Lipomata of the Brachial Plexus Causing Neurogenic and Venous Thoracic Outlet Syndrome: Case Reports and Review of the Literature
Received: 26-Mar-2016 / Accepted Date: 21-Apr-2016 / Published Date: 22-Apr-2016 DOI: 10.4172/2161-0681.1000270
Abstract
Compression of the brachial plexus causing neurogenic symptoms is a common presentation in the majority of cases referred to vascular surgeons with thoracic outlet syndrome. The causative factor of the compression can be difficult to diagnose with multiple pathologies implicated. Lipomas are benign soft tissue tumours with progressive expansion in volume. Along with frequently aesthetic consequences, lipomas can also apply extrinsic pressure on surrounding tissues and structures especially in constrained space and outlets in body. Lipomas causing brachial plexus compression are rare; fourteen cases have been described in the literature worldwide. We present two cases of supraclavicular lipomata causing compression of the neurovascular structures in the thoracic outlet. We highlight that there are a small number of neurogenic thoracic outlet syndrome (N-TOS) cases where the pathology is managed wholly by surgery and good recovery can be expected.
Keywords: Thoracic outlet syndrome; Neurogenic; Venous; Lipoma; Brachial plexus
313186Introduction
Thoracic outlet syndrome (TOS) affects approximately 8% of the population with a female to male ratio of up to 4:1. Almost all cases of TOS (95-98%) affect the brachial plexus, with only 2-5% affecting vascular structures. Common congenital causes of N-TOS are structural anomalies such as clavicular deformity, cervical ribs, anomalous fibromuscular bands, or hypertrophy/injury to the scalene musculature. Acquired causes such as repetitive strain injury and trauma have also been implicated. Diagnosing neurogenic thoracic outlet syndrome (N-TOS) can pose a challenge for the vascular surgeon. Standard techniques include plain thoracic outlet view x-ray, duplex ultrasound to exclude vascular compromise, magnetic resonance imaging and electrophysiology studies. Surgical results from brachial plexus neurolysis, scalenectomy and first rib resection are variable as reviewed by Balci et al. [1]. We present two cases where lipomata of brachial plexus compression were demonstrated and TOS repair (scalenectomy, neurolysis, 1st rib resection) with excision of lipomata led to relief of neurological symptoms.
Case Report
Patient 1
A 64 year old lady presented with a three month history of numbness and tingling in the right hand and fingers with generalised weakness and pain aggravated by continuous overhead activity. On examination a soft, non-tender mass in the right supra-clavicular fossa was palpable with a tense, swollen & cyanotic right arm and hand. Distended veins over the right shoulder and chest wall were noted. She recently had a left breast wide local excision for carcinoma with axillary clearance and had an indwelling Hickman line into the right subclavian vein for chemotherapy. MRA confirmed an interbrachial plexus lipoma causing compression of the subclavian vein around the Hickman line. On arterial duplex scanning the arterial signal in the right subclavian artery disappeared on 90° of abduction; Adson’s test positive.
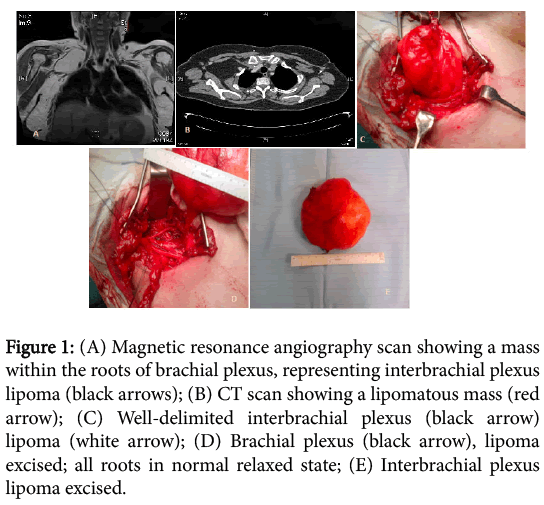
A supraclavicular approach was carried out to excise the lipoma, along with a scalenectomy and first rib resection. The Hickman line was removed. Operative findings found a lipoma within the roots of brachial plexus, C5-C6 stretched anteriorly and C7, C8-T1 pushed posteriorly. Post operatively, patient complained of right arm heaviness associated with some paraesthesia in the right thumb and index finger, these symptoms improved over the next two days. She was discharged on the 3rd post-operative day. The histology confirmed lipoma. Outpatient review at 3 months showed on going neurological improvement and reduction in the chest wall venous distension. At one year, she is asymptomatic from symptoms of N-TOS (Figure 1).
Figure 1: (A) Magnetic resonance angiography scan showing a mass within the roots of brachial plexus, representing interbrachial plexus lipoma (black arrows); (B) CT scan showing a lipomatous mass (red arrow); (C) Well-delimited interbrachial plexus (black arrow) lipoma (white arrow); (D) Brachial plexus (black arrow), lipoma excised; all roots in normal relaxed state; (E) Interbrachial plexus lipoma excised.
Patient 2
A 39-year-old maintenance engineer, presented to the upper limb unit with right-sided periscapular and shoulder pain that increased with exercise, persisting after cessation of activities often being present at rest. The pain was exacerbated by continuous overhead activities and with associated limb weakness. His symptoms had started after surgical removal of a lipoma from the right supraclavicular fossa in another unit. The supraclavicular swelling had not been completely removed. On examination he had altered sensation in the medial aspect of his right arm with pins and needles in the ulnar nerve distribution affecting right hand. Palpation of right infraclavicular fossa revealed a large, soft and fluctuant swelling approximately 8 cm × 10 cm. There was a fullness tracking down to trapezius and further fullness over the anterior aspect of shoulder. Passive movements of the shoulder were well-preserved. Active abduction was limited to 90 degrees. Right upper limb pulses were normal and the hand was normal in colour with Adson’s test being negative. He had dilated veins visible over the anterior chest wall. Ipsilateral trapezius, supraspinatus, infraspinatus and deltoid muscles were weaker than the contralateral side.
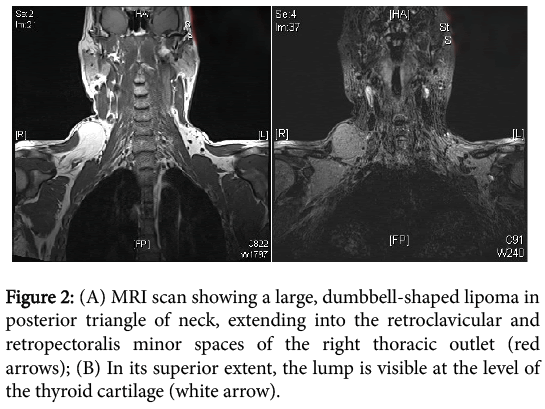
MRI scan of the thorax showed a large lipoma in the right thoracic outlet. Surgical excision of the lipoma was performed to relieve the neurogenic symptoms. This was performed through a clavicular osteotomy and pectoralis minor muscle tenotomy. The patient had uneventful post-operative recovery and was discharged on the 5th day with arrangement for standard post-clavicular plating rehabilitation and shoulder physiotherapy. The histology confirmed lipoma. Five month follow up revealed no evidence of any recurrence of lipoma on clinical examination, alleviation of sensory deficit and a full range of shoulder movements (Figure 2).
Figure 2: (A) MRI scan showing a large, dumbbell-shaped lipoma in posterior triangle of neck, extending into the retroclavicular and retropectoralis minor spaces of the right thoracic outlet (red arrows); (B) In its superior extent, the lump is visible at the level of the thyroid cartilage (white arrow).
Discussion
Lipomas, comprising one-third of all adult soft tissue tumours, may be grouped anatomically as subcutaneous or subfascial. They generally arise between 40 and 60 years of age [6]. There are two lipomatous conditions that can affect a nerve: a solitary lipoma may cause neural compression and an encapsulated lipoma can be located in the nerve. The usually fatty tumors are benign, globose or ovoid, and subcutaneous. They have a fine capsule, are composed entirely of adipose tissue and usually do not involve nerves. Exceptions occur when a large lipoma envelops or compresses a nerve, or originates at a deeper level in the limb and compresses or entraps a nerve, producing symptoms [2] as in our two cases. In these situations, removal is not easy and neural damage can result. Lipomas usually surround a nerve and removal is difficult if this occurs at a brachial plexal level Table 1.
| Author | Year | Cases (No) | Presentation | Interbrachial/ extrabrachial | Intervention | Result |
|---|---|---|---|---|---|---|
| Kim et al. [2] | 1969-1999 | 4 | Neurogenic TOS | Not available | Lipoma excision | No follow up available. |
| Ciampi et al. [3] | 1999-2006 | 4 | Unknown | Not available | Lipoma excision | The minimum follow-up was of three years. Full remission. |
| Sergeant et al. [4] | 2003 | 1 | Neurogenic TOS. | Extrabrachial | Surgical removal of the lipoma. | Complete remission of the symptoms. |
| McKay et al. [5] | 2007 | 1 | Neurogenic and arterial TOS | Extrabrachial | Lipoma excision using a supraclavicular approach extended to a full hemiclamshell. | One month postoperatively a mild residual right eye ptosis noted, otherwise full remission of the symptoms. |
| Guhaet al. [6] | 2011 | 1 | Neurogenic TOS | Extrabrachial | Lipoma excised using supra- and infra-clavicular approaches | No follow up available. |
| Kuyumdzhievet al. | 2013 | 2 | Neurogenic and venous TOS | Interbrachial | Surpaclavicular approach: 1st patient had excision of lipoma, 1st rib resection &scalenectomy; 2nd patient had excision of lipoma with pectoralis minor tenotomy and osteotomy of the clavicle. | Complete remission of the symptoms. |
| Nakamura et al. [7] | 2014 | 2 | Neurogenic TOS | Case 1 -Extrabrachial case 2- Interbrachial | Lipoma excision | Remission of symptoms. |
| Massine El Hammoumi et al. [8] | 2014 | 1 | Palpable mass along the subclavian artery | Extrabrachial | Lipoma excised | Uneventful post op recovery. No follow up. |
Table 1: Literature review of lipomata presenting with neurogenic/venous TOS.
The main problem in the diagnosis of large lipomas is to rule out liposarcomas. Generally, differential diagnosis between lipomas and liposarcomas is impossible by the clinical appearance alone. Large lipomas were reported to show sarcomatous transformation. Computed tomography and MRI are well-established methods of diagnosis. However, even though these methods may yield negative results, the probability of malignancy still cannot be excluded. The histological evaluation of the entire lesion is essential for diagnosis.
The cases discussed here demonstrate a small proportion of presentations that can confront the vascular or orthopaedic surgeon when dealing with N-TOS. Careful preoperative examination and investigation will reveal one of many possible causes for N-TOS. Lipoma is another rare cause of TOS usually presenting as an enlarging neck mass or with nondescript upper limb or shoulder pain. These are slow growing benign tumours, and in reported cases they have had to reach a size of at least 5 or >5 cm to significantly compress the neurovascular bundle [3-5] and present with brachial plexus compressive symptoms, venous thrombosis, or rarely arterial insufficiency [1,3]. The lipoma can be within the trunks/cords of the plexus (interbrachial) or outside (extrabrachial), both creating a surgical challenge during dissection in protecting and preserving the brachial plexus and surrounding structures. The first patient's lipoma stretched C5-C6 (upper trunk) anteriorly and C7 (middle trunk), and C8-T1 (lower trunk) pushed posteriorly.
Computed tomography and MRI are the best modalities in terms of a more detailed delineation of the extent of the lesion and its proximity to the vital structures in the thoracic outlet [5,9]. MRI is especially useful for evaluation of the brachial plexus involvment, as in our cases where both lipomas were interbrachial. The main concern when evaluating a large lipoma is to rule out malignancy. Liposarcomas are the most common soft tissue sarcomas, comprising 7% to 27% of all soft tissue sarcomas [9]. Although rare, malignant transformation into liposarcoma always needs to be taken into consideration.
Scalenectomy, by creating more room, facilitated dissection of this interbrachial lipoma. It is debatable whether or not this patient required 1st rib resection. The second patient had a dumbbell-shaped lipoma extending onto posterior triangle of the neck. The inferior portion of the dumbbell being infra-clavicular, necessitated osteotomy of the right clavicle for a safe approach to the brachial plexus.
Success rates for symptomatic resolution in N-TOS vary in the literature. The operative experience of Balci et al. in 47 cases of N-TOS revealed that 75% with lower brachial plexus and 50% upper plexus compressions remained asymptomatic at 4.6 years [1]. However Franklin et al. at 4.8 years of follow-up found that 72.5% patients were still limited in their activities [10]. As Wood et al. stated in 1998 “there will always be some errors in diagnosis, and surgery must be advised on the basis of exclusion and with great reservation” [11]. In the cases we have reported and the only 12 other cases of brachial plexus lipomata that could be found in the world literature, such pathology appears to provide an opportunity for complete symptomatic resolution through surgery from an identifiable cause of N-TOS[3-5]. These cases highlight the importance of pre-operative investigation if a compressive lesion is causing a mass effect. Surgeons operating on these lesions can expect good symptom resolution for their patients.
References
- Balci AE, Balci TA, Cakir O, Eren S, Eren MN (2003) Surgical treatment of thoracic outlet syndrome: effect and results of surgery. Ann ThoracSurg 75: 1091-1096.
- Kim DH, Murovic JA, Tiel RL, Moes G, Kline DG (2005) A series of 146 peripheral non–neural sheath nerve tumors: 30-year experience at Louisiana State University Health Sciences Center. J Neurosurg 102: 256-266.
- Ciampi P, Scotti C, Gerevini S, De Cobelli F, Chiesa R, et al. (2011) Surgical treatment of thoracic outlet syndrome in young adults: single centre experience with minimum three-year follow-up. IntOrthop 35:1179-1186.
- Sergeant G, Gheysens O, Seynaeve P, Van Cauwelaert J, Ceuppens H (2003) Neurovascular Compression by a SubpectoralLipoma A Case Report of a Rare Cause of Thoracic Outlet Syndrome. Actachirbelg 103: 528-531.
- McKay G, Arlet V, Kern JA, Lau CL, Jones DR,et al. (2009) A bilobed thoracic outlet mass: Options for resection. J ThoracCardiovascSurg 137 :245-247.
- Guha D, Kiehl TR, Guha A (2011) Lipoma compressing the brachial plexus in a patient with sarcoidosis: case report. Br J Neurosurg 25: 530-531.
- Nakamura Y, Teramoto Y, Sato S, Yamada K, Nakamura Y, et al. (2014) Axillary giant lipoma: A report of two cases and published work review. J Dermatol 41: 841-844.
- El Hammoumi M, Taberkanet M, Kabiri el H (2014) Extra-vascular lipoma of the subclavian artery. Arch Bronconeumol 50: 562-563.
- Allen B, Rader C, Babigian A (2007) Giant lipomas of the upper extremity. Can J PlastSurg 15:141-144.
- Franklin GM, Fulton-Kehoe D, Bradley C, Smith-Weller T (2000) Outcome of surgery for thoracic outlet syndrome in Washington state workers' compensation. Neurology 54: 1252-1257.
- Wood VE, Twito R, Verska JM (1988) Thoracic outlet syndrome. The results of first rib resection in 100 patients. OrthopClin North Am 19: 131-146.
Citation: Kuyumdzhiev S, Rogoveanu R, Power D, Vohra R (2016) Lipomata of the Brachial Plexus Causing Neurogenic and Venous Thoracic Outlet Syndrome: Case Reports and Review of the Literature. J Clin Exp Pathol 6:270. DOI: 10.4172/2161-0681.1000270
Copyright: © 2016 Kuyumdzhiev S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 16823
- [From(publication date): 4-2016 - Aug 31, 2025]
- Breakdown by view type
- HTML page views: 15816
- PDF downloads: 1007