Liver biopsy confirming the diagnosis of hepatic and splenic tuberculosis: A report case
Received: 20-Oct-2021 / Accepted Date: 03-Nov-2021 / Published Date: 10-Nov-2021 DOI: 10.4172/2167-7964.1000348
Introduction
Hepatic and splenic tuberculosis are a rare form of extra-pulmonary tuberculosis [1]. Radiological findings of abdominal tuberculosis can mimic those of many different diseases. We report the case of a patient with medical history of joint and pulmonary tuberculosis, who presented hypochondria pain, four months after starting anti-bacillary treatment. CT scan and Echo-guided biopsy diagnosed hepato-splenic tuberculosis.
Case Report
We report the case of a 52-year-old patient with history of scleromyositis, who presented a fever (39-40), associated to dry cough, joint pain and weight loss.
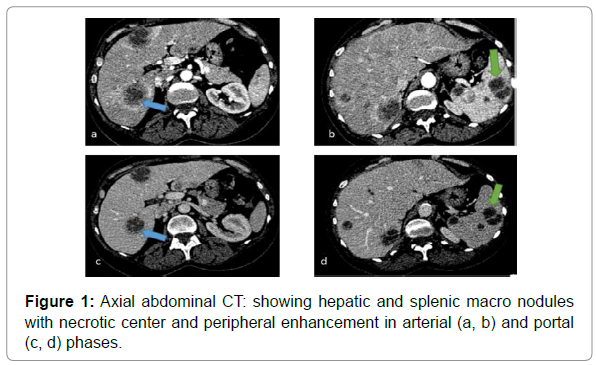
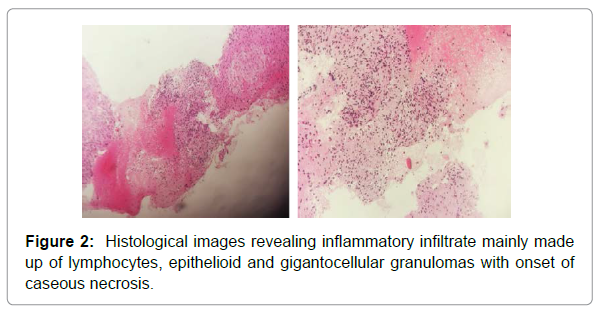
The tuberculin qauntiferon was positive, anti-tuberculosis therapy was started, and 4 months later the patient presented abdominal pain. She underwent for abdominal CT scan that revealed a diffuse hepatic and splenic macro nodules with necrotic center and peripheral enhancement in arterial and portal phases (Figure 1). this aspect was suggestive to hepatic and splenic tuberculosis but we couldn’t eliminate the probability of metastasis. The reason why we complete our investigation by a liver biopsy and the anatomical pathology examination revealed inflammatory infiltrate mainly made up of lymphocytes, epithelioid and gigantocellular granulomas with onset of cases necrosis which match with hepatic tuberculosis (Figure 2).
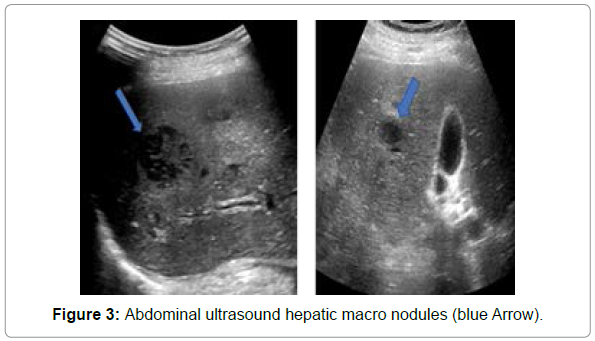
The patient was correctly treated and after one month, she underwent for abdominal ultrasound, which eliminated the presence of a post-biopsy abscess or hematoma and showed an almost stable appearance of the hepatic and splenic macro nodules (Figure 3).
Discussion
Hepatic and splenic tuberculosis is a rare clinical entity even in countries endemic for tuberculosis, representing less than 1% of all cases of tuberculosis, and is usually associated with generalized military tuberculosis [2].
Tuberculosis of the liver and spleen is most likely secondary to hemato genius dissemination of the primary form of the disease [3].
Generally, the disease remains silent and is often incidentally detected while the patient is being evaluated for a mostly non-specific symptomatology. It may however present in the form of abdominal pain or organomegaly which may or may not be associated with clinical jaundice. Jaundice if present is usually a consequence of extra hepatic biliary obstruction secondary to attendant per portal lymphadenopathy [4].
On CT, the liver tubercular appears as an un-enhancing, central, low-density lesion owing to caseation necrosis with a slightly enhancing peripheral rim corresponding to surrounding granulation tissue [5-7]. One of the typical CT features of hepatic tuberculosis might be multiple lesions of varying density, indicating that there are lesions in different pathologic stages coexisting in hepatic TB, including tuberculosis granuloma, liquefaction necrosis, fibrosis or calcification [8].
Tubercular hepatic lesions that are more than 2 cm in size are referred to as macro nodular or pseudotumoral tuberculosis. This form of hepatic tuberculosis is rare compared to the military variant and frequently manifests as solitary or multiple variable-sized hepatic masses. Often it may be difficult to distinguish these lesions from the more common neoplastic and other infective lesions. Depending on the stage of the hepatic granuloma, the imaging appearances can be quiet variable [4].
MRI of hepatic tuberculosis shows a hypo intense nodule with a hypo intense rim on T1-weighted imaging and hypo intense is intense or hypo intense with a less intense rim on T2-weighted imaging, and peripheral enhancement or internal septal enhancement on post-contrast MRI [6,9].
Splenic tuberculosis is rare, clinical and imaging characteristics are similar to those of hepatic tuberculosis and in fact, in the miliary form, both liver and spleen are commonly involved [10]. Radio logically; splenic tuberculosis has been categorized into micro nodular or macro nodular forms, depending on whether it is smaller or larger than 10 mm [11, 12]. Micro nodular tuberculosis is more common and tends to have multiple nodules, usually seen in disseminated systemic tuberculosis. If the nodules are below the resolution capability of imaging techniques, they could manifest as simple splenomegaly. Macro nodular splenic tuberculosis is rare and could manifest as a singular abscess or multiple large nodules [13].
In our case, the abdominal CT revealed the association of hepatic and splenic macro nodules, and even if the patient had medical history of joint and pulmonary tuberculosis. We preferred to complete our investigation by a liver biopsy in order to eliminate the other probable diagnoses.
Conclusion
Hepatic and splenic tuberculosis usually associated with atypical clinical manifestations. Imaging associated with image-guided fine needle aspiration biopsy is the best diagnostic method. Thus allows an early diagnosis and adequate therapeutic management.
References
- Mohamed Jira, Youssef Sekkach, Ali Abouzahir, Driss Ghafir ,Taoufik Amezyane (2015) Tuberculose hépato-splénique, Driss Ghafir University Mohammed V Souissi, hospital militaire instruction Mohammed V, service de medicine interne B, 10000 Rabat, Maroc  44:258-259.
- Essop AR, Posen JA, Hodkinson JH (1984) Tuberculosis hepatitis: a clinical review of 96 cases. Q J Med 53:465-77.
- Mukesh G, Harisinghani, Theresa C, McLoud, Jo-Anne O Shepard, et al.(2000) Tuberculosis from Head to Toe in Radiographic 20:449-470.
- Chandan Kakkar, Ashwin M. Polnay, Prakashini Koteshwara,S Smiti, K. V. Rajagopal, et al.(2015) Hepatic tuberculosis a multimodality imaging review  6:647-658.
- Zheng Wu, Wan-Li Wang, Ying Zhu, Ji-Wen Cheng, Jian Dong1, et al.(2013) Bo Wang Diagnosis and treatment of hepatic tuberculosis: report of five cases and review of literature.. Int J Clin Exp Med 6:845-850.
- Kawamori Y, Matsui O, Kitagawa K, Kadoya M, Takashima T, et al. (1992)Â Macro nodular tuberculoma of the liver: CT and MR findings. AJR Am J Roentgen 158: 311-313.
- Zhang F, Zhang XL, Qiu SJ, Zhang YZ, Wen G, et al. (2006) Diagnostic value of CT on hepatic tuberculosis. Chin J Acad Radiol 40: 658-661.
- Yu RS, Zhang SZ, Wu JJ, Li RF (2004) Imaging diagnosis of 12 patients with hepatic tuberculosis, World J Gastroenterol 10:1639.
- Fan ZM, Zeng QY, Huo JW, Bai L, Liu ZS (1998) Macro nodular multi-organs tuberculoma: CT and MR appearances. J Gastroenterol 33:285-288.
- Pankaj Gupta, Suresh Kumar, Vishal Sharma, Harshal Mandavdhare, Narender Dhaka et al.(2019) Common and uncommon imaging features of abdominal Tuberculosis. J Med Imaging Radiat Oncol 63:329-339.
- Vanhoenacker FM, De Backer AI, Op de BB, Maes M, Van Altena R, et al.(2004) Imaging of gastrointestinal and abdominal tuberculosis, Eur Radiol 14:E103-E115.
- Porcel-Martin A, Rendon-Unceta P, Bascuñana-Quirell A, Amaya-Vidal A, Rodriguez-Ramos C, et al.(1998) Martin-Herrera L Focal splenic lesions in patients with AIDS: sonographic findings. Abdom Imaging 23:196-200.
- Dede F, Doğan E, Demir M, Sener D, Kös M, et al.(2006) Unusual présentation of tuberculoses as a splenic mass, Tohoku J Exp Med. 210:79-82.
Citation: Moslih H, Lrhorfi N, Jidal M, Znati K, Billah NM, et al. (2021) Liver Biopsy Confirming the Diagnosis of Hepatic and Splenic Tuberculosis: A Report Case. OMICS J Radiol 10: 348. DOI: 10.4172/2167-7964.1000348
Copyright: © 2021 Moslih H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Open Access Journals
Article Tools
Article Usage
- Total views: 2995
- [From(publication date): 0-2021 - Dec 19, 2025]
- Breakdown by view type
- HTML page views: 2275
- PDF downloads: 720