Case Report Open Access
Lighting on PET Scan-Not Always Cancer
Valentin Zumstein*, Martin Bolli and Michael Manz
Department of Surgery, 27 Department of Gastroenterology and Hepatology, St. 8 Claraspital Basel, 4058 Basel, Switzerland
- Corresponding Author:
- Valentin Zumstein
Department of Surgery, 27 Department of Gastroenterology and Hepatology
St. 8 Claraspital Basel, 4058 Basel, Switzerland
Tel: 0041616858585
E-mail: valentin.zumstein@gmail.com
Received Date: October 19, 2014; Accepted Date: January 24, 2015; Published Date: January 30, 2015
Citation: Zumstein V, Bolli M, Manz M (2015) Lighting on PET Scan-Not Always Cancer. J Gastrointest Dig Syst 5:250. doi:10.4172/2161-069X.1000250
Copyright: © 2015 Zumstein V, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
A PET scan showing a hypermetabolic focus in the gastric antrum is suspicious of gastric cancer. Nevertheless other reasons should be kept in mind in the differential of gastric tumors as for example gastric mucosal prolapse polyps.
Presentation of case: A 84-year-old woman had been scoped at a referring hospital due to lower gastrointestinal bleeding. The external gastroscopy revealed an indistinct tumor in the area of the gastric antrum.
An obtained PET scan showed a hypermetabolic focus in the antrum. At our hospital we repeated gastroscopy, the antral mass had no malignant aspect but looked like thickened mucosal fold partially prolapsing in the duodenal bulb, the biopsies ruled out cancer and showed polypous foveolar hyperplasia consistent to an antral mucosal prolapse polyp. The patient could be discharged on PPI therapy.
Keywords
PET; Gastric cancer; Mucosal prolapse polyp
Introduction
In 2012, gastric cancer was the sixth commonest cancer diagnosis and the fourth commonest cause of cancer-related death across all European countries 1. Diagnosis should be made from endoscopy and endoscopic biopsy, computed tomography (CT) and endoscopic ultrasound (EUS); Positron emission tomography (PET) imaging may improve staging if available. A hypermetabolic mass causing lighting on PET scan can be explained due to infections, local inflammation or cancer.
Case Report
An 84-year old woman had been scoped at a referring hospital due to lower gastrointestinal bleeding. The bleeding was attributed to diverticular disease or hemorrhoids and self-limited. Surprisingly and asymptomatic, the external Gastroscopy revealed an indistinct tumor in the area of the gastric antrum, highly suspicious of gastric cancer and the patient was referred to our hospital for further staging.
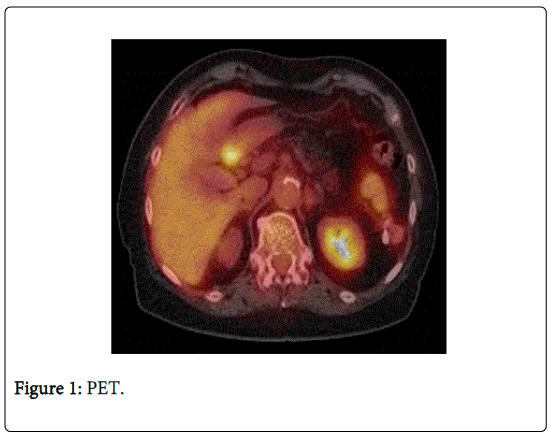
PET scan showed correspondingly a hypermetabolic focus in the antrum but no distant metastases (Figure 1).
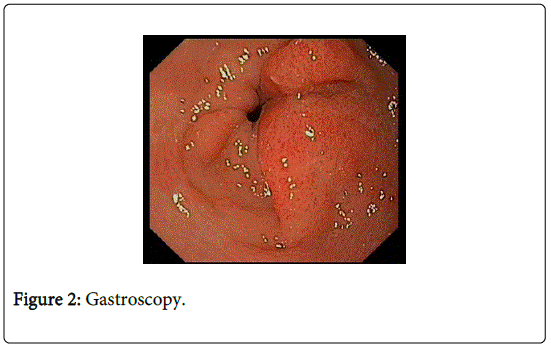
At our hospital, we repeated gastroscopy and performed radial endosonography for further staging. The antral mass had no malignant aspect but looked like a thickened mucosal fold partially prolapsing in the duodenal bulb (Figure 2). Endosonography revealed no signs of invasion.
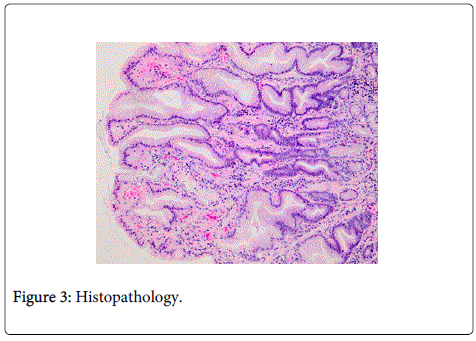
The macroscopic suspected gastric mucosal prolaps polyp was confirmed on histology. The biopsies ruled out cancer and showed polypous foveolar hyperplasia with moderate chronic inflammation and marked myofibrosis of the lamina propria, consistent to an antral mucosal prolapse polyp (Figure 3). The unburdened patient could reassured and discharged on PPI therapy.
Hyperplastic polyps represent the second most common subtype of gastric polyps and are mostly found incidentally during endoscopies [1]. They can be sessile or pedunculated and are predominantly located in the antropyloric region. Histology typically shows basal glandular elements, hypertrophic muscle fibers ascending perpendicularly from the muscularis mucosae and thick-walled blood vessels.
FDG-PET/CT has demonstrated clinical utility in detection, staging, and follow-up of tumors, infections as well as sterile inflammation, including intestinal track inflammatory entities [2]. The molecular substrate for increased FDG-uptake at sites of infection or inflammation has been attributed to the overexpression of distinct facultative glucose transporter (GLUT) isotypes (mainly GLUT-1 and GLUT-3) and by an overproduction of hexokinase in inflammatory cells - stimulated macrophages, lymphocytes and neutrophils [3]. The inflammation leads to high intracellular accumulation of FDG depending upon the degree of stimulation [4]. We consider that the gastric focal hypermetabolism described in our case could be explained based on this biological phenomenon and also by an increased cell-density in the context of foveolar hyperplasia and marked myofibrosis (described on histopathology).
The predominantly antral location of gastric mucosal prolapse polyps, a zone of intense peristalsis, suggests that prolapse plays a role in the development of these polyps [5].
Gastric mucosal prolaps polyps are rare but should be kept in mind in the differential of gastric tumors.
The authors thank PD Dr. A. Zettl for providing the histologic Figures.
Discussion
Hyperplastic polyps represent the second most common subtype of gastric polyps, predominantly located in the antropyloric region and are mostly found incidentally during endoscopies. The predominantly antral location of gastric mucosal prolapse polyps, a zone of intense peristalsis, suggests that prolapse plays a role in the development of these polyps. Gastric mucosal prolapse polyps are rare but should be kept in mind in the differential of gastric tumors.
References
- Carmack SW, Genta RM, Graham DY, Lauwers GY (2009) Management of gastric polyps: a pathology-based guide for gastroenterologists. Nat Rev GastroenterolHepatol 6: 331-341.
- Bettenworth D, Reuter S, Hermann S, Weckesser M, Kerstiens L, et al. (2013) Translational 18F-FDG PET/CT imaging to monitor lesion activity in intestinal inflammation. J Nucl Med 54: 748-755.
- Meller J, Sahlmann CO, Scheel AK (2007) 18F-FDG PET and PET/CT in fever of unknown origin. J Nucl Med 48: 35-45.
- Basu S, Kumar R, Alavi A (2010) PET and PET-CT imaging in infection and inflammation: its critical role in assessing complications related to therapeutic interventions in patients with cancer. Indian J Cancer 47: 371-379.
- Gonzalez-Obeso E, Fujita H, Deshpande V, Ogawa F, Lisovsky M, et al.(2011)Gastric hyperplastic polyps: a heterogeneous clinicopathologic group including a distinct subset best categorized as mucosal prolapse polyp. Am J SurgPathol 35: 670-677.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 20485
- [From(publication date):
February-2015 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 15838
- PDF downloads : 4647