Case Report Open Access
Hemosiderosis due to Chronic Alcoholism
Pinar Tosun Tasar1*, Ozlem Ozdemir1, Omer Binicier2 and Omer Selahattin Topalak2
1 Department of Internal Medicine, Dokuz Eylul University Faculty of Medicine, Izmir/Turkey
2 Department of Internal Medicine, Division of Gastroenterology, DokuzEylul University Faculty of Medicine, Izmir/Turkey
- *Corresponding Author:
- Pinar TosunTasar
Department of Internal Medicine
DokuzEylül University Faculty of Medicine, Izmir, Turkey
Tel: +9005053988985
E-mail: pinar.tosun@gmail.com
Received date: March 11, 2014; Accepted date: March 28, 2014; Published date: April 01, 2014
Citation: Tasar PT, Ozdemir O, Binicier O, Topalak OS (2014) Hemosiderosis due to Chronic Alcoholism. J Gastroint Dig Syst 4:182. doi:10.4172/2161-069X.1000182
Copyright: © 2014 Tasar PT, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
Alcoholic liver disease is characterized with excess consumption of alcohol for long term and variable hepatic injury. Chronic alcohol consumption often leads to a disease called alcoholic liver disease [ALD]. It is generally with an accompaning iron accumulation. Increased plasma iron levels and tissue iron overload stimulate synthesis of hepcidin, resulting with release of iron from macrophages and duodenal enterocytes to the plasma. This homeostasis ensures that plasma iron level is maintained within a constant range and excess absorption and accumulation of iron in tissues are prevented. Alcohol-induced oxidative stress in hepatocytes is one of the main mechanisms by which hepcidin expression in the liver is down-regulated by alcohol. The decrease in liver hepcidin synthesis leads to an increase in intestinal iron transport and liver iron content. We report a case hemosiderosis secondary to chronic alcoholism.
Keywords
Hepcidin; Hemosiderosis
Introduction
Chronic ethyl alcohol consumption damages almost all organs and tissues. Such effects are secondary to direct toxicity of alcohol and metabolites, while it is also known that intestinal absorption of folate and Vitamin B12 is impaired. In addition, it is found that free radicals play a role in tissue damage secondary to metabolism of alcohol.
Whatsoever the mechanism, chronic alcoholism results with many hepatic conditions ranging from fatty degeneration to cirrhosis, acute or chronic pancreatitis, alcoholic cardiomyopathy, and neurological lesions ranging from WernieckeKorsak of syndrome, peripheral neuropathy and cerebral and cerebellar atrophy, and gastritis, peptic ulcer and endocrine disorders such as testicular atrophy and amenorrhea [1,2].
Alcoholic liver disease is a clinical picture which is characterized with excess consumption of alcohol for long term and variable hepatic injury. Alcoholic liver disease is a condition which is due to cumulative alcohol intake for a long period of time and characterized by hepatic injury with a variable severity. Excess consumption of alcohol leads to Alcoholic Liver Disease [ALD] which is associated with excess iron accumulation and is characterized with hepatosteatosis, fibrosis, hepatitis and cirrhosis.
A derivative of denatured ferritin, referred as hemosiderin, accumulates in hepatic Kupffer cells, spleen and bone marrow in chronic hemolytic anemia, excess blood transfusion and various hepatic diseases. Hemosiderin is usually produced and microscopically determined in case of excess iron loading characterized with synthesis of apoferrin and maximal iron retention. Fe+3[Iron] accounts for 35% of molecular weight of hemosiderin; however, iron mobilization is slower in hemosidering in comparison with ferritin.
Hemosiderosis is a condition which is characterized with severe iron overload resulting with accumulation of hemosiderin in liver, pancreas, skin and joints. Increase in total total body iron and hemosyderin deposition at liver, pancreas, skin and articulations is described as hemosiderosis.Iron is accumulated in hepatocytes and Kupffer cells in alcoholic liver disease.
Case
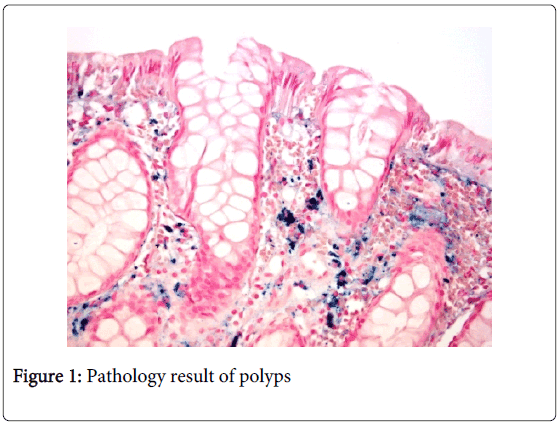
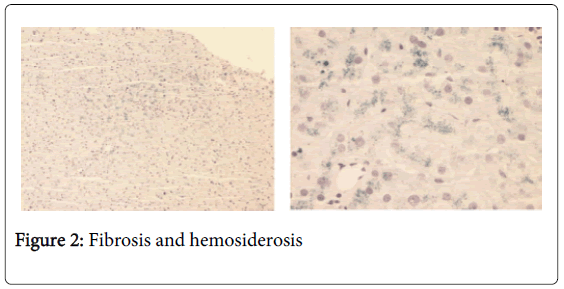
The 49 years old male patient has medical history of chronic ethyl alcohol consumption and the patient with lower gastrointestinal bleeding was hospitalized. On sigmoidoscopy, colon polyps and edematous hemorrhagic mucosa were found and pathology result of polyps was consistent with hemosiderosis (Figure 1). Although portal doppler ultrasonography [USG] was reported as normal there was diffuse hepatomegaly in abdominal USG. Biochemical serum analysis such as Iron:272µg/dL, total iron binding capacity [TIBC]:272 µg/dL, Saturation:100% and Ferritin:3249 ng/dl . Liver biopsy was performed since ferritin level was high and hemosiderosis was found in colon biopsy specimens. Liver biopsy indicated minimal portal and lobular inflammation, minimal steatosis, bridging fibrosis and hemosiderosis (Figure 2). Echocardiography, performed to eradicate the possibility of cardiac storage, was reported as otherwise normal than LVEF 60 %, mild tricuspid dysfunction and left ventricular dysfunction. Treatment was planned and the patient was consulted to alcohol cessation unit, and ferritin level of the patient, who avoided consumption of alcohol, regressed to174 ng/dL within two years. Hemosiderosis was not found in colon biopsies which were taken for control purposes.
Discussion
Chronic alcohol consumption is among leading causes of liver diseases in many countries. Hepatosteatosis, alcoholic hepatitis, hepatic fibrosis, cirrhosisis are found among the liver pathologies as a result of chronic alcohol consumption or addiction. Recently, effects of pathological changes caused by alcohol and oxidative stress on pathogenesis of such diseases are very often emphasized.
Ethanol is rapidly absorbed [90%] via gastrointestinal tract and metabolized in hepatic cells; it is oxidized to acetaldehyde by alcohol dehydrogenase, microsomal ethanol oxidixing system [MEOS] and catalase. Alcohol is metabolized by alcohol dehydrogenase [ADH] and cytochrome P4502E1 [CYP2E1] in the liver.Alcohol-induced oxidative stress leads to the suppression of hepcidin promoter activity and hepcidin transcription in the liver.The parenchymal, but not the non-parenchymal cells of the liver are involved in the regulation of hepcidin transcription by alcohol-induced oxidative stress [3].
It’s implicated that alcohol consumption leads to lipid peroxidation [LP] via induction of oxidative stress in hepatic and non-hepatic tissues[4]. In this reaction, NAD is reduced to NADH by alcohol dehydrogenase and oxidized to NAD by aldehyde oxidase in order to re-use it and reactive oxygen species are also synthesized [5]. MEOS is activated when blood and tissue alcohol level is >50 mg/dL; the enzyme has component of cytochrome p450 2 E1. Metabolization of alcohol with cytochrome P450 2E1 leads to synthesis of free oxygen radicals such as superoxide and hydroxyl.
At early phase of ethanol metabolism, which occurs usually in the liver, oxygen and nitric oxide radicals, synthesized with complete oxidation, and increased aldehyde levels dramatically change intra-cellular redox status [6].
In addition, it is suggested that ethanol and the principal metabolite, acetaldehyde, lead to synthesis of free radical species in tissues where they cannot be metabolized, and they may be responsible for alcohol-dependent toxicity and damage based on pro-oxidative effect in such tissues [7].
Alcohol intake affects a lot of iron parameters and alcohol addiction is observed more frequently in patients with excess iron.Increased serum ferritin concentrations are more often seen in cases of alcohol abuse.
In healthy persons, a fasting serum Transferrin saturation greater than 50% is abnormal and suggests for hemochromatosis.Transferrin saturationis used as indirect indicator of iron overload and it may increase in patients with alcoholic liver disease [8]. Severe iron accumulation is often encountered in patients with alcoholic liver disease [9,10]. Alcohol-dependent iron overload aggravates synthesis of free radicals and release of proinflammatory cytokines [11,12].However, the mechanism of accumulation of excess iron in patients with alcoholic liver is not yet illuminated.By the way, many studies show that hepcidin may have an important role in this process [13,14].
Hepcidin is an antimicrobial protein that is synthesized in the liver.However, the mechanism of accumulation of excess iron in patients with alcoholic liver is not yet illuminated.By the way, many studies show that hepcidin may have an important role in this process [15,16].Increased plasma iron levels and tissue iron overload stimulate synthesis of hepciding, resulting with release of iron from macrophages and duodenal enterocytes to the plasma. This homeostasis ensures that plasma iron level is maintained within a constant range and excess absorption and accumulation of iron in tissues are prevented [17,18].
Hepcidin whose synthesis is stimulated by the increase in plasma iron levels and iron stores in tissues, reduces the release of iron from duodenal enterocytes, macrophages to the plasma. This homeostasis ensures that plasma iron level is maintained within a constant range and excess absorption and accumulation of iron in tissues are prevented [19,20]. The liver-derived peptide hepcidin is the central regulator of iron homeostasis and recent animal studies have demonstrated that exposure to alcohol reduces hepcidin expression.This down-regulation of hepcidin in vivo implies that disturbed iron sensing may contribute to the hepatosiderosis seen in alcoholic liver disease [11].
Our case was deemed as hemosiderosis secondary to chronic alcoholism and combination of intestinal involvement and hemosiderosis in hepatic tissue further supports the relation between alcohol and hemosiderosis. On the other side, it was observed that iron levels are recovered to normal ranges when the patient quit alcohol, as indicated by one-year follow-up, and hemosiderin was not found in colonoscopic biopsy specimen, which was taken for control purpose.
References
- Cotran RS, Kumar V, Robbins SL(1989) Robbins Pathologic Basis of Disease, 4th ed. Philadelphia:Saunders 469-514.
- Edmondson HA (1980) Pathology of alcoholism. Am J ClinPathol 74: 725-742.
- Harrison-Findik DD (2009) Is the iron regulatory hormone hepcidin a risk factor for alcoholic liver disease? World J Gastroenterol 15: 1186-1193.
- Nordmann R, Ribière C, Rouach H (1992) Implication of free radical mechanisms in ethanol-induced cellular injury. Free RadicBiol Med 12: 219-240.
- Mira L, Maia L, Barreira L, Manso CF (1995) Evidence for free radical generation due to NADH oxidation by aldehyde oxidase during ethanol metabolism. Arch BiochemBiophys 318: 53-58.
- Zima T, Fialová L, Mestek O, Janebová M, Crkovská J, et al. (2001) Oxidative stress, metabolism of ethanol and alcohol-related diseases. J Biomed Sci 8: 59-70.
- Nordmann R, Ribière C, Rouach H (1990) Ethanol-induced lipid peroxidation and oxidative stress in extrahepatic tissues. Alcohol Alcohol 25: 231-237.
- Herbert V, Jayatilleke E, Shaw S, Rosman AS, Giardina P, et al. (1997) Serum ferritin iron, a new test, measures human body iron stores unconfounded by inflammation. Stem Cells 15: 291-296.
- Whitfield JB, Zhu G, Heath AC, Powell LW, and Martin NG (2001) “Effects of alcohol consumption on indices of iron stores and of iron stores on alcohol intake markers”. Alcohol ClinExp Res 25: 1037–1045.
- Duane P, Raja KB, Simpson RJ, Peters TJ (1992) Intestinal iron absorption in chronic alcoholics. Alcohol Alcohol 27: 539-544.
- Valerio LG, Parks T, and Petersen DR (1996) “Alcohol mediates increases in hepatic and serum nonheme iron stores in a rat model for alcohol-induced liver injury”. Alcohol ClinExp Research 20: 1352–1361.
- Lin M, Rippe RA, Niemelä O, Brittenham G, Tsukamoto H (1997) Role of iron in NF-kappa B activation and cytokine gene expression by rat hepatic macrophages. Am J Physiol 272: G1355-1364.
- Harrison-Findik DD (2009) Is the iron regulatory hormone hepcidin a risk factor for alcoholic liver disease? World J Gastroenterol 15: 1186-1193.
- Flanagan JM, Peng H, Beutler E (2007) Effects of alcohol consumption on iron metabolism in mice with hemochromatosis mutations. Alcohol ClinExp Res 31: 138-143.
- Pigeon C, Ilyin G, Courselaud B, Leroyer P, Turlin B, et al. (2001) “A new mouse liver-specific gene, encoding a protein homologous to human antimicrobial peptide hepcidin, is overexpressed during iron overload”. J BiolChem11: 7811–7819.
- Park CH, Valore EV, Waring AJ, Ganz T (2001) Hepcidin, a urinary antimicrobial peptide synthesized in the liver. J BiolChem 276: 7806-7810.
- Nicolas G, Viatte L, Bennoun M, Beaumont C, Kahn A, et al. (2002) Hepcidin, a new iron regulatory peptide. Blood Cells Mol Dis 29: 327-335.
- Nemeth E, Tuttle MS, Powelson J, Vaughn MB, Donovan A, et al. (2004) Hepcidin regulates cellular iron efflux by binding to ferroportin and inducing its internalization. Science 306: 2090-2093.
- Harrison-Findik DD, Schafer D, Klein E, Timchenko NA, Kulaksiz H, et al.(2006) “Alcohol metabolism-mediated oxidative stress down-regulates hepcidin transcription and leads to increased duodenal iron transporter expression”. J BiolChem281: 22974–22982.
- Rossi E (2005) Hepcidin--the iron regulatory hormone. ClinBiochem Rev 26: 47-49.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 22999
- [From(publication date):
April-2014 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 18270
- PDF downloads : 4729