI, since age and gender distribution were quite similar. Of the 90 children ten had experienced only one instance of vHI, and 80, recurrent attacks of vHI (Table 1).
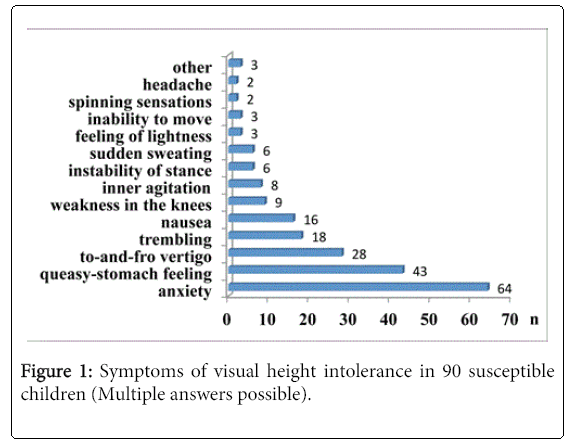
Symptomatology: The main symptoms were fearfulness and a queasy-stomach feeling. Often the children described tingling sensations, postural to-and-fro vertigo, trembling, nausea, weakness in the knees, inner agitation, sudden sweating, and subjective instability of stance (Figure 1). The gender distribution for the particular symptoms was nearly equal, with the exception of to-and-fro vertigo, which was perceived more frequently by boys (19 vs. 9) during attacks of visual height intolerance.
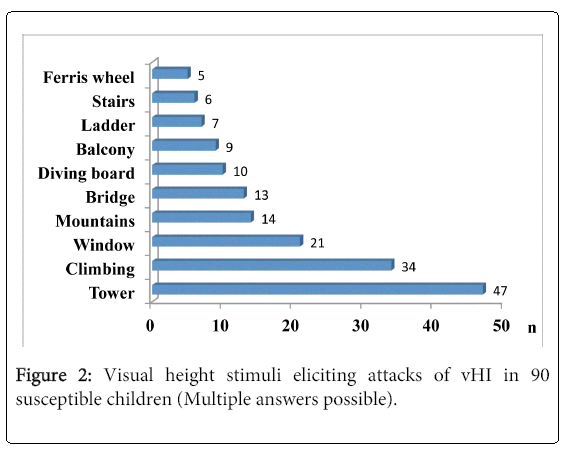
Triggers: Climbing a tower was the first and most common precipitating stimulus, followed by climbing in trees, in parks and on walls, looking out of windows in high buildings, hiking in high mountains, walking over a bridge, standing on a diving board, looking from a balcony, and climbing a ladder or staircase (Figure 2). Boys stated more often that the trigger situation “tower” was a precipitating stimulus (30 vs. 17), whereas the other triggers showed no gender preponderance.
When asked about the occurrence of vHI attacks in triggering situations 36 of the children (40%) reported “sometimes”, 26 children (29%) “always”, 18 (20%) said that the frequency varied, and 10 (11%) children had experienced only one single attack of vHI.
First manifestation and spontaneous course: The mean age of the first vHI attack was 5.9 years. The course of the frequency of attacks was as follows: worsened with increasing frequency in 11 children (12%); remained stable in 36 children (40%); improved with less frequent attacks in 23 children (26%); spontaneous remission occurred in 10 children (11%; 6 boys, 4 girls) after a mean of 2.9 years; experience of only one single attack of vHI in 10 children (11%; 4 boys, 6 girls).
Nearly half of the children who had experienced more than one vHI attack (n=80) reported that the attacks always occurred when exposed to the trigger situations (32.5%), mostly or sometimes in 67.5%. Only one child indicated that the kind of trigger stimuli showed a tendency to generalize. The severity of symptoms during the attacks increased in 15%, remained equal in 45%, and became less severe in 40%. Only nine children remembered an event preceding the first attack, which might possibly have triggered manifestation of vHI; this was mostly a fall from a height, but without severe injury.
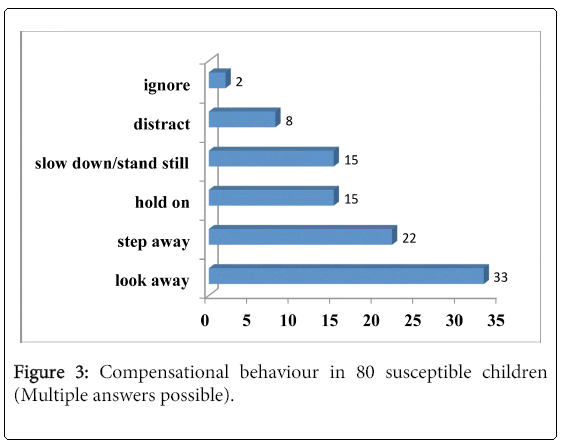
Behavior and coping strategies: Susceptible children reported different compensational behaviour in the triggering situations, for example, looking away, stepping away from the abyss, holding on to something, or slowing down or standing still (Figure 3). Some of the children had developed various strategies of coping with vHI, e.g., ignoring the symptoms or distracting themselves. Avoidance behaviour was reported by 26 children (29%); this involved mostly towers, climbing, high buildings, or mountains. Nevertheless, children with avoidance behaviour did not feel restricted in their daily activities. Most children (n=73; 81%) were able to talk freely about their problem in the acute situation, eight children hesitated to talk about it, and nine felt embarrassed. Only ten children (11%) stated that their susceptibility to vHI evoked feelings of inferiority to their peers. Nevertheless, about two thirds (n=61; 68%) considered themselves as courageous as other children, but more than one third (n=35; 39%) felt themselves more anxious. In the acute situation 11 children (12%) had even needed help. VHI was in general not regarded as a disease. Forty-two children believed that about one half or more of their peers were also susceptible to vHI. A total of 59% of the children had talked to their parents about their susceptibility. Parental behaviour in the case of 19% of the children was described as cautious and anxious in comparison to that of parents of the peers. None of the parents had sought a medical consultation for their children.
More than half of the children (n=54; 60%) stated that they had other fears; most often these were fears of certain animals (n=32), followed by injections or sharp things, darkness, and being alone. If children knew of relatives who were also affected by vHI they were mostly the parents (34%), more often the mother, rarely siblings (15%). Nearly three quarters (n=63; 70%) reported that they were susceptible to motion sickness. Episodic headache lasting for hours occurred independently of vHI in 36 children (19 boys, 17 girls) with varying frequency.
Survey of parents
Fifty-four of the 90 parents could be contacted for an interview. None of the contacted parents refused to take part in the interview. Half of them knew of their children’s susceptibility to vHI. Only five (9%) considered that the susceptibility had led to constraints, especially in sporting activities like climbing. One parent mentioned a restriction in daily family life. Seven parents (8%) had observed avoidance behavior when walking over bridges or looking down from high buildings, and during sporting activities including riding in gondolas. Half of the parents rated their children as more cautious than siblings or peers; 56% (n=30) indicated that there was a family history of vHI, mostly (n=20) affecting the mothers. A frequency of migraine within the family was referred to by 56% (n=30), again mostly affecting the mothers (n=22). Only ten parents (19%) were aware that their children suffered from episodic headaches.
Discussion
A major finding of this study is the high prevalence (one third) of vHI in prepubertal children, without any gender preponderance. In the following we discuss the phenomenology, developmental aspects, and the spontaneous course of vHI in children compared to the condition in adults.
Our study closes a gap in the available data on vHI in children. Earlier studiesfocused on anxiety disorders [9] and specific phobias in children [10]. According to the latter review on specific phobias in childhood, the prevalence rates ranged from 2.4 to 3.5%; there were no differences in ethnicity. When the definition of “excessive fears and worries or phobias” was broadened, prevalence rates of 7 to 9% were found. A survey on the prevalence and comorbidity of psychiatric disorders among 6-year-olds revealed that specific phobias (without any specification of the subtypes, e.g., animal, natural environment, blood or injection injury) were the most common subtypes of anxiety disorders, having a frequency of 5.4% [12]. In another study on dishabituation processes in fear of heights in children, fear of heights was found to occur in 6.9% of children aged 11 years and in 19.1% of young adults aged 18 years, if moderate and severe forms were included [13].
In the general adult population specific phobias also rank among the most frequent anxiety disorders with prevalence rates between 9.4 and 12.8% [14-18]. The life-time prevalence of the specific phobia fear of heights (acrophobia) ranged between 3.1 and 6.4% [2-4]. If the survey on fear of heights includes the less severe form of visual height intolerance as described in the Introduction, the prevalence rate in adults is much higher, i.e. 28% [7].
Our finding in the current study that 34% of children between 8 and 10 years of age report a susceptibility to vHI is only slightly higher than the prevalence rate of 28% found in adults. This finding seemingly contradicts the data of our earlier study in adults. Here only 4.5% of susceptible adults indicated that their first manifestation of vHI occurred in the first decade. The most probable explanation for this is that intolerance to heights in children takes a benign spontaneous course with remission occurring within a few years. This view is supported by the interviews in which nearly half of the children reported a spontaneous improvement or remission already at an age of 8 to 10 years. On the other hand, the evaluation of our data may be biased due to the uncertainties of adults trying to recall exactly the onset of vHI retrospectively. However, the benign course corresponds to other follow-up studies in children with specific phobias including fear of heights [13,14]. This allows the conclusion that vHI does not begin in prepubertal childhood in the vast majority of the general adult population.
Gender-specific differences?
In adults the prevalence of vHI is higher in women (32%) than in men (25%) [7]. A higher female susceptibility has also been reported for the specific phobia fear of heights [3-19]. The prepubertal children in the current study showed no gender predominance in susceptibility. The survey in adults [7] revealed that the female preponderance of susceptibility to vHI develops in the third decade. This is very similar to the manifestation of the female preponderance of migraine, which also becomes evident in the third decade [20]. Our study on vHI found the same frequency of episodic headache in boys and girls.
Phenomenology with respect to vHI in adulthood
There are some congruencies in the phenomenology of vHI in children and adults. The trigger situations, for example, are similar: climbing a tower was the most common trigger in both. Also the main bodily symptoms appear in both age groups; they differ only in frequency. Fearfulness and a queasy-stomach feeling predominate in children and adults, whereas postural to-and-fro vertigo, subjective instability of stance and gait, and weakness in the knees occur less often in children than in adults. Some features are distinctive for children: they generally do not consider the condition a disease or a shameful attribute; avoidance behavior occurs in less than one third, it causes no harmful physical inactivity in the majority of those afflicted, especially no essential constraint in sporting activities; none of the children reported having seen a doctor about this matter. In contrast more than 50% of adult susceptibles exhibited an avoidance behavior that was perceived as having a considerable impact on their daily life activities and interpersonal interactions, i. e., quality of life [8], so much so that 11% had consulted a medical doctor [7].
Visual height intolerance and the course of anxiety development
Children develop fears that come and go at particular stages of their life [11] which are determined by an interaction between genetic susceptibility, environmental influences, and individual experiences. There are inborn fears that do not require any triggering experiences, but other fears such as fear of heights require a certain stage of perceptual and cognitive functions [21] to become sensitive to the visual trigger of heights. There is, however, also an inborn behavioral protective strategy when exposed to heights, the visual cliff behavior comprehensively studied by Walk and Gibson [22-24]. The innate ability of the human infant to visually perceive and avoid a brink is supported by animal experiments in a number of species including chicks, rats, kittens, and goats. Visual depth avoidance does not require prior experience of falling off high places; it can even be observed at the very beginning of locomotion. In an ambivalent situation in which heavy glass covered the steep, precipitous side of a cliff, crawling children still refused to cross the glass-covered brink despite the somatosensory tactual assurance of a solid surface [23]. The behavior of infants near cliffs has been further examined, and studies have emphasized that visual proprioception or locomotor experience influences behavioral reactions at edges of drop-offs [21,25-27]. Psychological mechanisms also play an important role: the child can cope with the emotional distress caused by the artificial depth if the mother shows positive support but not if she exhibits an overanxious emotional reaction [28].
The acquisition of anxiety during childhood when exposed to heights has been described in several models. As in other psychiatric disorders the antagonism nature vs. environment led to a multifactorial model for the manifestation of specific phobias [29]. Cognitive aspects and biases, which consider specific phobias as learned and habituated reactions, are integrated into the nonassociative learning theory, i.e., evolution-primed responses to threatening stimuli in predisposed individuals [13,30-34]. This means an inborn disposition is expressed after certain trigger experiences. These are mostly non-traumatic: a fall-off is not required to induce a height phobia [13]. Motor function is described as impaired in many children who have anxiety disorders that may interfere with their activities of daily living [35]. Especially the excessive sensitivity of anxiety-disordered children to balance-challenging situations is emphasized [36,37]. It is conceivable that this sensitivity negatively influences the perception of heights in the sense that a dangerous situation may in turn reduce the feeling of safety at heights and evoke the described symptomatology.
Acrophobia and vHI also impair visual exploration with less eye and head movements [38]. Body posture during an attack of vHI is characterized by a stiffening of the musculo-skeletal system with cocontraction of anti-gravity leg and neck muscles [6,39]. Walking is slow and cautious [40,41]. Anxiety appears to be the critical symptom that causes the typical, but non-specific eye- and motor behavior which can be described as tonic immobility [6].
For children an important environmental factor is how parents cope with anxiety. Higher levels of parental anxiety lead to a lower threshold of anxiety-induced reactions in children [42]. Moreover, children’s play behavior has an important function in the process of learning to master age-adequate and possibly dangerous challenges. Especially playing children perform multiple kinds of trial actions that are supposed to have an anti-phobic effect in normal child development [43]. VHI may possibly be a predictor for the development of other anxiety disorders over the course of time, especially since comorbidity of fear of heights with anxiety conditions is a common phenomenon as well as comorbidity with depressive disorders [2,16,18,44-46].
The following are limitations of our study in children:
Some data were obtained retrospectively such as the reported age at onset. Possibly children cannot recall the timing of such past events with precise accuracy.
Our hypothesis of two types of vHI - one benign starting in prepubertal childhood and another much more chronic, associated with major psychiatric comorbidity, and starting in adolescence and adulthood - can only be validated within a longitudinal research design.
Conclusion
Whilethe prevalence of vHI in children is higher than in adults, the disorder takes a favorable spontaneous course in children. This means our study suggest two types of vHI: a benign early-onset type in childhood and a more chronic type with first manifestation in adulthood [7]. The existing literature describes the development of fears to certain stimuli as a protective mechanism that keeps children out of situations with which they are too immature to cope. However,activation and risky play during the process of maturation may have an anti-phobic effect [43]. One could argue that the spontaneous benign course of vHI in childhood could be supported if parents encouraged their children to controlled exposure to the feared or avoided situations as a strategy of desensibilization. A too restrictive parental behavior may promote the persistence of the condition.
Acknowledgement
The authors would like to thank the school headmasters for their helpful support with organizing the interviews and Judy Benson (MA) for copyediting the manuscript. The study was supported by the German Federal Ministry of Education and Research (Grant 01 EO 0901) and the Hertie Foundation.
References
- Zelazny K, Simms LJ2 (2015) Confirmatory factor analyses of DSM-5 posttraumatic stress disorder symptoms in psychiatric samples differing in Criterion A status. J Anxiety Disord 34: 15-23.
- Depla MF, ten Have ML, van Balkom AJ, de Graaf R (2008) Specific fears and phobias in the general population: Results from the Netherlands Mental Health Survey and Incidence Study (NEMESIS). Soc Psychiatry Psychiatr Epidemiol 43: 200-208.
- LeBeau RT, Glenn D, Liao B, Wittchen HU, Beesdo-Baum K, et al. (2010) Specific phobia: a review of DSM-IV specific phobia and preliminary recommendations for DSM-V. Depress Anxiety 27: 148-167.
- Kapfhammer HP, Huppert D, Grill E, Fitz W, Brandt T (2015) Visual height intolerance and acrophobia: clinical characteristics and comorbidity patterns.Eur Arch Psychiatry Clin Neurosci 265: 375-385.
- Brandt T, Benson J, Huppert D (2012) What to call “non-phobic” fear of heights? Br J Psychiatry 190:81.
- Brandt T, Huppert D (2014) Fear of heights and visual height intolerance. Curr Opin Neurol 27: 111-117.
- Huppert D, Grill E, Brandt T (2013) Down on heights? One in three has visual height intolerance. J Neurol 260: 597-604.
- Schäffler F, Müller M, Huppert D, Brandt T, Tiffe T, et al. (2014) Consequences of visual height intolerance for quality of life: a qualitative study.Qual Life Res 23: 697-705.
- Simon E, Bögels SM (2009) Screening for anxiety disorders in children. Eur Child Adolesc Psychiatry 18: 625-634.
- Silverman WK, Moreno J (2005) Specific phobia. Child Adolesc Psychiatr Clin N Am 14: 819-8, ix-x.
- Marks I1 (1987) The development of normal fear: a review.J Child Psychol Psychiatry 28: 667-697.
- Petresco S, Anselmi L, Santos IS, Barros AJ, Fleitlich-Bilyk B, et al. (2014) Prevalence and comorbidity of psychiatric disorders among 6-year-old children: 2004 Pelotas Birth Cohort.Soc Psychiatry Psychiatr Epidemiol 49: 975-983.
- Poulton R, Davies S, Menzies RG (1998) Evidence for a non-associative model of the acquisition of a fear of heights. Behav Res Ther 36: 537-544.
- Kessler RC, McGonagle KA, Zhao S (1994) Lifetime and 12-month prevalence of DSM-III-R psychiatric disorders in the United States. Results from the National Comorbidity Survey. Arch Gen Psychiatry 51: 8-19.
- Bijl RV, Ravelli A, van Zessen G (1998) Prevalence of psychiatric disorder in the general population: results of The Netherlands Mental Health Survey and Incidence Study (NEMESIS).Soc Psychiatry Psychiatr Epidemiol 33: 587-595.
- Kessler RC, Chiu WT, Demler O, Merikangas KR, Walters EE (2005) Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry 62: 617-627.
- Becker ES, Rinck M, Türke V, Kause P, Goodwin R, et al. (2007) Epidemiology of specific phobia subtypes: findings from the Dresden Mental Health Study. Eur Psychiatry 22: 69-74.
- Stinson FS, Dawson DA, Patricia Chou S, Smith S, Goldstein RB, et al. (2007) The epidemiology of DSM-IV specific phobia in the USA: results from the National Epidemiologic Survey on Alcohol and Related Conditions. Psychol Med 37: 1047-1059.
- de Girolamo G, Polidori G, Morosini P, Scarpino V, Reda V, et al. (2006) Prevalence of common mental disorders in Italy: results from the European Study of the Epidemiology of Mental Disorders (ESEMeD).Soc Psychiatry Psychiatr Epidemiol 41: 853-861.
- Lipton RB, Scher AI, Kolodner K, Liberman J, Steiner TJ, et al. (2002) Migraine in the United States: epidemiology and patterns of health care use. Neurology 58: 885-894.
- Dahl A, Campos JJ, Anderson DI, Uchiyama I, Witherington DC, et al. (2013) The epigenesis of wariness of heights. Psychol Sci 24: 1361-1367.
- WALK RD, GIBSON EJ, TIGHE TJ (1957) Behavior of light- and dark-reared rats on a visual cliff. Science 126: 80-81.
- Walk RD, Gibson EG (1961) A comparative and analytical study of visual depth perception. Psychol Monogr.
- GIBSON EJ, WALK RD (1960) The "visual cliff".Sci Am 202: 64-71.
- Adolph KE1 (2000) Specificity of learning: why infants fall over a veritable cliff. Psychol Sci 11: 290-295.
- Kretch KS, Adolph KE (2013) Cliff or step? Posture-specific learning at the edge of a drop-off. Child Dev 84: 226-240.
- Kretch KS, Adolph KE (2013) No bridge too high: infants decide whether to cross based on the probability of falling not the severity of the potential fall.Dev Sci 16: 336-351.
- Hiatt SW, Campos JJ, Emde RN (1979) Facial patterning and infant emotional expression: happiness, surprise, and fear. Child Dev 50: 1020-1035.
- Muris P, Merckelbach H, de Jong P, Ollendick TH (2002) The etiology of specific fears and phobias in children: a critique of the non-associative account. Behav Res Ther 40: 185-195.
- Coelho CM, Wallis G (2010) Deconstructing acrophobia: physiological and psychological precursors to developing a fear of heights. Depress Anxiety 27: 864-870.
- Menzies RG, Clarke JC (1993) The etiology of fear of heights and its relationship to severity and individual response patterns. Behav Res Ther 31: 355-365.
- Menzies RG, Clarke JC (1995) The etiology of phobias: a nonassociative account. Clin Psychol Rev 15: 23-48.
- Menzies RG (1997) Height phobia, in Phobias. A handbook of theory, research and treatment. Edited by Davey GLC. Chichester, Wiley 129-138.
- Poulton R, Menzies RG (2002) Non-associative fear acquisition: a review of the evidence from retrospective and longitudinal research. Behav Res Ther 40: 127-149.
- Skirbekk B, Hansen BH, Oerbeck B, Wentzel-Larsen T, Kristensen H (2012) Motor impairment in children with anxiety disorders. Psychiatry Res 198: 135-139.
- Emck C, Bosscher R, Beek P, Doreleijers T (2009) Gross motor performance and self-perceived motor competence in children with emotional, behavioural, and pervasive developmental disorders: a review. Dev Med and Child Neurol 51: 501-517.
- Erez O, Gordon CR, Sever J, Sadeh A, Mintz M (2004) Balance dysfunction in childhood anxiety: findings and theoretical approach. J Anxiety Disord 18: 341-356.
- Kugler G, Huppert D, Schneider E, Brandt T1 (2014) Fear of heights freezes gaze to the horizon. J Vestib Res 24: 433-441.
- Wuehr M, Kugler G, Schniepp R, Eckl M, Pradhan C, et al. (2014) Balance control and anti-gravity muscle activity during the experience of fear at heights. Physiol Rep 2: e00232.
- Kugler G, Huppert D, Eckl M, Schneider E, Brandt T1 (2014) Visual exploration during locomotion limited by fear of heights. PLoS One 9: e105906.
- Schniepp R, Kugler G, Wuehr M, Eckl M, Huppert D, et al. (2014) Quantification of gait changes in subjects with visual height intolerance when exposed to heights. Front Hum Neurosci 8: 963.
- Gonzalez A, Peris TS, Vreeland A (2015) Parental anxiety as a predictor of medication and CBT response for anxious youth. Child Psychiatry Hum Dev 46:84-93.
- Sandseter EB, Kennair LE (2011) Children's risky play from an evolutionary perspective: the anti-phobic effects of thrilling experiences.Evol Psychol 9: 257-284.
- Curtis GC, Magee WJ, Eaton WW, Wittchen HU, Kessler RC (1998) Specific fears and phobias. Epidemiology and classification.Br J Psychiatry 173: 212-217.
- Magee WJ, Eaton WW, Wittchen HU, McGonagle KA, Kessler RC (1996) Agoraphobia, simple phobia, and social phobia in the National Comorbidity Survey. Arch Gen Psychiatry 53: 159-168.
- Choy Y, Fyer AJ, Goodwin RD (2007) Specific phobia and comorbid depression: a closer look at the National Comorbidity Survey data. Compr Psychiatry 48: 132-136.
Relevant Topics
- Adolescent Anxiety
- Adult Psychology
- Adult Sexual Behavior
- Anger Management
- Autism
- Behaviour
- Child Anxiety
- Child Health
- Child Mental Health
- Child Psychology
- Children Behavior
- Children Development
- Counselling
- Depression Disorders
- Digital Media Impact
- Eating disorder
- Mental Health Interventions
- Neuroscience
- Obeys Children
- Parental Care
- Risky Behavior
- Social-Emotional Learning (SEL)
- Societal Influence
- Trauma-Informed Care
Recommended Journals
Article Tools
Article Usage
- Total views: 24806
- [From(publication date):
August-2015 - Aug 17, 2025] - Breakdown by view type
- HTML page views : 20059
- PDF downloads : 4747