Case Report Open Access
Immediate Effects of Acute Postural Correction on Plantar Pressures and Gait Characteristics in an Individual with Diabetic Peripheral Neuropathy: A Case Report
| Andrea Franz, Greg Rickert and Mansoo Ko* | |
| Assistant Professor, Doctor of Physical Therapy Program, Angelo State University Member, Texas Tech University System, ASU Station #10923, San Angelo, TX 76909- 0923, USA | |
| Corresponding Author : | Mansooko, PT, Ph.D Assistant Professor Doctor of Physical Therapy Program Angelo State University Member, Texas Tech University System ASU Station #10923, San Angelo, TX 76909-0923, USA Tel: (325) 942-2579 Fax: (325) 942-2548 E-mail: mko@angelo.edu |
| Received May 06, 2013; Accepted June 12, 2013; Published June 14, 2013 | |
| Citation: Franz A, Rickert G, Ko M (2013) Immediate Effects of Acute Postural Correction on Plantar Pressures and Gait Characteristics in an Individual with Diabetic Peripheral Neuropathy: A Case Report. J Nov Physiother 3:152. doi:10.4172/2165-7025.1000152 | |
| Copyright: © 2013 Franz A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
Purpose: The purpose of this case report is to assess the immediate effects of acute postural changes on plantar pressure distribution and gait characteristics during comfortable walking speed in an individual with diabetic peripheral neuropathy.
Case description/intervention: Subject is a 71 year old Caucasian male with a BMI of 31.3 and a medical diagnosis of Type II Diabetes given 8 years ago. The patient exhibits mild peripheral neuropathy as scored by the Michigan Neuropathy Screening Instrument (MNSI; 7/23) as well as callous formation over the 2nd and 3rd metatarsal heads. The patient performed 3 separate walking conditions at a comfortable walking speed. The 3 conditions were: (1) Normal walking (NW), (2) Forward bending walking (FBW), and (3) Upright walking (UW). Measurements were recorded and averaged from these 3 conditions. NW condition was used as a control for comparing gait characteristics and plantar pressure parameters with the other gait conditions.
Results: UW may be the most mechanically efficient condition for distributing plantar pressure with increased gait speed (1.441 m/s), largest contact surface area of the foot, and increased hip range of motion; however, for this individual the increased plantar pressure in the forefoot (FF) area may contribute to the risk of ulceration. The FBW condition showed the limited medial to lateral excursion of the center of forceand lowest pressure in the FF area; therefore, FBW may be the most beneficial for this patient in decreasing the risk of ulceration in the area of greatest concern.
Conclusion: Variations in gait characteristics during UW and FBW indicate that alterations in posture may serve as another method to reduce the risk of plantar ulcer formation; however, further research is needed to examine the long term effects of such an intervention.
| Introduction |
| Diabetes in the United States is prevalent, costly, and associated with serious health complications. According to the most recent comprehensive report on diabetes from the Center for Disease Control, [1] diabetes has become the seventh leading cause of death in the US, affecting 23.6 million people (7.8% of the US population) and is expected to rise to 48 million by the year 2050 [2]. Every 24 hours in the US there are 4,100 new cases of diabetes diagnosed; of those new cases, 810 people will die, 230 people will have an amputation, 120 people will require kidney dialysis or transplant, and 55 people will go blind [2]. Annual health costs of a person with type 2 diabetes is 2.3 times the average American without the disease [1]. The estimated total cost of diabetes in the US during 2007 was $174 billion, 67% of which is “direct” or medically related [1]. |
| Diabetes has been associated with lower limb muscle dysfunction3 and abnormal plantar pressures in the foot, [3-5] resulting in ulcerations in plantar integumentary tissue, [4] gait abnormalities, [3] increased risk for falls, [6] and decline in function [7]. Neuropathy is the greatest risk factor for ulceration in patients with diabetes [8]. Peripheral sensory neuropathy usually affects the lower extremities resulting in a loss of vibration sense, proprioception, temperature, light touch, and eventually pain sensation. In effect, individuals with diabetic peripheral neuropathy may have a diminished or absent ability to respond to potentially injurious stimuli, such as increased shear force and elevated or prolonged peak plantar pressure [9]. People with diabetes and peripheral neuropathy exhibit increased plantar pressures especially at the forefoot [10-14]. Increased plantar pressure increases the risk for tissue breakdown and ulceration [11,13]. |
| The progressive loss of protective sensation and muscle function in the lower limbs that is associated with Diabetic Peripheral Neuropathy (DPN) may cause an alteration of motor control such as decreased muscle activation timing due to slow or absent sensory input that may ultimately lead to poor locomotor propulsion or decreased postural stability duringgait or static posture [4]. Patients with DPN have increased fall occurrence, [15] slower walking velocity [16,17], shorter step and stride length [16,17], decreased ankle range of motion [17], and longer double support time [18] when compared to normal agematched controls. By studying the kinetic and kinematic properties of gait in individuals with diabetic peripheral neuropathy, researchers may be able to infer effective interventions in order to prevent foot pathologies associated with gait abnormalities. |
| The cause and effect relationship between increased plantar pressure and ulceration has become the focus in research for prevention and treatment of ulcers [19]. Therefore, the primary target for prevention and healing of neuropathic plantar ulcers is a pressure relief during walking. Kwon et al. [5] defined plantar pressure as Pressure=Force/Area, where forcedescribesthe ground reaction force (GRF) exerted upwards from the ground through the foot during walking and area describes the surface area of the foot that is in contact with the ground during walking. It stands to reason that pressure reduction can occur bydecreasingthe GRF or increasingthecontact area of the foot. Many strategies are currently used to decrease peak plantar pressures during walking for people with diabetic neuropathies such as casting, insoles, rocker shoes, and customized shoes;[19] however, few studies have documented the effect of postural reeducation training and its impact on muscle and gait performance. |
| Increased forward head posture and thoracic kyphosis are the most noticeable and commonly acknowledged postural changes in older adults [20,21]. According to Saha et al. [22] anterior translation of the body’s center of mass caused by forward bending during gait results in kinematic changes (i.e. increased cadence, decreased step length, decreased hip range of motion, decreased push-off force) for which the body will attempt to compensate (i.e. crouched gait). Increased cadence and stance time has been associated with higher plantar pressures [23]. Hirose et al. found that elderly individuals with thoracic kyphosis have shorter stride and step length, longer step width, longer stride time and double stance time, and slower gait speed [21]. Many of these gait characteristics are presentin individuals with DPN; therefore, by changing an individual’s posture during gait it may be possible to improve gait biomechanics and decrease peak plantar pressure, thereby decreasing the risk of ulceration associated with DPN. |
| The purpose of this case study is to assess plantar pressure distribution and gait characteristics during a comfortable walking speed in relation to acute posture changes in an individual with DPN. |
| Case Description |
| The subject is a 71 year-old Caucasian male diagnosed with type II diabetes mellitus (DM) 8 years ago. He has also been diagnosed with DPN and is currently under the care of a physician for his neuropathy. He has a past medical history of lymphoma and hypertension and he underwent surgery on April 15, 2009 for removal of lymphoma from his chest. There has been no evidence of lymphoma since this procedure. The subject denies using an assistive device for ambulation or having ever had an ulcer on his feet. He is allergic to sulfa based medications and hydrocodone. He is currently taking 2mg Amaril twice per day for diabetes, Diovan for hypertension, and symvastatin for cholesterol management. He also takes Tylenol, and 900 mg of gabapentin as directed by his physician for neuropathy. He is 5 ft 10 in tall and weighs 218 lbs. He is retired and lives at home in a one-story, ranch-style house with his wife. The patient is right foot dominant. |
| Examination |
| The subject was first asked to sign an informed consent form to participate in the study which stated: (1) the purpose of the study, (2) explanation of the procedures, (3) benefits and risks for the subject, (4) confidentiality statement, and (5) refusal/withdrawal policy. After signing this informed consent form,a thorough history and physical examination were used to determine the severity of the subject’s DPN. A patient demographic form was used for recording subject history and current medication. Height and weight were measured and recorded and BMI was calculated from these measurements. Photographs were taken of the plantar aspect of the subject’s right foot using a digital camera. The subject was then screened and evaluated for peripheral neuropathy and other foot abnormalities using the Michigan Neuropathy Screening Instrument (MNSI) and vibration and monofilament sensation testing on the plantar surface of the foot. |
| The MNSI is a screening instrument designed to screen for the presence of DPN in an outpatient setting by health care providers. The first part of the MNSI consists of 15 self-administered “yes or no” questions on foot sensation including pain, numbness, and temperature sensitivity. A higher score on this portion indicates more severe neuropathic symptoms. The questions were chosen from among those in the Neuropathy Screening Profile of Peter Dyck that showed the highest degree of specificity and sensitivity for DPN among normal subjects and those with a variety of neuromuscular disorders [24]. The second part of the MNSI is a brief physical exam involving: (1) inspection of the feet for (a) deformities, (b) dry skin, (c) hair or nail abnormalities, and (d) callus or infection;(2) assessment of vibration sensation at the dorsum of the great toe; (3) grading of ankle reflexes; and (4) monofilament testing. A positive screen, greater than a score of 2/10, indicates neuropathy and the patient should be referred for further testing if he/she has not already done so. |
| Lunetta et al looked at the reliability and reproducibility of the MNSI on 80 diabetic patients and found the inter-observer reproducibility to be 88.75% and the intra-observer reproducibility was 95 and 94% respectively for each observer with good correlation between the two measurements (p<0.001) [25]. They concluded that by using a score of 2.5 as a cut-off on the second portion of the screen, the MNSI may be considered a rapid, simple, reproducible and reliable test for rapid ambulatory screening of PDN.25Moghtaderi and colleagues found sensitivities of 79%, 65%, 50% and 35% and specificities of 65%, 83%, 91%, and 94% for MNSI scores on the second portion of the screen of 1.5, 2.0, 2.5, and 3.0 respectively [26]. They concluded that the accuracy of the MNSI makes it a useful screening test for DPN. |
| Vibration and monofilament sensation testing are commonly used in screening and evaluation of plantar surface sensation. Perkins et al conducted a study to assess the operating characteristics of the 10 g Semmes-Weinstein monofilament examination (SWME), superficial pain sensation, vibration testing by the on-off method with a 128 Hz tuning fork, and vibration testing by the timed method with a 128 Hz tuning fork in 478 subjects with independent blinded evaluations as compared with standardized electrophysiological tests in the diagnosis of distal symmetrical polyneuropathy [27]. They found the point estimates of the positive likelihood ratios for vibration testing by the on-off method, vibration testing by the timed method, the SWME, and superficial pain sensation test to be 26.6, 18.5, 10.2, and 9.2, respectively. The point estimates of the negative likelihood ratios were 0.33, 0.51, 0.34, and 0.50, respectively, and the screening tests showed comparable sensitivity and specificity results. The authors conclprevious study inidicated that annual screening for DPN should be conducted using superficial pain sensation testing, SWME, or vibration testing by the on-off method and that the findings from these techniques could be used in the assessment of DPN similarly to that of electrophysiological tests [27]. For the purposes of this study, vibration sensation was assessed using a 128 HZ tuning fork using the on-off method and sensation to light tough was assessed with the 10 g SWME. |
| The distribution of plantar pressure during the intervention conditions was monitored by Tekscan HR Mat (Tekscan Inc; South Boston, Massachusetts) and gait characteristics were analyzed via VICON Motion Analysis System (VICON Inc; Los Angeles, California) as the subject walked across the 15-m walkway. The Tekscan HR Mat is a digital pressure mapping system that analyses plantar pressure and center of pressure sway characteristics during walking trials. Using the average of 5 walking trials enhances the reliability of the pressure measurement, although 100% replicability cannot be expected because of inherent differences in each walking trial [28]. The system displayed moderate to good reliability of mean and mediancalculations for the three analyzed variables across all seven regions, as indicated byintra-class correlation coefficients ranging from 0.44 to 0.95 for the mean and 0.54 to 0.97 for the median, and coefficients of variation ranging from 5 to 20% for the meanand 3 to 23% for the median in a study by Zammit et al. [29]. Data obtained from a plantar pressure assessment can be used by the physical therapist and podiatrist in the evaluation and management of patients with a wide variety of foot and lower-extremity disorders associated with the neurological, integumentary, and musculoskeletal systems [28]. Unlike the force platform, pressure systems measure only vertical force, but they provide the clinician or researcher with information regarding the effects of various interventions, including use of footwear, foot orthoses, gait training, and surgical management, on forces and pressures applied to specific locations of the foot [28]. |
| The VICON MX Motion Analysis System is a state-of-the-art optical,three-dimensional motion capture system comprised of 8 cameras, a controlling hardware module, and a computer software package, all contained in a controlled laboratory setting. In addition to the VICON system, two Kistler force plates (Kistler Instrument Corp; Amherst, New York) were used to obtain GRF data.VICON has been used in previous studies as a “gold standard” of comparison to determine validity and reliability of other instruments (i.e. GaitMat II, Kinematic Support System, GAITRite, and Global Positioning System) [30-33]. VICON has been shown to have high reliability and validity with an extremely small error range for angle and distance measures (0.16-0.18 degrees and 0.42-0.50 mm respectively) [34,35]. |
| The VICON’s 8-camera system utilizes infrared technology and reflective markers to capture real-time kinetic and kinematic data during full-body motion (i.e. barefoot walking), which is later analyzed using dynamic plug-in gait protocol. Each marker was attached to the skin via double-sided adhesive tape with the exception of the shoulder, trunk, and pelvic markers. These markers were attached to the subject’s clothing in a manner that would minimize error (clothing pulled taut to prevent movement). The subject was prepared and the VICON system was calibrated as indicated by the manufacturer [36] prior to all data collection trials. |
| Evaluation |
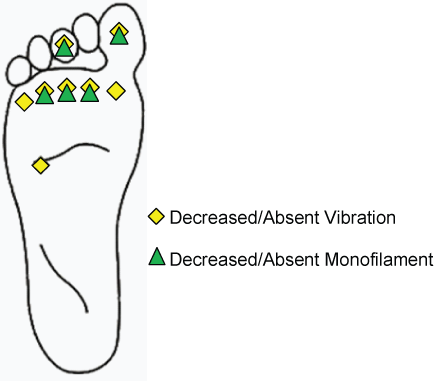
| The subject’s BMI was calculated from height and weight measurements to be 31.3 placing him in the obese category [37]. This along with the diagnosis of type II DM and resultant diagnosis of DPN are poor overall health indicators. Upon physical examination a callus formation was noted over the 2nd metatarsal head of the right foot which indicates increased pressure in this area. The subject scored 4/13 on the self-administered portion of the MNSI and his response to item No. 4 indicates the presence of impaired circulation. He scored 3/10 on the physical assessment portion of the MNSI yielding an overall score of 7/23. This score was then converted into a percentage of severity placing him in the mild DPN category. See Figure 1 for results from vibration sensation and 10 g monofilament sensation testing. |
| According to The Task Force of the Foot Care Interest Group of the American Diabetes Association [38] this subject has two risk factors for plantar ulceration present: |
| • Peripheral neuropathy |
| • Foot deformity in the form of a callus |
| These findings from the examination would place this subject in the mild risk category due to loss of protective sensation and presence of foot deformity [11]. |
| Diagnosis and Prognosis |
| The subject has a pre-existing medical diagnosis of Diabetes Mellitus Type II with neurological manifestations (ICD-9 Code: 250.6) which is confirmed by our findings through examination. According to the Guide to Physical Therapist Practice, this subject falls into Practice Pattern 5G: Impaired Motor Function and Sensory Integrity Associated with Acute or Chronic Polyneuropathies [38]. |
| If this patient were seeking gait training in the out patient physical therapy clinic, the appropriate amount of visits would be in the range of 6-24 [38]. However, this case study is based on a single instance of time and therefore will only include one session for intervention and outcome measurement. |
| Intervention |
| An initial gait observation was conducted at a self-selected, comfortable walking pace for the subject in order to monitor the subject for potential safety concerns during walking. The subject was then instructed to perform 3 different barefoot walking conditions at a comfortable speed over a 15-m walkway: (1) Normal (NW), (2) Forward bending (FBW), and (3) Upright (UW). In NW, the subject was instructed to walk comfortably as they would in the community. In FBW, he was instructed to walk while maintaining a hip flexion angle of 25 degrees measured via goniometer prior to ambulating. In UW, he was instructed to walk as if a string was pulling his chest straight up towards the ceiling, keeping his head facing forward. Each condition was repeated 3-5 times and an average of the trials was used for data calculation. |
| During each condition, plantar pressure was assessed using the Tekscan HR Mat. Video recording and digital analysis of the subject’s lower extremity and trunk position via VICON Motion Analysis System was used to assist investigators with evaluation of gait characteristics. Abnormalities or deviations during trials were recorded when missteps or stutter steps occurred and that trial was thrown out of the data due to deviations. For purposes of recording plantar pressure distribution, the foot was broken into 3 sections: (1) forefoot (FF), (2) midfoot (MF), (3) rearfoot (RF). Maximum plantar pressure (MPP) will be the two key measurements of concern, especially in the area of the FF and the callus. For purposes of gait characteristics, VICON Motion Analysis System was used to focus on kinematic data such as cadence, double and single leg support time, walking speed, stride time, swing time, step length, stride length, and hip flexion and extension sduring all trials in all three conditions. The normal walking trials were used as the subject’s “control” condition and changes that occurred during the other two walking conditions were to be compared to the normal condition as well as to each other. |
| Outcomes |
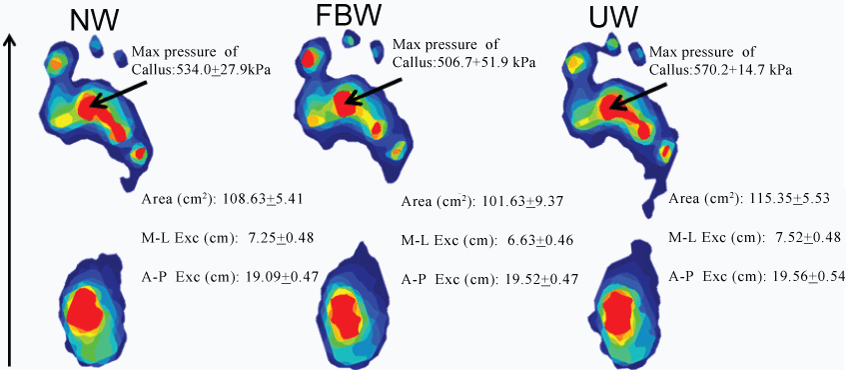
| The area of greatest concern for this subject is the 2nd-4th metatarsal heads due to callus formation and decreased sensation to vibration and monofilament. Therefore the focus of the results will be changes in the area of the FF and the callus. Tekscan HR Mat was used to observe changes in max plantar pressure (KPa) (Figures 1 and 2) in the areas of the FF and callus especially as well as to evaluate the center of pressure sway analysis during the [3] gait conditionstrials (Fgure 2). VICON Motion Analysis System was used to assess changes in gait characteristics during the 3 trials (Table 1). A compensatory increase in plantar pressure in the area of the great toe was noted during FBW and was greater in this condition as compared to the other two conditions. |
| UW revealed the most even distribution of pressure over the greatest surface area of the foot (115.4 cm2) with wider M-L exc (7.52 cm) during barefootwalking trials. FBW yielded the lowest pressure on the FF (276.1 ± 12.0 KPa), but decreased surface area of the foot (101.6 cm2) and limited M-L exc (0.63 cm). In the area of the callus, the FBW resulted in the lowest max pressure (506.7 ± 52.0 KPa). FBW showed the greatest decrease in plantar pressure in the area of the callus and the FF. However, the UW condition was the most efficient at evenly distributing pressure over a greater surface area with a decreased time of exposure to pressure on the FF. These results can be seen in Figure 2. |
| Compared to NW, FBW condition showed increased cadence (121 steps/min), gait speed (1.41 m/s), step length (0.698 m), stride length (1.399 m), gait cycle (1.410 sec) but hip extension (15.7°) were decreased. The UW condition showed that cadence (121 steps/min), walking speed (1.441 m/sec), step length (0.726 m) and stride length (1.465 m), and hip range of motion (flexion 25.2°; extension 22.6°) was increased while gait cycle time (1.012 Sec), and double support time (19% GC) were decreased when compared to NW. Please refer to Table 1. |
| Discussion |
| This case study analyzes the potential usefulness of acute postural changes on plantar pressure distribution during comfortable walking speed in an individual with diabetic peripheral neuropathy. The results of this study indicate that changing an individual’s posture during gait from normal to either forward-bent or upright will alter peak plantar pressure a as well as gait kinetics and kinematics. UW appears to be the most mechanically efficient condition for distributing plantar pressure due to increased gait speed and largest contact surface area of the foot; however, for this individual, the increased plantar pressure in forefoot area may contribute to the risk of ulceration. The FBW condition showed the lowest pressure in the forefoot area; butthe impracticality and inefficiency of this walking condition preclude its use as a viable means to prevent ulceration [21-23]. |
| The UW condition is potentially more efficient and beneficial in this case as a means to facilitate improved gait biomechanics and plantar pressure distribution [39-42]. Increased forefoot peak plantar pressure is higher in UW possibly due to a greater walking speed, resulting in a more forceful push-off phase of gait [43,44]. Faster selfselected gait speed, thus higher push-off force, has been associated with upright posture [21]. |
| The effect of postural reeducation training during gait has not been studied extensively; however, other interventions may prove to be effective in reducing the risk of ulceration. Allet et al. studied the benefits of an exercise intervention to improve diabetic patient’s gait in a real-life environment [45]. Gait characteristics were determined during an outdoor gait assessment over even and uneven terrain using miniature gyroscopes attached to each leg. Training involved twiceper- week sessions of group therapy with a 60-minute duration for a total of 12 weeks. Dropout was small and exercise adherence ranged from 11 to 24 treatments, which were comprised of: (1) five-minute warm up of different walking modes and different velocities, and exercise for general mobilization for trunk and limbs, (2) forty-minute circuit training (10 tasks of either balance and walking tasks, or functional strength-endurance exercises), (3) ten-minute interactive team game such as badminton or obstacle race, and (4) feedback concerning the training session and individual suggestions for home exercises. The intervention group lost some of the treatment benefit after six-month follow-up, but their performance level remained superior to baseline. On both terrains, the intervention group showed increased habitual walking speed and significant improvement in cadence, gait cycle time, and stance time. Plantar pressure was not analyzed in this study; however, one could speculate that improving gait characteristics that are associated with increased plantar pressure may result in a reciprocal improvement in plantar pressure distribution. |
| Other methods of evaluating plantar pressure exist besides an expensive, computerized pressure map. Menz and Morris conducted a study to determine which clinical tests could predict plantar pressure during walking in older adults [46]. They found that structural foot and ankle characteristics identified from clinical measurements, such as the arch index and metatarsophalangeal joint range of motion, can explain some key aspects of plantar loading patters of the foot [46]. Additionally, plantar fascia plays a key role in shock absorption during walking. A study by D’Ambrogi et al. found that diabetics develop thicker plantar fascial tissue, which can adversely alter foot structure and conformity while in contact with the ground [47]. Impaired tissue extensibility will result in higher plantar pressures [47]. Perhaps a soft-tissue mobilization technique could be a useful intervention to increase plantar fascial tissue extensibility. D’Ambrogi et al. also found that individuals with diabetes can present with increased plantar pressure in the absence of peripheral neuropathy [47]. |
| There are two important limitations to this study. First, only a single instance intervention was used for a single individual; thus, the potential for lasting benefit over time as well as generalization to other subjects could not be determined. Human gait is a dynamic, highlyrefined motor skill that requires cardiovascular fitness, stability and elasticity of peripheral musculoskeletal elements, and functioning neural mechanisms; [48] therefore, effective interventions must be comprehensive in nature [45] and promote lasting benefits [49]. |
| The second limitation pertains to the gait laboratory, which is a controlled environment with good lighting, a level surface, and a short distance for ambulation–not comparable to all “real-world” situations. DeMott et al. studied falls in older persons with peripheral neuropathy to identify gait characteristics on smooth versus irregular surfaces associated with falls [15]. The gait lab in this study utilized low lighting (50 lux) and irregular surface to simulate a “real-world” environment. The walkway was covered with industrial carpet with randomly placed prism-shaped pieces of wood (1.5 cm×3.5 cm×6-16 cm) under the carpet to create the surface irregularities. This study concluded that peripheral neuropathic persons have a high rate of falls, which are often associated with walking on irregular surfaces; thus, gait analysis on an irregular surface may be superior to that on a smooth surface for detecting fall risk [15]. |
| Conclusion |
| Variations in gait characteristics during UW and FBW indicate that alterations in posture may serve as another method to reduce the risk of plantar ulcer formation by dispersing plantar pressures in a more even distribution over a greater surface area. UW redistributes plantar pressure over a greater surface area of the foot, thereby decreasing the occurrence of forefoot peak plantar pressure over a small surface arearesulting in a decrease in risk of plantar ulceration. Future studies should look at postural education and gait training as a treatment technique for redistributing plantar pressures in a larger study population. Further research is also needed to examine the long term effects of such an intervention. |
| Grant and Financial Support |
| This material is the result of work supported with resources and the use of facilities at the Physical Therapy Program, Angelo State University. |
References |
|
Tables and Figures at a glance
| Table 1 |
Figures at a glance
 |
 |
| Figure 1 | Figure 2 |
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 15861
- [From(publication date):
May-2013 - Aug 28, 2025] - Breakdown by view type
- HTML page views : 11212
- PDF downloads : 4649
